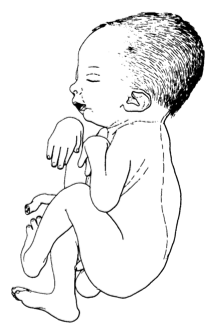
Arthrogryposis Multiplex Congenita
Original Editors - Casey Sisk and Shelby White
Top Contributors - Casey Sisk, Jess Bell, Kim Jackson, Uchechukwu Chukwuemeka, Robin Tacchetti, Evan Thomas, Shelby White, Mande Jooste, WikiSysop, Rucha Gadgil, 127.0.0.1, Naomi O'Reilly, George Prudden, Priyanka Chugh, Meaghan Rieke, Nupur Smit Shah and Elaine Lonnemann
Introduction[edit | edit source]
Arthrogryposis Multiplex Congenita (AMC) "describes joint contractures in two or more areas of the body."[1] AMC is not a specific diagnosis. Contractures can be caused by a range of medical conditions; there are over 400 conditions associated with AMC.[1] If a congenital contracture forms in just one area, it is not AMC. Instead it is referred to as an isolated congenital contracture (e.g. clubfoot).[2]
AMC is a non-progressive condition of unknown cause, but it is associated with a lack of foetal movement - i.e the joint is initially forming as expected, but a lack of movement in utero causes extra connective tissue to form around the joint (fibrous ankylosis).[3][4] AMC is diagnosed at birth, and the primary impairments of children diagnosed with AMC are:[5]
- decreased joint movement in more than one joint
- decreased muscle strength and bulk
Prevalence[edit | edit source]
AMC occurs in around 1 in 3,000 live births.[1] It affects males and females almost equally and it occurs in Asian, African and European populations.[2]
Characteristics/Clinical Presentation[edit | edit source]
The signs and symptoms of AMC vary considerably from person to person.[2]As there are many conditions and syndromes that come under the umbrella of AMC, it can be helpful to use the following categories:[6]
- Amyoplasia
- Distal
- Other types of arthrogryposis
The prognosis of AMC depends on the cause of this condition, as well as the extent of contractures and other changes associated with the condition.[1] It is estimated that around one-third of infants born with AMC will be still born or die before their first birthday.[6]
Clinical signs and symptoms of AMC include:[2][edit | edit source]
- Decreased or absent movement around small and large joints due to contractures
- Muscles of affected limbs are underdeveloped with decreased strength and bulk
- Long bones of the arms and legs are fragile
- Slender build
- Cleft palate
- Cognition may or may not be affected
- Around one-third of babies affected have structural or functional abnormalities of the central nervous system (CNS)
- Usually painless to the child[7]
Most Typical Presentations of AMC[edit | edit source]
- Flexed and dislocated hips, extended knees, clubfeet, internally rotated shoulders, flexed elbows, and flexed and ulnarly deviated wrists
- Abducted and externally rotated hips, flexed knees, clubfeet, internally rotated shoulder, extended elbows, and flexed and ulnarly deviated wrists[5]
Systemic Involvement[edit | edit source]
AMC may be associated with the following:
- neurologic conditions including epilepsy, defects in neural migration, cerebral hypoplasia, holoprosencephaly, pyramidal tract degeneration, and olivopontocerebellar degeneration[8]
- congenital heart defect[8]
- respiratory problems[8]
Other possible effects of AMC include:[4][edit | edit source]
- Undescended testes
- Eating difficulties due to difficulty swallowing and jaw opening weakness
Aetiology[edit | edit source]
The aetiology of AMC is unknown, but it is believed that this condition begins in the first trimester of pregnancy.[5] There are several theories on the cause of AMC, including:
- Decreased movement in utero allowing excessive connective tissue to form around the joints. This can lead to the joint becoming fixed and/or limit joint movement. Decreased foetal movement can have various causes, including foetal crowding (e.g. in multiple births), maternal disorders (viral infections, drug use, trauma, or other maternal illness), and low levels of amniotic fluid around the foetus.[2]
- Genetic and environmental factors[8]
- Less commonly, can be associated with specific muscle conditions, including muscular dystrophy, some mitochondrial disorders, and congenital myopathies[2]
Differential Diagnosis[edit | edit source]
Because AMC is an umbrella term with more than 400 conditions associated with contractures, the differential diagnosis covers many conditions and symdromes. Conditions that might be considered, include:[9]
- Bony fusion (symphalangism, coalition, synostosis)
- Contractural arachnodactyly (Beals syndrome)
- Multiple pterygium syndrome
- Lethal multiple pterygium syndrome
- Osteochondrodysplasias
- Distal arthrogryposis
- Freeman-Sheldon Syndrome
Diagnostic Tests[edit | edit source]
The diagnosis of AMC relies heavily on the clinical examination and evaluation of characteristic symptoms and a detailed patient history. However, other tests that may be done include:
- Ultrasound- used to diagnose lack of foetal mobility and abnormal position in the womb[8]
- Nerve conduction, electromyography and muscle biopsy - to diagnose myopathic or neuropathic disorder[2]
- Imaging studies of the central nervous system (CNS)[2]
- Comparative genomic hybridization (CGH) array[2] - used to identify segmental DNA copy number changes[10]
- Microarray[2]
- Exome studies[2]
Rehabilitation Management[edit | edit source]
There is no specific cure for AMC, but it can be managed with surgical and conservative treatment approaches.[11]
Rehabilitation (occupational therapy, physiotherapy etc) are first-line treatments for AMC. The goal of rehabilitation is to maintain and maximise function, improve joint range of motion and prevent additional muscle atrophy. Physiotherapy treatments can include:
- Gentle joint manipulation[2]
- Use of removable splints for the knees and feet that enable movement[2]
- Application of appropriate orthotics to assist mobility and enhance indendence[12]
- Serial casting of contracted joints[7]
- Muscle strengthening, specifically the hip extensors, quadriceps, and shoulder depressors[7]
- Stretching of joint and muscle contractures to promote active movement and avoid immobilisation[13]
- Encourage parents to initiate a stretching programme at home (3-5 times a day, 3-5 repetitions per set, holding each stretch 20-30 seconds)[5]
- Aquatic therapy [4]
- Hippotherapy[4]
- Prescribing assistive devices (e.g. gait trainer, a walker, crutches, etc)[4]
- Dynamic trunk strengthening
- Ambulation either independently or with an assistive device
- Specifically for infants, physiotherapy might include: gross motor skills (rolling, sitting, crawling, standing, walking, etc)[4], foot abduction braces, thermoplastic serial splinting, position activities such as stretching the hip flexors and prone positioning, and standing in a standing frame/stander.[5]
Surgical and Medical Management[edit | edit source]
Surgical options might be discussed if joint contractures persist after other rehabilitation approaches (therapy, stretching, casting) have been tried. Surgical options vary depending on the location of the contractions.
Surgical interventions may include osteotomies and tendon/ muscle lengthening.[4] In AMC, the tissues surrounding the contracted joint are also affected, which can add complexity to treatment.[14] If an individual with AMC does have muscular limitations, tendon transfers may be performed to improve the length tension relationship and the mechanics of the specific muscle.[2] If a tendon is causing a joint to be held in an abnormal position, a tenotomy can be performed to release the joint from the pull of the tendon. These procedures are usually assisted by capsulotomies as well.[15]
If surgery is being discussed as an option for the child, the following factors are important consideration:
- Soft tissue surgery, such as bone and tendon transfers, should be done early in life (ages 3-12 months)
- Other procedures, such as opponensplasty or osteotomies, should be performed later in life when the joint is almost finished growing
- Casting and bracing are beneficial post-operatively[15]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Society for Maternal-Fetal Medicine; Rac MWF, McKinney J, Gandhi M. Arthrogryposis. Am J Obstet Gynecol. 2019 Dec;221(6):B7-B9.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 Hall JG. Arthrogryposis Multiplex Congenita - NORD (National Organization for Rare Disorders)Available from: http://rarediseases.org/rare-diseases/arthrogryposis-multiplex-congenita/ ( accessed 10 April 2016)
- ↑ Staheli LT. Arthrogryposis: a text atlas. New York: Cambridge University Press; 1998 Available from: http://www.global-help.org/publications/books/help_arthrogryposis.pdf (accessed 10 April 2016)
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 AMCSUPPORT.ORG | Arthrogryposis Multiplex Congenita Support, Inc. Available from: https://www.amcsupport.org/about-us:accessed 2 April 2016)
- ↑ 5.0 5.1 5.2 5.3 5.4 Campbell SK, Palisano RJ, Orlin MN. Physical therapy for children. 4th ed. St. Louis, MO: Elsevier/Saunders; 2012. p313–32.
- ↑ 6.0 6.1 AMSCI. What is Arthrogryposis Multiplex Congenita (AMC)?. Available from: https://www.amcsupport.org/about-arthrogryposis (last accessed 24 April 2023).
- ↑ 7.0 7.1 7.2 Perajit E, Kamolporn K, Ekasame V. Walking ability in patients with arthrogryposis multiplex congenita. Indian Journal Of Orthopaedics. 2014; 48(4): 421-425.
- ↑ 8.0 8.1 8.2 8.3 8.4 Kalampokas E, Kalampokas T, Sofoudis C, Deligeoroglou E, Botsis D. Diagnosing Arthrogryposis Multiplex Congenita: A Review. ISRN Obstetrics & Gynecology. 2012;264918.
- ↑ Gucev ZS, Pop-Jordanova N, Dumalovska G, Stomnaroska O, Zafirovski G, Tasic VB. Arthrogryposis multiplex congenital (AMC) in a three year old boy: differential diagnosis with distal arthrogryposis: a case report. Cases journal. 2009; 2:9403. doi: 10.1186/1757-1626-2-9403.http://casesjournal.biomedcentral.com/articles/10.1186/1757-1626-2-9403
- ↑ Lockwood WW, Chari R, Chi B, Lam WL. Recent advances in array comparative genomic hybridization technologies and their applications in human genetics. Eur J Hum Genet. 2006 Feb;14(2):139-48.
- ↑ Johns Hopkins Medicine. Arthrogryposis. Available from https://www.hopkinsmedicine.org/health/conditions-and-diseases/arthrogryposis (last accessed 24 April 2023).
- ↑ Bartonek Å. The use of orthoses and gait analysis in children with AMC. Journal Of Children's Orthopaedics. 2015; 9(6): 437-447.
- ↑ Kimber E. AMC: amyoplasia and distal arthrogryposis Springer Link. Journal of Children's Orthopaedics; 2015. Available from: http://link.springer.com/article/10.1007/s11832-015-0689-1 (accessed 10 April 2016)
- ↑ Graydon AJ, Eastwood DM. Orthopaedic Management of Arthrogryposis Multiplex Congenita. Springer Link. European Surgical Orthopaedics and Traumatology; 2014 Available from: http://link.springer.com/referenceworkentry/10.1007/978-3-642-34746-7_172 (accessed 10 April 2016)
- ↑ 15.0 15.1 Chen H. Arthrogryposis Treatment & Management: Medical Care, Surgical Care, Consultations. Medscape; 2015. Available from: http://emedicine.medscape.com/article/941917-treatment#d6 (accessed 10 April 2016)