Cervical Cancer: Difference between revisions
No edit summary |
No edit summary |
||
| Line 40: | Line 40: | ||
== Medications == | == Medications == | ||
'''Drugs Approved to Prevent Cervical Cancer'''<br> | '''Drugs Approved to Prevent Cervical Cancer'''<br> | ||
*Cervarix (Recombinant HPV Bivalent Vaccine) | *Cervarix (Recombinant HPV Bivalent Vaccine) | ||
*Gardasil (Recombinant HPV Quadrivalent Vaccine) | *Gardasil (Recombinant HPV Quadrivalent Vaccine) | ||
*Recombinant Human Papillomavirus (HPV) Bivalent Vaccine | *Recombinant Human Papillomavirus (HPV) Bivalent Vaccine | ||
*Recombinant Human Papillomavirus (HPV) Quadrivalent Vaccine | *Recombinant Human Papillomavirus (HPV) Quadrivalent Vaccine | ||
'''Drugs Approved to Treat Cervical Cancer'''<br> | '''Drugs Approved to Treat Cervical Cancer'''<br> | ||
*Blenoxane (Bleomycin) | '''''*'''Systemic Chemotherapy involves injecting or orally administering cancer-treating drugs. These drugs then enter the bloodstream, and travel throughout the body, reaching areas of cancerous growth.Chemotherapy can work in the following ways:'' | ||
*Bleomycin | |||
*Cisplatin | ''<br> -Cure the cancer<br> -Shrink the cancer<br> -Relieve symptoms<br> -Prolong life span by controlling cancer or putting it into remission <br>'' | ||
*Hycamtin (Topotecan Hydrochloride) | |||
*Platinol (Cisplatin) | ''Chemotherapy is often delivered in cycles. Periods of treatment are followed by a recovery period. ''<br> | ||
*Platinol-AQ (Cisplatin) | |||
*Topotecan Hydrochloride | *Blenoxane (Bleomycin) | ||
*Carboplatin | *Bleomycin | ||
*Paclitaxel (Taxol) | *Cisplatin | ||
*Topotecan | *Hycamtin (Topotecan Hydrochloride) | ||
*Platinol (Cisplatin) | |||
*Platinol-AQ (Cisplatin) | |||
*Topotecan Hydrochloride | |||
*Carboplatin | |||
*Paclitaxel (Taxol) | |||
*Topotecan | |||
*Gemcitabine (Gemzar) | *Gemcitabine (Gemzar) | ||
| Line 114: | Line 120: | ||
[[Category:Bellarmine_Student_Project]] | [[Category:Bellarmine_Student_Project]] | ||
<br> | |||
Revision as of 02:45, 19 March 2014
Original Editors - Anna Marie Usery & Stephanie Wilton from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Anna Usery, Stephanie Wilton, Kim Jackson, Nupur Smit Shah, WikiSysop, Rewan Elsayed Elkanafany, Elaine Lonnemann, Wendy Walker, Vidya Acharya, Manisha Shrestha and Lucinda hampton
Definition/Description[edit | edit source]
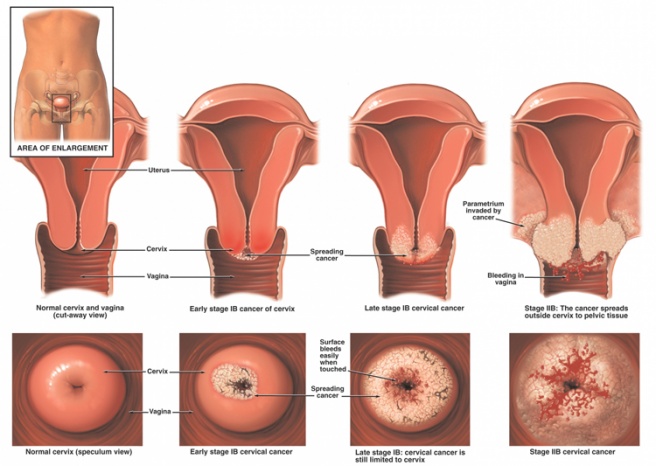
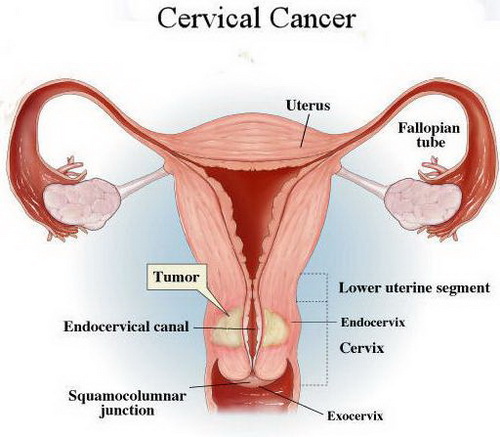
Cervical cancer is a type of cancer that forms within the tissues of the cervix.[1]The cervix connects the uterus with the vagina (birth cancal).[1], [2]The endocervix is the portion of the cervix closest to the uterus whereas the exocervix or ectocervix is closest to the vagina.[2] The cervix is covered in two main types of cells: squamous cells found on the exocervix, and glandular cells on the endocervix.[2] Squamous and glandular cells come together at the area known as the transformation zone. It is here where most cervical cancers originate.[2] Gradually, the normal cells lining this area develop pre-cancerous changes that change into cancer.[2] Cervical cancer typically grows at a slow rate and presents asymptomatically.[1] Therefore, it is recommended to receive routine Papanicolaou smears to test for changes in the lining of the cervix and/or the development of cancerous cells.[1]
Prevalence[edit | edit source]
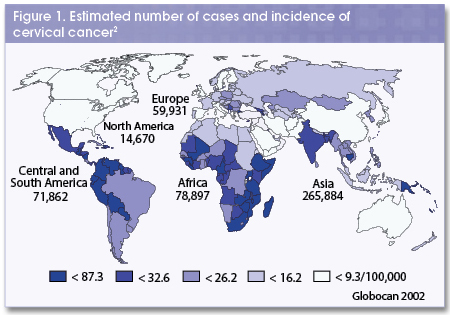
In the United States, cervical cancer is the fourteenth most common type of cancer found in women, and the third most common gynecological malignancy.[3],[4] However worldwide, cervical cancer is the most commonly found type of cancer in women.[3] In the United States, diagnosis of invasive stage cervical cancer has declined (75% decline since the 1960s) steadily.[3],[4]Screening for cervical cancer has become more common due to the introduction of the Pap smear in the 1930’s which made early detection possible.[5] Although cervical cancer is the most common cause of gynecological cancer-related death worldwide, mortality rates have decreased significantly in the United States (more than 45% since the early 1970s).[4],[5]
In the United States, approximately 11,000 women are diagnosed with cervical cancer and 3,700 women die due to the disease each year.[5] Worldwide,nearly 500,000 women are diagnosed with cervical cancer annually.[6] The disease accounts for 288,000 deaths per year.[5]
80% to 85% of cervical cancer realted deaths occur in developing countries.[6]
Pre-invasive carcinoma in situ (no invasion of surrounding tissues) is more common in women 30-40 years of age.[4] Invasive carcinoma is more frequent in women over 40 years of age.[4] Women ages 65 and over account for 25% of new cases of cervical cancer.[5]
Characteristics/Clinical Presentation[edit | edit source]
- May be asymptomatic (early stages)[4]
- Painful intercourse or pain after intercourse[4]
- Unexplained or unexpected bleeding (after intercourse or between menstrual periods)[3],[4]
- Watery, foul-smelling vaginal discharge (serosanguineous or yellowish color)[3],[4]
- Pelvic, epigastric, or low back pain (with large lesions)[3],[5]
- Hemiparesis, headache (cancer recurrence with brain metastases)[4]
- Bowel and bladder problems (later stages)[5]
Associated Co-morbidities[edit | edit source]
add text here
Medications[edit | edit source]
Drugs Approved to Prevent Cervical Cancer
- Cervarix (Recombinant HPV Bivalent Vaccine)
- Gardasil (Recombinant HPV Quadrivalent Vaccine)
- Recombinant Human Papillomavirus (HPV) Bivalent Vaccine
- Recombinant Human Papillomavirus (HPV) Quadrivalent Vaccine
Drugs Approved to Treat Cervical Cancer
*Systemic Chemotherapy involves injecting or orally administering cancer-treating drugs. These drugs then enter the bloodstream, and travel throughout the body, reaching areas of cancerous growth.Chemotherapy can work in the following ways:
-Cure the cancer
-Shrink the cancer
-Relieve symptoms
-Prolong life span by controlling cancer or putting it into remission
Chemotherapy is often delivered in cycles. Periods of treatment are followed by a recovery period.
- Blenoxane (Bleomycin)
- Bleomycin
- Cisplatin
- Hycamtin (Topotecan Hydrochloride)
- Platinol (Cisplatin)
- Platinol-AQ (Cisplatin)
- Topotecan Hydrochloride
- Carboplatin
- Paclitaxel (Taxol)
- Topotecan
- Gemcitabine (Gemzar)
Drug Combinations Used in Cervical Cancer
- Gemcitabine-Cisplatin
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
add text here
Etiology/Causes[edit | edit source]
add text here
Systemic Involvement[edit | edit source]
627
Medical Management (current best evidence)[edit | edit source]
add text here
Physical Therapy Management (current best evidence)[edit | edit source]
add text here
Alternative/Holistic Management (current best evidence)[edit | edit source]
add text here
Differential Diagnosis[edit | edit source]
add text here
Case Reports/ Case Studies[edit | edit source]
add links to case studies here (case studies should be added on new pages using the case study template)
Resources
[edit | edit source]
add appropriate resources here
Recent Related Research (from Pubmed)[edit | edit source]
see tutorial on Adding PubMed Feed
Extension:RSS -- Error: Not a valid URL: addfeedhere|charset=UTF-8|short|max=10
References[edit | edit source]
see adding references tutorial.
- ↑ 1.0 1.1 1.2 1.3 Available at: http://www.cancer.gov/cancertopics/types/cervical. Accessed March 18, 2014.
- ↑ 2.0 2.1 2.2 2.3 2.4 Available at: http://www.cancer.org/cancer/cervicalcancer/detailedguide/cervical-cancer-what-is-cervical-cancer. Accessed March 18, 2014.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Ph.d. SE, Ph.d. KL. Understanding Pathophysiology. Mosby Incorporated; 2011.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 4.9 Goodman CC, Snyder TE. Differential Diagnosis for Physical Therapists, Screening for Referral. W B Saunders Company; 2012.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 Reviews CT. e-Study Guide for: Pathology: Implications for the Physical Therapist by Catherine C. Goodman, ISBN 9781416031185. Cram101 Textbook Reviews; 2012.
- ↑ 6.0 6.1 Available at: http://www.rho.org/about-cervical-cancer.htm. Accessed March 18, 2014.