Distal Clavicular Osteolysis
Original Editors - Habibu Salisu Badamasi
Top Contributors - Habibu Salisu Badamasi
Introduction[edit | edit source]
Distal clavicular osteolysis (DCO) is a rare condition that is more common among athletes and weight lifters, particularly those who engage in frequent overhead motions. Also referred to as "weight lifter's shoulder."[1] DCO has been classified as occurring by either traumatic or atraumatic means. DCO results from repetitive excess load on the AC joint, typically through horizontal adduction, adduction, internal rotation, and forward/lateral flexion of the shoulder, such as bench pressing or overhead lifting, and causes pain at the acromial clavicle (AC) joint. Any patient presenting with AC joint or superior shoulder pain should be evaluated for distal clavicular osteolysis.[2]
Anatomy[edit | edit source]
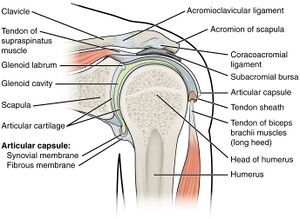
The acromial clavicular (AC) joint is diarthrodial in nature. The proximal clavicle interfaces with the sternum at the sternoclavicular (SC) joint, and the distal clavicle adjoins the acromion process to make the acromioclavicular (AC) joint. A meniscus composed of fibrocartilage is present between the distal clavicle and the acromion. [1] The AC joint receives its static stability from the AC joint capsule (AC ligaments) and the coracoclavicular ligaments; its dynamic stability comes from the deltoid and trapezius muscles.[2]
Causes[edit | edit source]
The most common cause of DCO is aggravating activities such as bench pressing, overhead lifting, and overhead athletic movements such as volleyball, basketball, tennis, and swimming.[2]
These movements cause frequent traction and compression loading of the AC joint, which leads to the repetitive microtrauma pattern implicated in DCO. This repetitive loading causes micro-trauma to the subchondral bone of the distal clavicular head, resulting in subchondral cystic changes, disruption of the articular cartilage, and metaplastic bone formation with increased osteoclastic activity.[1]
An additional cause of DCO was synovial invasion of the subchondral bone, leading to osteolysis. However, this mechanism is debated.[1]
Epidemiology[edit | edit source]
Distal clavicular osteolysis is almost exclusively a diagnosis of young athletes and weight lifters, particularly those engaging in repetitive pressing or overhead activities. However, there is no limit to the age at which DCO can occur physiologically. Historically, DCO was exclusively a disease of young male weightlifters and athletes, but it is now known to appear in females engaged in similar provoking activities.
Signs and symptoms[edit | edit source]
Patients will complain of vague anterior shoulder girdle pain without the sensation of subluxation. They may have tenderness over the AC joint and pain over the lateral clavicle. Often, patients will not be able to recall an isolated traumatic event. Pain may radiate to the trapezius or deltoid region and is relieved with decreased activity and time off from the offending action.[1]
Patients with DCO complain of the gradual onset of dull aching pain, which may be unilateral or bilateral over the distal clavicle and AC joint. localized tenderness and swelling of the lateral clavicle.
Clinical findings[edit | edit source]
There is pain with palpation over the area of the AC joint. Strength is often preserved but there may be some pain inhibition during testing. Range of motion is also typically complete and pain-free outside of the extremes of shoulder abduction and internal rotation. Loading of the AC joint through Hawkins and Scarf tests elicits pain. Including a cervical spine and neurologic exam helps rule out referred pain.
Differential diagnosis[edit | edit source]
Musculoskeletal
- AC joint arthritis
- subacromial bursitis
- superior labral (SLAP) tears
Non-musculoskeletal
- Hyperparathyroidism
- Gout
- Scleroderma
- Rheumatoid arthritis
- Multiple myeloma
- Infection
- Gorham disease
- Referred pain from cervical region
Investigations[edit | edit source]
X-ray: Plain film X-ray of the AC joint is typically sufficient to evaluate for distal clavicular osteolysis. Imaging of DCO often demonstrates microcysts, loss of subchondral bone detail, and osteolysis of the distal clavicle. Early, mild, or unclear radiograph findings warrant consideration of other imaging modalities such as MRI, bone scan, or ultrasound. Diagnostic musculoskeletal ultrasound is an emerging option for diagnosing DCO. Ultrasound may be performed during evaluation by a trained clinician and it may also be more sensitive than plain film X-ray. MRI findings include cortical irregularity, periarticular erosions, joint widening, soft tissue swelling, and edema.[4]
Management[edit | edit source]
The management of DCO includes Physiotherapy, modification of activity, and oral analgesia. excision of the AC joint.
Patient education[edit | edit source]
As with other overuse injuries, educating patient on limitation of provocative maneuvers such as repetitive loading and traction of the AC joint can prevent worsening of DCO.
[edit | edit source]
This allows for counseling these specific patients and identifying their goals and treatment options.[5]
Conservative management[edit | edit source]
Activity modification and nonsteroidal anti-inflammatory medication use are the first line management for DCO. Activity modification of bench press motion modification is widely recommended.[4]
Physiotherapy[edit | edit source]
Although no studies or position statements to date advocate a specific physical therapy regimen for DCO, restoring flexibility and rotator cuff strength are standard recommendations for those with additional shoulder pathology. [6] This consisted of soft tissue therapy (STT), spinal manipulation therapy (SMT), and rehabilitation exercises.[4]
- Soft tissue therapy (STT)- The soft tissue therapy focus on pectoralis minor, teres minor and major, supraspinatus, infraspinatus, subscapularis, rhomboids minor and major, latissimus dorsi, trapezius, and levator scapulae.[4]
- Spinal manipulation therapy (SMT)- The cervical and thoracic spine restricted segments and stretching exercises of the pectoralis minor.[4]
- Rehabilitation exercises- The purpose of exercises is to improve scapular kinesis and ultimately glenoid humeral range of motion. The rehabilitation exercises can be classified into three phases as described by: A case presentation of a 24-year-old female hockey player presented with trauma-induced injury, where she was diagnosed with type II acromio-clavicular joint separation. She presented 5-months later with residual pain and limitations in ranges of motion (ROM). Radiographic images revealed DCO.[4]
Surgical[edit | edit source]
Surgical management can be highly effective for those who fail nonoperative management or athletes unable to modify specific athletic tasks and activities. The mainstay of surgical intervention is resectioning the distal clavicle with no more than 8 mm of excision to avoid iatrogenic AC joint instability. This is performed through an open or arthroscopic technique.[6]
- Open distal clavicle resection: The open procedure offers the surgeon direct visualization and the ability to adjust the resection margin with a broader frame of reference. Additionally, many patients have a large superior osteophyte, which is more easily resected through an open approach. Recovery time for the open approach ranges from 5 to 12 weeks. The argument against the open technique is that it disrupts the deltotrapezial fascia superiorly.[6]
- Arthroscopic distal clavicle resection: The two arthroscopic approaches are direct and indirect. Advantages of these techniques are less tissue dissection and potentially an earlier return to sport and recovery. The direct approach utilizes two portals, one located 1 cm posterior to the AC joint and the other 1 cm anterior.[6] The indirect method requires three portals (anterior, posterior, and lateral), utilizing the subacromial space to visualize the inferior AC joint capsule. Both procedures involve a cutting burr to remove no more than 8 mm to 10mm of the distal end of the clavicle to preserve the anterior and posterior AC ligaments.[6]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 DeFroda SF, Nacca C, Waryasz GR, Owens BD. Diagnosis and management of distal clavicle osteolysis. Orthopedics. 2017 Mar 1;40(2):119-24.
- ↑ 2.0 2.1 2.2 Evans DC, Schroeder JD. Distal Clavicular Osteolysis. InStatPearls [Internet] 2022 May 25. StatPearls Publishing.)
- ↑ Distal clavicular osteolysis Available from:https://youtu.be/kJM8xA4uEFw [last accessed 2 February 2023]
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Abdelkader N, Degraauw C. Detailed management of post-traumatic distal clavicle osteolysis in a 24-year-old female: a case report. The Journal of the Canadian Chiropractic Association. 2021 Dec;65(3):360.
- ↑ Carmona C, Crutwell J, Burnham M, Polak L. Shared decision-making: summary of NICE guidance. bmj. 2021 Jun 17;373.
- ↑ 6.0 6.1 6.2 6.3 6.4 Pensak M, Grumet RC, Slabaugh MA, Bach Jr BR. Open versus arthroscopic distal clavicle resection. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2010 May 1;26(5):697-704.