Suprascapular Nerve Palsy
Introduction[edit | edit source]
The suprascapular nerve is a mixed nerve of the upper limb. Suprascapular nerve injury is experiencing an increase in clinical significance due to its role in shoulder pain and upper limb weakness.[1]
Anatomy[edit | edit source]
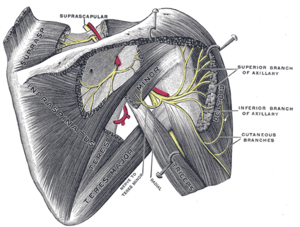
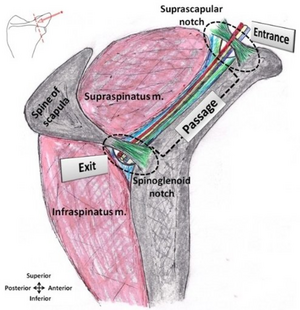
The suprascapular nerve branches out from the upper trunk of the brachial plexus. Its nerve roots are C5 and C6. Sporadically, it may have roots from C4 as well. From the posterior triangle of the neck, the nerve goes over the upper part of the scapula, then downward and laterally, parallel to the omohyoid muscle belly. It then passes below the suprascapular ligament, through the suprascapular notch and into the supraspinous fossa where it innervates the supraspinatus muscle. Through here it curves around the spinous process of the scapula, through the spinoglenoid notch and then into the infraspinous fossa where it innervates the infraspinatus muscle.[1]The suprascapular nerve also provides sensory innervation to the glenohumeral and acromioclavicular joint.[2]
Etiology[edit | edit source]
Compression neuropathy resulting from nerve entrapment is the most common cause of suprascapular nerve palsy. The common sites of nerve entrapment are the suprascapular notch and the spinoglenoid notch.[3]
Trauma to the shoulder resulting from fractures of scapula, clavicle and proximal humerus can significantly damage the suprascapular nerve.[4][5]
Post-surgical complications after open or athroscopic shoulder surgery can lead to suprascapular nerve damage.[6]
Scapula dyskinesia can lead to suprascapular nerve palsy.[7]
Tumours, cysts and other space-occupying lesions around the shoulder can compress the suprascapular nerve.[8]
In rare cases, systemic conditions like systemic lupus erthymatosus and rheumatoid arthritis can result in suprascapular nerve palsy.[9]
Clinical presentation[edit | edit source]
Usually, patients will present with dull, aching pain over the superior or posterolateral aspect of the shoulder. Pain might radiate down the upper limb or to the neck. Cross-body adduction and internal rotation may increase pain. Pain will not be present if nerve injury is distal to spinoglenoid notch. Almost 40% of cases present with associated trauma to the shoulder. This is common in athletes involved in repeated overhead activities. Patients with history of trauma can also report a sense of instability in the shoulder.[7]
The most common clinical sign of suprascapular nerve palsy is atrophy of the supraspinatus and/or infraspinatus muscles. It is seen in 80% of cases. Owing to the anatomical course of the nerve, if the injury is proximal to the spinoglenoid notch, both muscles will be atrophied and if the injury is distal to the spinoglenoid notch, the supraspinatus is spared and only the infraspinatus will present with atrophy.[7]
The "suprascapular nerve stretch test" is useful to determine the involvement of the suprascapular nerve during physical examination. Here, the patient is asked to laterally rotate the head away from the affected shoulder and retract the neck. If the pain at the shoulder worsens with this manoeuvre, the test is positive.[10]
Diagnosis[edit | edit source]
Nerve conduction studies and electromyography is considered to be the gold standard for the diagnosis of suprascapular nerve palsy. Prolonged latency, decreased amplitude, fibrillation potentials, and positive sharp waves in the nerve conduction study are indicative of suprascapular nerve compression and denervation. X-rays can help rule out trauma to the surrounding bones. CT, MRI, and diagnostic ultrasound can help localize the site of injury. Instant pain relief following an aesthetic injection to either the suprascapular or supraglenoid notch can support the diagnosis.[7]
Management[edit | edit source]
Medical[edit | edit source]
Non-steroidal anti-inflammatory drugs and anaesthetic injections (nerve block) are used to conservatively manage the pain.[7]
Surgical[edit | edit source]
Surgery is only considered in cases that show no improvement after 6-12 months of conservative management. Surgical decompression of the suprascapular nerve is performed along with repair of the contributing shoulder pathology (if present).[7]
Physiotherapy[edit | edit source]
Sports-specific activity modification is advised for overhead athletes to prevent repetitive trauma. Full range of motion should be maintained at the shoulder to prevent adhesive capsulitis. Posterior shoulder capsule stretching and strengthening of the rotator cuff and shoulder muscles is recommended. There are no protocols for physiotherapy management of suprascapular nerve palsy.[7] Research must focus on addressing this area of clinical significance.
For a detailed description of nerve injury rehabilitation in general, visit this page on Physiopedia.
References[edit | edit source]
- ↑ 1.0 1.1 Kostretzis L, Theodoroudis I, Boutsiadis A, Papadakis N, Papadopoulos P. Suprascapular Nerve Pathology: A Review of the Literature. Open Orthop J. 2017 Feb 28;11:140-53.
- ↑ Avery BW, Pilon FM, Barclay JK. Anterior coracoscapular ligament and suprascapular nerve entrapment. Clin Anat. 2002 Nov;15(6):383-6.
- ↑ Gosk J, Urban M, Rutowski R. Entrapment of the suprascapular nerve: anatomy, etiology, diagnosis, treatment. Ortop Traumatol Rehabil. 2007 Jan-Feb;9(1):68-74.
- ↑ Zoltan JD. Injury to the suprascapular nerve associated with anterior dislocation of the shoulder: case report and review of the literature. J Trauma. 1979 Mar;19(3):203-6.
- ↑ Solheim LF, Roaas A. Compression of the suprascapular nerve after fracture of the scapular notch. Acta Orthop Scand. 1978 Aug;49(4):338-40.
- ↑ Mallon WJ, Bronec PR, Spinner RJ, Levin LS. Suprascapular neuropathy after distal clavicle excision. Clin Orthop Relat Res. 1996 Aug;(329):207-11
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 Reece CL, Varacallo M, Susmarski A. Suprascapular Nerve Injury. [Updated 2021 Jul 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559151/
- ↑ Sjödén GO, Movin T, Güntner P, Ingelman-Sundberg H. Spinoglenoid bone cyst causing suprascapular nerve compression. J Shoulder Elbow Surg. 1996 Mar-Apr;5(2 Pt 1):147-9.
- ↑ Zehetgruber H, Noske H, Lang T, Wurnig C. Suprascapular nerve entrapment. A meta-analysis. Int Orthop. 2002;26(6):339-43.
- ↑ Lafosse L, Piper K, Lanz U. Arthroscopic suprascapular nerve release: indications and technique. J Shoulder Elbow Surg. 2011 Mar;20(2 Suppl):S9-13.