Supracondylar Humeral Fracture
Original Editor - Peter Sheehy
Top Contributors - Manisha Shrestha, Andeela Hafeez, Admin, Kim Jackson, Peter Sheehy, WikiSysop, Karen Wilson and Rishika Babburu
Clinically Relevant Anatomy[edit | edit source]
The Supracondylar fracture of the humerus is a fracture of the distal end of the humerus just above the elbow joint. The transverse section of the shaft of the humerus is somewhat circular in shape which gets more flattered as it descends down to meet the distal end of the humerus.[1]
The distal end of humerus comprises of both articular and non-articular structures. Non- articular structure comprises of the medial epicondyle, lateral epicondyle, anterior coronoid and radial fossa and posterior olecranon fossa.Whereas articular structure includes the lateral capitulum articulating with radial head and the medial trochlea articulates with the ulna.
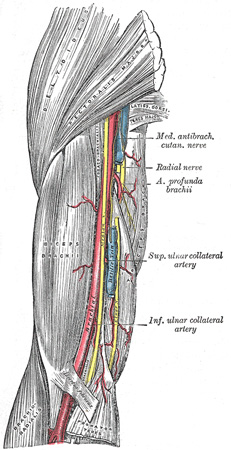
The medial epicondyle is the site for the common origin of flexor musculature of the forearm and the ulnar nerve runs in a groove on the back of this epicondyle. The lateral epicondyle is the site for the common origin of extensor musculature of the forearm. These muscles attachment are responsible for the displacement and rotation of the distal fragment.[2] In the anterior aspect of distal humerus allow the passage of the brachial artery and median nerve.[1] The brachial artery which commonly gets involved in supracondylar fracture of humerus lies along the anteromedial aspect of the distal humerus just superficial to the brachialis muscle.[2] The radial nerve runs between the brachialis and brachioradialis muscles before crossing the elbow and penetrating the supinator muscle.[2]
Epidemiology[edit | edit source]
- Supracondylar fractures of the humerus are the most frequent fractures of the pediatric humerus, with the median age being 6 years and a peak incidence at the ages of five to eight years.
- It is the second most common bony injury in the pediatric population.[3]
- It accounts for 55% to 80% of total elbow fractures in children and up to two-thirds of pediatric elbow injuries requiring hospitalization.
- Their incidence has been estimated at 177.3 per 100 000.
- Higher incidence of supracondylar fractures is in boys, affecting the non-dominant arm 1.5 times more frequently.
- About 10% to 20% of displaced supracondylar fractures present with alterations in vascular status. In most cases, fracture reduction restores perfusion.
- Neural injuries occur in 6.5% to 19% of cases involving displaced fractures. Most of them are neurapraxias. [4]
Mechanism of Injury / Etiology[edit | edit source]
Pediatric population predisposed, especially during ages when the supracondylar bone is undergoing skeletal maturation and has a thin and weak cortex. The ossification process of distal humerus occurs at different ages. The supracondylar area undergoes remodelling between 6 to 7 years of age and is typically thinner with a more slender cortex, predisposing this area to fracture.[5][2]
The distal humerus anatomy is especially predisposed to injury because its configuration in two columns connected by thin bone represents a zone of weakness.[4]
Supracondylar fractures usually occur as a result of a fall from height or from sports or leisure or fall on outstretched hand( FOOSH).
Extension type injury (97% to 99%) is more common than flexion type(1-3%). [4]
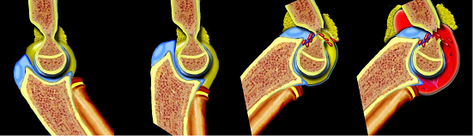
When a fall on the outstretched hand occurs, the olecranon engages on the olecranon fossa and if elbow extension progresses, the olecranon finally acts as a fulcrum on the fossa. While the anterior elbow joint capsule produces an anterior tensile load, resulting in fracture and disruption of anterior periosteum. Therefore, the bone begins to break at first anteriorly and the fracture progresses posteriorly. If the energy is high, the posterior cortex disrupts, and finally complete posterior displacement of the distal fragment occurs with the posterior periosteum acting as a hinge. This is the mechanism of extension-type fractures.[4]
Flexion-type fractures are usually caused by direct trauma to the flexed elbow. In these cases, the anterior periosteum acts as a hinge, and the progression of the injury goes from the posterior to the anterior part of the distal humerus. The distal fragment also tends to be translated in the coronal plane.[4][2]
Clinical Presentation[edit | edit source]
Supracondylar fracture often present with associated forearm fractures, soft tissue damage, neurologic injury, and significant risk for developing compartment syndrome, thus an examination of the entire upper extremity should be performing thoroughly. It includes:[2][4]
History
- Classical history of fall on an outstretched hand followed by pain and swelling over the elbow with loss of function of the upper limb, the onset of pain holds special consideration.
- It is very important to know whether the pain is due to fracture or because of muscle ischemia which has a late-onset (hours after the injury).[2]
Observation
- Painful swollen elbow and forearm with hesitant to move.[2]
- Ecchymosis, skin puckering (this sign appears when the proximal fragment transects the brachialis muscle, ‘puckering’ the deep dermis), bruises[4]
- Bleeding puncture wound (indicates open fracture)
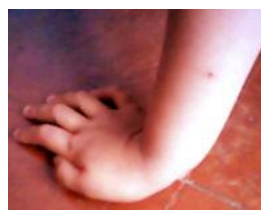
- In displaced extension-type fractures, the so-called ‘S-deformity’ is usually present.[4]
Vascular status evaluation:
Vascular compromise exists in up to 10% to 20% of displaced fractures. Both radial and ulnar pulses must be palpated at the wrist of the injured extremity. In case of pulselessness ( Pulseless hand), other signs of perfusion must be checked viz., color (the hand should be pink), temperature, capillary refill ( less than 2 seconds), and oxygen saturation on the pulse oximeter. [2]
Classification:
- Class I - well perfused (warm and red) with radial pulse
- Class II – well perfused but radial pulse absent
- Class III – poorly perfused (cool and blue or blanched) and radial pulse absent
Neurologic status:
The degree of involvement and possible progression/ regression of symptoms of the nerve is a must before and after treatment. Neuropraxias is common and generally resolve with the restoration of normal alignment and lengths.[2]Neuropraxias that usually resolve within two to three months.
- Anterior Interosseous Nerve Branch (AIN) of the median nerve is most prone to get involved in postero-lateral displacement of the distal fracture fragment. A child may present with no sensory loss in hand but a weak" OK sign" (e.g., more of a pincer grasp than an OK sign) on physical examination.
- Radial nerve impingement most commonly occurs when the distal fracture fragment is displaced posteromedially. It can be examined with decreased sensation in dorsal aspect of the hand and weak wrist extensors.
- Ulnar nerve is prone to injury following flexion type of supracondylar fractures and loss of sensation in its distribution can be examined following weakness of intrinsic muscles of the hand.[2][4]
Compartment syndrome: Severe swelling and/or ecchymosis, anterior skin puckering, and vascular compromise with severe pain.
Diagnostic Procedures[edit | edit source]
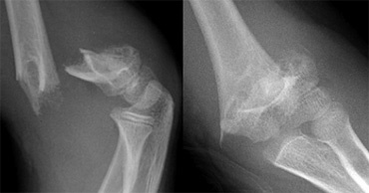
Radiographs should include true AP of distal humerus (not elbow) and true lateral elbow views.If there is only minimal or no displacement these fractures can be occult on radiographs. The only sign will be a positive fat pad sign.[2]
On lateral view
The lateral view also allows assessing the degree of displacement and the integrity of the posterior cortex.
On the lateral view, the following radiological parameters are looked for: (a) Anterior humeral line; (b) Coronoid line; (c) Fish tail sign; (d) Fat pad sign; (Anterior and Posterior).
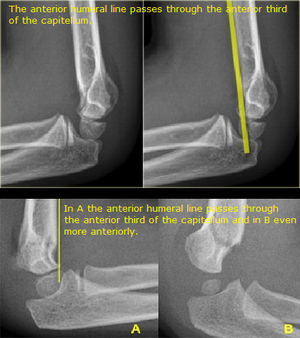
Anterior humeral line to capitulum orientation on a lateral view
- Normal elbow - line continues the anterior cortical of the humerus and should traverse the capitulum in its middle third line.
- Extension type injury: capitulum posterior to line
- Flexion type injury: capitulum anterior to the line[3]
On AP view
It helps to evaluate the direction of displacement, the presence of varus or valgus alignment, and the extent of the fracture comminution.
The Baumann angle (Humeral capitular angle) on AP view
- Angle between linea perpendicular to longthe axis of humeral shaft and the physeal line of the capitulum, isused to assess varus or valgus alignment of the distal humerus.
- Normal range – 64º to 82º degrees
- Decrease in angle – varus angulated fracture with possible medial column comminution
The Ulnohumeral angle or radiological carrying angle on AP view
- The angle formed by the diaphyseal axis of the humerus and the axis of the proximal third of the ulna.
- It is also used to assess varus or valgus deformity and it is more accurate and useful than Baumann’s angle [4]
Classification of Supracondylar fracture[edit | edit source]
Modified Gartland classification( 2006)of supracondylar fractures (based on lateral radiograph):[5][4][7]
Type I
- Nondisplaced or minimally displaced (<2mm) with intact anterior humeral line
- No disruption of periosteum – stable fracture
- Fat pad signs may be only found
Type II
- Displaced (>2mm) with hinged intact posterior cortex
- Anterior humeral line does not pass through the middle third of capitulum on lateral radiographs
- No rotational deformity on AP radiograph
Type III
- Displaced with no meaningful cortical contact, usually sagittal plane extension and frontal/horizontal plane rotation
- Significant periosteum disrupture, soft tissue and neurovascular injuries common
- Medial column comminution and collapse with malrotation in the frontal plane
Type IV
- Multidirectional instability
- Incompetent periosteal hinge circumferentially, with instability in flexion and extension
Complications of supracondylar fracture[2][edit | edit source]
Immediate complications are associated with neurovascular involvement including
- Vascular insufficiency / pink pulseless hand- involvement of the brachial artery is most commonly associated with Type II and III supracondylar fractures, frequently encountered in posterolaterally displaced fracture.
- Compartment syndrome: It can occur in 0.1% to 0.3% of cases.Associated forearm fractures and elbow flexion > 90° increase compartment pressures. To minimize the risk of compartment syndrome, the elbow should be immobilized in about 30° of flexion in the emergency room and 60° to 70° of after surgery.[2]
- Neurologic deficit-10 to 20 percent of supracondylar fracture and mainly associated with Type III supracondylar fractures.[4]
- Open or associated forearm fractures
Long term complications in Pediptric population is due to the fact that bones in this age group have an enormous growth as well as remodelling ability. So that long term functional outcome and radiological appearance of a fracture may be quiet different than that of immediate post-management status.
- Cubitus varus deformity: It occurs due to the malunion and also known as "gunstock” deformity. Posttraumatic cubitus varus deformity has important problems, which are associated with tardy ulnar nerve palsy, tardy Postero-Lateral Rotatory Instability (PLRI), shift of the medial head of the triceps and secondary distal humeral fractures. Modern surgical techniques (e.g., closed reduction with percutaneous pinning) have reduced its frequency from 58 percent to approximately 3 percent in children treated for supracondylar fractures. Humeral osteotomy is used to correct this deformity and to avoid such later complications.[4]
- Volkmann’s ischemic contracture: If compartment syndrome is not treated timely, the associated ischemia may progress to infarction and subsequent development of Volkmann's ischemic contracture: fixed flexion of the elbow, pronation of the forearm, flexion at the wrist, and joint extension of the metacarpal-phalangeal joint.[2]
Management / Interventions[edit | edit source]
Medical[edit | edit source]
Management of supracondylar fracture is determined based on the type of fracture based on Modified Gartland Classification.
Type I ( Non-displaced fracture)
- Immobilization with a long-arm cast or splint.
- With elbow flexion up to 80° to 90° and mid pronation-supination are well toleratable for ~3weeks.
- Flexion of the elbow within the cast should not pass 90° because it can increase forearm pressures and impede distal vascular flow.
- Radiographic check at 1 and 2 weeks
Types II
- A closed reduction(CR) and percutaneous pinning fixation is recommended than CR and immobilization as the risk of complication are low. Pins are removed in the hospital approximately three weeks after surgery.[8]
Type III and Type IV
- Closed reduction and percutaneous pinning is the gold standard for all displaced fractures and is widely used in Type III and IV fractures.
- Open reduction is indicated:
- When the surgeon is not able to reduce the fracture by closed means
- When there is soft-tissue entrapment (i.e. muscle, median nerve, brachial artery) or
- When a cold hand remains without perfusion after an attempt at closed reduction has been performed.
There is an increased incidence of infection, stiffness, and myositis ossificans in open reduction. The anterior approach is the most widely used approach for open reduction mainly when vascular repair is necessary. The lateral approach is standard for elbow surgery but in supracondylar fracture increases the risk of radial nerve injury and stiffness. The bilaterotricipital posterior approach (Alonso-Llames approach) is not recommended as it has a high rate of complications described, such as stiffness, unsightly scarring and risk of trochlea osteonecrosis.
Physiotherapy Management[edit | edit source]
Physiotherapy treatment is vital in all patients with a supracondylar fracture to hasten healing and ensure an optimal outcome. The goal of physiotherapy treatment is:
- To achieve painless and full mobility of the elbow joint.
- To enhance healing process.
- To strength the affected musculature.
- To improve overall functional abilities of children.
Outcome measures that can be used to compare and evaluate the outcome of treatment are :
- Numerical pain rating scale (NPRS)/ Faces Pain Scale
- Range of motion- Goniometry
- Manual muscle testing ( MMT)
- ASK-p (Activities Scale for Kids-performance version)[8]
- Flynn's criteria include two factors 'cosmetic factor' (loss of carrying angle) and 'Functional factor' (motion loss in degrees).[9]
- Neuro-vascular assessment is must post-operatively and during rehabilitation.
Evidence[edit | edit source]
The physical therapy management in the pediatric population is very controversial, in both its effect and its necessity. A randomized controlled trial was done by Schmale et al. in 2014, had shown that children with supracondylar fracture treated with either casting or CR with percutaneous pining followed by casting were not benefited by a short course of physical therapy (six sessions of physical therapy performed over a five-week period beginning the week after cast removal) in terms of either return of function or motion.[8]Supporting the above study, another study was done in 2018, also shows that children managed with CR for uncomplicated supracondylar fracture with immobilization for three weeks regain their functional ROM within 12 weeks of mobilization by themselves, with no added benefit from physiotherapy.[9]
Physiotherapy treatment has not shown significant difference, it may be due to the involvement of children of a ( 5- 10 years) in more involved in daily household activities from an early period and urge for a motion for playing.[9] It would be either affected as the therapist may have been unduly aggressive or unduly conservative while providing treatment.[9][8]
On the contrary, in a more severe type of injury with neurovascular involvement and in an adult patient, physiotherapy treatment has a significant role.[8] And in the pediatric population, evidence has been lacking to address the strength of upper extremity as an outcome after physiotherapy treatment.
Therefore,
- Optimal loading(pain-free activities based on a child) is very necessary for the pediatric population with supracondylar fracture as pain aggravating activities may delay the healing process and cause further damage as they are in the growing phase.[8]
- Thus, active exercise and active involvement in sports and ADLs are recommended rather than passive joint mobilization and stretching exercises.[9]
- Those activities such as lifting, weight-bearing, or pushing activities that pose large amounts of stress through the humerus should also be avoided in the initial week after immobilization removable.[9]
- Progressive strengthening exercises can be addressed.
Advice and Exercises During the Immobilization Period[edit | edit source]
- Normally elbow is immobilized for 3 weeks so, during that period, adjacent joints ( Shoulder joint and wrist joint and hand) should be kept moving active or active-assisted exercises frequently in a day.
- Elbow shouldn't be moved and used of arm sling should be proper.
- Postural training( sitting upright with relaxed shoulder and retraction of the scapula) should be taught.
1-2 Weeks After Removal of Cast[edit | edit source]
- Hot fermentation can be used to ease joint stiffness.
- Gentle soft tissue release can be done in arm and forearm musculature.
- Gentle active and active-assisted exercises using a wand and be taught in pain- free limit- frequently in a day.
- Isometric exercises for arm and forearm musculature can be addressed.
- Educate parents and child to use the affected hand to use in daily activities like brushing, writing, eating, dressing, etc.
- Avoid weight lifting and pushing activities.
Advice and Exercise After 2 Weeks of Cast Removal[edit | edit source]
- Progressive and interactive range of motion exercise and strengthening exercise should be addressed eg: passing a ball, dressing and undressing clothes.
Conclusion[edit | edit source]
- Supracondylar fractures of the humerus are the most frequent fractures in children with a peak incidence at the ages of five to eight years.
- FOOSH is the most mechanism of injury of Supracondylar fracture of the humerus.
- The Neurovascular assessment is must pre and post-operatively.
- Closed reduction with percutaneous pinning is the recommended medical management for displaced fracture without neurovascular involvement.
- Active exercise is recommended in pediatric elbow fracture rather than passive treatment.
References[edit | edit source]
- ↑ 1.0 1.1 Gray H. Anatomy of the human body. Lea & Febiger; 1878.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 Kumar V, Singh A. Fracture supracondylar humerus: A review. Journal of clinical and diagnostic research: JCDR. 2016 Dec;10(12):RE01.
- ↑ 3.0 3.1 Zhang XN, Yang JP, Wang Z, Qi Y, Meng XH. A systematic review and meta-analysis of two different managements for supracondylar humeral fractures in children. Journal of orthopaedic surgery and research. 2018 Dec 1;13(1):141.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 Vaquero-Picado A, González-Morán G, Moraleda L. Management of supracondylar fractures of the humerus in children. EFORT open reviews. 2018 Oct;3(10):526-40.
- ↑ 5.0 5.1 Brubacher JW, Dodds SD. Pediatric supracondylar fractures of the distal humerus. Curr Rev Musculoskelet Med 2008;1:190-196.
- ↑ nabil ebraheim. Supracondylar Fractures Of The Humerus In Children. Available from: https://www.youtube.com/watch?v=Z46LtJko9SY [last accessed 22/6/2020]
- ↑ Alton TB, Werner SE, Gee AO. Classifications in brief: the Gartland classification of supracondylar humerus fractures.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 Schmale GA, Mazor S, Mercer LD, Bompadre V. Lack of benefit of physical therapy on function following supracondylar humeral fracture: a randomized controlled trial. The Journal of Bone and Joint surgery. American Volume. 2014 Jun 4;96(11):944.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 Jha SC, Shakya P, Baral P. Efficacy of Physiotherapy in Improving the Range of Motion of Elbow after the Treatment of Pediatric Supracondylar Humeral Fracture. Birat Journal of Health Sciences. 2018 Sep 5;3(2):432-6.