Vulvar Cancer
Original Editor - Khloud Shreif
Top Contributors - Khloud Shreif and Sehriban Ozmen
Introduction[edit | edit source]
Vulvar cancer is an uncommon malignancy and the fourth most common gynecologic cancer[1] that usually affects post-menopausal women, and it can be misdiagnosed and considered an inflammatory condition so it is important to be familiar with vulvar malignancies. It forms a mass or ulcer on the vulva and usually causes itching. The incidence of vulvar cancer is increasing in the last decades. The two main categories of vulvar cancer; human papillomavirus (HPV) dependant vulvar cancer that is common in younger women, and independant HPV that is found in women after menopause[2]. It may spread to lymph nodes, or to nearby structures.
Anatomy Background[edit | edit source]
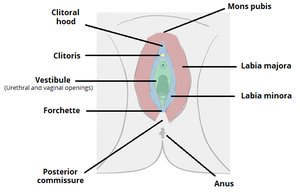
The vulva refers to the outer part of the external female genitalia, it includes the entrance to the vagina and the internal reproductive tract in addition to the urethra opening. It forms from labia majora (outer lips), labia minora (inner lips), and clitoris.
Vulval Warts are a growth of epithelium caused by HPV infection and usually transmitted between sexual partners but they do not develop tinto cancer.
Incidence[edit | edit source]
The incidence of vulvar cancer has increased by an average of 4.6% every 5 years in the last decades, in 2018 there was about 1200 reported case of death because of vulvar cancer. Vulvar squamous cell carcinoma is the most common vulvar cancer and represents about 90% of all vulvar cancer and occurs in 2-7 of every 100,000 women, the second most is vulvar melanoma representing about 5%-10% of all vulvar malignancies[3].
Histological Types[edit | edit source]
Vulvar squamous cell carcinoma (VSCC)
Also referred to as vulvar intraepithelial neoplasia VIN, divided into; usual-type VIN or vulvar high-grade squamous intraepithelial lesions (HSILs), it is associated with HPV infection more common in young, and has a higher risk of progress to invasive squamous cell carcinoma (SCC) but it is slowly progrss, and tends to be multifocal. the second type is differentiated VIN (dVIN) it is not HPV dependant and with a higher recurrence rate, worse prognosis, and rapid progression to invasive VSCC[3][1].
Vulvar melanoma
It is the second most common vulvar cancer, starts on the skin of the vulva, most commonly to be found in the labia majora and clitoral area, and most common in white women usually starting in their 5th to 7th decades of life. The area is sun- protected so, the genetic studies suggest it is more similar to what happens in acral lentiginous melanoma, the melanocytes in the skin become malignant and the tumor continues to grow and spread until surgical excision of the tumor. The lesion color may be black, white, pink, red, or other colors[1][3].
Vulvar basal cell carcinoma (BCC)
It represents only about 2%-4% of all vulvar cancers, with a good prognosis and low risk to develop metastasis. Chronic irritation, pelvic radiation, immunosuppression, or trauma might be risk factors to develop BCC. The lesion may be pigmented and the majority of BCC treated with surgical excision. There is also vulvar extramammary Paget disease which is rare to present in cases[3].
Clinical Presentataion[edit | edit source]
- Pruritus, burning, pain, or bleeding for invasive type.
- The lesion is flat and ulcerated for SCC, or nodule, papule with irregular borders and coloration in vulvar melanoma.
- The skin may be white, erythematous, or pigmented.
- Symptoms of VBCC if present are nonspecific symptoms including irritation, discomfort, pain, ulceration, or bleeding.
Risk factors[edit | edit source]
- Immunosuppression.
- Smoking.
- History of cervical cancer.
- Aging is considered a risk factor.
- HPV infection.
Staging of Vulvar Cancer[edit | edit source]
Surgical staging of vulvar cancer according to FIGO 2021[1].
| Stage | Description | |
|---|---|---|
| I | Tumor confined to the vulva | |
| IA | Tumor size ≤2 cm and stromal invasion ≤1 mma | |
| IB | Tumor size >2 cm or stromal invasion >1 mma | |
| II | Tumor of any size with extension to lower one-third of the urethra, lower one-third of the vagina, lower one-third of the anus with negative nodes. | |
| III | Extension to upper part of adjacent perineal structures, or with any number of nonfixed, nonulcerated lymph node | |
| IIIA | Tumor of any size with disease extension to upper two-thirds of the urethra, upper two-thirds of the vagina, bladder mucosa, rectal mucosa, or regional lymph node metastases ≤5 mm. | |
| IIIB | Regionalb lymph node metastases >5 mm | |
| IIIC | Regionalb lymph node metastases with extracapsular spread | |
| IV | Fixed to bone, or fixed, ulcerated lymph node metastases, or distant metastases | |
| IVA | Disease fixed to pelvic bone, or fixed or ulcerated regionalb lymph node metastases. | |
| IVB | Distant metastases[1] | |
Histological grades
- G0: cannot be assessed
- G1: Well differentiated
- G2: Moderately differentiated
- G3: Poorly or undifferentiated
Management[edit | edit source]
It is important the treatment is individualized according to the patient and it should include psychosexual counseling services along with a multidisciplinary team. The treatment depends on the patient's general status, any associated co morbidities, the age of the patient, and the histology and grade of the tumor.
The vulvar medical treatment may include one or more of the following:
- Surgical excision of the tumor mmargins it may extend to lymph nodes excision. The excision of vulvar tumor is considere the gold standard for early management for vulvar tumor. For example; radical wide local excision, in which groin node excision is not necessary it demonstrated a decrease in the psychosexual morbidity than radical vulvectomy[5]. Plastic surgery is recommended after surgical excision for extensive vulvar cancer[2].
- Radiation therapy, external beam radiotherapy (EBRT).
- Chemotherapy, according to the analysis of the National Cancer Data Base (NCDB) in 2015 suggested that women with lymphnode-positive vulvar cancer benefitted the most from the addition of chemotherapy to radiation[6].
If lympnode is suspected it is importanrt to first do a biopsy of the node, pelvic CT or MRI to detect the extent of the spread in this case radiotherapy or chemoradiotherapy to the groin and pelvis should be offered for early-stage disease[7].
Physical Therapy management[edit | edit source]
The physical therapy role with patients with cancer pre or post-treatment concentrates on improving their quality of life QoL, and helping them to continue their ADL without fatigue or exhaustion. Cancer rehabilitation
will concentrate on exercise therapy, pain management, radiotherapy, and chemotherapy side effects.
Lymphoedema management / complete decongestive therapy.
Pelvic floor physiotherapy intervention is important after surgery, chemotherapy, or radiotherapy it helpes to improve sexual function, power and health-related quality incontinence, incontince, and restore pelvic floor muscles function. Our physiotherapy role will iclude; patient education, manual physical therapy techniques, biofeedback, pelvic floor muscle training, general exercise programme, and home training programme[8].
Resources[edit | edit source]
Treating vulvar cancer, American Cancer Society.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Olawaiye AB, Cuello MA, Rogers LJ. Cancer of the vulva: 2021 update. International Journal of Gynecology & Obstetrics. 2021 Oct;155:7-18.
- ↑ 2.0 2.1 Alkatout I, Schubert M, Garbrecht N, Weigel MT, Jonat W, Mundhenke C, Günther V. Vulvar cancer: epidemiology, clinical presentation, and management options. International journal of women's health. 2015;7:305.
- ↑ 3.0 3.1 3.2 3.3 Tan A, Bieber AK, Stein JA, Pomeranz MK. Diagnosis and management of vulvar cancer: A review. Journal of the American Academy of Dermatology. 2019 Dec 1;81(6):1387-96.
- ↑ The Medical Education. Gyn Vaginal Vulvar Cancer The Medical Education . Available from: http://www.youtube.com/watch?v=XRdEjDiy9HY[last accessed 5/7/2022]
- ↑ Dellinger TH, Hakim AA, Lee SJ, Wakabayashi MT, Morgan RJ, Han ES. Surgical management of vulvar cancer. Journal of the National Comprehensive Cancer Network. 2017 Jan 1;15(1):121-8.
- ↑ Gill BS, Bernard ME, Lin JF, Balasubramani GK, Rajagopalan MS, Sukumvanich P, Krivak TC, Olawaiye AB, Kelley JL, Beriwal S. Impact of adjuvant chemotherapy with radiation for node-positive vulvar cancer: A National Cancer Data Base (NCDB) analysis. Gynecologic oncology. 2015 Jun 1;137(3):365-72.
- ↑ Gaffney DK, King B, Viswanathan AN, Barkati M, Beriwal S, Eifel P, Erickson B, Fyles A, Goulart J, Harkenrider M, Jhingran A. Consensus recommendations for radiation therapy contouring and treatment of vulvar carcinoma. International Journal of Radiation Oncology* Biology* Physics. 2016 Jul 15;95(4):1191-200.
- ↑ Brennen R, Lin KY, Denehy L, Frawley HC. The effect of pelvic floor muscle interventions on pelvic floor dysfunction after gynecological cancer treatment: A systematic review. Physical therapy. 2020 Aug 12;100(8):1357-71.