Gout: Difference between revisions
No edit summary |
(Linking to other PP pages, spelling correction, general page formatting) |
||
| Line 4: | Line 4: | ||
'''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} | '''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} | ||
</div> | </div> | ||
== Definition/Description | == Definition/Description == | ||
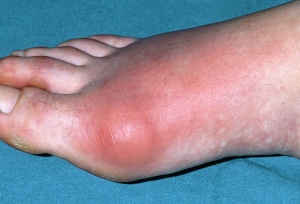
[[Image:1st mtp gout.jpg|thumb|1st mtp gout.jpg]] | [[Image:1st mtp gout.jpg|thumb|1st mtp gout.jpg]] | ||
[[Gout]] is a [[Metabolic/Endocrine Disorders|metabolic disorder]]; however, because the clinical presentation closely resembles [[arthritis]], gout is also classified as '''a form of crystal-induced arthritis''' <ref name="Goodman, Fuller">Goodman CC, Fuller KS. Pathology: Implications for the Physical Therapist. 3rd ed. Saint Louis, MO: Saunders; 2009.</ref> <ref name="Beers">Beers MH, et. al. eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Whitehouse Station, NJ: Merck Research Laboratories; 2006.</ref>.There are three main types of gout, all of which usually begin '''monoarticularly''' at the '''first metatarsophalangeal''' joint and are characterized by sudden pain, swelling, and redness.<ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder">Goodman C, Snyder T. Differential Diagnosis for Physical Therapists: Screening for Referral. St. Louis, Missouri: Saunders Elsevier, 2007.</ref> | |||
Gout is caused by monosodium urate crystal deposition in tissues leading to arthritis, soft tissue masses (i.e., tophi), nephrolithiasis, and urate nephropathy. The biologic precursor to gout is '''elevated serum uric acid levels''' (i.e., hyperuricemia). <ref>Eggebeen AT. University of Pittsburgh Arthritis Institute, Pittsburgh, Pennsylvania 15261, USA</ref><br> | Gout is caused by monosodium urate crystal deposition in tissues leading to arthritis, soft tissue masses (i.e., tophi), nephrolithiasis, and urate nephropathy. The biologic precursor to gout is '''elevated serum uric acid levels''' (i.e., hyperuricemia). <ref>Eggebeen AT. University of Pittsburgh Arthritis Institute, Pittsburgh, Pennsylvania 15261, USA</ref><br>'''Gout''' and '''pseudogou'''t are the 2 most common crystal-induced arthropathies. They are debilitating illnesses in which pain and joint inflammation are caused by the formation of crystals within the joint space. <ref>Joseph Kaplan, MD, MS, FACEP Attending Physician, Department of Emergency Medicine, Martin Army Community Hospital, Fort Benning, Georgia</ref><br> | ||
== Prevalence == | |||
Effects over 2 million people in the US. | |||
Effects over 2 million people in the US. | |||
* The most common crystalopathy (in the US) | * The most common crystalopathy (in the US) | ||
| Line 26: | Line 24: | ||
* Frequency increases in postmenopausal women (lack of oestrogen) <ref name="Goodman, Fuller" /> <ref name="Goodman, Snyder" /> | * Frequency increases in postmenopausal women (lack of oestrogen) <ref name="Goodman, Fuller" /> <ref name="Goodman, Snyder" /> | ||
== Characteristics/Clinical Presentation | == Characteristics/Clinical Presentation == | ||
There are four stages of gout, although diagnosis does not require the presence or occurrence of each stage. The four stages are:<br> | There are four stages of gout, although diagnosis does not require the presence or occurrence of each stage. The four stages are:<br> | ||
#'''Asymptomatic hyperuricemia ( serum urate > 7mg/dl)''': is the phase of gout prior to the first attack, when serum urate levels are elevated but no symptoms are present. <ref name="Goodman, Fuller" /><br> | |||
#'''Acute gouty arthritis:''' is the most often found (90%) at the first '''metatarsophalangeal joint'''. Symptoms generally begin with a sudden onset of localized, intense pain, often occurring at night. The pain may be great enough to awaken the patient. Redness, extreme tenderness, and swelling around the joint will occur within a few hours of the initial pain. Hypersensitivity, chills, tachycardia, malaise, and fever may also be present.<ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" /> The skin may also become red or purplish, shiny, tense, and warm. <ref name="Beers" /> | |||
'''Gouty arthritis is the''' '''most common clincial presentation:''' | |||
Occasionally, acute gouty arthritis can also occur at the '''fingers, [[Wrist and Hand|wrist]], [[elbow]], [[knee]], [[Ankle and Foot|ankle]], and instep.''' Even more '''rarely''', acute gouty arthritis may present at the '''cervical spine, sternoclavicular joint, shoulder, hip''', and '''sacroilliac joint.'''<ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" /> The initial attack may last a few days to 2 weeks, if left untreated <ref name="Beers" /> <ref name="Goodman, Snyder" />. Attacks will recur; however time periods of months or years may elapse between them. As the attacks recur, they will become more intense and may spread to other joints in the body <ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" />. A patient may eventually experience several attacks per year <ref name="Goodman, Fuller" /> <ref name="Beers" /> | Occasionally, acute gouty arthritis can also occur at the '''fingers, [[Wrist and Hand|wrist]], [[elbow]], [[knee]], [[Ankle and Foot|ankle]], and instep.''' Even more '''rarely''', acute gouty arthritis may present at the '''cervical spine, sternoclavicular joint, shoulder, hip''', and '''sacroilliac joint.'''<ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" /> The initial attack may last a few days to 2 weeks, if left untreated <ref name="Beers" /> <ref name="Goodman, Snyder" />. Attacks will recur; however time periods of months or years may elapse between them. As the attacks recur, they will become more intense and may spread to other joints in the body <ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" />. A patient may eventually experience several attacks per year <ref name="Goodman, Fuller" /> <ref name="Beers" /> | ||
{| | {| | ||
| Line 40: | Line 39: | ||
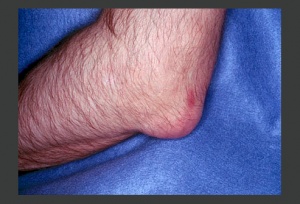
| [[Image:Gout olecranon.jpg|thumb|Presentation of acute gout at the olecranon]] | | [[Image:Gout olecranon.jpg|thumb|Presentation of acute gout at the olecranon]] | ||
|} | |} | ||
3. '''The intercritical phase:''' occurs after recovery from each episode. This phase is asymtomatic and may last for months to years at a time.It is important to note that although this is an aysmptomatic stage, serum urate levels are often still elevated and urate crystals may still be present. <ref name="Goodman, Fuller" /><br>As the gout attacks continue, '''tophi''' will develop in the joints, tendons, bursae, subchondral bone, cartilage, ligaments, subcutaneous tissue, and synovium.<ref name="Goodman, Fuller" /> '''Tophi are hard nodules of sodium urate deposits''' that may vary in number and location.<ref name="Goodman, Fuller" /> <ref name="Goodman, Snyder" /> <ref name="Beers" /> Although typically a painless structure, the formation of tophi can cause an acute inflammatory response within the tissue. <ref name="Goodman, Snyder" /> <ref name="Beers" /> As the tophi become enlarged they may cause deformities, and there is potential for them to protrude through the skin and exude a white chalky substance (urate crystals). <ref name="Goodman, Fuller" /> <ref name="Goodman, Snyder" /> <ref name="Beers" /> Some of the most common sites of enlarged tophi are the forearm, ear, knee and foot. <ref name="Goodman, Fuller" /> | |||
Note: ''Prior'' to the use of urate-lowering drugs for the treatment of acute gouty arthritis, tophi developed in approximately 30 - 50% of patients. <ref name="Goodman, Snyder" /><br> [[Image:Urate crystals.jpg|thumb|Urate Crystals removed from tophi]] 4. '''Chronic tophaceous''' gout is characterized by increased pain, deformity (from tophi), decreased ROM, and subsequent functional loss.<ref name="Goodman, Fuller" /> <ref name="Beers" /> Due to the treatments used for gout today, chronic tophaceous gout is rare. | |||
== Associated Co-morbidities == | |||
== Associated Co-morbidities | |||
Comorbidities with the patterns of gout treatment, the occurrence and the frequency of acute attacks. Cardiometabolic comorbidities, common in this patients' population, were associated with an increased risk of flares<ref name=":0">Primatesta P, Plana E, Rothenbacher D. Gout treatment and comorbidities: a retrospective cohort study in a large US managed care population. BMC musculoskeletal disorders. 2011 Dec;12(1):103.</ref> | Comorbidities with the patterns of gout treatment, the occurrence and the frequency of acute attacks. Cardiometabolic comorbidities, common in this patients' population, were associated with an increased risk of flares<ref name=":0">Primatesta P, Plana E, Rothenbacher D. Gout treatment and comorbidities: a retrospective cohort study in a large US managed care population. BMC musculoskeletal disorders. 2011 Dec;12(1):103.</ref> | ||
== '''Management | == '''Management''' == | ||
The acute gout attacks are painful and potentially disabling, needing immediate treatment. The optimal therapy is towards controlling pain and inflammation '''Drug therapy''' for gout has become an important part of the therapeutic approach to the disease, which includes '''lifestyle modifications'''. Current standards for first-line treatment for acute attacks include '''nonsteroidal anti-inflammatory drugs (NSAIDs),''' '''colchicine''' and '''corticosteroids.''' '''Urate-lowering treatment (ULT)''' ('''most commonly allopurinol''') is usually recommended after the acute attack has resolved.<ref name=":0" /> | The acute gout attacks are painful and potentially disabling, needing immediate treatment. The optimal therapy is towards controlling pain and inflammation '''Drug therapy''' for gout has become an important part of the therapeutic approach to the disease, which includes '''lifestyle modifications'''. Current standards for first-line treatment for acute attacks include '''nonsteroidal anti-inflammatory drugs (NSAIDs),''' '''colchicine''' and '''corticosteroids.''' '''Urate-lowering treatment (ULT)''' ('''most commonly allopurinol''') is usually recommended after the acute attack has resolved.<ref name=":0" /> | ||
== Medications | == Medications == | ||
*NSAIDS ((selective/non-selective),Corticosteroids (oral or injections)<ref name="Goodman, Fuller" /> <ref name="Beers" />: for pain and inflammation management during an acute attack<ref name=":0" />. | *NSAIDS ((selective/non-selective),Corticosteroids (oral or injections)<ref name="Goodman, Fuller" /> <ref name="Beers" />: for pain and inflammation management during an acute attack<ref name=":0" />. | ||
*Allopurinol: to slow the rate of uric acid production and help prevent future attacks | *Allopurinol: to slow the rate of uric acid production and help prevent future attacks | ||
*Cholchicine: occasionally used in the acute phase; however, use is less common due to frequency of side effects and narrow therapeutic range<ref name="Beers" /> <ref name="Goodman, Fuller" /> | *Cholchicine: occasionally used in the acute phase; however, use is less common due to frequency of side effects and narrow therapeutic range<ref name="Beers" /> <ref name="Goodman, Fuller" /> | ||
*Supplementary analgesics | *Supplementary analgesics | ||
*Probenecid and sulfinpyrazone may be used to lower serum urate levels<ref name="Beers" /> | *Probenecid and sulfinpyrazone may be used to lower serum urate levels<ref name="Beers" /> | ||
== Diagnostic Tests/Lab Tests/Lab Values == | |||
*Arthrocentesis and synovial fluid analysis: should be performed upon initial presentation.<ref name="Beers" /> <ref name="Goodman, Fuller" />. | |||
(Gout and pseudogout can be differentiated by examination of the fluid aspirate contents of a joint viewed under '''polarised red light: Urate crystals –''' are '''negatively birefringent –''' they will appear a needle shaped crystals) | |||
= | * Gram stain and culture: to rule out infectious arthritis<ref name="Beers" /> | ||
*Elevated serum urate levels may support diagnosis but are not sensitive or specific. Levels should be measured on several different occasions and it is possible for levels to be normal during and actute attack. Elevated levels are considered to be greater than 7mg/dL.<ref name="Goodman, Fuller" /> <ref name="Beers" /> | |||
*24 hour urate excretion: normal is 600-900 mg. This may help identify hyper production of uric acid or decreased excretion.<ref name="Beers" /> | |||
*Elevated serum urate levels may support diagnosis but are not sensitive or specific. Levels should be measured on several different occasions and it is possible for levels to be normal during and actute attack. Elevated levels are considered to be greater than 7mg/dL.<ref name="Goodman, Fuller" /> <ref name="Beers" /> | |||
*24 hour urate excretion: normal is 600-900 mg. This may help identify hyper production of uric acid or decreased excretion.<ref name="Beers" /> | |||
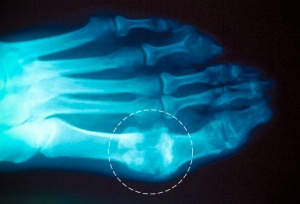
*X-rays: to examine tophi. X-rays are not essential for diagnosis. <ref name="Goodman, Fuller" /> <ref name="Beers" /> | *X-rays: to examine tophi. X-rays are not essential for diagnosis. <ref name="Goodman, Fuller" /> <ref name="Beers" /> | ||
[[Image:X-ray gout.jpg|thumb|X-ray gout.jpg]] | [[Image:X-ray gout.jpg|thumb|X-ray gout.jpg]] | ||
== Causes | == Causes == | ||
There are three types of hyperuricemia based on cause<ref name="Goodman, Fuller" />: <br> | There are three types of hyperuricemia based on cause<ref name="Goodman, Fuller" />: <br> | ||
| Line 89: | Line 79: | ||
#Secondary hyperuricemia can result from a variety of causes including: <br> | #Secondary hyperuricemia can result from a variety of causes including: <br> | ||
* | *Renal dysfunction or disease (haemodialysis, polycystic kidney disease, renal insufficiency)<ref name="Goodman, Snyder" /> <ref name="Beers" /><br> | ||
* | *Leukaemia, lymphomas, psoriasis<ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" /><br> | ||
* | *Hematopoietic disorders (haemolytic anaemia, myeloma, polycythaemia vera, myeloproliferative disorder)<ref name="Goodman, Snyder" /><br> | ||
* | *Chemotherapy agents <ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" /><br> | ||
* | *[[Obesity]], fasting <ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" /><br> | ||
* | *Medications (diuretics, salicylates, levodopa, cyclosporine, low dose aspirin, vitamin B12)<ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" /><br> | ||
* | *Heavy alcohol consumption<ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" /><br> | ||
* | *[[Hypertension]]<ref name="Goodman, Fuller" /> <ref name="Goodman, Snyder" /><br> | ||
* | *[[Metabolic/Endocrine Disorders|Endocrine disorders]]: (hyperparathyroidism, hypoparathyroidism, hyperthyroidism, diabetes mellitus)<ref name="Goodman, Snyder" /><br> | ||
* | *A diet rich in purines (shellfish, organ meats, beans, spinach, etc.)<ref name="Goodman, Fuller" /> <ref name="Beers" /> <ref name="Goodman, Snyder" /><br> | ||
* | *Medical stressors (surgery, trauma, infection, etc.)<ref name="Beers" /><br> | ||
* | *Fatigue or emotional stress <ref name="Beers" /><br> | ||
* | *Toxaemia of pregnancy, hyperlipidaemia, chondrocalcinosis <ref name="Goodman, Snyder" /> | ||
== Systemic Involvement | == Systemic Involvement == | ||
None | |||
None | |||
== Medical Management (current best evidence) == | |||
There are three main goals of the medical management of gout: | |||
#Terminate acute attacks | #Terminate acute attacks | ||
#Prevent | #Prevent recurrence | ||
#Correct and prevent further damage from hyperuricemia<ref name="Goodman, Fuller" /><ref name="Beers" /> | #Correct and prevent further damage from hyperuricemia<ref name="Goodman, Fuller" /><ref name="Beers" /> | ||
<u>Termination of acute attacks</u> - NSAIDs are the most common and generally effective treatment for acute attacks.<ref name="Goodman, Fuller" /><ref name="Beers" /> Cox-2 inhibitors are often the second choice for those who develop GI toxicity; however, they should be used with great caution with any patient with a history of CV complications or co-morbidities.<ref name="Beers" /> Intraarticular corticosteroid injection may also be effective for the management of an acute attack. Colchicine may also be used either po or by IV and may produce substantial pain relief if started immediately after onset of symptoms. Supplementary analgesics may also be recommended along with rest, elevation, and joint protection strategies. <ref name="Goodman, Fuller" /><ref name="Beers" /> | <u>Termination of acute attacks</u> - NSAIDs are the most common and generally effective treatment for acute attacks.<ref name="Goodman, Fuller" /><ref name="Beers" /> Cox-2 inhibitors are often the second choice for those who develop GI toxicity; however, they should be used with great caution with any patient with a history of CV complications or co-morbidities.<ref name="Beers" /> Intraarticular corticosteroid injection may also be effective for the management of an acute attack. Colchicine may also be used either po or by IV and may produce substantial pain relief if started immediately after onset of symptoms. Supplementary analgesics may also be recommended along with rest, elevation, and joint protection strategies. <ref name="Goodman, Fuller" /><ref name="Beers" /> | ||
<u>Prevention of | <u>Prevention of recurrence</u> - Daily low doses of NSAIDs or Colchicine are commonly used to prevent recurrent attacks.<ref name="Beers" /> | ||
<u>Correction and prevention of hyperuricemia</u> - Uricosuric drugs or allopurinol may be used alone or in conjunction. Hypouricemic therapy may also be used for patients with tophi and a higher | <u>Correction and prevention of hyperuricemia</u> - Uricosuric drugs or allopurinol may be used alone or in conjunction. Hypouricemic therapy may also be used for patients with tophi and a higher recurrence rate. Dietary restriction of high-purine foods is a less effective treatment technique but is still recommended. Carbohydrate restrictions may also be helpful. Other treatment possibilities include hydration greater than 3 litres per day. Alkalinization of urine, extracorporeal shock wave lithotripsy, and surgical excision may also be beneficial.<ref name="Beers" /> | ||
See here for a [http://www.niams.nih.gov/Health_Info/Gout/default.asp list of high-purine foods] <ref name="FDA" /> | |||
== Physical Therapy Management (current best evidence) | == Physical Therapy Management (current best evidence) == | ||
Physical therapy management of gout falls under preferred practice pattern 4E: Impaired joint mobility, motor function, muscle performance, and range of motion associated with localized inflammation. <ref name="Goodman, Fuller" /> | Physical therapy management of gout falls under preferred practice pattern 4E: Impaired joint mobility, motor function, muscle performance, and range of motion associated with localized inflammation. <ref name="Goodman, Fuller" /> | ||
The physical therapist should be aware that any patient with a history of gout, hyperuricemia, and/or a septic joint presentation should be | The physical therapist should be aware that any patient with a history of gout, hyperuricemia, and/or a septic joint presentation should be referred for medical evaluation prior to treatment.<ref name="Goodman, Fuller" /> | ||
During acute exacerbations the physical therapist should focus on reinforcement of management program and splinting, orthotics, or other assistive devices to protect the affected joint(s). <ref name="Goodman, Fuller" /> | During acute exacerbations the physical therapist should focus on reinforcement of management program and splinting, orthotics, or other assistive devices to protect the affected joint(s). <ref name="Goodman, Fuller" /> | ||
A 2002 study in the Journal of Rheumatology found that the use of | A 2002 study in the Journal of Rheumatology found that the use of cryotherapy to alleviate the pain associated with acute bouts of gout may be effective. <ref name="cryro">Schlesinger N, Detry MA, Holland BK, Baker DG, Beutler AM, Rull M, Hoffman BI, Schumacher HR Jr. Local ice therapy during bouts of acute gouty arthritis. J Rheumatol 2002; 29(2): 331-334</ref> | ||
During intercritical phases physical therapists may offer assistance with | During intercritical phases physical therapists may offer assistance with maintenance of ROM, strength, and function. The physical therapist can also assist the patient in the creation of a suitable exercise routine and keeping their weight under control. <ref name="Goodman, Fuller" /><ref name="FDA">Gout. National Institute of Arthritis and Musculoskeletal and Skin Diseases. December 2006. http://www.niams.nih.gov/Health_Info/Gout/default.asp. Accessed March 2010.</ref>There is a Randomized Clinical Trial which suggests that Electroacupuncture in combination with blood letting puncture and cupping has relatively good results as a treatment for Gout. The treatment is effective mostly because the blood uric acid decreased significantly after the treatment was given to the patients. <ref>Zhao QW, Liu J, Qu XD, Li W, Wang S, Gao Y, Zhu LW.Department of Nutrition, Longnan Hospital, Daqing Oilfield General Hospital Group in Daqing City of Heilongjiang Province, Daqing 163453, China</ref><br>There is another study about Electroacupuncture combined with local blocking therapy on acute gouty arthritis that shows an improvement in health status of the patients. This treatment is positive and it also decreases blood uric acid levels. <ref>Liu B, Wang HM, Wang FY. The Forth Affiliated Hospital of Harbin Medical University, Harbin, Heilongjiang 150001, China</ref><br> | ||
== Differential Diagnosis == | |||
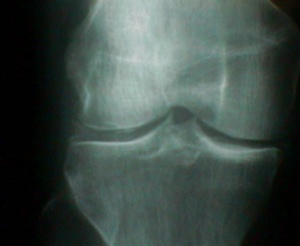
<u>'''Pseudogout:'''</u> is a form of arthritis that occurs 1/8th as often as gout. Symptoms are very similar to gout; however, the knee joint is primarily affected. Diagnosis is made by aspiration of synovial fluid.<ref name="Goodman, Snyder" /><ref name="Wheeless">Wheeless, C R. Pseudogout and Chondrocalcinosis. Wheeless' Textbook of Orthopaedics. November 2008. www.wheelessonline.com/image9/cppd2.jpg. Accessed March 2010.</ref> | |||
<u>'''Pseudogout:'''</u> is a form of arthritis that occurs 1/8th as often as gout.Symptoms are very similar to gout; however, the knee joint is primarily affected. Diagnosis is made by aspiration of synovial fluid.<ref name="Goodman, Snyder" /><ref name="Wheeless">Wheeless, C R. Pseudogout and Chondrocalcinosis. Wheeless' Textbook of Orthopaedics. November 2008. www.wheelessonline.com/image9/cppd2.jpg. Accessed March 2010.</ref> | |||
'''The difference between pseudogout and gout''' : | '''The difference between pseudogout and gout''' : | ||
{{#ev:youtube| KdyEuYhrjlM}}[[Image:Pseuodgout.jpg|thumb]] | {{#ev:youtube| KdyEuYhrjlM}}[[Image:Pseuodgout.jpg|thumb]] | ||
* Other differential diagnosis include: RA, neoplasm, septic arthritis, infectious arthritis, acute rheumatic fever, juvenile RA, acute fracture, and palindromic rheumatism. <ref name="Goodman, Fuller" /><ref name="Beers" /> | * Other differential diagnosis include: [[Rheumatoid Arthritis|RA]], neoplasm, [[Septic (Infectious) Arthritis|septic arthritis]], infectious arthritis, acute rheumatic fever, juvenile RA, acute fracture, and palindromic rheumatism. <ref name="Goodman, Fuller" /><ref name="Beers" /> Gouty arthritis typically presents with rapid development of severe joint pain, swelling, and tenderness that reaches its maximum within just 6-12 h, especially with overlying erythema, most classically in the first metatarsophalangeal joint. Demonstrating the presence of monosodium urate (MSU) crystals in the joint fluid or tophus has been the gold standard for the diagnosis of gout. <ref>Schlesinger N. Department of Medicine, UMDNJ-Robert Wood Johnson Medical School, New Brunswick, NJ 08903</ref> | ||
Case | == Case Reports == | ||
One [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1001146/ case report] that presents interesting implications for the physical therapist involves an elderly patient with lumbar spondylodiscal pathology secondary to her polyarticular gout. <ref>Lagier R, Gee W M. Spondylodiscal erosions due to gout: anatomicoradiological study of a case. Annals of the Rheumatic Diseases. 1983 June; 42(3): 350-353.</ref><br>Interesting [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2572609/?tool=pmcentrez case report] involving a middle aged man that developed symptoms of gout during a hospitalization. <ref>Dhoble A, Balakrishnan V, Smith R. Chronic tophaceous gout presenting as acute arthritis during an acute illness: a case report. Cases Journal. 2008; 1: 238.</ref><br>[https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2572609/?tool=pmcentrez Case report] of a patient whose tophi were limiting the FDS tendon. <ref>Sano K, et. al. Atypical Triggering at the Wrist due to Intratendinous Infiltration of Tophaceous Gout. Springer Hand. 2009 March; 4(1): 78-80.</ref><br>[https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2612045/?tool=pmcentrez Case report] involving presentation and differential diagnosis of acute monoarthritis. <ref>Ma L, Cranney A, and Holroyd-Leduc J. Acute monoarthritis: What is the cause of my patient's painful swollen joint. CMAJ. 2009 January; 180(1): 59-65.</ref> | |||
A series of | A series of [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC286251/?tool=pmcentrez case reports] that examine some of the negative effects of Colchicine as a form of pharmacological management. <ref>Morris I, Varughese G, and Mattingly P. Colchicine in acute gout. BMJ. 2003 November; 327(7426): 1275-1276.</ref> | ||
== References | == References == | ||
<references /> | <references /> | ||
Revision as of 13:59, 14 September 2021
Original Editors - Maggie Kraemer from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Maggie Kraemer, Admin, Lucinda hampton, Shaimaa Eldib, Fitim Cami, Kim Jackson, Simisola Ajeyalemi, Elaine Lonnemann, WikiSysop and Wendy Walker
Definition/Description[edit | edit source]
Gout is a metabolic disorder; however, because the clinical presentation closely resembles arthritis, gout is also classified as a form of crystal-induced arthritis [1] [2].There are three main types of gout, all of which usually begin monoarticularly at the first metatarsophalangeal joint and are characterized by sudden pain, swelling, and redness.[1] [2] [3]
Gout is caused by monosodium urate crystal deposition in tissues leading to arthritis, soft tissue masses (i.e., tophi), nephrolithiasis, and urate nephropathy. The biologic precursor to gout is elevated serum uric acid levels (i.e., hyperuricemia). [4]
Gout and pseudogout are the 2 most common crystal-induced arthropathies. They are debilitating illnesses in which pain and joint inflammation are caused by the formation of crystals within the joint space. [5]
Prevalence[edit | edit source]
Effects over 2 million people in the US.
- The most common crystalopathy (in the US)
- Rarely seen in children (< 10% of all cases) [1]
- Predominantly seen in men (most common inflammatory disease in men over age 30) , however it could affect female patients[6].
- Peak incidence in the 4th - 5th decades of life
Characteristics/Clinical Presentation[edit | edit source]
There are four stages of gout, although diagnosis does not require the presence or occurrence of each stage. The four stages are:
- Asymptomatic hyperuricemia ( serum urate > 7mg/dl): is the phase of gout prior to the first attack, when serum urate levels are elevated but no symptoms are present. [1]
- Acute gouty arthritis: is the most often found (90%) at the first metatarsophalangeal joint. Symptoms generally begin with a sudden onset of localized, intense pain, often occurring at night. The pain may be great enough to awaken the patient. Redness, extreme tenderness, and swelling around the joint will occur within a few hours of the initial pain. Hypersensitivity, chills, tachycardia, malaise, and fever may also be present.[1] [2] [3] The skin may also become red or purplish, shiny, tense, and warm. [2]
Gouty arthritis is the most common clincial presentation:
Occasionally, acute gouty arthritis can also occur at the fingers, wrist, elbow, knee, ankle, and instep. Even more rarely, acute gouty arthritis may present at the cervical spine, sternoclavicular joint, shoulder, hip, and sacroilliac joint.[1] [2] [3] The initial attack may last a few days to 2 weeks, if left untreated [2] [3]. Attacks will recur; however time periods of months or years may elapse between them. As the attacks recur, they will become more intense and may spread to other joints in the body [1] [2] [3]. A patient may eventually experience several attacks per year [1] [2]
File:Gout pip.jpg Presentation of acute gout at the PIP joint |
3. The intercritical phase: occurs after recovery from each episode. This phase is asymtomatic and may last for months to years at a time.It is important to note that although this is an aysmptomatic stage, serum urate levels are often still elevated and urate crystals may still be present. [1]
As the gout attacks continue, tophi will develop in the joints, tendons, bursae, subchondral bone, cartilage, ligaments, subcutaneous tissue, and synovium.[1] Tophi are hard nodules of sodium urate deposits that may vary in number and location.[1] [3] [2] Although typically a painless structure, the formation of tophi can cause an acute inflammatory response within the tissue. [3] [2] As the tophi become enlarged they may cause deformities, and there is potential for them to protrude through the skin and exude a white chalky substance (urate crystals). [1] [3] [2] Some of the most common sites of enlarged tophi are the forearm, ear, knee and foot. [1]
Note: Prior to the use of urate-lowering drugs for the treatment of acute gouty arthritis, tophi developed in approximately 30 - 50% of patients. [3]
4. Chronic tophaceous gout is characterized by increased pain, deformity (from tophi), decreased ROM, and subsequent functional loss.[1] [2] Due to the treatments used for gout today, chronic tophaceous gout is rare.
Associated Co-morbidities[edit | edit source]
Comorbidities with the patterns of gout treatment, the occurrence and the frequency of acute attacks. Cardiometabolic comorbidities, common in this patients' population, were associated with an increased risk of flares[7]
Management[edit | edit source]
The acute gout attacks are painful and potentially disabling, needing immediate treatment. The optimal therapy is towards controlling pain and inflammation Drug therapy for gout has become an important part of the therapeutic approach to the disease, which includes lifestyle modifications. Current standards for first-line treatment for acute attacks include nonsteroidal anti-inflammatory drugs (NSAIDs), colchicine and corticosteroids. Urate-lowering treatment (ULT) (most commonly allopurinol) is usually recommended after the acute attack has resolved.[7]
Medications[edit | edit source]
- NSAIDS ((selective/non-selective),Corticosteroids (oral or injections)[1] [2]: for pain and inflammation management during an acute attack[7].
- Allopurinol: to slow the rate of uric acid production and help prevent future attacks
- Cholchicine: occasionally used in the acute phase; however, use is less common due to frequency of side effects and narrow therapeutic range[2] [1]
- Supplementary analgesics
- Probenecid and sulfinpyrazone may be used to lower serum urate levels[2]
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
(Gout and pseudogout can be differentiated by examination of the fluid aspirate contents of a joint viewed under polarised red light: Urate crystals – are negatively birefringent – they will appear a needle shaped crystals)
- Gram stain and culture: to rule out infectious arthritis[2]
- Elevated serum urate levels may support diagnosis but are not sensitive or specific. Levels should be measured on several different occasions and it is possible for levels to be normal during and actute attack. Elevated levels are considered to be greater than 7mg/dL.[1] [2]
- 24 hour urate excretion: normal is 600-900 mg. This may help identify hyper production of uric acid or decreased excretion.[2]
- X-rays: to examine tophi. X-rays are not essential for diagnosis. [1] [2]
Causes[edit | edit source]
There are three types of hyperuricemia based on cause[1]:
- Primary hyperuricemia is an inherited form of the disorder.
- Idiopathic hyperuricemia does not have a known cause.
- Secondary hyperuricemia can result from a variety of causes including:
- Renal dysfunction or disease (haemodialysis, polycystic kidney disease, renal insufficiency)[3] [2]
- Leukaemia, lymphomas, psoriasis[1] [2] [3]
- Hematopoietic disorders (haemolytic anaemia, myeloma, polycythaemia vera, myeloproliferative disorder)[3]
- Chemotherapy agents [1] [2] [3]
- Obesity, fasting [1] [2] [3]
- Medications (diuretics, salicylates, levodopa, cyclosporine, low dose aspirin, vitamin B12)[1] [2] [3]
- Heavy alcohol consumption[1] [2] [3]
- Hypertension[1] [3]
- Endocrine disorders: (hyperparathyroidism, hypoparathyroidism, hyperthyroidism, diabetes mellitus)[3]
- A diet rich in purines (shellfish, organ meats, beans, spinach, etc.)[1] [2] [3]
- Medical stressors (surgery, trauma, infection, etc.)[2]
- Fatigue or emotional stress [2]
- Toxaemia of pregnancy, hyperlipidaemia, chondrocalcinosis [3]
Systemic Involvement[edit | edit source]
None
Medical Management (current best evidence)[edit | edit source]
There are three main goals of the medical management of gout:
- Terminate acute attacks
- Prevent recurrence
- Correct and prevent further damage from hyperuricemia[1][2]
Termination of acute attacks - NSAIDs are the most common and generally effective treatment for acute attacks.[1][2] Cox-2 inhibitors are often the second choice for those who develop GI toxicity; however, they should be used with great caution with any patient with a history of CV complications or co-morbidities.[2] Intraarticular corticosteroid injection may also be effective for the management of an acute attack. Colchicine may also be used either po or by IV and may produce substantial pain relief if started immediately after onset of symptoms. Supplementary analgesics may also be recommended along with rest, elevation, and joint protection strategies. [1][2]
Prevention of recurrence - Daily low doses of NSAIDs or Colchicine are commonly used to prevent recurrent attacks.[2]
Correction and prevention of hyperuricemia - Uricosuric drugs or allopurinol may be used alone or in conjunction. Hypouricemic therapy may also be used for patients with tophi and a higher recurrence rate. Dietary restriction of high-purine foods is a less effective treatment technique but is still recommended. Carbohydrate restrictions may also be helpful. Other treatment possibilities include hydration greater than 3 litres per day. Alkalinization of urine, extracorporeal shock wave lithotripsy, and surgical excision may also be beneficial.[2]
See here for a list of high-purine foods [8]
Physical Therapy Management (current best evidence)[edit | edit source]
Physical therapy management of gout falls under preferred practice pattern 4E: Impaired joint mobility, motor function, muscle performance, and range of motion associated with localized inflammation. [1]
The physical therapist should be aware that any patient with a history of gout, hyperuricemia, and/or a septic joint presentation should be referred for medical evaluation prior to treatment.[1]
During acute exacerbations the physical therapist should focus on reinforcement of management program and splinting, orthotics, or other assistive devices to protect the affected joint(s). [1]
A 2002 study in the Journal of Rheumatology found that the use of cryotherapy to alleviate the pain associated with acute bouts of gout may be effective. [9]
During intercritical phases physical therapists may offer assistance with maintenance of ROM, strength, and function. The physical therapist can also assist the patient in the creation of a suitable exercise routine and keeping their weight under control. [1][8]There is a Randomized Clinical Trial which suggests that Electroacupuncture in combination with blood letting puncture and cupping has relatively good results as a treatment for Gout. The treatment is effective mostly because the blood uric acid decreased significantly after the treatment was given to the patients. [10]
There is another study about Electroacupuncture combined with local blocking therapy on acute gouty arthritis that shows an improvement in health status of the patients. This treatment is positive and it also decreases blood uric acid levels. [11]
Differential Diagnosis[edit | edit source]
Pseudogout: is a form of arthritis that occurs 1/8th as often as gout. Symptoms are very similar to gout; however, the knee joint is primarily affected. Diagnosis is made by aspiration of synovial fluid.[3][12]
The difference between pseudogout and gout :
- Other differential diagnosis include: RA, neoplasm, septic arthritis, infectious arthritis, acute rheumatic fever, juvenile RA, acute fracture, and palindromic rheumatism. [1][2] Gouty arthritis typically presents with rapid development of severe joint pain, swelling, and tenderness that reaches its maximum within just 6-12 h, especially with overlying erythema, most classically in the first metatarsophalangeal joint. Demonstrating the presence of monosodium urate (MSU) crystals in the joint fluid or tophus has been the gold standard for the diagnosis of gout. [13]
Case Reports[edit | edit source]
One case report that presents interesting implications for the physical therapist involves an elderly patient with lumbar spondylodiscal pathology secondary to her polyarticular gout. [14]
Interesting case report involving a middle aged man that developed symptoms of gout during a hospitalization. [15]
Case report of a patient whose tophi were limiting the FDS tendon. [16]
Case report involving presentation and differential diagnosis of acute monoarthritis. [17]
A series of case reports that examine some of the negative effects of Colchicine as a form of pharmacological management. [18]
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 1.22 1.23 1.24 1.25 1.26 1.27 1.28 1.29 1.30 1.31 1.32 1.33 1.34 1.35 Goodman CC, Fuller KS. Pathology: Implications for the Physical Therapist. 3rd ed. Saint Louis, MO: Saunders; 2009.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 2.23 2.24 2.25 2.26 2.27 2.28 2.29 2.30 2.31 2.32 2.33 2.34 2.35 Beers MH, et. al. eds. The Merck Manual of Diagnosis and Therapy. 18th ed. Whitehouse Station, NJ: Merck Research Laboratories; 2006.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 Goodman C, Snyder T. Differential Diagnosis for Physical Therapists: Screening for Referral. St. Louis, Missouri: Saunders Elsevier, 2007.
- ↑ Eggebeen AT. University of Pittsburgh Arthritis Institute, Pittsburgh, Pennsylvania 15261, USA
- ↑ Joseph Kaplan, MD, MS, FACEP Attending Physician, Department of Emergency Medicine, Martin Army Community Hospital, Fort Benning, Georgia
- ↑ Dirken-Heukensfeldt KJ, Teunissen TA, Van de Lisdonk EH, Lagro-Janssen AL. “Clinical features of women with gout arthritis.” A systematic review. Clinical rheumatology. 2010 Jun 1;29(6):575-82.
- ↑ 7.0 7.1 7.2 Primatesta P, Plana E, Rothenbacher D. Gout treatment and comorbidities: a retrospective cohort study in a large US managed care population. BMC musculoskeletal disorders. 2011 Dec;12(1):103.
- ↑ 8.0 8.1 Gout. National Institute of Arthritis and Musculoskeletal and Skin Diseases. December 2006. http://www.niams.nih.gov/Health_Info/Gout/default.asp. Accessed March 2010.
- ↑ Schlesinger N, Detry MA, Holland BK, Baker DG, Beutler AM, Rull M, Hoffman BI, Schumacher HR Jr. Local ice therapy during bouts of acute gouty arthritis. J Rheumatol 2002; 29(2): 331-334
- ↑ Zhao QW, Liu J, Qu XD, Li W, Wang S, Gao Y, Zhu LW.Department of Nutrition, Longnan Hospital, Daqing Oilfield General Hospital Group in Daqing City of Heilongjiang Province, Daqing 163453, China
- ↑ Liu B, Wang HM, Wang FY. The Forth Affiliated Hospital of Harbin Medical University, Harbin, Heilongjiang 150001, China
- ↑ Wheeless, C R. Pseudogout and Chondrocalcinosis. Wheeless' Textbook of Orthopaedics. November 2008. www.wheelessonline.com/image9/cppd2.jpg. Accessed March 2010.
- ↑ Schlesinger N. Department of Medicine, UMDNJ-Robert Wood Johnson Medical School, New Brunswick, NJ 08903
- ↑ Lagier R, Gee W M. Spondylodiscal erosions due to gout: anatomicoradiological study of a case. Annals of the Rheumatic Diseases. 1983 June; 42(3): 350-353.
- ↑ Dhoble A, Balakrishnan V, Smith R. Chronic tophaceous gout presenting as acute arthritis during an acute illness: a case report. Cases Journal. 2008; 1: 238.
- ↑ Sano K, et. al. Atypical Triggering at the Wrist due to Intratendinous Infiltration of Tophaceous Gout. Springer Hand. 2009 March; 4(1): 78-80.
- ↑ Ma L, Cranney A, and Holroyd-Leduc J. Acute monoarthritis: What is the cause of my patient's painful swollen joint. CMAJ. 2009 January; 180(1): 59-65.
- ↑ Morris I, Varughese G, and Mattingly P. Colchicine in acute gout. BMJ. 2003 November; 327(7426): 1275-1276.