Psychosocial Considerations in Patellofemoral Pain
Top Contributors - Carin Hunter, Jess Bell, Ewa Jaraczewska, Kim Jackson and Wanda van Niekerk
Introduction[edit | edit source]
Patellofemoral pain is a common knee condition. It can cause pain around or behind the kneecap, and certain activities can exacerbate it. This is a complex condition and often difficult to treat. Anxiety, depression, and fear of movement may be elevated in individuals with patellofemoral pain. It correlates with pain and reduced physical function. Recent research highlights these psychosocial considerations that can negatively impact managing this condition.[1]
This article discusses psychosocial factors and how they can influence recovery in individuals with patellofemoral pain.
The Pain and Movement Reasoning Model[edit | edit source]
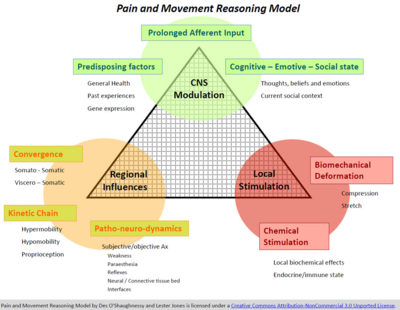
The Pain and Movement Reasoning Model is designed to improve clinical reasoning.[2] It aims to "capture the complexity of the human pain experience by integrating these multiple dimensions into a decision-making process."[3] As is shown in Figure 1, this model includes three categories.
- Local stimulation[3][4]
- Biomechanical stimulation
- Chemical stimulation
- Regional influences[3][4]
- Kinetic chain
- Patho-neurodynamics
- Convergence
- Central nervous system modulation[3][4]
- Prolonged afferent input
- Predisposing factors
- Cognitive - emotive - social state
Clinicians use the model to identify the most important category for each patient. Once identified, it can help to direct treatment. The model also enables clinicians to identify when there are changes in presentation and, thus, if a new/different treatment approach should be adopted.[3]
While the pain and movement reasoning model was not designed for patellofemoral pain, the theory can be effectively applied to patients with this condition.[5] Local stimulation in patellofemoral pain consists of bone oedema, fat pad swelling, effusion, retinacular ischaemic changes, bone bruising, or anything local at the knee. Regional influences include excessively pronating feet, an anteverted femoral neck or poor hip abduction control. There is not, however, much available research to show the role played by the central nervous system.
This video discusses pain and movement reasoning model presented by Jones and O'Shaughnessy and explains the complexity of the human pain experience:
Psychosocial Factors and Patellofemoral Pain[edit | edit source]
There is a general lack of research on the impact of psychosocial factors on patellofemoral pain, but they should not be ignored.[5]
Depression and Anxiety[edit | edit source]
Research by Wride and Bannigan[1] highlights important correlations between anxiety and depression and patellofemoral pain:
- The prevalence of anxiety and/or depression is higher in the patellofemoral population than the general population[1]
- The prevalence of anxiety and/or depression is higher in young females[1]
- Individuals with high anxiety scores were more likely to be female[1]
- The rate of patellofemoral pain is higher in females[7]
A systematic review by Maclachlan et al. [8]indicates that a group of adolescents with patellofemoral pain had three times the risk of anxiety and/or depression than healthy individuals. The following methods can be used to assess depression and anxiety:
Depression:
- Hospital Anxiety and Depression Scale (HADS): focus on non-physical symptoms, contains seven questions for anxiety and seven questions for depression, and takes 2–5min to complete.
- Arthritis Impact Measurement Scales: a self-administered outcome measure takes 15 minutes to complete and consists of nine sub-scales.
Anxiety:
- Arthritis Impact Measurement Scales
- Beck Anxiety Index (BAI)
- Hospital Anxiety and Depression Scale
- State-Trait Anxiety Inventory (STAI): self-report measure for anxiety [9], Y from is the most popular, comprises twenty items for assessing trait anxiety and twenty for state anxiety
Loss, Confusion and Fear-Avoidance Associated with Patellofemoral Pain[edit | edit source]
Smith et al.[10] conducted a qualitative study on the experience of living with patellofemoral pain and the associated sense of loss, confusion and fear avoidance. The full article is available here: The experience of living with patellofemoral pain-loss, confusion and fear-avoidance: a UK qualitative study.
Many patients with patellofemoral pain reported experiencing a loss of identity and a decrease in their social interactions. For example, if an individual has patellofemoral pain, which limits them from participating in their sport of choice, we need to remember that it is not only the activity/sport they are suddenly unable to participate in. They may also lose the sense of well-being and social interaction normally offered by the sport.
Thus, patellofemoral pain can have wide-ranging effects, and an individual's beliefs about their knee pain can cause them to make significant lifestyle adaptations.[5] For example, some individuals have reported feeling they might need to change their career aspirations[10] or their housing choices.[5]
Patients can battle with their understanding of the causes of their knee pain, especially when it is of insidious onset. Unlike a traumatic injury, knee pain of insidious onset is not marked by a specific event to which the pain can be attributed. This can lead to confusion, uncertainty and the incorrect assumption that exercise or activity worsens their pain.[10] When a physiotherapist then prescribes exercise-based treatment, a patient might be hesitant and/or non-compliant due to their belief that exercise caused their pain. Thus, the patient should be educated on the effects of load, repetitive volume, warm-up, cool-down, footwear, and the many other facets that are vital to understanding exercise.[5]
When study participants discussed treatments or 'coping strategies, many focused on rest and postural adjustments, such as avoiding flexion in sitting. They also felt that passive treatments, such as pain medication and knee supports, would be of benefit.[10] While these might help the pain temporarily, they will not be beneficial to the patient in the long term.[5]
Psychologically-Informed Treatments[edit | edit source]
A study by Selhorst et al.[11] offers insight into how psychologically informed treatments may benefit adolescents with patellofemoral pain. The study group were shown an educational video which focused on pain-related fear and pain catastrophising. Compared to the control, the study group showed a reduction in kinesiophobia, catastrophisation and pain scores immediately and at two weeks. This highlights the significance of education in patellofemoral pain.
Sleep[edit | edit source]
In patients with patellofemoral pain, it is also important to consider their sleep patterns, including the quantity/duration of sleep and the quality of sleep. When conducting an assessment, we should consider asking questions such as, "How many times do you wake up in the night? How long does it take to get to sleep?"[5]
Patient's sleeping position can impact the symptoms associated with patellofemoral pain syndrome:
- can place unnecessary stress on the knees, increasing pain and discomfort, or
- can alleviate pressure on the patella and promote better sleep quality.The following positions are recommended:[12]
- position on the back with a pillow or rolled-up towel under your knees to reduce stress on the patella
- position on the side with a pillow between your knees to minimise the strain on the patella
- Semi-fetal position involves sidling and drawing knees slightly towards the chest with a pillow between the knees to support and reduce knee pressure.
- sleeping with the leg propped on the wedge to reduce swelling and improve circulation
Mindfulness[edit | edit source]
Research carried out by Bagheri et al.[13] showed that when mindfulness was included with physical treatments, there was a greater improvement in pain reduction, catastrophisation and kinesiophobia in female runners with patellofemoral pain. Mindfulness aims to increase awareness of thoughts, sensations and emotions with acceptance, curiosity and openness.[13] The focus of mindfulness is to reduce stress, take control of the situation, stay in control, and not be overly alarmed by it.
Some patients might be resistant to mindfulness practice, which may necessitate a measure of convincing them to engage in it. Hence, approaching it according to the following steps might result in better acceptance:
- Mindfulness practice should be introduced in a gentle, non-judgemental and open way
- Exploring mindfulness can start with bare awareness to simple breathing.[14] Incorporate easy breathing techniques into the patient’s daily routine/exercise programme while asking them to pay attention to their breath - feeling the breathing in and breathing out, the rise and fall of the abdomen, the “touch of air at the nostrils.”[14]
- The simple breathing exercises can be progressed to more specific breathing techniques such as the “3-minute breathing space”[14], “4-7-8 breathing” and “box breathing.”[15]
- Provide patients with handouts and additional resources to increase their knowledge
- Engage patients in guided meditations performed either by a therapist or through the use of mindfulness applications available online or on smartphones (Apps)
- Help patients find structured or community mindfulness programmes (i.e. 6-14 week programmes)
- Encourage patients to engage in mindfulness practice long-term for maximal benefit. [16]
You can learn more about mindfulness for patients here.
Rehabilitation therapists often focus on reducing pain. However, if a patient is discharged from treatment with incorrect beliefs about their knee pain, they could continue to fear avoidance behaviours and experience anxiety while playing sports.[17] Thus, it is important to address both psychosocial and physical factors.
Tampa Scale of Kinesiophobia[edit | edit source]
Kinesiophobia is a fear of painful movement, which leads to activity limitation.[18]A cognitive behavioural therapy helps to reduce cognitive biases and modify kinesiophobia. [18]The Tampa Scale of Kinesiophobia (TSK) helps to quantify the fear of movement and can be a useful measure in patellofemoral pain.[5]
The TSK was first developed in 1990 by R. Miller, S. Kopri, and D. Todd. It is a 17-item self-report questionnaire which evaluates fear of movement, fear of physical activity, and fear avoidance. It was first developed to distinguish between "non-excessive fear and phobia"[19] in patients with chronic musculoskeletal pain, specifically chronic low back pain. It is now widely used for different parts of the body.[19]The short form of TSK (TSK-4) is a reasonable substitute for the full TSK. It is recommended as a brief screening measure in patient care to assess the influence of kinesiophobia on lower extremity-specific limitations.[18]
Links:
- Tampa Scale of Kinesiophobia
- Tampa Scale of Kinesiophobia (TSK) pdf
- MDApp, Tampa Scale of Kinesiophobia
Addressing Psychosocial Factors[edit | edit source]
Psychosocial factors are predictors of negative outcomes in musculoskeletal pain conditions. They should also be considered in patellofemoral pain as these patients demonstrate increased levels of emotional distress and kinesiophobia when compared with the general population. [20]
Psychosocial Factors[edit | edit source]
- Depressive symptoms[21]
- Higher levels of anxiety[21]
- Fear avoidance
- Lifestyle changes
- Kinesiophobia[11][13]
- Catastrophisation[11][13]
- Increased emotional distress [20]
- Low self-efficacy (personal judgement on the ability to perform an activity or meet a challenge) [22]
Questions to ask[edit | edit source]
| Question | Reason | Treatment Implication |
| Duration of symptoms? | The longer the duration, the more likely there will be central pain changes | Assess for central changes |
| Alteration in sleep quality? | Serotonin (natural painkiller) production suppressed with poor sleep | Recommend re-establishing routine;
Non-painful exercise; Decrease anxiety through education. |
| Change in exercise profile? | Can affect sleep, mood, self-esteem, social interactions and conditioning | Consider exercise programmes for non-painful body parts initially;
Education to minimise fear-avoidance |
| Can they tolerate the sense of clothing on their knee, e.g. skinny jeans/tights? | Some patients cannot bear the feeling of material on their knee - this is highly suggestive of non-mechanical pain | Graduated exposure;
May need medical management to de-sensitise |
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Wride J, Bannigan K. Investigating the prevalence of anxiety and depression in people living with patellofemoral pain in the UK: the Dep-Pf Study. Scandinavian Journal of Pain. 2019 Apr 1;19(2):375-82.
- ↑ Jones LE, Heng H, Heywood S, Kent S, Amir LH. The suitability and utility of the pain and movement reasoning model for physiotherapy: A qualitative study. Physiother Theory Pract. 2021:1-14.
- ↑ 3.0 3.1 3.2 3.3 3.4 Jones LE, O'Shaughnessy DF. The pain and movement reasoning model: introduction to a simple tool for integrated pain assessment. Manual therapy. 2014 Jun 1;19(3):270-6.
- ↑ 4.0 4.1 4.2 O’Shaughnessy D, Jones LE. Making sense of pain in sports physiotherapy: applying the Pain and Movement Reasoning Model. A Comprehensive Guide to Sports Physiology and Injury Management: An Interdisciplinary Approach. 2020 Nov 13:107.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 Robertson C. Psychosocial Considerations in Patellofemoral Pain Course. Plus. 2022.
- ↑ Claire Patella. Claire Patella's top tips pain&reasoning model. Available from: https://www.youtube.com/watch?v=YuQALRxhVVo [last accessed 31/08/2022]
- ↑ Boling M, Padua D, Marshall S, Guskiewicz K, Pyne S, Beutler A. Gender differences in the incidence and prevalence of patellofemoral pain syndrome. Scandinavian journal of medicine & science in sports. 2010 Oct;20(5):725-30.
- ↑ Maclachlan LR, Collins NJ, Matthews MLG, Hodges PW, Vicenzino B. The psychological features of patellofemoral pain: a systematic review. Br J Sports Med. 2017 May;51(9):732-742.
- ↑ Pretorius TB, Padmanabhanunni A. Anxiety in Brief: Assessment of the Five-Item Trait Scale of the State-Trait Anxiety Inventory in South Africa. Int J Environ Res Public Health. 2023 May 1;20(9):5697.
- ↑ 10.0 10.1 10.2 10.3 Smith BE, Moffatt F, Hendrick P, Bateman M, Rathleff MS, Selfe J, et al. The experience of living with patellofemoral pain-loss, confusion and fear-avoidance: a UK qualitative study. BMJ Open. 2018;8(1):e018624.
- ↑ 11.0 11.1 11.2 Selhorst M, Fernandez-Fernandez A, Schmitt L, Hoehn J. Effect of a Psychologically Informed Intervention to Treat Adolescents With Patellofemoral Pain: A Randomized Controlled Trial. Archives of Physical Medicine and Rehabilitation. 2021 Jul 1;102(7):1267-73.
- ↑ Patellofemoral pain syndrome sleeping position. Available from https://vocal.media/lifehack/patellofemoral-pain-syndrome-sleeping-position [last access 31.10.2023]
- ↑ 13.0 13.1 13.2 13.3 Bagheri S, Naderi A, Mirali S, Calmeiro L, Brewer BW. Adding mindfulness practice to exercise therapy for female recreational runners with patellofemoral pain: A randomized controlled trial. Journal of Athletic Training. 2021 Aug 1;56(8):902-11.
- ↑ 14.0 14.1 14.2 Shapiro SL, Carlson LE. The art and science of mindfulness: Integrating mindfulness into psychology and the helping professions. 2nd ed. Washington, DC: American Psychological Association; 2017.
- ↑ Shrey Vazir. Mindfulness for Patients. Plus Course. 2021
- ↑ Zeidan F, Baumgartner JN, Coghill RC. The neural mechanisms of mindfulness-based pain relief: a functional magnetic resonance imaging-based review and primer. Pain reports. 2019 Jul;4(4).
- ↑ Smith IV BN. Resiliency, Generalized Self-Efficacy and Mindfulness as Moderators of the Relationship between Stress and Life Satisfaction and Depression among College Students: An Investigation of the Resilience Process. 2017.
- ↑ 18.0 18.1 18.2 Kortlever JTP, Tripathi S, Ring D, McDonald J, Smoot B, Laverty D. Tampa Scale for Kinesiophobia Short Form and Lower Extremity Specific Limitations. Arch Bone Jt Surg. 2020 Sep;8(5):581-588.
- ↑ 19.0 19.1 Hudes K. The Tampa Scale of Kinesiophobia and neck pain, disability and range of motion: a narrative review of the literature. The Journal of the Canadian Chiropractic Association. 2011 Sep;55(3):222.
- ↑ 20.0 20.1 Hott A, Pripp AH, Juel NG, Liavaag S, Brox JI. Self-efficacy and Emotional Distress in a Cohort With Patellofemoral Pain. Orthop J Sports Med. 2022 Mar 8;10(3):23259671221079672.
- ↑ 21.0 21.1 Alabajos-Cea A, Herrero-Manley L, Suso-Martí L, Alonso-Pérez-Barquero J, Viosca-Herrero E. Are psychosocial factors determinant in the pain and social participation of patients with early knee osteoarthritis? A Cross-Sectional Study. International Journal of Environmental Research and Public Health. 2021 Apr 26;18(9):4575.
- ↑ Bandura A. Self-efficacy: toward a unifying theory of behavioural change. Psychol Rev. 1977 Mar;84(2):191-215