Tularemia: Difference between revisions
Dana Collins (talk | contribs) No edit summary |
No edit summary |
||
| (99 intermediate revisions by 7 users not shown) | |||
| Line 1: | Line 1: | ||
<div class="editorbox"> | |||
'''Original Editors '''- Dana Collins [[Pathophysiology of Complex Patient Problems|from Bellarmine University's Pathophysiology of Complex Patient Problems project.]] | '''Original Editors '''- Dana Collins [[Pathophysiology of Complex Patient Problems|from Bellarmine University's Pathophysiology of Complex Patient Problems project.]] | ||
''' | '''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} | ||
</div> | </div> | ||
== Definition/Description == | == Definition/Description == | ||
Tularemia, named after the infectious gram-negative bacterium Francisella tularensis, is a zoonotic disease. A zoonotic disease is one that is spread from animal to human. This spread may be directly i.e. handling contaminated meat or through a carrier i.e. a tick. It is also known as “Ohara’s disease”, “rabbit fever”, “deer-fly fever”,<ref name="A">Wilson M, Lountzis N, Ferringer T. Zoonoses of dermatologic interest. Dermatologic Therapy. 2009;22:367-378. http://onlinelibrary.wiley.com/doi/10.1111/j.1529-8019.2009.01248.x/abstract. Accessed February 2011.</ref> “market’s men disease”, “meat-cutter’s disease”, “glandular type of tick fever”, “water rat-trappers’ disease”. It is highly infectious, <10 organisms causing severe disease in both humans and animals.<ref name="F">Petersen JM, Schriefer ME. Tularemia: emergence/re-emergence. Vet Res. 2005;36:455-467. http://digitalcommons.unl.edu/cgi/viewcontent.cgi?article=1031&context=zoonoticspub&sei-redir=1#search=%22Petersen+JM,+Schriefer+ME.+Tularemia:+emergence/re-emergence.%22. Accessed February 2011.</ref> There are 4 sub-types of the bacterium, the most common in the United States are Type A, tularenis, and Type B, holarctica. It is on the Center for Disease Control’s list of bioterroism threats. | Tularemia, named after the infectious gram-negative bacterium Francisella tularensis, is a [[Zoonotic Diseases|zoonotic disease]]. A zoonotic disease is one that is spread from animal to human (infected humans can NOT pass the disease to other humans). This spread may be directly i.e. handling contaminated meat or through a carrier i.e. a tick. It is also known as “Ohara’s disease”, “rabbit fever”, “deer-fly fever”,<ref name="A">Wilson M, Lountzis N, Ferringer T. Zoonoses of dermatologic interest. Dermatologic Therapy. 2009;22:367-378. http://onlinelibrary.wiley.com/doi/10.1111/j.1529-8019.2009.01248.x/abstract. Accessed February 2011.</ref> “market’s men disease”, “meat-cutter’s disease”, “glandular type of tick fever”, “water rat-trappers’ disease”. It is highly infectious, <10 organisms causing severe disease in both humans and animals.<ref name="F">Petersen JM, Schriefer ME. Tularemia: emergence/re-emergence. Vet Res. 2005;36:455-467. http://digitalcommons.unl.edu/cgi/viewcontent.cgi?article=1031&context=zoonoticspub&sei-redir=1#search=%22Petersen+JM,+Schriefer+ME.+Tularemia:+emergence/re-emergence.%22. Accessed February 2011.</ref> There are 4 sub-types of the bacterium, the most common in the United States are Type A, tularenis, and Type B, holarctica. It is on the Center for Disease Control’s list of bioterroism threats. | ||
<br> | <br>{{#ev:youtube| zUVQB39ATME }} [[Image:Tularmemia Colonis.jpg|right|http://sfcdcp.org/tularemia.html]]<br> | ||
http:// | |||
== Prevalence == | == Prevalence == | ||
| Line 17: | Line 14: | ||
The prevalence of Tularemia in the United States depends on the geographical location and the time of year. During the spring and summer months (May-September), there is a rise in reported cases. South-Central, Pacific Northwest, and parts of the East Coast have the highest incidence of Tularemia. While the population most effected is young males 5-9 years old and those > 75 years old.<ref name="E">Hayes E, Marshall S, Dennis D. Tualremia--United States,1990-2000. www.cdc.gov/mmwr/preview/mmwrhtml/mm5109a1.htm. February 20, 2011.</ref><br> | The prevalence of Tularemia in the United States depends on the geographical location and the time of year. During the spring and summer months (May-September), there is a rise in reported cases. South-Central, Pacific Northwest, and parts of the East Coast have the highest incidence of Tularemia. While the population most effected is young males 5-9 years old and those > 75 years old.<ref name="E">Hayes E, Marshall S, Dennis D. Tualremia--United States,1990-2000. www.cdc.gov/mmwr/preview/mmwrhtml/mm5109a1.htm. February 20, 2011.</ref><br> | ||
[[Image:Tularemia_Image_1.jpg]]<br> | [[Image:Tularemia Image 1.jpg|Image:Tularemia_Image_1.jpg]]<br> | ||
[[Image:Tularemia_Image_2.jpg]]<br> | [[Image:Tularemia Image 2.jpg|Image:Tularemia_Image_2.jpg]]<br> | ||
[[Image:Tularemia_Image_3.jpg]]<br> | [[Image:Tularemia Image 3.jpg|Image:Tularemia_Image_3.jpg]]<br> | ||
The above images from: http://www.cdc.gov/tularemia/statistics/.<br> | The above images from: http://www.cdc.gov/tularemia/statistics/.<br> | ||
== Characteristics/Clinical Presentation == | == Characteristics/Clinical Presentation<ref name="CIDRAP" /><ref name="B" /><ref name="Treatment of" /><ref name="E" /><ref name="A" /> == | ||
{| style="width: 702px; height: 136px" border="1" cellspacing="1" cellpadding="1" | {| style="width: 702px; height: 136px" border="1" cellspacing="1" cellpadding="1" | ||
|- | |- | ||
| | | | ||
| | *'''''Fever''''' | ||
| | *Abdominal pain | ||
*''Arthralgias'' | |||
*''Shortness of breath'' | |||
*'''Malaise''' | |||
*Nausea/Vomiting | |||
*''Sore throat''<br> | |||
*'''Tender local lymph nodes ''' | |||
| style="vertical-align: top" | | |||
| | |||
*'''Chills''' | |||
*Prostration | |||
*Conjunctivitis | |||
*'''Diaphoresis<br>''' | |||
*'''Axillary adenopathy''' | |||
*''Non-Productive Cough'' | |||
*Hemoptysis | |||
*''Pt usually presents w/ what appears to be community acquire pneumonia, however it does not respond to conventional treatment'' | |||
| | |||
*''Headache'' | |||
*'''''Myalgias''''' | |||
*'''''Cutaneous ulcers''''' | |||
*Weight loss | |||
*'''Epitrochlear adenopathy''' | |||
*Pleuritic chest pain, retrosternal pain | |||
*'''Painful skin lesion''' @ site of infection (ulceroglandular only) <br> | |||
|} | |||
Note: The 2 most common forms are glandular/ulcerglandular and pneumonic.<br>Those occurring in ≥25% of those infected with the '''glandular''' and '''ulceroglandular''' form are in bold<ref name="CIDRAP" /><br>Those occurring in ≥25% of those infected with the ''pneumonic'' form are in italics<ref name="CIDRAP" /> | |||
<br> <br> | |||
{| border="1" cellspacing="1" cellpadding="1" width="200" align="center" | |||
|- | |||
| bgcolor="#cccccc" width="100" | [[Image:Tularemia Thumb.jpg|border|left|250x300px|http://pathmicro.med.sc.edu/ghaffar/zoonoses.htm]] | |||
| [[Image:Tularemia Lymph.jpg|border|left|260x300px|http://www.cdc.gov/ncidod/eid/vol8no1/01-0131G1.htm]] | |||
|} | |} | ||
| |||
== Expectations/Prognosis<ref name="B" /> == | |||
Untreated: Fatality ~5%<br> | |||
Treated: Fatality <1% | |||
<br> | |||
Poor outcomes have been associated with those who have underlying co-morbidities such as alcoholism or diabetes and those who delay seeking medical treatment.<ref name="CIDRAP" /> | |||
== Medications<ref name="CIDRAP" /> == | == Medications<ref name="CIDRAP" /> == | ||
| Line 50: | Line 84: | ||
Antibiotic therapy is used to treat Tularemia. Streptomyocin and Gentamicin are usually the first administered. Ciprofloxacin along with other fluoroquinolones. Tetracycline and chloramphenicol may also be used to treat Tularemia, however they have higher relapse rates than the previously mentioned.<br> | Antibiotic therapy is used to treat Tularemia. Streptomyocin and Gentamicin are usually the first administered. Ciprofloxacin along with other fluoroquinolones. Tetracycline and chloramphenicol may also be used to treat Tularemia, however they have higher relapse rates than the previously mentioned.<br> | ||
Resistant to beta-lactam antibiotics and azithromycin.<br> | Resistant to beta-lactam antibiotics and azithromycin.<br> | ||
== Diagnostic Tests/Lab Tests/Lab Values<ref name="CIDRAP">CIDRAP. Tularemia: Current, comprehensive information on pathogenesis, microbiology, epidemiology, diagnosis, treatment, and prophylaxis. http://www.cidrap.umn.edu/cidrap/content/bt/tularemia/biofacts/tularemiafactsheet.html. Updated March 16, 2010. Accessed February 2011.</ref><ref name="B" /> == | == Diagnostic Tests/Lab Tests/Lab Values<ref name="CIDRAP">CIDRAP. Tularemia: Current, comprehensive information on pathogenesis, microbiology, epidemiology, diagnosis, treatment, and prophylaxis. http://www.cidrap.umn.edu/cidrap/content/bt/tularemia/biofacts/tularemiafactsheet.html. Updated March 16, 2010. Accessed February 2011.</ref><ref name="B" /> == | ||
There are numerous ways to test for F. tularensis:<br>• Gold Standard: Bacteriologic Culture<ref name="F" /><br>• Most Common: Serology<ref name="F" /><br>• | There are numerous ways to test for F. tularensis:<br>• Gold Standard: Bacteriologic Culture<ref name="F" /><br>• Most Common: Serology<ref name="F" /><br>• Polymerase Chain Reaction of sample ulcer<br>• Direct Stains<br>• Blood Culture<br>• Direct Fluorescent Antibody Stain<br>• Slide Agglutination<br>• Antimicrobial Susceptibility<br>• Biochemical Identification<br>• Enviornmental Specimen Evaluation<br>• Chest X-ray<br><br> | ||
[[Image:Beaver.jpg|left|Beaver]] | |||
== Etiology/Causes <ref name="F" /> == | |||
Direct transmission occurs from direct contact with the infected animal or direct contact from soil, water, or landscape. This may be from ingestion of contaminated meat (most likely rabbit), water, or inhaled dust. It can also be passed from handling or skinning contaminated animals or from a bite/scrath from a contaminated animal. Animal hosts that may spread Tularemia include lagomorphs (rabbit and hare), rodents, insectivores, carnivores, ungulates, marsupials, birds, amphibians, fish, and invertebrates. Secondary carriers include ticks, mosquitoes, biting flies or deerfly. With such a wide variety of hosts and carriers available of this disease, it is has the possibility to appear/outbreak in other regions. | |||
[[Image:Rabbit.jpg|right|http://www.wormsandgermsblog.com/tags/tularemia/]][[Image:Tick's.jpg|center|http://www.mybwmc.org/library/2/19660]] | |||
== Systemic Involvement <ref name="CIDRAP" />,<ref name="B" /> == | |||
*Supporation of local lymph nodes | |||
*2<sup>o</sup> Pneumonia | |||
*Hematogenous Spread to other organs resulting in: | |||
Pericarditis | |||
Osteomyelitis | |||
Meningitis | |||
Sepsis | |||
Hepatitis/Jaundice | |||
Splenic Rupture | |||
Encephalitis | |||
Peritonitis | |||
*Renal Failure | |||
*Rhabomyolisis (typhoidal form) | |||
*ARDS (penumonic form) | |||
*Lung Abscess (pneumonic form) | |||
*Fibrosis/Calcification of affected lung areas (pneumonic form) | |||
*Pleuritis (pneumonic form) | |||
<br> | |||
With all forms of Tularmemia illness MAY result in such debilitating conditions (more so when other systems are involved), that recovery can take several months. | |||
| |||
== Medical Management (current best evidence) == | == Medical Management (current best evidence) == | ||
Antimicrobials are currently the best treatment option for Tularemia infections. | Antimicrobials are currently the best treatment option for Tularemia infections. After beginning treatment one should expect to see an improvement in symptoms and fever within 24-48 hours.<ref name="CIDRAP" /><br> | ||
*'''Aminoglycosides<ref name="A" />''' | *'''[http://www.drugs.com/drug-class/aminoglycosides.html Aminoglycosides]<ref name="A" />''' | ||
* | *Streptomyocin 10-14 days (1st choice) | ||
*May also be treated with gentamicin or | *May also be treated with [http://www.drugs.com/mtm/gentamicin.html gentamicin] or [http://www.drugs.com/tetracycline.html tetracycline] for 14+ days | ||
Tetracycline should not be used as a treatment in those whose permanent teeth have not came in.<ref name="B">Tularemia. PubMed Health. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001859/. Updated March 17,2009. Accessed February 19, 2011.</ref> | Tetracycline should not be used as a treatment in those whose permanent teeth have not came in.<ref name="B">Tularemia. PubMed Health. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001859/. Updated March 17,2009. Accessed February 19, 2011.</ref> | ||
*'''Quinolones''' | *[http://www.drugs.com/drug-class/quinolones.html '''Quinolones'''] | ||
*Contraindicated in those < 18 years of age | *Contraindicated in those < 18 years of age | ||
*"well tolerated, achieve adequate blood levels...and have excellent intracellular penetration"<ref name="Treatment of">Limaye AP, Hooper CJ. Treatment of tularemia with flouroquinolones: two cases and review. Clinical Infectious Diseases. 1999;29:922-924. http://www.ncbi.nlm.nih.gov/pubmed/10589911. Accessed February 2011.</ref> | *"well tolerated, achieve adequate blood levels...and have excellent intracellular penetration"<ref name="Treatment of">Limaye AP, Hooper CJ. Treatment of tularemia with flouroquinolones: two cases and review. Clinical Infectious Diseases. 1999;29:922-924. http://www.ncbi.nlm.nih.gov/pubmed/10589911. Accessed February 2011.</ref> | ||
| Line 80: | Line 149: | ||
<br> | <br> | ||
A review of 10 documented treatment cases in the United States found that those treated with Aminoglycosides have a 6-12% relapse rate of infection, while those treated with Quinolones had a 0% relapse rate.<ref name="Treatment of" /> | A review of 10 documented treatment cases in the United States found that those treated with Aminoglycosides have a 6-12% relapse rate of infection, while those treated with Quinolones had a 0% relapse rate.<ref name="Treatment of" /> | ||
== Physical Therapy Management (current best evidence) == | == Physical Therapy Management (current best evidence) == | ||
Currently did not come across any management in | Currently did not come across any management in regards to physical therapy. | ||
Points to consider: | |||
*Pt's with tularemia present with generalized musculoskeletal aches. | |||
*Pt's who have complications develop 2<sup>o</sup> to their primary Tularemia infection may take months to recover. During this time physical therapy may play a roll in conditioning,balance retraining, rebuilding strength and endurance, and regaining patient's independence in their functional roles in society and home.<br> | |||
== Differential Diagnosis == | == Differential Diagnosis == | ||
'''Alternative Diagnosis''' | |||
Differential Characteristics to rule out Tularemia | |||
<br> | |||
=== Glandular<ref name="CIDRAP" /> === | |||
*'''Bubonic Plague''' [[Image:Lymph node.jpg|right|300x300px|http://www.nzma.org.nz/journal/120-1248/2403/]] | |||
Systemic toxicity | |||
*'''Cat-Scratch Disease''' | |||
History of cat scratch | |||
Takes weeks to develop | |||
*'''Myobacterial Infection''' | |||
Lymph Nodes painless/non-tender | |||
*'''Sporotrichosis''' | |||
No systemic symptom | |||
Lymph nodes painless | |||
History of contact w/ soil/plants | |||
Lesions along lymphatic chains | |||
*'''Streptococcal''' | |||
*'''Lymphogranuloma Venereum''' | |||
Adenitis in genital lymph chains only | |||
*'''Primary Genital Herpes''' | |||
Adenitis in genital lymph chains only | |||
*'''Secondary Syphilis''' | |||
Enlarged lymph nodes in inguinal region only | |||
=== Ulceroglandular<ref name="CIDRAP" /> === | |||
*'''Anthrax''' | |||
Painless ulcer --> black eschar; non-pitting edema around lesion | |||
*'''Orf''' | |||
Pustule that progresses to weeping nodule [[Image:Forearm ulcer.jpg|right|250x250px|http://www.upmc-biosecurity.org/website/focus/agents_diseases/fact_sheets/tularemia.html]] | |||
*'''Pasteurella infections''' | |||
History of dog/cat bite or licking of open wound | |||
*'''Primary Syphillis''' | |||
Painless ulcer at genital site | |||
*'''Ricketsialpox''' | |||
Painless papule --> black eschar; maculopapular rash in 2-3 days | |||
*'''Scrub Typhus''' | |||
Maculopapular rash; Infection from chigger bites | |||
*'''Staphylococcal/Stretococcal Cellulitis''' | |||
History of trauma or pre-existing lesion | |||
=== Pneumonic <ref name="CIDRAP" /> === | |||
*'''Community Acquired Pneumonia[[Image:Chest X-ray.jpg|right|300x650px|http://cchealth.org/topics/bioterrorism/providers/how_to_recognize.php]]''' | |||
Won't cure with conventional antibiotic therapy | |||
*'''Inhalation of Anthrax''' | |||
Often fulminant | |||
*'''Pneumonic Plague''' | |||
Consolidation on Chest X-ray | |||
Often Fulminant | |||
*'''Q Fever''' | |||
Exposure to sheep, goat, cattle, cat<br> | |||
Difficult to differentiate from Tularemia<br> | |||
*'''Tuberculosis''' | |||
More common in elderly and those living in close living quarters | |||
(shelters,jails,schools etc...) | |||
*'''Viral Pneumonia''' | |||
Recent cruise or trip to tropics | |||
Exposure to feces/urine of mice | |||
*'''Respiratory Syncytial Virus''' | |||
More common in children during Winter and Spring<br> | |||
*'''Cytomegalovirus''' | |||
=== Oculoglandular <ref name="CIDRAP" /> === | |||
*'''Adenoviral Infection''' | |||
*'''Cat-Scratch Disease''' | |||
*'''Coccidiodomycosis''' | |||
*'''Herpes Infection''' | |||
*'''Pyogenic Bacterial Infections''' | |||
*'''Sporotrichosis''' | |||
*'''Syphilis''' | |||
*'''Tuberculosis''' | |||
=== Oropharyngeal <ref name="CIDRAP" /> === | |||
*'''Streptococcal Pharyngitis''' | |||
*'''Infections Mononucleosis''' | |||
*'''Adenoviral Infection''' | |||
*'''Diptheria''' | |||
=== Typhoidal <ref name="CIDRAP" /> === | |||
*'''Brucellosis''' | |||
*'''Disseminated Mycobacterial/Fungal Infection''' | |||
*'''Endocarditis''' | |||
*'''Leptspirosis''' | |||
*'''Pontiac Fever''' | |||
*'''Malaris''' | |||
*'''Q Fever''' | |||
*'''Typhoid Fever''' | |||
== Case Reports/ Case Studies == | == Case Reports/ Case Studies == | ||
| Line 100: | Line 312: | ||
Tularemia: Emergency department presentation of an infrequently recognized disease.<ref name="ER Dept.">Harrell RE, Whitaker GR. Tularemia: Emergency department presentation of an infrequently recognized disease. Am J Emerg Med. 1985;3:415-418. http://www.sciencedirect.com/science?_ob=ArticleURL&_udi=B6W9K-4C4FJTF-GS&_user=10&_coverDate=09%2F30%2F1985&_rdoc=1&_fmt=high&_orig=gateway&_origin=gateway&_sort=d&_docanchor=&view=c&_rerunOrigin=google&_acct=C000050221&_version=1&_urlVersion=0&_userid=10&md5=8437c09158b0597f13c1896c220c972e&searchtype=a. Accessed February 2011.</ref><br> | Tularemia: Emergency department presentation of an infrequently recognized disease.<ref name="ER Dept.">Harrell RE, Whitaker GR. Tularemia: Emergency department presentation of an infrequently recognized disease. Am J Emerg Med. 1985;3:415-418. http://www.sciencedirect.com/science?_ob=ArticleURL&_udi=B6W9K-4C4FJTF-GS&_user=10&_coverDate=09%2F30%2F1985&_rdoc=1&_fmt=high&_orig=gateway&_origin=gateway&_sort=d&_docanchor=&view=c&_rerunOrigin=google&_acct=C000050221&_version=1&_urlVersion=0&_userid=10&md5=8437c09158b0597f13c1896c220c972e&searchtype=a. Accessed February 2011.</ref><br> | ||
Treatment of tularemia with fluoroquinolones: two cases and review.<ref name="Treatment ">Limaye AP, Hooper CJ. Treatement of tularemia with fluoroquinolones: Two cases and review. Clinical Infectious Diseases. | Treatment of tularemia with fluoroquinolones: two cases and review.<ref name="Treatment">Limaye AP, Hooper CJ. Treatement of tularemia with fluoroquinolones: Two cases and review. Clinical Infectious Diseases. 1999;29:922-924.http://www.ncbi.nlm.nih.gov/pubmed/10589911. Accessed February 2011.</ref><br> | ||
== Resources | == Resources == | ||
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001859/ | |||
http://emergency.cdc.gov/agent/tularemia/faq.asp | |||
http://www.cdc.gov/tularemia/index.html | |||
== References == | == References == | ||
<references /> | |||
<references /> | |||
[[Category:Bellarmine_Student_Project]] | [[Category:Bellarmine_Student_Project]] | ||
Latest revision as of 08:29, 6 March 2020
Original Editors - Dana Collins from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Dana Collins, Elaine Lonnemann, Admin, Kim Jackson, Wendy Walker, WikiSysop, Lucinda hampton and 127.0.0.1
Definition/Description[edit | edit source]
Tularemia, named after the infectious gram-negative bacterium Francisella tularensis, is a zoonotic disease. A zoonotic disease is one that is spread from animal to human (infected humans can NOT pass the disease to other humans). This spread may be directly i.e. handling contaminated meat or through a carrier i.e. a tick. It is also known as “Ohara’s disease”, “rabbit fever”, “deer-fly fever”,[1] “market’s men disease”, “meat-cutter’s disease”, “glandular type of tick fever”, “water rat-trappers’ disease”. It is highly infectious, <10 organisms causing severe disease in both humans and animals.[2] There are 4 sub-types of the bacterium, the most common in the United States are Type A, tularenis, and Type B, holarctica. It is on the Center for Disease Control’s list of bioterroism threats.
Prevalence[edit | edit source]
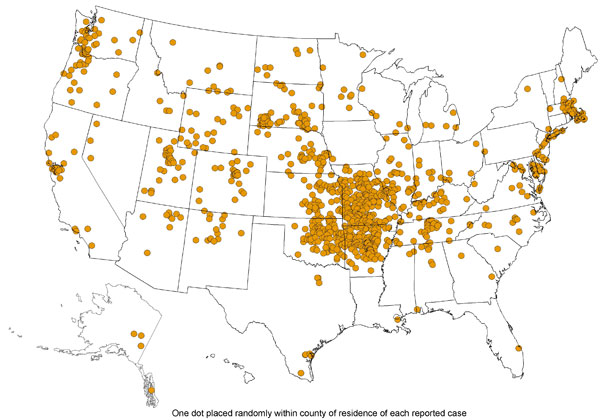
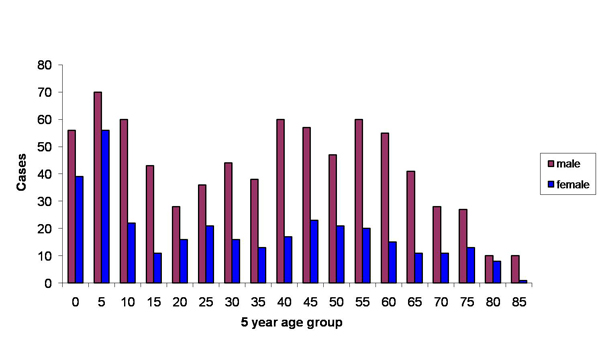
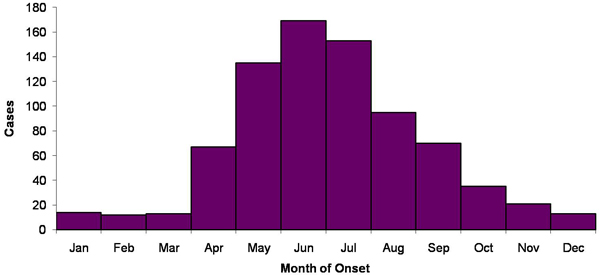
The prevalence of Tularemia in the United States depends on the geographical location and the time of year. During the spring and summer months (May-September), there is a rise in reported cases. South-Central, Pacific Northwest, and parts of the East Coast have the highest incidence of Tularemia. While the population most effected is young males 5-9 years old and those > 75 years old.[3]
The above images from: http://www.cdc.gov/tularemia/statistics/.
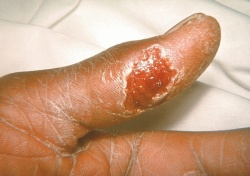
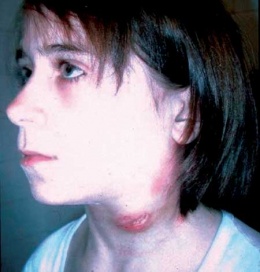
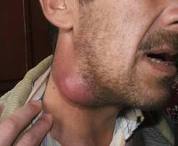
Characteristics/Clinical Presentation[4][5][6][3][1][edit | edit source]
|
|
|
Note: The 2 most common forms are glandular/ulcerglandular and pneumonic.
Those occurring in ≥25% of those infected with the glandular and ulceroglandular form are in bold[4]
Those occurring in ≥25% of those infected with the pneumonic form are in italics[4]
Expectations/Prognosis[5][edit | edit source]
Untreated: Fatality ~5%
Treated: Fatality <1%
Poor outcomes have been associated with those who have underlying co-morbidities such as alcoholism or diabetes and those who delay seeking medical treatment.[4]
Medications[4][edit | edit source]
Antibiotic therapy is used to treat Tularemia. Streptomyocin and Gentamicin are usually the first administered. Ciprofloxacin along with other fluoroquinolones. Tetracycline and chloramphenicol may also be used to treat Tularemia, however they have higher relapse rates than the previously mentioned.
Resistant to beta-lactam antibiotics and azithromycin.
Diagnostic Tests/Lab Tests/Lab Values[4][5][edit | edit source]
There are numerous ways to test for F. tularensis:
• Gold Standard: Bacteriologic Culture[2]
• Most Common: Serology[2]
• Polymerase Chain Reaction of sample ulcer
• Direct Stains
• Blood Culture
• Direct Fluorescent Antibody Stain
• Slide Agglutination
• Antimicrobial Susceptibility
• Biochemical Identification
• Enviornmental Specimen Evaluation
• Chest X-ray
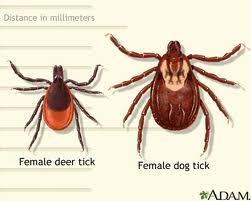
Etiology/Causes [2][edit | edit source]
Direct transmission occurs from direct contact with the infected animal or direct contact from soil, water, or landscape. This may be from ingestion of contaminated meat (most likely rabbit), water, or inhaled dust. It can also be passed from handling or skinning contaminated animals or from a bite/scrath from a contaminated animal. Animal hosts that may spread Tularemia include lagomorphs (rabbit and hare), rodents, insectivores, carnivores, ungulates, marsupials, birds, amphibians, fish, and invertebrates. Secondary carriers include ticks, mosquitoes, biting flies or deerfly. With such a wide variety of hosts and carriers available of this disease, it is has the possibility to appear/outbreak in other regions.
Systemic Involvement [4],[5][edit | edit source]
- Supporation of local lymph nodes
- 2o Pneumonia
- Hematogenous Spread to other organs resulting in:
Pericarditis
Osteomyelitis
Meningitis
Sepsis
Hepatitis/Jaundice
Splenic Rupture
Encephalitis
Peritonitis
- Renal Failure
- Rhabomyolisis (typhoidal form)
- ARDS (penumonic form)
- Lung Abscess (pneumonic form)
- Fibrosis/Calcification of affected lung areas (pneumonic form)
- Pleuritis (pneumonic form)
With all forms of Tularmemia illness MAY result in such debilitating conditions (more so when other systems are involved), that recovery can take several months.
Medical Management (current best evidence) [edit | edit source]
Antimicrobials are currently the best treatment option for Tularemia infections. After beginning treatment one should expect to see an improvement in symptoms and fever within 24-48 hours.[4]
- Aminoglycosides[1]
- Streptomyocin 10-14 days (1st choice)
- May also be treated with gentamicin or tetracycline for 14+ days
Tetracycline should not be used as a treatment in those whose permanent teeth have not came in.[5]
- Quinolones
- Contraindicated in those < 18 years of age
- "well tolerated, achieve adequate blood levels...and have excellent intracellular penetration"[6]
A review of 10 documented treatment cases in the United States found that those treated with Aminoglycosides have a 6-12% relapse rate of infection, while those treated with Quinolones had a 0% relapse rate.[6]
Physical Therapy Management (current best evidence)[edit | edit source]
Currently did not come across any management in regards to physical therapy.
Points to consider:
- Pt's with tularemia present with generalized musculoskeletal aches.
- Pt's who have complications develop 2o to their primary Tularemia infection may take months to recover. During this time physical therapy may play a roll in conditioning,balance retraining, rebuilding strength and endurance, and regaining patient's independence in their functional roles in society and home.
Differential Diagnosis[edit | edit source]
Alternative Diagnosis
Differential Characteristics to rule out Tularemia
Glandular[4][edit | edit source]
- Bubonic Plague
Systemic toxicity
- Cat-Scratch Disease
History of cat scratch
Takes weeks to develop
- Myobacterial Infection
Lymph Nodes painless/non-tender
- Sporotrichosis
No systemic symptom
Lymph nodes painless
History of contact w/ soil/plants
Lesions along lymphatic chains
- Streptococcal
- Lymphogranuloma Venereum
Adenitis in genital lymph chains only
- Primary Genital Herpes
Adenitis in genital lymph chains only
- Secondary Syphilis
Enlarged lymph nodes in inguinal region only
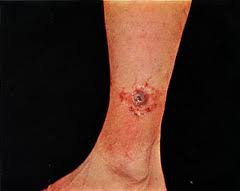
Ulceroglandular[4][edit | edit source]
- Anthrax
Painless ulcer --> black eschar; non-pitting edema around lesion
- Orf
Pustule that progresses to weeping nodule
- Pasteurella infections
History of dog/cat bite or licking of open wound
- Primary Syphillis
Painless ulcer at genital site
- Ricketsialpox
Painless papule --> black eschar; maculopapular rash in 2-3 days
- Scrub Typhus
Maculopapular rash; Infection from chigger bites
- Staphylococcal/Stretococcal Cellulitis
History of trauma or pre-existing lesion
Pneumonic [4][edit | edit source]
- Community Acquired Pneumonia
Won't cure with conventional antibiotic therapy
- Inhalation of Anthrax
Often fulminant
- Pneumonic Plague
Consolidation on Chest X-ray
Often Fulminant
- Q Fever
Exposure to sheep, goat, cattle, cat
Difficult to differentiate from Tularemia
- Tuberculosis
More common in elderly and those living in close living quarters
(shelters,jails,schools etc...)
- Viral Pneumonia
Recent cruise or trip to tropics
Exposure to feces/urine of mice
- Respiratory Syncytial Virus
More common in children during Winter and Spring
- Cytomegalovirus
Oculoglandular [4][edit | edit source]
- Adenoviral Infection
- Cat-Scratch Disease
- Coccidiodomycosis
- Herpes Infection
- Pyogenic Bacterial Infections
- Sporotrichosis
- Syphilis
- Tuberculosis
Oropharyngeal [4][edit | edit source]
- Streptococcal Pharyngitis
- Infections Mononucleosis
- Adenoviral Infection
- Diptheria
Typhoidal [4][edit | edit source]
- Brucellosis
- Disseminated Mycobacterial/Fungal Infection
- Endocarditis
- Leptspirosis
- Pontiac Fever
- Malaris
- Q Fever
- Typhoid Fever
Case Reports/ Case Studies[edit | edit source]
Isolation of Francisella tularensis from blood.[7]
Tularemia: Emergency department presentation of an infrequently recognized disease.[8]
Treatment of tularemia with fluoroquinolones: two cases and review.[9]
Resources[edit | edit source]
http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001859/
http://emergency.cdc.gov/agent/tularemia/faq.asp
http://www.cdc.gov/tularemia/index.html
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Wilson M, Lountzis N, Ferringer T. Zoonoses of dermatologic interest. Dermatologic Therapy. 2009;22:367-378. http://onlinelibrary.wiley.com/doi/10.1111/j.1529-8019.2009.01248.x/abstract. Accessed February 2011.
- ↑ 2.0 2.1 2.2 2.3 Petersen JM, Schriefer ME. Tularemia: emergence/re-emergence. Vet Res. 2005;36:455-467. http://digitalcommons.unl.edu/cgi/viewcontent.cgi?article=1031&context=zoonoticspub&sei-redir=1#search=%22Petersen+JM,+Schriefer+ME.+Tularemia:+emergence/re-emergence.%22. Accessed February 2011.
- ↑ 3.0 3.1 Hayes E, Marshall S, Dennis D. Tualremia--United States,1990-2000. www.cdc.gov/mmwr/preview/mmwrhtml/mm5109a1.htm. February 20, 2011.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 CIDRAP. Tularemia: Current, comprehensive information on pathogenesis, microbiology, epidemiology, diagnosis, treatment, and prophylaxis. http://www.cidrap.umn.edu/cidrap/content/bt/tularemia/biofacts/tularemiafactsheet.html. Updated March 16, 2010. Accessed February 2011.
- ↑ 5.0 5.1 5.2 5.3 5.4 Tularemia. PubMed Health. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001859/. Updated March 17,2009. Accessed February 19, 2011.
- ↑ 6.0 6.1 6.2 Limaye AP, Hooper CJ. Treatment of tularemia with flouroquinolones: two cases and review. Clinical Infectious Diseases. 1999;29:922-924. http://www.ncbi.nlm.nih.gov/pubmed/10589911. Accessed February 2011.
- ↑ Provenza JM, Klotz SA, Penn RL. Isolation of francisella tularenis from blood. Journal of Clinical Microbiology. 1986;24:453-455. http://jcm.asm.org/cgi/content/short/24/3/453. Accessed February 2011.
- ↑ Harrell RE, Whitaker GR. Tularemia: Emergency department presentation of an infrequently recognized disease. Am J Emerg Med. 1985;3:415-418. http://www.sciencedirect.com/science?_ob=ArticleURL&_udi=B6W9K-4C4FJTF-GS&_user=10&_coverDate=09%2F30%2F1985&_rdoc=1&_fmt=high&_orig=gateway&_origin=gateway&_sort=d&_docanchor=&view=c&_rerunOrigin=google&_acct=C000050221&_version=1&_urlVersion=0&_userid=10&md5=8437c09158b0597f13c1896c220c972e&searchtype=a. Accessed February 2011.
- ↑ Limaye AP, Hooper CJ. Treatement of tularemia with fluoroquinolones: Two cases and review. Clinical Infectious Diseases. 1999;29:922-924.http://www.ncbi.nlm.nih.gov/pubmed/10589911. Accessed February 2011.