Myasthenia Gravis: Case Study: Difference between revisions
No edit summary |
No edit summary |
||
| Line 3: | Line 3: | ||
== Introduction == | == Introduction == | ||
It is necessary for physiotherapists to take a comprehensive past medical history to screen for the comorbidities associated with MG, including a screen for red flags. It is also important to consider the patient's medications (especially corticosteroid use), and the presence of possible underlying conditions. These findings can limit treatment approaches and be contraindications or precautions for some manual therapy or exercise treatments. | Myasthenia Gravis (MG) is an autoimmune disease affecting the antibodies to receptors at the neuromuscular junction, causing muscle weakness and fatigue<ref name=":0">Gilhus, N.E., Nacu, A., Andersen, J.B. and Owe, J.F. Myasthenia gravis and risks for comorbidity. Eur J Neurol 2015; 22: 17-23. doi: 10.1111/ene.12599 </ref>. It is necessary for physiotherapists to take a comprehensive past medical history to screen for the comorbidities associated with MG, including a screen for red flags. It is also important to consider the patient's medications (especially corticosteroid use), and the presence of possible underlying conditions. These findings can limit treatment approaches and be contraindications or precautions for some manual therapy or exercise treatments. | ||
=== Pathophysiology === | |||
Individuals with MG have decreased acetylcholine and voltage-gated sodium channels due to damage of their postsynaptic membranes (Dresser et al., 2021). This dysfunction in the neuromuscular junction results in decreased response and amplitude of the corresponding muscles (Dresser et al., 2021).{{#ev:youtube|e31zVpZXug4}} | |||
Gravis: A Systematic Review, International Journal of Neuroscience 2011; 121:3, 121-129. doi: 10.3109/00207454.2010.539307 </ref>, [[Rheumatoid Arthritis]] <ref name=":2" /><ref name=":3" />, and [[Diabetes Mellitus Type 1]] <ref name=":0" /><ref name=":1" /><ref name=":2" />. Some other common comorbidities include [[Hypertension]], [[COPD (Chronic Obstructive Pulmonary Disease)|COPD]] <ref name=":2" />, and an increased risk for respiratory infections due to muscle weakness and other issues related to prolonged corticosteroid use<ref name=":1" /> | === Combordities === | ||
Patients diagnosed with MG may present with several comorbidities. Since it is an autoimmune disorder, patients are at an increased risk for other autoimmune diseases such as Thymoma (thymus tumor) <ref name=":0" /><ref name=":1">Gilhus N. E. Myasthenia gravis, respiratory function, and respiratory tract disease. Journal of neurology 2023; 1–12. Advance online publication. doi: 10.1007/s00415-023-11733-y </ref>, [[Systemic Lupus Erythematosus]] <ref name=":0" /><ref name=":2">Misra, U. K., Kalita, J., Singh, V. K., & Kumar, S. A study of comorbidities in myasthenia gravis. Acta neurologica Belgica 2020; 120(1), 59–64. doi: 10.1007/s13760-019-01102-w </ref><ref name=":3">Zhi-Feng Mao, Long-Xiu Yang, Xue-An Mo, Chao Qin, Yong-Rong Lai, NingYu He, Tong Li & Maree L. Hackett. Frequency of Autoimmune Diseases in Myasthenia | |||
Gravis: A Systematic Review, International Journal of Neuroscience 2011; 121:3, 121-129. doi: 10.3109/00207454.2010.539307 </ref>, [[Rheumatoid Arthritis]] <ref name=":2" /><ref name=":3" />, and [[Diabetes Mellitus Type 1]] <ref name=":0" /><ref name=":1" /><ref name=":2" />. Some other common comorbidities include [[Hypertension]], [[COPD (Chronic Obstructive Pulmonary Disease)|COPD]] <ref name=":2" />, and an increased risk for respiratory infections due to muscle weakness and other issues related to prolonged corticosteroid use<ref name=":1" />. | |||
== Introduction == | |||
== Presentation == | == Presentation == | ||
This autoimmune disease is relatively uncommon with approximately 20 out of 100,000 individuals diagnosed with MG in the United States <ref name=":7">Jayam Trouth A, Dabi A, Solieman N, Kurukumbi M, Kalyanam J. Myasthenia Gravis: A Review. Autoimmune diseases. 2012;2012:874680–10. doi: 10.1155/2012/874680</ref>. Reported prevalence in Ontario, Canada is similar with 32 out of 100,000 individuals<ref name=":5">Breiner A, Widdifield J, Katzberg HD, Barnett C, Bril V, Tu K. Epidemiology of myasthenia gravis in Ontario, Canada. Neuromuscular disorders : NMD. 2016;26(1):41–6. doi: 10.1016/j.nmd.2015.10.009</ref>. In both Canada and the United States, there appears to be a greater incidence of younger women (<60 and <50 years old, respectively), diagnosed with MG<ref name=":7" /><ref name=":5" />. Whereas, in Canada and the United States, incidence appears to be greater in older men (>60 and >50 years old, respectively)<ref name=":7" /><ref name=":5" />. | This autoimmune disease is relatively uncommon with approximately 20 out of 100,000 individuals diagnosed with MG in the United States <ref name=":7">Jayam Trouth A, Dabi A, Solieman N, Kurukumbi M, Kalyanam J. Myasthenia Gravis: A Review. Autoimmune diseases. 2012;2012:874680–10. doi: 10.1155/2012/874680</ref>. Reported prevalence in Ontario, Canada is similar with 32 out of 100,000 individuals<ref name=":5">Breiner A, Widdifield J, Katzberg HD, Barnett C, Bril V, Tu K. Epidemiology of myasthenia gravis in Ontario, Canada. Neuromuscular disorders : NMD. 2016;26(1):41–6. doi: 10.1016/j.nmd.2015.10.009</ref>. In both Canada and the United States, there appears to be a greater incidence of younger women (<60 and <50 years old, respectively), diagnosed with MG<ref name=":7" /><ref name=":5" />. Whereas, in Canada and the United States, incidence appears to be greater in older men (>60 and >50 years old, respectively)<ref name=":7" /><ref name=":5" />. | ||
| Line 83: | Line 87: | ||
*'''Ankle:''' dorsiflexion 3+/5 BL; plantarflexion 4+/5 BL | *'''Ankle:''' dorsiflexion 3+/5 BL; plantarflexion 4+/5 BL | ||
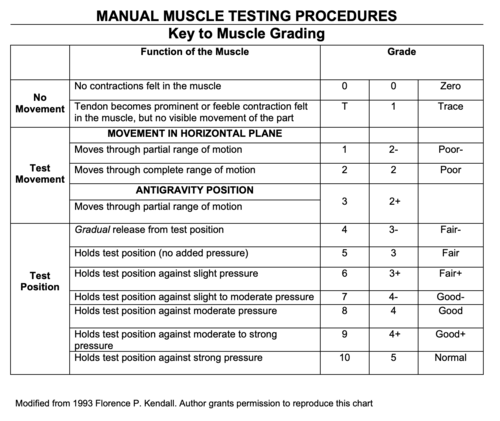
(Figure | (Figure 2 - Manual Muscle Testing Procedure - Key to muscle grading)<ref>National Institute of Environmental Health Sciences. Manual Muscle Testing Procedures. Available from: <nowiki>https://www.niehs.nih.gov/research/resources/assets/docs/muscle_grading_and_testing_procedures_508.pdf</nowiki> (accessed 11 May 2023).</ref> | ||
=== Neurological Scan === | === Neurological Scan === | ||
Revision as of 15:05, 12 May 2023
Abstract[edit | edit source]
This project is a fictional case study developed by Physical Therapy students from Queen's University to help with the understanding of the implications of a Myasthenia Gravis (MG) diagnosis on physical therapy assessment and treatment. The case study shows the clinical presentation, expectation of symptoms, comorbidities, and impairments of a patient diagnosed with MG. The case also presents some objective measures and treatment options based on individualities of the patient’s disease presentation. It is important to note that MG symptoms can vary among individuals, so the following assessment, outcome measures, and treatment plan may not be appropriate for all individuals diagnosed with MG, and an individual assessment would be necessary to determine the best course of action for other patients.
Introduction[edit | edit source]
Myasthenia Gravis (MG) is an autoimmune disease affecting the antibodies to receptors at the neuromuscular junction, causing muscle weakness and fatigue[1]. It is necessary for physiotherapists to take a comprehensive past medical history to screen for the comorbidities associated with MG, including a screen for red flags. It is also important to consider the patient's medications (especially corticosteroid use), and the presence of possible underlying conditions. These findings can limit treatment approaches and be contraindications or precautions for some manual therapy or exercise treatments.
Pathophysiology[edit | edit source]
Individuals with MG have decreased acetylcholine and voltage-gated sodium channels due to damage of their postsynaptic membranes (Dresser et al., 2021). This dysfunction in the neuromuscular junction results in decreased response and amplitude of the corresponding muscles (Dresser et al., 2021).
Combordities[edit | edit source]
Patients diagnosed with MG may present with several comorbidities. Since it is an autoimmune disorder, patients are at an increased risk for other autoimmune diseases such as Thymoma (thymus tumor) [1][2], Systemic Lupus Erythematosus [1][3][4], Rheumatoid Arthritis [3][4], and Diabetes Mellitus Type 1 [1][2][3]. Some other common comorbidities include Hypertension, COPD [3], and an increased risk for respiratory infections due to muscle weakness and other issues related to prolonged corticosteroid use[2].
Introduction[edit | edit source]
Presentation[edit | edit source]
This autoimmune disease is relatively uncommon with approximately 20 out of 100,000 individuals diagnosed with MG in the United States [5]. Reported prevalence in Ontario, Canada is similar with 32 out of 100,000 individuals[6]. In both Canada and the United States, there appears to be a greater incidence of younger women (<60 and <50 years old, respectively), diagnosed with MG[5][6]. Whereas, in Canada and the United States, incidence appears to be greater in older men (>60 and >50 years old, respectively)[5][6].
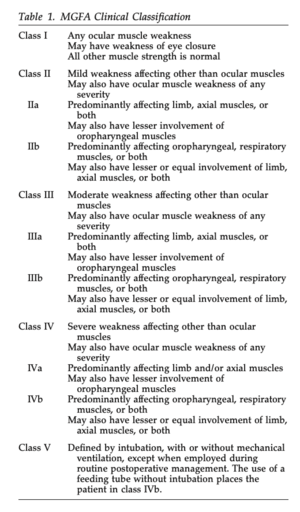
As seen in Figure 1, the Myasthenia Gravis Foundation of America defines five main classes of MG with corresponding subclasses[7]. This system helps to determine a patient’s prognosis and potential response to treatment depending on their symptom severity[7].
Signs and Symptoms[edit | edit source]
The initial symptom that presents for two thirds of individuals is weakness of the extrinsic ocular muscles of the eyes[5]. This can present as ptosis, diplopia, and blurry vision[5]. The symptoms typically progress to include other bulbar and limb muscles in approximately half of patients within two years[5]. One of the primary symptoms of MG is muscle fatigue and weakness, primarily skeletal muscle groups, that is exacerbated by activity and improves with rest[5]. Factors such as heat exposure, stress, and infection also worsen fatigue[5]. Muscle weakness can present as generalized or localized to oculomotor muscles, respiratory muscles, and pharyngeal muscles affecting the ability to swallow[2].
Client Characteristics[edit | edit source]
The client is a 34-year-old, Caucasian woman, named Maya Stevens, who was recently diagnosed with Myasthenia Gravis. Mrs. Stevens reached out to her family doctor after experiencing a number of abnormal symptoms apart from her other diagnoses (Rheumatoid Arthritis and Hypertension). She was aware that a common comorbidity of these conditions is Myasthenia Gravis, and thought it was appropriate to seek medical advice. She was referred to Physical Therapy to address concerns, and to learn preventative techniques to avoid a decline in function and maintain future symptoms associated with the disease. Mrs. Stevens is a motivated, pleasant individual who is prepared to take a rehabilitative approach to her diagnosis.
Subjective[edit | edit source]
History of Present Illness (HPI)[edit | edit source]
Patient reports feeling fine in the morning, but becomes more fatigued in the afternoon and as the day progresses. She has been increasingly stressed while starting back at work after maternity leave, taking care of two young kids, and having a husband who works long hours. She has been taking care of many of the household duties and has a hard time picking up her kids. She initially noticed difficulty keeping her eyes open while attempting to take out her contacts at night, 9 months ago. Over the next month, her eye drooping became more persistent throughout the day and she began experiencing episodes of double vision. Additionally, she noticed muscular fatigue in her shoulders while kayaking, as she isn’t able to paddle for as long without taking breaks. She describes her fatigue as unusual, not like the sensation one has after working out or after exertion. Other activities that are particularly bothersome are baking and grocery shopping. She also noticed increased shortness of breathing while kayaking, which has progressed to less exertional activities, such as entering the stairs into her home at the end of the day.
Past Medical History (PMHx)[edit | edit source]
Mrs. Stevens was diagnosed with Rheumatoid Arthritis five years ago (currently well maintained and has not caused any problems) and hypertension nine months ago (currently well maintained and has not caused any problems) after giving birth to her second child. Mrs. Stevens was diagnosed with Myasthenia Gravis two months ago and has been experiencing an increase in symptoms.
Family History (FHx)[edit | edit source]
Mrs. Stevens Great Aunt had MG.
Medications (MEDS)[edit | edit source]
- Methotrexate for RA (10 mg, 1x/week)
- Lisinopril for hypertension (5 mg, 1x/day)
- Women’s Multivitamin (1x/day)
Social History (SHx)[edit | edit source]
Patient lives in Kingston, Ontario in a bungalow with four steps to enter the home with a railing on both sides. She lives with her husband and two kids (one year and four years old). Mrs. Stevens works at a dental clinic as a receptionist and spends most of her day sitting, using the computer, and answering client questions and phone calls.
Health Habits (HH)[edit | edit source]
Does not smoke or use drugs. Has one glass of wine every evening (6-7 drinks/week) to wind down. Patient has been increasingly stressed after returning to work since leaving maternity leave, and has been partaking in a majority of the household and childcare duties while her husband works long hours in construction.
Current Functional Status (FnSt)[edit | edit source]
- bADLs: independent in most bADLs, but becomes fatigued from prolonged walking (greater than 30 minutes)
- iADLs: independent in the morning, but becomes more fatigued throughout the day making it more difficult to clean, cook meals, shop, drive, or do housework
- Physical Activity: difficulty finding time to exercise as she is often fatigued and tends to become more tired from exercise
Functional History (FnHx)[edit | edit source]
About a year before diagnosis, patient was fully independent in all bADLs, iADLs, ambulation, work activities, and family activities.
Objective[edit | edit source]
Observation[edit | edit source]
Upon observation, Mrs. Stevens was alert and oriented, making light conversation. Patient demonstrates some hoarseness of speech, and an apical breathing pattern. She demonstrates right-sided asymmetrical ptosis with exertion, as well as forward head posture.
Vital Signs[edit | edit source]
- Heart Rate (HR): 74 beats per minute
- Respiratory Rate (RR): 18 breaths per minute
- Blood Pressure (BP): 128/82
- Radial Pulse: strong and regular
Active and Passive Range of Motion[edit | edit source]
Active range of motion (AROM) and passive range of motion (PROM) were tested for upper extremity (U/E) and lower extremity (L/E) joints, and Mrs. Stevens demonstrated pain free AROM and PROM within normal limits bilaterally.
Strength[edit | edit source]
Manual Muscle Testing (MMT) was performed for U/E and L/E bilaterally (BL), as well as for the cervical spine. Upon assessment, Mrs. Stevens had the following MMT results:
- Cervical Spine: flexion & extension 3/5 BL; side flexion and rotation 4+/5 BL
- Shoulder: 3/5 flexion & abduction BL; 4/5 extension and adduction BL
- Elbow: 4/5 flexion & extension BL
- Wrist: 4+/5 flexion, extension; radial & ulnar deviation BL
- Handgrip: 4-/5 BL
- Hip: 3/5 flexion & abduction BL; 4-/5 extension & adduction BL
- Knee: 4+/5 knee flexion & extension BL
- Ankle: dorsiflexion 3+/5 BL; plantarflexion 4+/5 BL
(Figure 2 - Manual Muscle Testing Procedure - Key to muscle grading)[8]
Neurological Scan[edit | edit source]
A neurological scan was conducted to determine if the patient has any neurological deficits from her condition such as loss of sensation, loss of motor function, change to deep tendon reflexes, and assessment of Upper Motor Neuron lesions.
Mrs. Stevens cervical and lumborosacral dermatomes were intact, while all myotomes were affected, likely due to muscular weakness. All Upper Motor Neuron tests (Babinski, Hoffman's, and Clonus) were negative, while Lower Motor Neuron (Triceps - C7, Biceps - C6, Patellar - L3/L4, Achilles - S1/S2) reflex tests all had a normal grade. A table below provides the Cranial Nerve test results and the possible effects these tests may have on the individual.
| Cranial Nerves | CN V (Trigeminal) | CN VI (Abducens) | CN X (Vagus) |
|---|---|---|---|
| Result | (+) Motor, Sensation Intact | (+) Motor, Diplopia | (+) Motor, Dysphonia |
Balance, Ambulation, and Cognitive Functioning[edit | edit source]
- Balance: The Berg Balance Scale was completed and Mrs. Stevens scored 41/56. This indicates a greater risk of future falls (42 and under), however, she is still within the category of being independent with no gait aid.
- Ambulation: Mrs. Stevens presents with an unsteady gait; she is unable to walk in a straight line, and has slight side deviations, likely due to diploplia.
- Cognitive Functioning: Mrs. Stevens cognition is intact, and she is alert and oriented.
Outcome Measures[edit | edit source]
Myasthenia Gravis Composite[9][edit | edit source]
This 10-item scale measures primary signs and symptoms of Myasthenia Gravis based on physical exam and patient history (2). Items include weakness of the ocular, neck and proximal limb muscles, as well as patient-reported impairments in speech, chewing, swallowing, visual and respiratory function[10]. Each item is scored on a weighted, ordinal scale, based on symptom severity[10]. Total score ranges from 0 to 50, in which higher scores indicate more severe impairment (2). Improvement of 3-points in the total score on the MGC denotes clinically meaningful change[10]. The MGC has been found to be both a reliable and valid tool for the measurement of clinical status of Myasthenia Gravis patients, due to its excellent test-retest reliability and concurrent validity with other MG-specific measurement scales[9]. Due to its simplicity and timely delivery, the MGC will be used to evaluate muscle strength as well as global functional impairments[11].
Myasthenia Gravis Quality of Life[12][edit | edit source]
This 15-item, patient-reported outcome is derived from the MG-QOL60 and measures health-related quality of life, specific to the Myasthenia Gravis patient population[11]. Items are related to physical, emotional, functional and social elements, such as mobility, well-being and symptoms, and each are scored on a Likert scale ranging from 0 to 4[11]. The total score ranges from 0 to 60, such that higher scores suggest poorer quality of life[11]. The MG-QOL15 has been translated and validated in numerous languages, has excellent test-retest reliability, and its scores correlate well with other MG-specific measurement tools, such as the MGC, Myasthenia Gravis Activities of Daily Living measure (MG-ADL), and Quantitative Myasthenia Gravis Score (QMGS)[11].
Berg Balance Scale[edit | edit source]
The BBS is a 14-item measurement that evaluates balance in the elderly, as well as several neurological conditions, including, but not limited to stroke, multiple sclerosis, and peripheral neuropathies[13]. The scale assesses the patient’s ability to maintain balance throughout the performance of listed tasks (9). Each item is scored on a Likert-scale, ranging from 0 to 4, in which 0 represents the lowest level of function and 4 represents the highest level of function (9). A total score is out of 56 (9). When a patient achieves a score less than 42 and has no history of falls, this indicates the patient is at a greater risk of future falls (8). The BBS has high test-retest reliability and internal validity for measuring balance in neurological conditions, independent of the etiology of the balance impairment[13].
Problem List[edit | edit source]
Body Structure & Function[edit | edit source]
- Impaired breathing mechanics and increased dyspnea on exertion.
- Decreased endurance presenting as weakness in proximal limb muscles (arms, legs, neck).
- Impaired balance leading to an increased risk of falls.
Activity Limitations[edit | edit source]
- Decreased endurance when standing and ambulating for longer than 30 minutes without rest.
Participation Restrictions[edit | edit source]
- Reduced ability to kayak for long durations.
- Reduced ability to care for and play with her children.
Clinical Hypothesis[edit | edit source]
- Medical Diagnosis: Myasthenia Gravis - Class IIIb
- Add picture of description?
- Physiotherapy Diagnosis: Generalized fatigue which presents as bilateral muscle weakness, primarily in the proximal joints in the upper and lower extremity, affecting balance, endurance, and participation in social roles.
- Prognosis: Mrs. Stevens is a young, previously active woman who demonstrates high motivation to manage her symptoms and improve her quality of life, positively contributing to her prognosis. Barriers to improvement include her comorbidities of rheumatoid arthritis and hypertension, as well as familial responsibilities, which may exacerbate her fatigue. Additionally, her depressive symptoms may challenge her progress and impede adherence to her exercise plan. We anticipate that with regular participation in exercise, her endurance will improve to aid with symptom management and participation in meaningful activities.
Interventions[edit | edit source]
Patient-Centered Goals[edit | edit source]
Goal setting is an essential component of physiotherapy to outline a course of action for the patient and therapist to follow throughout a rehabilitation journey. Creating meaningful, patient-centered goals can enhance patient engagement, satisfaction, and adherence which will supplement recovery and improvement. Long-term and short-term goals for Mrs. Stevens will be outlined below, and were determined based off of the subjective interview and objective assessment.
- LTG1: Patient will be able to kayak for 30 minutes at a low intensity with minimal rest time within the next two months associated with improvements in MGS score.
- STG1: Patient will increase the repetitions of their resistance exercises before fatigue to 20 reps within four weeks.
- STG2: Patient will improve her MGS score from 20/60 to 15/60 by week four.
- STG3: Patient will improve her aerobic endurance on the stationary bike to 30 minutes by three weeks.
- LTG2: Patient will be able to ambulate for at least 45 minutes with minimal rest before onset of fatigue within six weeks.
- STG4: Patient will improve her aerobic endurance on the stationary bike to 30 minutes by three weeks.
- LTG3: Patient will be able to engage in meaningful activities for 45 minutes with minimal shortness of breath within six weeks.
- STG5: By week two, patient will learn and implement pursed lip breathing when she feels short of breath 50% of the time.
- STG6: By week four, patient will use diaphragmatic breathing at rest and during activity for 75% of the time.
- LTG4: Patient will be able to engage more with care and activities with her children, as a result of reduction in symptom severity, as demonstrated by improvements in her MG-QOL15 score within 6 weeks.
- STG7: STG6: By week four, patient will improve her MGC-QOL 15 score from 32/60 to 25/60.
- Patient will be able to maintain a single leg stance bilaterally for one minute on an even surface without assistance within two weeks.
- LTG5: Patient will reduce their risk of falls demonstrated through improvements in Berg Balance Score within 6 weeks.
- STG8: Patient will be able to maintain a single leg stance bilaterally for 1 minute on an uneven surface without assistance within 2 weeks.
- STG9: Patient will increase her Berg Balance score from 41/56 to 45/56 within two months.
Approaches and Techniques[edit | edit source]
Regression of Exercises[edit | edit source]
Innovative Technologies[edit | edit source]
Interdisciplinary Care Management[edit | edit source]
Speech Language Pathologist[edit | edit source]
A Speech Language Pathologist (SLP)[14] can help to identify and manage the presence of issues with speaking, chewing and swallowing. This may include exercises that strengthen the muscles of the throat, vocal exercises to improve voice clarity, swallowing exercises, and the timing of pharmacological interventions. Due to results from the MGC, there are indications that the patient would benefit from SLP therapy.
Occupational Therapist[edit | edit source]
An Occupational Therapist (OT)[14] can assist with the difficulties Mrs. Stevens faces with ADLs due to generalized muscular weakness. This could include tasks and activities that require endurance like food preparation, childcare, and grocery shopping. This could help Mrs. Stevens to reach her goals, including baking for her children.
Psychiatrist[edit | edit source]
Studies have shown MG to be associated with mood disorders[15]. This puts Mrs. Stevens at a higher risk of developing depression and anxiety. Therefore, it is recommended for her to have a psychiatric evaluation to address any of these factors that may be present. Further, this professional can help with acceptance and coping for her during a difficult time with a lifelong neurological diagnosis.
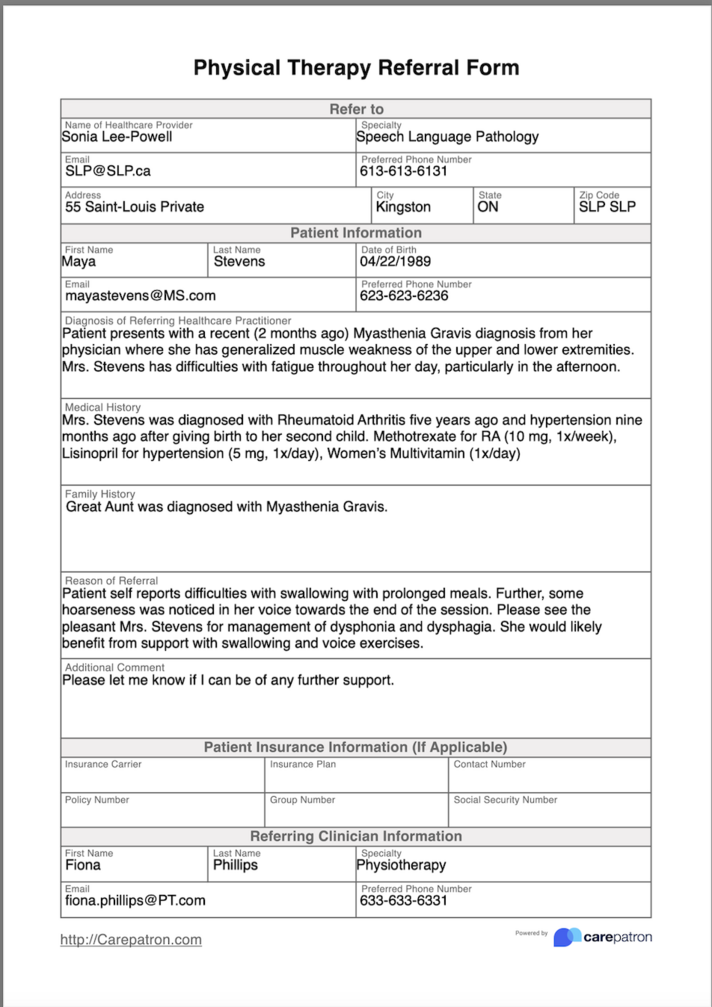
Referral Form[edit | edit source]
Outcome Re-Assessment[edit | edit source]
The outcome re-assessment was performed three months after the referral; results can be found below.
MGC score: Following 3 months of participating in physiotherapy, Mrs. Stevens completed the MGC again and scored a 15/50. This improvement in score suggests Mrs. Stevens symptom severity has decreased within the past 3 months. The minimally clinically important difference (MCID) for the MGS is 3 points, therefore improvement in this outcome measure reflects meaningful change in symptom severity for Mrs. Stevens[10].
MG-QOL15 score: After completing 3 months of physiotherapy, Mrs. Stevens also completed the MGS-QOL15 again and scored a 24/60. This suggests an improvement in Mrs. Stevens’ quality of life related to her MG. Subjectively, Mrs. Stevens reports feeling more motivated to participate in activities, such as kayaking due to reduction in her symptoms.
Berg Balance Scale: Following 3 months of physiotherapy, Mrs. Stevens was re-assessed on the Berg Balance Scale and scored a 48/56. This change in score suggests improvements in balance, and furthermore, decreased risk of falling. Subjectively, Mrs. Stevens describes feeling more steady on her feet.
Discharge Planning[edit | edit source]
Mrs. Stevens will be discharged from the Physiotherapist’s caseload once the she has met all her goals and is comfortable continuing all exercises independently at home. Patient is encouraged to continue to monitor her symptoms and return to physiotherapy should new circumstances arise.
Discussion[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Gilhus, N.E., Nacu, A., Andersen, J.B. and Owe, J.F. Myasthenia gravis and risks for comorbidity. Eur J Neurol 2015; 22: 17-23. doi: 10.1111/ene.12599
- ↑ 2.0 2.1 2.2 2.3 Gilhus N. E. Myasthenia gravis, respiratory function, and respiratory tract disease. Journal of neurology 2023; 1–12. Advance online publication. doi: 10.1007/s00415-023-11733-y
- ↑ 3.0 3.1 3.2 3.3 Misra, U. K., Kalita, J., Singh, V. K., & Kumar, S. A study of comorbidities in myasthenia gravis. Acta neurologica Belgica 2020; 120(1), 59–64. doi: 10.1007/s13760-019-01102-w
- ↑ 4.0 4.1 Zhi-Feng Mao, Long-Xiu Yang, Xue-An Mo, Chao Qin, Yong-Rong Lai, NingYu He, Tong Li & Maree L. Hackett. Frequency of Autoimmune Diseases in Myasthenia Gravis: A Systematic Review, International Journal of Neuroscience 2011; 121:3, 121-129. doi: 10.3109/00207454.2010.539307
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 Jayam Trouth A, Dabi A, Solieman N, Kurukumbi M, Kalyanam J. Myasthenia Gravis: A Review. Autoimmune diseases. 2012;2012:874680–10. doi: 10.1155/2012/874680
- ↑ 6.0 6.1 6.2 Breiner A, Widdifield J, Katzberg HD, Barnett C, Bril V, Tu K. Epidemiology of myasthenia gravis in Ontario, Canada. Neuromuscular disorders : NMD. 2016;26(1):41–6. doi: 10.1016/j.nmd.2015.10.009
- ↑ 7.0 7.1 7.2 Jaretzki A, Barohn RJ, Ernstoff RM, Kaminski HJ, Keesey JC, Penn AS, et al. Myasthenia gravis : Recommendations for clinical research standards. Neurology. 2000;55(1):16–23. doi: 10.1016/S0003-4975(00)01595-2
- ↑ National Institute of Environmental Health Sciences. Manual Muscle Testing Procedures. Available from: https://www.niehs.nih.gov/research/resources/assets/docs/muscle_grading_and_testing_procedures_508.pdf (accessed 11 May 2023).
- ↑ 9.0 9.1 Burns TM, Conaway M, Sanders DB. The MG Composite: A valid and reliable outcome measure for myasthenia gravis. Neurology. 2010;74(18):1434–40. doi: 10.1212/WNL.0b013e3181dc1b1e
- ↑ 10.0 10.1 10.2 10.3 Thomsen JLS, Andersen H. Outcome Measures in Clinical Trials of Patients With Myasthenia Gravis. Frontiers in neurology. 2020;11:596382–596382. doi: 10.3389/fneur.2020.596382
- ↑ 11.0 11.1 11.2 11.3 11.4 Barnett C, Herbelin L, Dimachkie MM, Barohn RJ. Measuring Clinical Treatment Response in Myasthenia Gravis. Neurologic clinics. 2018;36(2):339–53. doi: 10.1016/j.ncl.2018.01.006
- ↑ Burns TM, Conaway MR, Cutter GR, Sanders DB. Less is more, or almost as much: A 15-item quality-of-life instrument for myasthenia gravis. Muscle & nerve. 2008;38(2):957–63. doi: 10.1002/mus.21053
- ↑ 13.0 13.1 La Porta F, Caselli S, Susassi S, Cavallini P, Tennant A, Franceschini M. Is the Berg Balance Scale an Internally Valid and Reliable Measure of Balance Across Different Etiologies in Neurorehabilitation? A Revisited Rasch Analysis Study. Archives of physical medicine and rehabilitation. 2012;93(7):1209–16. doi: 10.1016/j.apmr.2012.02.020
- ↑ 14.0 14.1 Payedimarri A babu, Ratti M, Rescinito R, Vasile A, Seys D, Dumas H, et al. Development of a Model Care Pathway for Myasthenia Gravis. International journal of environmental research and public health. 2021;18(21):11591–.
- ↑ Law C, Flaherty CV, Bandyopadhyay S. A Review of Psychiatric Comorbidity in Myasthenia Gravis. Curēus (Palo Alto, CA). 2020;12(7):e9184–e9184.