Prosthetics for Individuals with Hip Disarticulation and Hemipelvectomy Amputations
Original Editor - Tarina van der Stockt
Top Contributors - Martina Lukin, Wanda van Niekerk, Kim Jackson, Tarina van der Stockt and Simisola Ajeyalemi
Introduction[edit | edit source]
Hip disarticulation (HD) and Hemipelvectomy (HP) are the most proximal amputations of the lower extremity. Although the two amputation levels are similar in appearance they feature important anatomical differences; Whilst a HD is performed directly through the hip joint, a HP includes removal of the entire hip joint along with a section of the pelvis on the same side[1].
Both HD and HP are very extensive amputations, most commonly performed due to malignant tumours[1]. Less frequently, they are also performed following severe trauma, vascular disease (vascular insufficiency), femoral osteomyelitis and other factors [1]. Both levels are not common and account for less than 1% of all amputations [2][3].
Because of the extent of HD and HP amputations, they can significantly impact functional mobility and independence. Coupled with an increased likelihood of chronic pain and skin complications[2], individuals with these proximal amputation levels tend to experience the most difficulty in activities such as walking, rising and sitting down and climbing stairs[1][4].
Despite the challenges associated with rehabilitation, prosthetic fitting for HD and HP amputees should not be discouraged[5]. Modern advancements in prosthetic design have seen the development of lighter and more functional lower limb components, including some specifically designed for HD and HP prostheses. Socket designs have also evolved to incorporate more modern interface materials such as silicone, that conform more closely to the individual's anatomy thus providing improved fit and comfort for the prosthetic user. HD and HP prostheses, particularly those incorporating modern designs and components, can help restore functional mobility to a higher level as well as benefit a more diverse demographic of amputees[5].
Requirements for Successful Prosthetic Function[edit | edit source]
Active Pelvic Lordosis[edit | edit source]
Due to the type of amputation, there is no residual limb left and thus no lever to control the prosthesis during gait. As a result, the main mechanism used by the prosthetic user to initiate knee flexion during gait is pelvic lordosis. To ensure successful prosthetic fitting, the prosthetic user must be able to achieve good lordotic range of motion through active use of the lower back and abdominal musculature[3].
Single leg balance[edit | edit source]
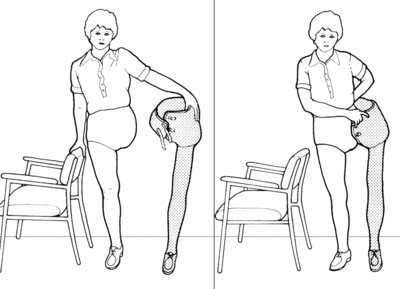
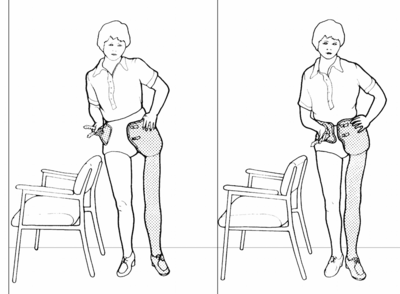
Ability to balance on the sound leg is essential for the prosthetic user to be able to donn and doff the prosthesis independently[3]. An overall good sense of balance may also allow the user to ambulate without using additional gait aids such as crutches. The images below are shared with permission from Engstrom et al in Therapy for Amputees.[8]
Ability to contain abdominal soft tissue[edit | edit source]
The HD socket must fit firmly and encompass all of the soft tissue in the abdominal region to enable more effective transfer of forces during gait, increase stability and capture lordosis more effectively[3]. Although not a strict requirement, individuals with firmer muscle tone tend to have more successful prosthetic outcomes at this level[3].
Prosthetic Design and Components for Hip Disarticulation and Hemipelvectomy[edit | edit source]
Despite the physical differences between HP and HD amputation levels, the prosthetic components and prosthetic design for the two levels is the same[9].
The current standard is based on the Canadian hip disarticulation prosthesis, a design originally pioneered in the 1950s by McLaurin[10][3][4]. This type of HP prosthesis features a prosthetic hip joint mounted anteriorly on the socket, and below the level of the anatomical hip joint. This joint positioning is in contrast to older HP prosthesis designs which mounted the hip joint laterally and in line with the anatomical hip position of the sound side.
A major challenge of the HD prosthesis is to ensure adequate safety and stability for the user while still enabling functionality (i.e. knee and hip flexion during swing and stance phase). Thus the key advantage of the Canadian hip disarticulation prosthesis is that the overall stability can be influenced by the prosthetic alignment[3], or the relationship between the position of the hip, knee and foot components. Placing the hip joint anteriorly on the socket brings the centre of gravity further anteriorly and allows it to fall in front of the knee joint, thus providing passive stability at both the hip and knee joints during standing[4].
Other factors affecting stability include the type of components used and how they function in combination with each other. A thorough physical assessment of the individual is essential as it can help can guide the selection of components, with careful consideration to the their personal requirements and activity level.
Another method to help aid stability is to shorten the overall length of the prosthesis by approximately 1cm compared to the contralateral limb. This allows for additional toe clearance during the swing phase of gait, although depending on the components used, this compensation may not always be necessary [9][4].
Prosthetic Socket and Suspension[edit | edit source]
The primary functional goals of the HP prosthetic socket are to:
- Define anatomical surfaces and provide the mechanism for weight transfer from the trunk to the prosthetic limb. A total embracing socket is made by taking a plaster cast of the individual's pelvis and iliac crests[8]. The cast is later modified to ensure that the inside of the socket or socket interface conforms well to the individual's anatomy and that all major weight-bearing surfaces are captured accurately [3][9]. Weight-bearing within the socket occurs at the ischial tuberosity and gluteals of the sound limb for HP, and the ischium and gluteals of the amputated side for a HD amputation.
- Provide mediolateral stability. This is achieved by ensuring the socket conforms well to the individual and fits firmly over the iliac crests and over the greater trochanter[3]. A firmly fitting socket also feels much lighter and requires less effort when walking [9].
- Provide suspension during the swing phase of gait. The socket extends proximally over the iliac crests and locks in tightly above them. This provides the main suspension mechanism of the prosthesis. Padding or relief is added in the bony crest region to ensure comfort while still enabling the socket to be tightened firmly[3].
- To capture biomechanical movements. Abdominal flexion and pelvic lordosis are the key movements of the trunk that enable prosthetic function[3].
In addition to these functional goals, it is important that the socket be comfortable for the user. It has been reported that socket comfort significantly improves user acceptance and increases prosthesis wear times[9]. Comfort can be improved by providing pressure relief inside the socket for the pubic bone, head of femur as well as any other sensitive areas identified during the initial assessment[3]. Pressure relief is added during socket fabrication by leaving a small space inside the socket on or around sensitive areas or incorporating softer padding materials.
Socket casting and fabrication[edit | edit source]
There are 2 main ways of taking a plaster impression for a HP / HD socket; Using forming blocks, where the individual is required to simulate the final weight bearing position[9] or by the total suspension casting method.
- Socket casting using forming blocks
Two forming blocks are placed facing each other on a weight-bearing platform or standing frame, spaced far enough apart to allow the individual to rest the amputated side in between them. The inner sides of the blocks are angled at 45 degrees and help to shape the anterior and posterior surfaces of the socket.
The posterior block is placed underneath the gluteus. The anterior block forms the flat surface that is used to attach the hip connector and is positioned according to the required placement of the hip joint.
Forming blocks work well for individuals with good muscle tone and less soft tissue in the abdominal and pelvic areas. If there is excessive soft tissue, the forming blocks will push it out sideways thus expanding the medio-lateral width of the socket and requiring additional modification during socket fabrication[3].
- Total suspension casting
Total suspension casting is the method of choice for individuals with more soft tissue and less muscle tone. Although soft tissue is contained more effectively within the suspension mechanism, there is still a tendency for the soft tissues to bulge anteriorly. This makes hip joint positioning more challenging later in the socket fabrication process[3].
In some cases, it is desirable to use both total suspension and forming blocks in combination. This is beneficial to help contain the soft tissue as well as define the anterior and posterior surfaces of the socket[3][9]. Regardless of the chosen casting method, care should be taken to:
- Define and accentuate the iliac crests to ensure adequate suspension[3][9].
- Ensure a close and accurate impression of the thoraco-lumbar region. This will help prevent any unwanted shifting and pistoning movements inside the socket during walking[3].
- Reduce the overall volume of the cast. As the final step in the casting process, the anterior panel of the cast is cut open after which the individual reclines backwards and the cast opening is re-tightened as much as possible. This step is not essential but can help ensure a firmer fitting socket.
Socket Materials[edit | edit source]
The socket can be made from different types of materials. Most commonly are thermoformable plastics or lamination. Thermoplastics come in a greater variety of options and are easier to fabricate, however they result in a thicker and heavier socket[3] that is generally less durable. Laminated sockets are stronger and can be made with varying degrees of stiffness depending on the users anatomy and stability requirements[9]. There is also a trend towards integrating softer and more flexible materials in the interface including flexible copolymer plastic sleeves or silicone to improve user comfort[9].
There are various HP socket designs currently in use, however the most common socket features an anterior opening with adjustable Velcro straps. The straps allow for tightening, volume adjustment, ML support and prevent AP migration of the socket[3].A shoulder strap can be added to provide additional suspension[8].
Hemipelvectomy Prosthesis Components / Joints[edit | edit source]
Hip Joints[3][8][edit | edit source]
Hip Limiter
This is a mechanism attached on the front of the socket that allows movement of the hip in swing phase. The limiter controls movement that can be adjusted to increase or decrease step length as the individual becomes more active. A locking mechanism can be attached if required by the individual.
Endoskeletal or Modular designs
Double anterior and posterior free motion hinges that allow for hip extension by means of rubber bands, and a manual hip lock. It is relatively lightweight. Sitting is difficult due to the distal components.
Four-bar or polycentric joint
Four-bar knee mechanism mounted upside down is a popular option for the hip joint in a HP Prosthesis[4]. The inherent design of the four-bar joint shortens the prosthesis during the swing phase thus enabling a smoother walking pattern as a result of the increased toe clearance. It also has adjustable swing and stance phase resistance, provides greater stability at heel-strike, and a low profile during sitting[9].
The Helix 3D Prosthetic Hip is an example of a more modern polycentric hip joint. This hip leads to a more natural gait pattern by providing three dimensional motion during stance and swing phase with additional hydraulic dampening or shock absorption. It functions more effectively when paired with specific microprocessor knees, allowing the user to easily navigate environmental obstacles such as inclines and stairs.
Knee joints[edit | edit source]
The choice of knee joint for a HD / HP Prosthesis applies the same considerations as for transfemoral or above-knee amputees. Read more about prosthetic knees using this link.
Single-axis knee joint
These types of knees are lightweight, durable and relatively inexpensive thus making them a good choice for HD Prostheses[3][9]. Single-axis knee joints utilise an internal, adjustable friction control mechanism to provide stability and are considered best for those with a single speed of walking[3].
Stance control knee joint
Also known as 'safety knees', these joints offer a high level of stability and are generally not recommended for HD prosthesis as they may prevent knee flexion and thus impede normal gait motion[3]. They may however, be considered for the novice amputee particularly as they are learning to transition from swing to stance phase because the knee mechanism will not buckle even when it is not in full extension[9]. The stance control knee should not be used for bilateral amputees[9].
Four-bar or polycentric joint
Although slightly heavier than single axis knee joint, polycentric knees are a good choice for HD Prostheses as they provide maximum stability during stance phase coupled with shortening of the limb during swing phase[3][9]. This inherent shortening during swing phase allows for the length of prosthesis to be made in accordance with the sound side. Polycentric knees are recommended for higher activity prosthetic users and are also the best choice for bilateral amputees.
Hydraulic knee joint
Hydraulic knees are not often used because of the increased weight but it may be chosen to help initiate hip flexion during the swing phase of gait. It has been demonstrated that hydraulic knees used in a HD prosthesis can significantly improve the flexion range of motion at the hip and knee joint joints and allow for faster walking speeds[9].
Microprocessor controlled knee joint
Despite the increased weight and cost, microprocessor control knees are a popular option as they offer improved functionality and smoother walking patters over a range of different terrains and walking speeds. Even just applying a microprocessor knee as part of the prosthesis can reduce energy expenditure during gait[15].
Hybrid knee joint
Hybrid knees incorporate pneumatic swing phase control within a polycentric knee unit. These joints are becoming increasingly common due to the added functionality of swing phase control which support a wider variety of walking speeds and activity levels of the prosthetic user[9].
Prosthetic Feet[edit | edit source]
Different prosthetic feet can be used for HD / HP prostheses and should be chosen based upon the requirements of the individual user. Important considerations when selecting the prosthetic foot include:
- The weight of the foot. It is desirable to keep the weight as low as possible to reduce energy expenditure and ease of walking.
- The cost of the foot. More modern and complex designs tend to be more expensive and may not necessarily add functionality.
- How the foot interacts with the remaining components, particularly with the knee joint, to either enhance or reduce stability. Feet with a softer forefoot used in combination with a polycentric or four-bar knee joint will enhance knee stability, while those with a harder forefoot will reduce knee stability during late stance phase of gait[9].
Feet most commonly used with a HD/HP prosthesis include:
SACH feet
Traditionally, the Canadian hip disarticulation prosthesis design recommends use of the SACH or 'Solid ankle Cushion Heel' foot. SACH feet have a softer heel than other types of feet which enhances knee joint stability thus making is a desirable option[9].
Dynamic Response feet
Are often used for individuals with higher activity levels. They incorporate a carbon fibre keel or inner which is designed to mimic the natural feeling of ‘push off’ and therefore allow for faster walking speeds[9]
Read more about Prosthetic Feet using this link.
Additional components for Hemipelvectomy Prostheses[edit | edit source]
Rotation Adapters
are attached below the knee mechanism to enable rotation of the leg section. This allows for a more comfortable and natural sitting position, particularly for cross-kegged sitting. It is also useful for easy donning and doffing of shoes while still wearing the prosthesis.
Torque absorber – Used to reduce the rotational forces transferred from the socket to the prosthesis during the stance phase of gait. They also reduce impact during the initial stance phase or heel strike.
Challenges associated with Hip disarticulation and hemipelvectomy prosthesis[edit | edit source]
It has been well documented that HD Prosthetic users are able to achieve a high level of activity and participation despite the complexities associated with prosthetic design, fitting and the rehabilitation process [1][5]. Nevertheless, there are several challenges that may arise, generally due to the prosthesis itself or issues associated with the amputation.
Low rates of prosthetic use
The most common reason for low rates of use is a poorly fitting and uncomfortable socket[19]. Low rates of prosthetic use have also been linked to age. Younger amputees tend to utilise the socket for longer periods throughout the day whilst older amputees may find the weight of the prosthesis, coupled with increased energy requirements for ambulation more problematic.
It has also been suggested that cause of amputation may play a role in influencing prosthetic use; amputees due to cancer are healthier and stronger than those due to vascular complications therefore allowing them to more readily and use the prosthesis[1][5][20]
High Rejection Rates
There are many reasons why HD and HP amputees may choose to discontinue use of their prosthesis. One of the most common reasons is the sharp increase in energy requirements during ambulation, which have been reported to be up to 200% more than for non-amputees[9]. In contrast, using crutches without the prosthesis requires only 45% more energy compared to non-amputees, thus leading many individuals to use crutches as their primary means of ambulation[21]
As for low rates of prosthetic use, the type of amputation and socket comfort are both highly influential in determining successful prosthetic fitting[4][19]. In addition, individual factors such as balance and ability to control the prosthesis are considered crucial with those that are able to donn the prosthesis independently and walk without walking aids observed to be more likely to become active users[3][4][19].
Overloading upper extremity[1]
For individuals using the prosthesis with the support of crutches may have a tendency to overload the upper limbs. This can be addressed with proper gait training and ensuring a well fitting socket that enables effective weight transfer to the lower limb.
Skin problems
As the cause of amputation is rarely due to vascular disease, skin problems primarily occur due to poorly fitted socket, or overuse[1]. It is generally recommended to wear the prosthesis for less than 8 hours per day.
While these problems have been addressed to some extent by using modern componentry and socket materials as well as more dynamic designs[3], it is still important for the prosthetic user to undergo adequate rehabilitation and learn to monitor the skin regularly in order to ensure successful prosthetic use.
Having access to peer support groups or individual mentors, may also be useful in setting realistic rehabilitation goals and expectations that can then lead to more successful outcomes. The HP and HD amputation levels are rare and there is less information available about the prosthesis and the challenges that may arise for the user. Peer support groups can thus be invaluable sources of information for both the prosthetic user and their families.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Yari P, Dijkstra PU, Geertzen JH. Functional outcome of hip disarticulation and hemipelvectomy: a cross-sectional national descriptive study in the Netherlands. Clinical Rehabilitation. 2008 Dec;22(12):1127-33
- ↑ 2.0 2.1 Huffman A, Schneeberger S, Goodyear E, West JM, O'Brien AL, Scharschmidt TJ, Mayerson JL, Schulz SA, Moore AM. Evaluating hip disarticulation outcomes in a 51-patient series. Journal of Orthopaedics. 2022 May 1;31:117-20.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 3.23 3.24 3.25 Stark G. Overview of hip disarticulation prostheses. JPO: Journal of Prosthetics and Orthotics. 2001 Jun 1;13(2):50-3.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Gholizadeh H, Baddour N, Botros M, Brannen K, Golshan F, Lemaire ED. Hip disarticulation and hemipelvectomy prostheses: A review of the literature. Prosthetics and Orthotics International. 2021 Oct 1;45(5):434-9
- ↑ 5.0 5.1 5.2 5.3 Kralovec ME, Houdek MT, Andrews KL, Shives TC, Rose PS, Sim FH. Prosthetic rehabilitation after hip disarticulation or hemipelvectomy. American Journal of Physical Medicine & Rehabilitation. 2015 Dec 1;94(12):1035-40
- ↑ Chandler Balkman. Hip disarticulation prosthetic gait demonstration 2022. Available from: https://www.youtube.com/watch?v=bSq-tirpTIM [last accessed 9/7/2022]
- ↑ prostheticsinmotion. Hip Disarticulation Amputee Excels with the Otto Bock Helix Hip Joint. Available from: https://www.youtube.com/watch?v=U77D-J46cnU [last accessed 9/7/2022]
- ↑ 8.0 8.1 8.2 8.3 Engstrom B, Van de Ven C, editors. Therapy for amputees. Elsevier Health Sciences; 1999
- ↑ 9.00 9.01 9.02 9.03 9.04 9.05 9.06 9.07 9.08 9.09 9.10 9.11 9.12 9.13 9.14 9.15 9.16 9.17 9.18 9.19 9.20 Van der Waarde T, Michael J. Hip Disarticulation and Transpelvic Amputation: Prosthetic Management. Atlas of Limb Prosthetics: Surgical, Prosthetic, and Rehabilitation Principles. 2002.
- ↑ Solomonidis SE, Loughran AJ, Taylor J, Paul JP. Biomechanics of the hip disarticulation prosthesis. Prosthetics and Orthotics International. 1977 Apr;1(1):13-8.
- ↑ Stark G. Overview of hip disarticulation prostheses. JPO: Journal of Prosthetics and Orthotics. 2001 Jun 1;13(2):50-3.
- ↑ Stark G. Overview of hip disarticulation prostheses. JPO: Journal of Prosthetics and Orthotics. 2001 Jun 1;13(2):50-3.
- ↑ Cale Konetchy. Ottobock Hip Casting Video. Available from: https://youtu.be/rRRXhef_0iM [last accessed 9/7/2022]
- ↑ Martin Bionics. Bikini of Hip Sockets Hammock Casting Stand Explained. Available from: https://youtu.be/rFIs9BOU2bU [last accessed 9/7/2022]
- ↑ Ueyama Y, Kubo T, Shibata M. Robotic hip-disarticulation prosthesis: evaluation of prosthetic gaits in a non-amputee individual. Advanced Robotics. 2020 Jan 2:1-8.
- ↑ Chandler Balkman. Helix Hip. Available from: https://youtu.be/668uiI0arN0
- ↑ crystald563. Crystal's prosthesis for hip disarticulation. Available from: https://www.youtube.com/watch?v=9G1rvk_Dt50
- ↑ POACFL. NPS Prosthesis for Hip Disarticulate / Hemipelvectomy Amputees. Crystal's prosthesis for hip disarticulation. Available from: https://youtu.be/soAB8qHl890
- ↑ 19.0 19.1 19.2 Fernandez A, Formigo J. Are Canadian prostheses used? A long-term experience. Prosthetics and orthotics international. 2005 Aug;29(2):177-81.
- ↑ Denes Z, Till A. Rehabilitation of patients after hip disarticulation. Archives of orthopaedic and trauma surgery. 1997 Oct;116(8):498-9.
- ↑ Nowroozi F, Salvanelli ML, Gerber LH. Energy expenditure in hip disarticulation and hemipelvectomy amputees. Archives of physical medicine and rehabilitation. 1983 Jul 1;64(7):300-3.

![Casting blocks HP prosthesis[11]](/images/thumb/4/4f/Casting_blocks_HP_prosthesis.jpg/400px-Casting_blocks_HP_prosthesis.jpg)
![Forming blocks positioning[12]](/images/thumb/9/98/Forming_blocks_positioning_Stark.png/208px-Forming_blocks_positioning_Stark.png)