Resistant Hypertension
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
Resistant hypertension (RHTN) is defined as the failure to lower systolic and diastolic blood pressure in patients who follow appropriate lifestyle measures and are taking the optimal doses of three antihypertensive drugs from different classes, one of which is a diuretic. The goal blood pressure (BP) is usually defined as <140 mm/90 mm Hg and <130/80 mm Hg for patients with diabetes mellitus, renal dysfunction and high risk patients. eg post CVA[1].
RHTN is important to recognise because it places patients at risk of end-organ damage.[2]
Genetic variability in BP-regulating genes and pathways may partially account for the variability in BP response to antihypertensive agents and may contribute to the RHTN phenotype[3].
Genetic Phenotype[edit | edit source]
RHTN is a complex phenotype having a multifactorial etiology, with usually no single cause, but an interaction between several pathophysiological mechanisms. The three predominant pathological mechanisms being:
- Primary hyperaldosteronism: estimated to be present in 20 % of patients with RHTN. However those with out primary hyperaldosteronism demonstrate higher levels of aldosterone and volume overload than individuals without RHTN.
- Sympathetic hyperactivity: likely connected with volume overload in RHTN. Activation of the renin-angiotensin aldosterone system (RAAS) may constitute the mechanistic link between elevated aldosterone levels and the sympathetic hyperactivity.
- Excessive vascular inflammation, and endothelial dysfunction: resulting from a heightened sympathetic system and aldosterone levels.[4]
Recent genetic studies have identified or confirmed several chromosomal regions containing susceptibility alleles for essential hypertension[5]. However due to the complex nature of essential HTN single genes affecting BP variability remain difficult to isolate and identify and have rendered the development of single-gene targeted therapies challenging[6].
Future Prospects[edit | edit source]
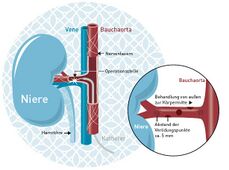
The successful management of resistant hypertension relies on lifestyle modification and the most effective medical therapy. Future developments in hypertension management, including a large number of new device-based therapies, are under active development. Renal denervation is the showing promise as a new therapy. Further study is needed before these devices can be recommended in the routine treatment of resistant hypertension[7].
References[edit | edit source]
- ↑ Fagard RH. Resistant hypertension. Heart. 2012 Feb 1;98(3):254-61.Available:https://heart.bmj.com/content/98/3/254 (accessed 13.7.2022)
- ↑ Yaxley JP, Thambar SV. Resistant hypertension: an approach to management in primary care. Journal of family medicine and primary care. 2015 Apr;4(2):193. Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4408700/#:~:text=extensive%20medical%20therapy.-,Resistant%20hypertension%20is%20defined%20as%20blood%20pressure%20that%20remains%20above,to%20suffer%20end%2Dorgan%20damage. (accessed 13.7.2022)
- ↑ El Rouby N, Cooper-DeHoff RM. Genetics of resistant hypertension: a novel pharmacogenomics phenotype. Current hypertension reports. 2015 Sep;17(9):1-1. Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4717470/ (accessed 13.7.2022)
- ↑ El Rouby N, Cooper-DeHoff RM. Genetics of resistant hypertension: a novel pharmacogenomics phenotype. Current hypertension reports. 2015 Sep;17(9):1-1. Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4717470/ (accessed 13.7.2022)
- ↑ Shih PA, O'connor DT. Hereditary determinants of human hypertension: strategies in the setting of genetic complexity. Hypertension. 2008 Jun 1;51(6):1456-64. Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2587105/ (accessed 13.7.2022)
- ↑ Ahn SY, Gupta C. Genetic programming of hypertension. Frontiers in pediatrics. 2018 Jan 22;5:285. Available: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5786744/ (accessed 13.7.2022)
- ↑ Pathan MK, Cohen DL. Resistant Hypertension: Where are We Now and Where Do We Go from Here?. Integrated blood pressure control. 2020;13:83. Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7415451/ (accessed 213.7.2022)