Systemic Resonse to Burns
Top Contributors - Carin Hunter, Jess Bell and Kim Jackson
Overview of the Skin[edit | edit source]
Our skin, which is part of the integumentary system, is a cutaneous membrane that covers the surface of the body. It is the largest organ system in the human body in terms of weight and surface area. However, it is often overlooked and underappreciated for the role it plays in overall health.[1]
Layers of the Skin[edit | edit source]
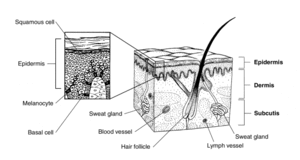
The skin has two principal layers: the epidermis and the dermis. The hypodermis is considered an extension or third layer of the skin by some sources, but not by others.[1] Table 1 provides a summary of the main features of each layer. These layers are also illustrated in Figure 1.
| Epidermis | Superficial layer[2] | Composed of five layers, provides a waterproof barrier and contributes to skin tone | Composed of epithelial tissue | Avascular |
| Dermis | Deeper, thicker layer[2] | Composed of two layers | Contains blood vessels, nerves, glands and hair follicles | Highly vascularised |
| Hypodermis | Deepest layer[2] | Storage for fat/ insulation
Attaches to underlying facia |
Made up of loose connective tissue and adipose tissue | Contains large blood vessels |
For more information on the skin, please see Skin Anatomy, Physiology, and Healing Process. This page provides a detailed discussion of the role of the skin, its layers and normal tissue healing.
Healing Process[edit | edit source]
When treating a burns patient, it is crucial to understand tissue healing. Your knowledge of tissue healing and the information gathered from your assessment will influence clinical decisions, including when to rest, exercise, stretch and strengthen during the recovery period.
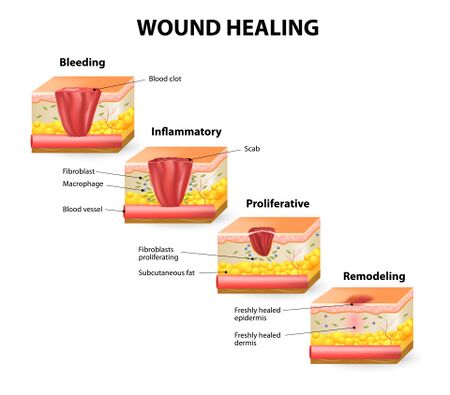
There are four stages of healing (see Figure 2). Each stage can be impacted by factors such as the size of the burn, surgical intervention and other complications. Clinical reasoning is essential when applying these principles in practice.
Haemostasis[edit | edit source]
- The process of wound closure by clotting
- This process starts when blood leaks out of the body, and the blood vessels constrict to restrict blood flow
- Platelets quickly aggregate and adhere to the sub-endothelium surface
- Within 60 seconds, the first fibrin strands begin to adhere
- As the fibrin mesh begins to form, blood is transformed from a liquid to a gel through pro-coagulants and the release of prothrombin
- The formation of a thrombus / clot traps the platelets and blood cells in the wound area
- Treatment at this stage focuses on:
- reducing heat, oedema and pain
- preventing infection and disruption of the wound
- Useful interventions include:
- immobilisation
- positioning
- splinting[3]
Inflammation[edit | edit source]
- Occurs 0-5 days post-injury
- Vasoconstriction is followed by vasodilatation and an influx of inflammatory mediators and white blood cells
- There is an increased capillary permeability and exudate leaks into the tissues - pus may also be produced
- Signs include:
- redness
- heat
- swelling
- pain
- Treatment focuses on:
- reducing heat, oedema and pain
- preventing infection and disruption of the wound
- Useful interventions include:
- immobilisation
- positioning
- splinting[3]
Proliferation (Fibroplasia)[edit | edit source]
- Begins days 3-5 and lasts 2-6 weeks
- Fibroblasts synthesise collagen (laid down haphazardly at this stage) and angiogenesis continues
- Signs include moist red raised tissue over the wound
- Treatment focuses on:
- reducing oedema
- preventing contractures
- Early interventions include:
- positioning
- immobilisation
- Later interventions include gentle stress with splinting and exercise[3]
Remodelling (Maturation)[edit | edit source]
- Begins weeks 4-6 and lasts up to 2 years
- Collagen synthesis is balanced by degradation
- Collagen fibres are organised along the lines of stress
- Signs include:
- wound closure
- red and raised scar, progressing to a flat, pale and pliable scar
- scar tissue tightens
- Treatment focuses on:
- optimising function
- splinting
- positioning
- exercise
- stretching
- strengthening[3]
For more information on the healing process, please see:
Systemic Response to Burns[edit | edit source]
Different factors contribute to the magnitude of the host response to a burn wound, including:
- burn severity (percentage total body surface area (TBSA) of the burn and burn depth)[4]
- burn cause
- inhalation injury
- exposure to toxins
- other traumatic injuries
- patient-related factors
- age
- pre-existing chronic medical conditions
- drug or alcohol intoxication
- timing of presentation to care
Pathophysiology of Burn Wounds[edit | edit source]
In severe burn injuries (i.e. >30% TBSA), complex reactions occur both at the burn and away from the burn. Excess cytokines, chemokines, histamines, prostaglandins and other inflammatory and vasoactive mediators are released.[5] This results in extensive inflammatory reactions within a few hours of the burn injury. As well as the inflammatory response, burn injuries, particularly severe burns, also cause an immune response, metabolic changes and distributive shock.[6] Depending on the size of the burn injury, a patient's initial response is similar to the response that occurs after "other inflammatory conditions triggered by tissue destruction such as trauma or major surgery".[7]
The pathophysiology of burn wounds can be summarised as follows.
The inflammatory response leads to rapid oedema formation. This is caused by:[8]
- increased microvascular permeability
- increased hydrostatic microvascular pressure
- vasodilation
- increased extravascular osmotic activity
These reactions are caused by the direct effect of heat on the microvasculature and the chemical mediators of inflammation:[8]
- the release of histamine tends to cause early vasodilation and increased venous permeability
- prostaglandin is rapidly formed because of damage to the cell membranes
- this damage is caused in part by oxygen-free radicals that are released from polymorphonuclear leucocytes
- this activates the enzymes that catalyse the hydrolysis of prostaglandin precursor
- prostaglandins inhibit the release of noradrenaline (also known as norepinephrine) - this may have a modulatory impact on the adrenergic nervous system, which is activated by thermal injuries
- there are further changes in the structure of the blood-lymph barrier, such as an increase in the number of vacuoles and more open endothelial intercellular junctions
- there are changes in the interstitial tissue
- there is a continuous loss of fluid from the blood circulation, resulting in increased haematocrit levels and a fall in plasma volume - this leads to decreased cardiac output and hypoperfusion at the cellular level
- burn shock occurs if fluid loss is not adequately restored[9] (to learn more about the complexities of burn shock, please see: Burn Shock)
Impact of Burn Injuries on Body Systems[edit | edit source]
1. Effect on the Cardiovascular System[edit | edit source]
The initial cardiovascular response to the catecholamine-mediated surge from a severe burn injury is hypovolaemia (decrease in blood volume) with myocardial depression and reduced venous return.[10] This leads to decreased cardiac output, increased heart rate, and peripheral resistance. In addition to the cardiac dysfunction, pulmonary resistance increases, which causes an increase in right- and left-ventricular workload.[11][12]
This then progresses to a "hyperdynamic-hypermetabolic phase with increased cardiac output."[10] This second phase is characterised by tachycardia, increased myocardial oxygen consumption, and increased cardiac output. It is important to note that cardiac stress continues for at least two years after a burn injury.[13]
Compromised cardiac function can:[11]
- cause hypoperfusion of organs
- affect peripheral microcirculation
- lead to an extension of the burn zone
- result in decreased resistance to bacterial infections at the wound
Burn Shock: "Burns exceeding 30% of total body surface area (TBSA) result in considerable hypovolemia coupled with formation and release of inflammatory mediators with subsequent systemic effect, namely a distinctive cardiovascular dysfunction known as burn shock."[14] Burn shock is a complex process that affects the circulatory and microcirculatory systems,[14] with "rapid and extensive fluid transfer in burn and non-burn tissues".[15]
"Burn shock is a unique combination of hypovolemic and distributive shock, accompanied by cardiogenic shock."[16]
- In severe burn wounds, there is an increase in local and systemic vascular permeability, which causes intravascular fluid to leak out
- Ultimately, this causes a gradual decrease in circulation volume, increased systemic vascular resistance, decreased cardiac output and peripheral tissue oedema[15]
- Management of burn shock requires fluid resuscitation and close monitoring to ensure there are adequate (though not excessive) IV fluids[10]
** Hypovolaemic shock: occurs when there is a loss of approximately one-fifth or more of the normal amount of blood in the body.
2. Effect on the Respiratory System[edit | edit source]
- Heat injury to the upper airway:[17]
- heat injury to airway structures causes extensive swelling of the tongue, epiglottis, and aryepiglottic folds, resulting in obstruction
- Chemical injury to the lower airway:[17]
- inflammatory mediators are released in the lungs, leading to bronchoconstriction, pulmonary oedema and acute respiratory distress syndrome (ARDS)
- Systemic toxicity:[17]
- inhalation of chemicals, cytotoxic liquids, fumes, mist and gases can cause systemic toxic changes
- smoke can combine with these toxins, resulting in increased mortality because of tissue hypoxia, metabolic acidosis, decreased oxygen supply to the brain and decreased metabolism[18]
For more information, please read Inhalation Injury.
3. Effect on the Renal System[edit | edit source]
Early kidney injury is due to:
- low blood volume
- inflammatory mediators
- increased release of protein in the bloodstream
- extensive tissue damage
- medications that are toxic to the kidneys
The renal system is affected by changes in the cardiovascular system caused by a burn injury. Blood flow to the kidneys is decreased due to hypovolaemia, reduced cardiac output and the effects of angiotensin, vasopressin and aldosterone. This marks the beginning of kidney failure. Appropriate fluid resuscitation can help prevent these issues. The rehabilitation team should always keep an eye out for decreased urine output (oliguria) as this is an early sign of renal compromise.[19]
4. Effect on the Endocrine System[edit | edit source]
The endocrine system is a network of glands in the body, which secrete hormones. The endocrine system can be affected after severe burn injuries.[20]
Trauma can affect the HPA Axis (hypothalamic-pituitary-adrenal axis), which controls the interaction between the hypothalamus, pituitary gland, and adrenal glands. The hypothalamus and pituitary gland are located just above the brainstem, while the adrenal glands are found on top of the kidneys.
Burn injuries commonly cause patients to have an elevated sympathetic drive. This is due to an increase in the release of cortisol and glucagon. These hormones affect the metabolic system (see below). Prolonged excess cortisol (hypercortisolaemia) is associated with increased infection rates in burn patients and lengthened duration of severe infection.[21]
Severe burn injuries can alter a patient's urine output. Glucose readings also need to be monitored closely, as misdiagnosis can have life-threatening consequences.[22]
Hypoparathyroidism, following a severe burn, can also affect the metabolism of bone and minerals. This also needs to be rectified by supplementing with calcium, magnesium, and phosphate.[22]
5. Effects on the Metabolic System[edit | edit source]
In the initial period, for around 72-96 hours post-burn,[6] individuals with severe burn wounds enter a hypometabolic state (known as the ebb phase). This may be caused by various intracellular processes. It results in:[23][6]
- decreased metabolic rate
- reduced intravascular volume
- poor perfusion of the tissues
- low cardiac output
Hypermetabolism (an increase, often of up to 100-150%, in the metabolic rate) begins approximately five days post-burn in patients with severe burns.[24] It can result in organ catabolism, greater incidence of organ failure, infections and death.[6] It occurs in response to "a series of events triggered by a significant and persistent rise in secretions of cateholamine, cortisol, glucagon and dopamine."[14] Effects can be seen for up to three years post-burn.[6]
Hypermetabolism can cause:[6][25][26]
- increased resting energy expenditure
- increased body temperature
- increased oxygen and glucose consumption
- increased CO2 and minute ventilation
- increased heart rate
- muscle wasting, etc
6. Immunological Changes[edit | edit source]
Burn injuries have a significant impact on the immune system. For example, in burn injuries, the actions of neutrophils, natural killer cells and macrophages are impaired, and there are reductions in the numbers of T lymphocytes. For a detailed discussion of immune system changes, please see: The pathogenesis and diagnosis of sepsis post burn injury.[27]
Ultimately, "the compromised alterations in innate and adaptive immune responses result in enhanced susceptibility to infection, sepsis and multiple organ failure."[27]
7. Oedema formation[edit | edit source]
Oedema formation is a characteristic response to burn injuries. It has two phases:[14]
- in the first hour after the burn, there is an increase in water content of the affected tissue
- in the second phase, there is a gradual increase in "fluid flux of both burned and intact skin and soft tissues 12-24 hours post-burn"[14]
Rapid oedema formation is caused by:[28]
- strongly negative interstitial fluid pressure developing
- greater microvascular permeability
- loss of glycocalyx
- endothelial activation
Fluid resuscitation (in terms of type, timing, total amount) will affect these shifts in fluid.[28]
References[edit | edit source]
- ↑ 1.0 1.1 Palmer, D. Skin Anatomy, Physiology, and Healing Course. Physiotherapy Wound Care Programme. Plus, 2022.
- ↑ 2.0 2.1 2.2 McCann C, Watson A, Barnes D. Major burns: Part 1. Epidemiology, pathophysiology and initial management. BJA education. 2022 Mar 1;22(3):94-103.
- ↑ 3.0 3.1 3.2 3.3 Hale A, O’Donovan R, Diskin S, McEvoy S, Keohane C, Gormley G. Impairment and Disability Short Course. Physiotherapy in Burns, Plastics and Reconstructive Surgery, 2013.
- ↑ Kumar R, Keshamma E, Kumari B, Kumar A, Kumar V, Janjua D, Billah AM. Burn Injury Management, Pathophysiology and Its Future Prospectives. Journal for Research in Applied Sciences and Biotechnology. 2022 Oct 31;1(4):78-89.
- ↑ Schaefer TJ, Nunez Lopez O. Burn Resuscitation and Management. [Updated 2023 Jan 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430795/
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 Jeschke MG, van Baar ME, Choudhry MA, Chung KK, Gibran NS, Logsetty S. Burn injury. Nat Rev Dis Primers. 2020 Feb 13;6(1):11.
- ↑ Jeschke MG. Pathophysiology of burn injury. Springer International Publishing; 2021.
- ↑ 8.0 8.1 Arturson G. Pathophysiology of the burn wound. Ann Chir Gynaecol.1980;69(5):178-90.
- ↑ Noreen S, Maqbool I, Ijaz S. Skin Burns: Pathophysiology, types and Therapeutic Approaches. Pathophysiology. 2010;1(3).
- ↑ 10.0 10.1 10.2 Panchal A, Casadonte J. Burn-induced myocardial depression in a pediatric patient leading to fulminant cardiogenic shock and multiorgan failure requiring extracorporeal life support. Clin Case Rep. 2020 Feb 22;8(4):602-605.
- ↑ 11.0 11.1 Abu-Sittah GS, Sarhane KA, Dibo SA, Ibrahim A. Cardiovascular dysfunction in burns: a review of the literature. Ann Burns Fire Disasters. 2012;25(1):26-37.
- ↑ Williams FN, Herndon DN, Suman OE, Lee JO, Norbury WB, Branski LK, Mlcak RP, Jeschke MG. Changes in cardiac physiology after severe burn injury. J Burn Care Res. 2011;32(2):269-74.Abu-Sittah GS, Sarhane KA, Dibo SA, Ibrahim A. Cardiovascular dysfunction in burns: a review of the literature. Ann Burns Fire Disasters. 2012;25(1):26-37.
- ↑ Williams FN, Herndon DN, Suman OE, Lee JO, Norbury WB, Branski LK, Mlcak RP, Jeschke MG. Changes in cardiac physiology after severe burn injury. Journal of burn care & research. 2011 Mar 1;32(2):269-74.
- ↑ 14.0 14.1 14.2 14.3 14.4 Kaddoura I, Abu-Sittah G, Ibrahim A, Karamanoukian R, Papazian N. Burn injury: review of pathophysiology and therapeutic modalities in major burns. Ann Burns Fire Disasters. 2017 Jun 30;30(2):95-102.
- ↑ 15.0 15.1 Chi Y, Liu X, Chai J. A narrative review of changes in microvascular permeability after burn. Ann Transl Med. 2021 Apr;9(8):719.
- ↑ Ishikawa T. Maeda H. Systemic response to trauma. In Siegel JA, Saukko PJ, Houck MM editors. Encyclopedia of Forensic Sciences (Second Edition), Academic Press, 2013. p47-53.
- ↑ 17.0 17.1 17.2 Galeiras R. Smoke inhalation injury: a narrative review. Mediastinum. 2021;5.
- ↑ Physiopedia. Inhalation Injury.
- ↑ Physiopedia. Burns Overview.
- ↑ D'Asta F, Cianferotti L, Bhandari S, Sprini D, Rini GB, Brandi ML. The endocrine response to severe burn trauma. Expert Rev Endocrinol Metab. 2014 Jan;9(1):45-59.
- ↑ Norbury WB, Herndon DN, Branski LK, Chinkes DL, Jeschke MG. Urinary cortisol and catecholamine excretion after burn injury in children. J Clin Endocrinol Metab. 2008 Apr;93(4):1270-5.
- ↑ 22.0 22.1 D’Asta F, Cianferotti L, Bhandari S, Sprini D, Rini GB, Brandi ML. The endocrine response to severe burn trauma. Expert review of endocrinology & metabolism. 2014 Jan 1;9(1):45-59.
- ↑ Clark A, Imran J, Madni T, Wolf SE. Nutrition and metabolism in burn patients. Burns & trauma. 2017 Dec 1;5.
- ↑ Herndon DN, Barrow RE, Rutan TC, Minifee PA, Jahoor FA, Wolfe RR. Effect of propranolol administration on hemodynamic and metabolic responses of burned pediatric patients. Annals of surgery. 1988 Oct;208(4):484.
- ↑ Grisbrook TL, Elliott CM, Edgar DW, Wallman KE, Wood FM, Reid SL. Burn-injured adults with long term functional impairments demonstrate the same response to resistance training as uninjured controls. Burns. 2013 Jun 1;39(4):680-6.
- ↑ Jeschke MG, Mlcak RP, Finnerty CC, Norbury WB, Gauglitz GG, Kulp GA, Herndon DN. Burn size determines the inflammatory and hypermetabolic response. Critical care. 2007 Aug;11(4):1-1.
- ↑ 27.0 27.1 Zhang P, Zou B, Liou YC, Huang C. The pathogenesis and diagnosis of sepsis post burn injury. Burns Trauma. 2021 Feb 4;9:tkaa047.
- ↑ 28.0 28.1 Wurzer P, Culnan D, Cancio LC, Kramer GC. 8 - Pathophysiology of Burn Shock and Burn Edema. In: Herndon DN editor. Total burn care (Fifth Edition). Elsevier, 2018. p66-76.e3.