Use of Hydrotherapy for the Management of Ankylosing Spondylitis (AS)
Introduction to Ankylosing Spondylitis[edit | edit source]
What is Ankylosing Spondylitis (AS)?[edit | edit source]
Ankylosing Spondylitis (also known as Radiographic Axial Spondyloarthritis) is a chronic inflammatory, sero-negative arthritic condition that typically affects the spine and the sacroilliac (SI) joints. Common clinical presentations of this disease can include: [1]
- Inflammatory nature of chronic back pain which improves with exercise
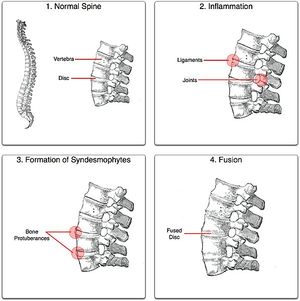
- SI joint and spinal fusions
- Formation of bony spurs and syndesmophytes along the intervertebral and SI joint
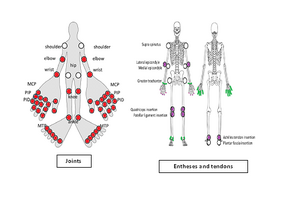
- Arthritis and enthesitis (typically asymmetrical distribution within the lower limb)
- Dactylitis (swelling of toes and fingers)
- Extra-articular manifestations (anterior uveitis, psoriasis, IBS etc.)
- Increased risk of osteoporosis and spinal fractures
- Early onset compared to mechanical back pain
- Morning Stiffness (>30 minutes)
- Intermittent difficulties with breathing due to reduced chest excursion [2]
- Reduced Quality-of-Life [3]
Common features that differentiate between mechanical back pain and inflammatory back pain are listed below.[4]
| Inflammatory Back Pain (AS) | Mechanical Back Pain |
| Age of onset typically below 40 years | Age of onset at any age |
| Insidious onset; less likely to be acute | Variable onset; may be acute |
| Pain does not improve with rest | Pain often improves with rest (particularly in acute stage) |
| Pain improves with exercise | |
| Morning stiffness for more than 30 minutes | |
| Pain at night which may cause patient to wake up (particularly in the latter half of the night) |
Aetiology[edit | edit source]
Although the aetiology of AS has currently no confirmed specific causes, [5] current evidence point to genetic markers and environmental changes that result in the development of AS in individuals.
Pathogenesis - Genetic[edit | edit source]
There appears to be a strong genetic pre-disposition in the development of AS. The most commonly associated genetic factor is the HLA-B27 allele.
The human leukocyte antigen (HLA) complex, also known as human major histocompatibility (MHC) complex, belongs to cell-surface proteins that helps in the process of acquired immunity. The MHC gene family is divided into subgroups: class I, II, and III.[1]
HLA-A, HLA-B, and HLA-C are encoded by the MHC class I complex and is found on all nucleated human cells and platelets. MHC class I complex is polymorphic in nature and links 8–10 amino acids (peptide) to initiate and propagate a series of immune responses. The HLA-B27 belonging to the MHC class I surface protein complex and encoded by the MHC B gene on chromosome 6. [1] Having HLA-B27 typically predisposes an individual to AS. HLA-B27 presents peptide antigens to T-cells within the human body as a defense mechanism and is widely considered to be significantly linked to inflammatory diseases such as AS with about 90 to 95% of people suffering with AS displaying a positive HLA-B27 allele. [6]
The pathogenic role of HLA-B27 currently remains disputed and unclear. Three theories accounting for the role of HLA-B27 in AS have been put forth.
- The arthritogenic peptide: HLA-B27 is critical in the pathogenesis of joint-specific peptides to CD8+ cytotoxic T cells. However, there has been lack of identification of any specific arthritogenic peptide thus far.[6]
- Misfolding of HLA-B27: It is hypothesised that misfolding of the HLA-B27 causes a stress to the Endoplasmic Reticulum and activates an unfolded protein response (UPR). This causes an increased expression of the IL-23 in dendritic cells. [7] The role of the UPR in instigating the inflammation is yet to be proven.
- Cell-surface homodimers: It is thought that the HLA-B27 aberrantly folds to form homodimers on the surface of the cell. These different forms of HLA-B27 are identified in vitro by immunoglobulin-like receptors. These receptors can be express by Natural Killer (NK) cells or circulating CD4+ T cells. This induces the transcription of the Th17 transcription factor for the expression of the Th17 immune pathway.[8]
Pathogenesis - Environmental[edit | edit source]
K. pneumoniae has been suggested to trigger and perpetuate symptoms of AS. Involvement of the gastrointestinal tract in the pathogenesis of AS is proposed due to studies showing the presence of gut inflammation in up to 60% of people with AS. [9] Gut inflammation in people with AS has been a prognostic factor for AS due to the association with extensive bone marrow oedema within the sacroiliac joints. Recent studies show rheumatoid arthritis (RA), a HLA class II-associated autoimmune disease, having a strong correlation with the presence of such gut microbes and subsequent development of inflammation and damage to the joints.[10][11]
K. pneumoniae is a bacterium that is typically present within a normal gut microbiome, but at times can act as an opportunistic pathogen.
It has been suggested that higher antibody levels are found in people with AS and positive HLA-B27 in the presence of specific serotypes of the bacterium (K26, K36, K50). There has been mixed results on the correlation and association between AS and K. pneumoniae. As of current research, two proposed theories aim to explain the relation.[12]
- One-gene theory, HLB27 gene codes for a molecule that is stereo chemically similar to antigens found in certain microorganisms, resulting in infections that are responsible for tissue damage characterized in AS. [12]
- Two-gene theory, there is a separate susceptibility gene similar to HLA-B27 which produces Immune Response (IR) genes which code for specific antigens that instigate the body’s immune response. Defects to these set of genes result in a flawed immune reaction and cause increased susceptibility to AS. [12]
Common Sites of Inflammation[edit | edit source]
Common areas are attachment points between tendon/ligament, bone, and peripheral sites. Enthesis can cause pain, and swelling, and lead to changes such as fibrosis, and ossification at the affected sites.
Common sites include the costochondral joints, the iliac-spine, lumbar spinous process, and achilles tendon. [13] In axial joints, repeated synovitis and fibrosis can result in ankylosis of the axial joints. [1]
Intervertebral disc enthesitis can occur at the insertion of the annulus fibrosis, i.e. the protective outer layer of the intervertebral disc between each spinal vertebrae. This results in bony growth and formation originating inside a ligament (syndesmophytes).[1]
Further features such as "Romanus Lesions" form as a result of squaring of the superior and inferior borders of the vertebral bodies due to erosion. [14] Over time, longitudinal ligaments can ossify and fuse, forming typical late-stage AS features such as a "Bamboo Spine".[15]
Hydrotherapy[edit | edit source]
Hydrotherapy is the external or internal use of water in any of its form (water, ice, steam) for health promotion or treatment of various diseases with various temperatures, pressure, duration, site, and equipment. [16]
Types of Hydrotherapy[edit | edit source]
Simple Use of Running Water[edit | edit source]
The use of cold, running water has been used as first line of first aid treatment in emergency situations, including the treatment of burns, wound irrigation, acid injuries, and alkali spills. Applying cool running water for 20 mnutes within the first three hours of injury has been found to significantly decrease the odds of patients requiring skin grafting and surgical intervention for wound management after a burn injury. [17] Immediate irrigation with water for at least an hour (and even for several hours), has been suggested to be an important treatment -depending on the severity of the injury, it could be the most important intervention- after an isolated chemical burn. [18]
Wraps, Compresses, Packs and Fomentation[edit | edit source]
A common and easy-to-administer form of hydrotherapy is the use of wraps, compresses or external packs which have been soaked in warm or cold water, or even ice. These are then applied directly to the skin of the painful/warm area, such as cold water wrap use on the forehead to treat fever or ice pack application to swollen, painful injuries. [19]
Water Baths[edit | edit source]
Water baths are another form of hydrotherapy – warm water baths are a simple, accessible, and cheap option. With the addition of Epsom salts/minerals and essential oils, this treatment can both aid relaxation and cause an anti-inflammatory effect. Contrast bath therapy is another form of water bath therapy – it involves the patient initially being immersed in a hot water bath, and after a few minutes they are immediately immersed in a cold-water bath. The patient will continue to alternate between the different temperature baths whilst performing simple exercises to enhance the effects of the treatment. This rapid alternation between temperatures causes the blood vessels to dilate (in the hot bath) and constrict (in the cold bath) which effectively increases blood circulation. [20]
Sitz Baths[edit | edit source]
Sitz baths involve using a warm, shallow bath – chemicals such as povidone (iodine with antibacterial properties) may also be added. The patient then squats or sits down to submerge their perineum in the bath. The warm water encourages blood circulation in the perineum region, this acts as pain relief as well as promotes healing. Sitz baths are used to treat various conditions such as haemorrhoids as well as post-surgery treatment for the vulva/vagina, hemorrhoids, or after childbirth. These baths can also be used to treat different parts of the body with the same treatment principles. [21]
Saunas[edit | edit source]
The use of a sauna is another form of hydrotherapy, which uses a small heated room filled with wet steam or dry heat. This causes the patient to perspire and sweat out toxins in the process. [22] The positive effects of sauna, when combined with exercise, on cardiovascular function have been demonstrated in the general population. [23] Despite potential health benefits on AS, more data are required on the optimal frequency and duration of distinct types of sauna bathing for targeted health effects and the specific clinical populations who are most likely to benefit. [24]
Aquatic Therapy[edit | edit source]
Aquatic therapy involves the application of therapeutic exercises in water environments, such as a pool. The water is often heated to 26-32 degrees Celsius. The treatment may be used on patients with neurological and musculoskeletal conditions. [25]
Water Circuits[edit | edit source]
Water circuits involve different forms of hydrotherapy used one after the other. [26]
Immersion Therapies[edit | edit source]
Similar to bath therapy, this therapy involves immersing the patient into water. Warm and cold-water immersion are the most commonly used types of this therapy. [27]
Mobility Aids and Equipment[edit | edit source]
Mobility aids can be used to provide equal opportunities for people with difficulty when using the pool facilities. This may include:
- The Dipper with Oxford Sling
- Mobile Hoist
- Aquaboard
- Mobile Shower Changing Table [28]
Equipment is sometimes used during hydrotherapy to maximise the "play" element for younger populations. It can also help provide tools to make exercise more efficient in achieving specific outcomes such as relaxation. This can include:
- Aqua Plinth
- Floatation Belts
- Swimming Discs
- Buoyant Dumbbells
- Kick Boards
- Water Noodles
- Wrist and Ankle Weights
- Aquatic Paddles [28]
Benefits and Evidence of Effectiveness[edit | edit source]
Hydrotherapy can be beneficial for controlling symptoms of AS as:
- The warmth and the buoyancy of the water can act as a relaxant - making stretches more effective
- It can help to reduce pain
- It’s easier to stay upright because the effect of gravity is less
- It requires less physical effort than land-based exercises
- Patients have sometimes reported improved sleep quality following hydrotherapy
- Water can act as resistance to help strengthen muscles
- Can provide shock absorption, therefore reducing the impact on the joints [30]
Testimonials of effectiveness of hydrotherapy have been documented in studies. 250 members of the national axial spondylitis association (NASS) completed an online survey on the patients’ experience with hydrotherapy. Thematic analysis of the questionnaires resulted in five emerging themes:
- Emotional well-being: Patients described greater control over their condition when exercising in water
- Exercise behavior: patients often performed a wider variety of exercises including challenging exercises that they would not usually attempt on land
- Group effect: patients described a sense of motivational support when exercising with others in a group
- Professional support: Patients cited the benefit of hydrotherapy sessions led by a physiotherapist who shared their expertise and discussed problems.
- Pool Environment: Patients described gains from non-impact exercise and weightlessness in the water. The warmer pool temperature was stated as a reason for the benefits obtained.
Hydrotherapy was reported to be most beneficial for improving pain relief, mood, quality of life stiffness, and flare management, but less beneficial for improving sleep quality and fatigue. [31]
The effectiveness of hydrotherapy in comparison to land-based therapy has been investigated in a randomized control trial of 69 patients (58 male and 11 female) randomly allocated to a land exercise or aquatic exercise group. Following a course of 4 weeks of completing either land based exercises or aquatic exercises, the study found that both groups showed significant improvements in their symptoms. Improvement in VAS score, bodily pain, general health, and social functioning were greater in the aquatic exercise group. However, improvements in lumbar range of motion and chest expansion were greater in the land-based exercise group.[32]
In terms of use on specific groups of AS patients, there is evidence that hydrotherapy is possibly effective when used in combnation with conventional physiotherapy (land-based exercises and drug management) for some outcomes. A study by van Tuburgen et al. [33] investigated the effects of hydrotherapy (spa therapy) on the effects of improving patient's well-being, pain, and duration of morning stiffness across 40 weeks. The control group consisted of AS patients who stayed home with weekly group physiotherapy sessions and their normal drug management while the intervention group consisted of AS patients who were treated in spa resorts consisting of a combination of group physiotherapy sessions, generalised exercise sessions, and hydrotherapy. There was a significant improvement after 4 weeks of hydrotherapy sessions as compared to conventional treatment and these improvements appear to last for up to 40 weeks. [33] A Spanish study [34] (n=30) investigated the use of an aquatic fitness plus relaxation programme (3 sessions per week) as compared to no treatment across 2 months. A significant improvement was reported by the end of 2 months in AS-specific outcome measures (p<0.05). This included physical function (Bath Ankylosing Spondylitis Functional Index), fatigue (Bath Ankylosing Spondylitis Disease Activity Index), pain at the neck, back and hips, swelling in joints and waking morning stiffness.[34]
Overall, the literature investigating outcomes of hydrotherapy on people with AS is promising but is currently limited. The broad width of what Hydrotherapy/Aquatic Therapy entails makes it difficult to create a fair basis of comparison for the individual literature.
Barriers and Contraindications[edit | edit source]
Barriers[edit | edit source]
Barriers for the use of hydrotherapy can be factorised by patient internal factors, clinician specific factors and environmental factors. When using Hydrotherapy in rehabilitation, these barriers must be accounted for to ensure effective management for the patient. Below is a non-exhaustive evidence supported list which shows barriers that may impact upon the use of hydrotherapy in conventional management of AS.
| Patient barriers | Physiotherapist barriers | Environmental factors |
| Pain | Training opportunities | Covid-19 |
| Lack of interest | Staffing levels | Availability |
| Insufficient Knowledge | Expenses on NHS | |
| Expenses | Transport | |
| Waiting times |
Essential communication skills as detailed by the NICE guidelines for 'Improving the experience of care for people using adult NHS services' [35] with patients ensures that these barriers are somewhat accounted for. Although barriers cannot be eliminated fully, physiotherapists can use their interpersonal communication skills to limit the patient barriers. The importance of ensuring these barriers are accounted for are highlighted in the 'Benefits of Hydrotherapy'. [29][30]
Contraindications[edit | edit source]
| Absolute Contraindications | Relative Contraindications | Precautions | Considerations |
| Acute Systemic Illness | Irradiated Skin during course of radiotherapy | Incontinence of urine/faeces | Shortness of breath with exertion (unfit or if any other causes) |
| Pyrexia | Known aneurysm | Gross obesity | Vertigo/nausea/blackouts |
| Acute vomiting or diarrhoea | Open wounds | Epilepsy | Multiple Sclerosis (especially those with high sensitivity to high temperatures) |
| Medical Instability following an acute episode | Unstable diabetes | Haemophilia | Communication problems |
| Proven chlorine or bromine allergy | Thyroid Deficiency | Widespread MRSA | Dermal sensitivity due to sanitising agents/Psoriasis |
| Resting Angina | Neutropaenia | Hypotension | Verruca/Tinea Pedia |
| Shortness of Breath at rest | Oxygen Dependency | Renal Failure | Boisterous, unpredictable or aggressive behaviour |
| Uncontrolled cardiac failure/paroxysmal nocturnal dyspnoea | Weight in excess of the evacuation equipment’s limit | Poor Skin integrity or open/surgical wounds | Contact lenses and conjunctivitis |
| Open, infected wounds | Pregnancy if water temperature exceeds 35°C | Hearing aids/grommets | |
| Known HIV positive and Hepatitis C patients – not to enter pool during menstruation | Invasive tubes in situ | Impaired sensation/vision/hearing |
Hydrotherapy Exercise and Prescription[edit | edit source]
Exercise[edit | edit source]
According to the NICE guidelines, an individualised structured exercise programme for AS could include: [3]
- Stretching, strengthening and postural exercises
- Deep breathing exercises
- Spinal extension exercises
- Range-of-motion exercises from cervical down to lumbar spine
- Aerobic exercises
- Elements of hydrotherapy as an adjunct therapy for improving pain and functional outcomes
Prescription[edit | edit source]
In terms of Exercise Prescription several key things of note: [36]
- Consider the most appropriate time for activity as symptoms may vary across the day (particularly in the morning)
- Place emphasis on warm-ups due to stiffness being a major concern for people with AS
- Range-of motion exercises should work along all the spinal segments towards its end-range, however ensure that it is tolerable and comfortable
- Emphasis can be placed on spinal extension due to the nature of the condition
- Important to remind participants about their posture throughout the session
- Avoid doing flexibility exercises right before strengthening or cardiovascular exercises due to the inhibition of muscular activities
- Strengthening of extensor muscles and flexibility in flexor muscles are preferred
- For strengthening: focus on low weight, high repetition movements with 2-3 sets progress by increasing number of sets as strength improve
- Cardiovascular exercise intensities are dependent on the level of fitness of the individual, a recommended 30 minutes session of moderate intensity for five times a week is recommended and progressed as appropriate. [3]
Recommendations from the American College of Sports Medicine (ACSM) [37] include:
| Frequency | Intensity | Time | Type | Resistance | Flexibility |
| 5 or more days a week of moderate exercise OR
3-5 days a week of moderate and vigorous exercises |
Moderate or vigorous (measure | At least 30 minutes of continuous or accumulated exercises (10-minute bouts) | Aerobic exercises in body positions that are well tolerated | 2-3 days per week
2-4 sets of 8-12 repetitions at 60 to 70% of 1RM intensity 10-15 repetitions with 40-50% 1RM for elderly |
2-3 days per week
Stretch to point of slight discomfort 2-4 repetitions, 10-30s for most adults 30-60s for elderly |
Case Study[edit | edit source]
Mr Smith (sufferer of AS)
Mr Smith is a 32 - year old male who has been diagnosed with AS in the past 3 years.
He reports:
Flare ups of pain to 7/8 on VAS scale. Pain is a dull ache and is usually in the lower thoracic spine but can often spread into legs when not managed. Occasional sleep disturbance when moving in the night and suffers with continued fatigue affecting office work.
Aggravating factors:
Sitting more 45 minutes at work. Thoracic rotation· Lifting and carrying any weight. Sudden movements
Easing factors:
Lying. Intermittent walking / sitting. Pain medication· Heat.
24 Hour Pattern:
Wakes occasionally in the night with dull ache pain. Feels very stiff in the morning, walks with hunched back to protect back. Pain is better during the day when more active, slowly stands into a more upright posture. Becomes more painful at late PM after a full day of work.
Social History:
Sales assistant – works in office 9-5. Has enjoyed playing football in the past and socialising with friends. Single, recently divorced, no children. Lives alone in 2-bedroom house, Toilet upstairs and downstairs. Driver.
Drug History:
Naproxen. Paracetamol (PRN).
Past Medical History:
Nil.
Physiotherapy Management of Case Study[edit | edit source]
Due to his symptoms fitting the aforementioned indications for hydrotherapy, Mr Smith would benefit from some sessions in adjunct to land-based exercises. A possible outline for hydrotherapy exercises are detailed below.
Hydrotherapy[edit | edit source]
Warm Up (5 minutes)[edit | edit source]
Walking the length of hydrotherapy pool
This is a good way to start the session to get used to the water and ease the muscles into exercise. The buoyancy nature of water means that a body can weigh 50-90% less than on land. This allows for less stress on the joints and so walking the length of the pool can help strengthen the joints with less impact.
Stretches (5-10 minutes)[edit | edit source]
AS can reduce Range of Motion (ROM) in the spine; therefore, stretches can be beneficial to help maintain ROM and relax sore muscles. [38] As Mr Smith can get pain into his legs, examples of stretches to use include:
- Quadricep Stretch
Can be performed either with patient’s own hand or by placing ankle behind a pool noodle and bringing knee up into flexion.
- Hamstring Stretch
Can be performed by having a patient’s back against pool wall and placing ankle over pool noodle, bringing up slowly in front of them.
The inflammation and possibly eventual bony fusion that occurs at the spine normally affects the lumbar region first but can spread and also cause stiffening at the ribcage as well, which could potentially be the case with Mr Smith due to his pain at the thoracic spine. This can affect chest expansion and breathing. Thoracic hydrotherapy stretches to help with this include:
- Wall Corner Stretch
Patient stands facing corners of pool and places hands against the two walls – helping to open up chest. A patient can practice deep, slow breathing in through their nose and out through their mouth during this stretch.
- Thoracic Rotation
Patient stands with their arms crossed over their chest and, keeping their feet pointing forwards, slowly rotate their thoracic spine to the left before returning back to centre. This is then repeated to the right side.
Strength Exercises (10 minutes)[edit | edit source]
Strength exercises are also important in AS to support joint structures and assist with reducing pain. [39] Examples include:
- Hip Abduction
Patient stands facing wall and abducts hip outwards before bringing back to centre. This exercise can help strengthen the muscles surrounding the hip and lower back.
- Hip Extension
Patient stands facing wall and slowly extends hip behind them before bringing back again.
- Squats
Patient faces wall and slowly squats in the water.
- Knee Extension
Patient stands in pool and brings knee up to a 45degree of flexion before extending outwards in front of them and then bringing back to flexion. The resistance from the water allows for greater strengthening of the quadricep muscles.
- Cycling
The patient has their back to the wall and supports their weight through their elbows/hands. Their legs then push through the water in a cycling motion. The resistance of the water helps to strengthen the gluteal, quadricep and hamstring muscles.
Examples of these exercises can be seen in the hydrotherapy video below:
Cool Down (5 minutes)[edit | edit source]
Deep Breathing Exercises
This allows for the patient to work again on their chest expansion.
Scapular Protraction and Retraction
By asking the patient to squeeze their shoulder blades together (retraction) and then 'push them away' from each other (protraction), this allows for some more mobilisation at the thoracic spine and can help the patient feel less stiff.
Conclusion[edit | edit source]
Overall, hydrotherapy can have beneficial effects for those with AS and multiple studies have proven the positive outcomes both physically and mentally. The evidence for whether hydrotherapy is a greater alternative to land-based exercises is lacking. Therefore, a clinician considering hydrotherapy as a treatment method should do so in adjunct with land-based treatment.[41]This way, the patient gets the therapeutic effects of the warm water, helping to reduce pain, in combination with the greater strengthening results from doing exercises on land.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Zhu W., He X., Cheng K., Zhang L., Chen D., Wang X., et al. Ankylosing spondylitis: etiology, pathogenesis, and Treatments. Bone Res. 2019 Aug 5;7(1):1–16.
- ↑ Kanathur N., Lee-Chiong T. Pulmonary Manifestations of Ankylosing Spondylitis. Clin Chest Med. 2010 Sep;31(3):547–54.
- ↑ 3.0 3.1 3.2 NICE. Ankylosing Spondylitis [Internet]. NICE. 2019 Available from: https://cks.nice.org.uk/topics/ankylosing-spondylitis/ [accessed 2022 May 19].
- ↑ Harris C., Gurden S., Martindale J., Jeffries C. Differentiating Inflammatory and Mechanical Back Pain. NASS. Available from: https://nass.co.uk/wp-content/uploads/2020/03/Physiotherapy-modules-1.pdf [accessed Feb 20 2023]
- ↑ Mauro D., Thomas R., Guggino G., Lories R., Brown M., Ciccia F. Ankylosing spondylitis: an Autoimmune or Autoinflammatory disease? Nature Reviews Rheumatology. 2021 Jun 10;17(7):387–404.
- ↑ 6.0 6.1 Brown MA. Genetics of Ankylosing Spondylitis. Curr Opin Rheumatol 2010 Mar;22(2):126–32.
- ↑ Colbert R., DeLay M., Layh-Schmitt G., Sowders D. HLA-B27 Misfolding and Spondyloarthropathies. Prion 2009; 3(1): 15-26.
- ↑ Bowness P., Ridley A., Shaw J., Chan A., Wong-Baeza I., Fleming M., et al. Th17 Cells Expressing KIR3DL2+ and Responsive to HLA-B27 Homodimers Are Increased in Ankylosing Spondylitis. J Immunol 2011 Jan 19;186(4):2672–80.
- ↑ Ciccia F., Ferrante A., Guggino G., Triolo G. The Role of the Gastrointestinal Tract in the Pathogenesis of Rheumatic Diseases. Best Pract Res Clin Rheumatol 2016 Oct;30(5):889–900.
- ↑ Pianta A., Arvikar S., Strle K., Drouin E., Wang Q., Costello C., et al. Two Rheumatoid Arthritis–specific Autoantigens Correlate Microbial Immunity with Autoimmune Responses in Joints. J Clin Invest 2017 Jun 26;127(8):2946–56.
- ↑ Maeda Y., Kurakawa T., Umemoto E., Motooka D., Ito Y., Gotoh K., et al. Dysbiosis Contributes to Arthritis Development via Activation of Autoreactive T Cells in the Intestine. Arthritis Rheumatol 2016 Oct 27;68(11):2646–61.
- ↑ 12.0 12.1 12.2 Zhang L., Zhang Y-J., Chen J., Huang X-L., Fang G-S., Yang L-J., et al. The Association of HLA-B27 and Klebsiella Pneumoniae in Ankylosing spondylitis: a Systematic Review. Microb Pathog. 2018 Apr;117:49–54.
- ↑ Heuft-Dorenbosch L., Spoorenberg A., van Tubergen A., Landewé R., van der Tempel H., Mielants H., et al. Assessment of enthesitis in ankylosing spondylitis. Ann Rheum Dis 2003;62:127–32.
- ↑ Bennett A., Rehman A., Hensor E., Marzo-Ortega H., Emery P., McGonagle D. The Fatty Romanus lesion: a non-inflammatory Spinal MRI Lesion Specific for Axial Spondyloarthropathy. Ann Rheum Dis. 2009 Aug 9;69(5):891–4.
- ↑ Czervionke L., Fenton D. Imaging Painful Spine Disorders. Philadelphia: Elsevier/Saunders; 2011.
- ↑ Mooventhan A., Nivethitha L. Scientific evidence-based effects of hydrotherapy on various systems of the body. N Am J Med Sci. 2014;6(5):199-209.
- ↑ Griffin B., Cabilan C., Ayoub B., Xu H., Palmieri T., Kimble R., Singer Y. The effect of 20 minutes of cool running water first aid within three hours of thermal burn injury on patient outcomes: A systematic review and meta-analysis. Australas Emerg Care. 2022 Dec;25(4):367-376.
- ↑ Abdel-Razek S. Isolated Chemical Burns to the Genitalia. Ann Burns Fire Disasters. 2006 Sep 30; 19(3): 148–152.
- ↑ Nagaich U. Hydrotherapy: Tool for preventing illness. J Adv Pharm Technol Res. 2016;7(3):69.
- ↑ van Tubergen A., van der Linden S. A brief history of spa therapy. Ann Rheum Dis. 2002 Mar 1;61(3):273–5.
- ↑ Tejirian T., Abbas M. Sitz Bath: Where Is the Evidence? Scientific Basis of a Common Practice. Dis Colon Rectum. 2005 Dec;48(12):2336–40.
- ↑ Laukkanen J., Laukkanen T., Kunutsor S. Cardiovascular and Other Health Benefits of Sauna Bathing: A Review of the Evidence. Mayo Clin Proc. 2018 Aug;93(8):1111–21.
- ↑ Lee E., Kolunsarka I., Kostensalo J., Ahtiainen J., Haapala E., Willeit P., et al. Effects of regular sauna bathing in conjunction with exercise on cardiovascular function: a multi-arm, randomized controlled trial. Am J Physiol Regul Integr Comp Physiol. 2022 Sep 1;323(3):R289-R299.
- ↑ Hussain J., Cohen M. Clinical Effects of Regular Dry Sauna Bathing: A Systematic Review. Evid Based Complement Alternat Med. 2018; 2018: 1857413.
- ↑ Becker B. Aquatic therapy: scientific foundations and clinical rehabilitation applications. PM & R. 2009;1(9):859–72.
- ↑ Rewald S., Mesters I., Emans P., Arts J., Lenssen A., Bie R. Aquatic circuit training including aqua-cycling in patients with knee osteoarthritis: A feasibility study. J Rehabil Med. 2015;47(4):376–81.
- ↑ Cochrane D. Alternating hot and cold water immersion for athlete recovery: a review. Phys Ther Sport. 2004 Feb;5(1):26–32.
- ↑ 28.0 28.1 St George's Hydrotherapy. Equipment List. Available from: http://www.hydrotherapypeterborough.com/shared/attachments.asp?f=bc7754b8%2Df57a%2D4b71%2D9063%2De5f1526af8a9%2Epdf&o=Equipment%2DList%2E%2D2016%2Epdf [accessed 26/2/2023]
- ↑ 29.0 29.1 Alexa Active Aging. Benefits Of Hydrotherapy in Ankylosing Spondylitis. Available from: http://www.youtube.com/watch?v=vkMaZyGv80k [accessed 3/9/2022]
- ↑ 30.0 30.1 NASS. Hydrotherapy. Available from: https://nass.co.uk/managing-my-as/exercise/hydrotherapy/ [accessed 26/2/2023]
- ↑ Martin M., Gilbert A., Jeffries C. OP0279-HPR A national survey of the utilization and experience of hydrotherapy in the management of axial spondyloarthritis: the patients’ perspective. Ann Rheum Dis 2018; 77(Suppl 2):187-8.
- ↑ Dundar U., Solak O., Toktas H., Demirdal U., Subasi V., Kavuncu V., et al. Effect of aquatic exercise on ankylosing spondylitis: a randomized controlled trial. Rheumatology International. 2014 Mar 14;34(11):1505–11.
- ↑ 33.0 33.1 Van Tubergen A., Boonen A., Landewé R., Rutten-Van Mölken M., Van Der Heijde D., Hidding A., et al. Cost Effectiveness of Combined spa-exercise Therapy in Ankylosing spondylitis: a Randomized Controlled Trial. Arthritis Rheum. 2002 Oct 14;47(5):459–67.
- ↑ 34.0 34.1 Fernández García R., Sánchez Sánchez L. de C., López Rodríguez M. del M., Sánchez Granados G. Efectos De Un Programa De Ejercicio Físico Y Relajación En El Medio Acuático En Pacientes Con espondiloartritis: Ensayo Clínico Aleatorizado. Medicina Clínica. 2015 Nov;145(9):380–4.
- ↑ NICE. Patient experience in adult NHS services: improving the experience of care for people using adult NHS services. Clinical guideline [CG138]. 2012. Available from: https://www.nice.org.uk/guidance/cg138/resources/patient-experience-in-adult-nhs-services-improving-the-experience-of-care-for-people-using-adult-nhs-services-pdf-35109517087429 [accessed 27/2/2023]
- ↑ 36.0 36.1 Wales Physiotherapy Advisory Group. All Wales Evidence-Based Guidance for Access to Hydrotherapy for NHS patients in Wales. Chartered Society of Physiotherapy. 2016.
- ↑ American College of Sports Medicine. ACSM’s Guidelines for Exercise Testing and prescription. 11th ed. Wolters Kluwer; 2018.
- ↑ Liang Z, Fu C, Zhang Q, Xiong F, Peng L, Chen L, et al. Effects of water therapy on disease activity, functional capacity, spinal mobility and severity of pain in patients with ankylosing spondylitis: a systematic review and meta-analysis. Disability and Rehabilitation. 2021;43(7):895–902.
- ↑ Nolte K, van Rensburg DCJ, Fletcher L. Effects of a 6-month exercise programme on disease activity, physical and functional parameters in patients with ankylosing spondylitis: Randomised controlled trial. South African Journal of Physiotherapy. 2021 Jun 29;77(1).
- ↑ SportsMed Mumbai. Hydrotherapy. Available from: https://www.youtube.com/watch?v=OIh8GLZ5nFs [accessed 27/02/2023]
- ↑ Carayannopoulos A., Han A., Burdenko I. The benefits of combining water and land-based therapy. J Exerc Rehabil. 2020 Feb 26;16(1):20–6.