Physiotherapy Management of the Elbow
Introduction[edit | edit source]
Physiotherapy has an important role to play in the management of pain and dysfunction around the elbow joint. Physiotherapists have a functional knowledge of the complicated 3-joint elbow complex as well as its associated anatomy. They can apply this knowledge to the various structures around the elbow as well as distant from the elbow that can contribute to a person's symptoms.
A physiotherapist can perform a detailed assessment of the elbow and identify all contributing factors as well as co-morbidities associated with the person's symptoms. This assessment will help them develop a multi-modal treatment approach that is individualised to the specific problems and contributing factors found in the assessment.
The Complex Anatomy of the Elbow[edit | edit source]
The elbow joint is where the distal humerus meets the proximal radius and ulna bones. It is known as a trochleogingylomoid joint as it can flex and extend as a hinge (ginglymoid) joint as well as pivot around an axis (trochoid motion), which is known as pronation and supination.[1][2] It is an extremely congruent and stable joint. Due to its complexity, even after severe injury, it is more prone to stiffness[3] than instability.
Joints[edit | edit source]
The humerus, radius and ulna articulate to form 3 joints that make up the elbow.
Ulnohumeral Joint
The ulnohumeral hinge joint is responsible for flexion and extension. The spool-shaped trochlea of the humerus articulates with the greater sigmoid arch of the proximal ulna.[1]
Radiocapitellar Joint
The radiocapitellar joint is where the radius and humerus articulate. It is partly responsible for pronation and supination. The capitellum of the lateral distal humerus is a spherical structure onto which the concave surface of the proximal radial head articulates.[2]
Proximal Radioulnar Joint
The proximal radioulnar joint is a trochoid joint responsible for pronation or supination of the forearm. The peripheral edge of the radial head articulates with the radial notch of the ulna.[2]
Carrying Angle
The carrying angle of the elbow is the angle made by the arm and forearm in full extension and supination.[4] It is an angle measured along the long axis of the humerus and ulna. In men, it is approximately 11-14° and women 13-16°. Is it appropriately named as it allows our arms to clear our hips as we walk and allows objects to be carried.
Movements at the Elbow[edit | edit source]
Flexion and Extension
Flexion and extension occur at the ulnohumeral joint. The normal range of movement is from 0-140° but only 30°-130° is required for most activities of daily living (ADL).[1]
Pronation and Supination
The radiocapitellar joint and proximal radioulnar joint are responsible for pronation and supination. Normal ROM is considered approximately 180° (80°-90° pronation and 90° supination). 100° of movement (50° pronation and 50° supination) is considered adequate for most ADLs. If pronation ROM is lost this can be compensated by using shoulder abduction. But, there is no compensatory action for supination and as such a loss of supination ROM can pose a greater disability than a loss of pronation ROM.[1]
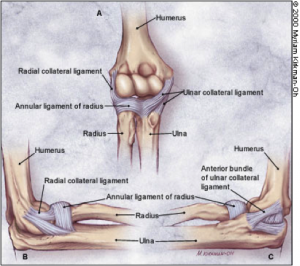
Ligaments and Capsule[edit | edit source]
There are 2 main ligament complexes at the elbow namely the Medial and Lateral Collateral.
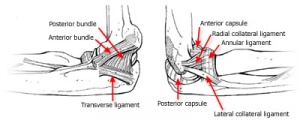
Medial Collateral Ligament Complex (MCLC)
The MCLC is comprised of the anterior bundle, posterior bundle and transverse ligament (the ligament of Cooper). The anterior bundle is considered to be the most important stabiliser of the elbow and provides valgus and posteromedial stability.[2] The anterior bundle is further divided into the anterior and posterior bands. The anterior band is more taught in extension and relaxes into flexion and the posterior band is taught in flexion and releases in extension.[2] This makes the anterior band more vulnerable to valgus stress when the elbow is extended and the posterior band of the AMCL more vulnerable to valgus stress when the elbow is flexed.[1]
Lateral Collateral Ligament Complex (LCLC)
The LCLC is the primary stabiliser against varus and external rotation stresses. The lateral ulnar collateral ligament, the radial collateral ligament and the annular ligament form the LCLC.[5] The lateral ulnar collateral ligament is important in maintaining posterolateral rotatory stability as well as stabilising against varus stresses.[5] The radial collateral ligament also contributes to posterolateral rotational stability. The Annular ligament surrounds the radial head but does not attach to it. It is am important stabiliser of the proximal radioulnar and radiocapitellar joint.[5]
Joint Capsule
The joint capsule of the elbow surrounds all 3 joints[5][2]. There are thickening medially and laterally of the joint capsule that blends with the MCLC and LCLC respectively and contributes to the stability of the elbow.[2][5]
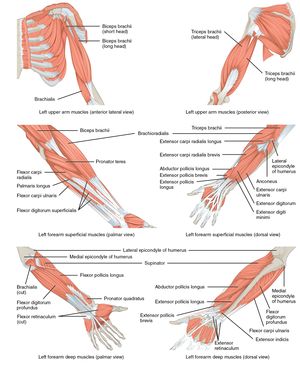
Musculature[edit | edit source]
There are 4 main muscle groups at the elbow. The anterior bicep group, the posterior tricep group, the lateral extensor-supinator group and the medial flexor-pronator group
Each muscle group applies a compressive load to the elbow joint when they contract.[1][2]
- Primary Elbow Flexors
- Secondary Elbow Flexors
- Pronator teres
- Extensor carpi radialis longus
- Flexor carpi radialis (at elbow angles 50 degrees or more)
- Primary Elbow Extensors
- Secondary extensors
- Flexor Carpi ulnaris
- Extensor carpi ulnaris
- Pronation
- Pronator teres
- Pronator quadratus
- Supination
- Mainly Biceps
- Assistance from supinator
- Lesser degree finger and wrist extensors
Differential Diagnosis of Elbow Pain[edit | edit source]
Lateral elbow pain is the most common site for pain to be felt at the elbow.[6] Lateral epicondylalgia or tennis elbow is a common cause of lateral elbow pain,[7] impacting between 1% and 3% of the population,[8] but it is not the only cause. There are many conditions that can cause pain and dysfunction at the elbow and a systematic differential diagnosis is important to identify all contributing and predisposing factors.
Lateral Elbow Conditions:
- Lateral Epicondylalgia
- Osteochondral Fractures of the capitellum
- Osteochondritis Dissecans
- Synovial Plica
- LCL tear/ strain
- Fractures of the Radial Head
- Loose Bodies
- OA radiohumeral joint
- Synovitis RH joint
- Radial tunnel syndrome
- Posterior interosseous Nerve entrapment
Medial Elbow Conditions:
- Medial Epicondylalgia
- MCL strain/rupture
- Ulnar Nerve Entrapments
- Medial olecranon fossa impingement
Posterior Elbow Conditions:
- Avulsion fractures of the olecranon
- Olecranon spurs
- Olecranon posterior impingement
- Triceps tendinopathy/ rupture
- Olecranon Bursitis
- Postero/lateral dislocation
Anterior Elbow Conditions:
- Biceps insertion tendinopathy rupture
- Brachialis Strain/ Tear
- Degenerative joint changes
- Adult annular ligament
Factors Contributing to Elbow Pain [edit | edit source]
Elbow pain does not occur in isolation. Many structures can refer pain to the elbow and others can contribute to the development of elbow pain and dysfunction.[6] It has been shown in various studies that structures distant to the elbow contribute to the development of elbow pain and dysfunction. These can be from a variety of dysfunctions namely neural, myofascial, joint-related or even centrally mediated.
Shoulder, Cervical Spine and Thoracic Spine[edit | edit source]
The cervical and thoracic spine have been shown to influence elbow pain. Berglund et al.[9] found that 70% of subjects with lateral elbow pain also experienced pain in their cervical and thoracic region whereas the asymptomatic group only reported 16%. Zunke et al. found that thoracic spine mobilisation can significantly increase pain-free grip strength in individuals with lateral epicondylalgia.[10]
Weakness of the scapular muscles, particularly serratus anterior as well as lower and middle trapezius, have been shown to be a significant risk factor in the development of elbow pathology.[11] Fatigue in these muscles can alter the biomechanics of upper limb activity and thereby cause dysfunction at the elbow.[11] A study conducted in 2012 by Lucado et al found that female tennis players with lateral epicondylalgia showed greater weakness in their wrist extensors and lower trapezius muscles compared to asymptomatic players.[12] This study contained a relatively small sample size and as such does not represent a direct causal relationship but rather factors to consider in the diagnosis and management of elbow pathology.
Compensatory movements at the elbow can occur as a result of dysfunction at other joint complexes in the body. An example being if there is a loss of glenohumeral lateral rotation range of motion there may be an increase in forearm supination or valgus as a compensatory strategy.[13] Alternatively, a loss of glenohumeral internal rotation range of motion may result in an increase in forearm pronation.[13] These compensatory movements can result in problems occurring at the various elbow structures. Treating the local elbow pain will not resolve symptoms as the primary problem of reduced shoulder mobility needs to be addressed to reduce the increased stress at the elbow.
The Role of the Central Nervous system[edit | edit source]
As in any pain condition, the central nervous system plays an important role in elbow pain and dysfunction. Depression and anxiety have been associated with upper extremity complaints and should be considered when managing elbow conditions.[14] Central sensitisation can be a cause of hyperalgesia and altered pain processing at the elbow.[15] This centrally mediated process is important to identify as standard peripheral biomechanical based treatment may not be as effective in patients presenting with symptoms of central sensitisation. Patients with central sensitisation potentially experience short-term and long-term pain as well as increased disability.[15] Cold hyperalgesia as a means of identifying central sensitisation in the elbow could be a useful diagnostic test to identify altered pain processing.[15] A study conducted by Maxwell and Sterling in 2013 on patients with neck pain showed that a Numeric Pain rating scale of greater than 5 after a 10-second application of ice to the neck is a good indicator of cold hyperalgesia.[16] More research in this field specific to the elbow is required.
Physiotherapy Assessment of the Elbow[edit | edit source]
Subjective Examination[edit | edit source]
As with all conditions, a detailed subjective examination is your foundation for being able to clinically reason. Specific questioning around the history of the condition, aggravating and easing factors as well as 24-hour patterns will help to form a picture of what is going on. Asking about any other problems anywhere else in the body may help give an indication of contributing factors. General health and red flag screening are important to exclude any serious pathologies as well as indicate if any co-morbidities may be contributing to the condition.
Outcome Measures[edit | edit source]
There are a variety of outcome measures that can be used for elbow and upper limb dysfunction. Evans et al (2019) recommended the use of either the DASH, Quick-Dash, Patient-Rated Tennis Elbow Evaluation and Oxford Elbow Score for lateral epicondylalgia.[17]
Imaging[edit | edit source]
X-rays are normally performed in elbow trauma and are important in excluding fractures and dislocations. Ultrasounds and MRIs are normally performed when there is suspected soft tissue (eg tendon) involvement. Imaging for the elbow may be useful for visualizing pathophysiology but the severity of pathophysiology seen on imaging does not correlate with the level of symptoms.[18] Positive findings on imaging should be interpreted with caution and should not be used as a primary clinical assessment tool. Negative findings on imaging may be helpful to rule out pathology.
Objective Examination[edit | edit source]
A comprehensive physical examination is performed to confirm or negate your potential hypothesis formed after the subjective examination.
Local examination of the elbow
- Active and passive movements
- Muscle strength testing
- Ligament stress tests
- Any other appropriate special tests
- Grip strength measured with a grip dynamometer[18]
- Palpation and manual examination of the joints and soft tissue structures
- Thermal hyperalgesia
Examination of other structures as identified on subjective examination
- Cervical Spine
- Thoracic Spine
- Shoulder
- Wrist
- Neurological System and Neurodynamics
- Any other potential contributing system
Physiotherapy Management of Elbow Pain and Dysfunction[edit | edit source]
The management of lateral epicondylalgia has been well researched. The other conditions found around the elbow have not been as widely researched and evidence-based practice for those conditions may be more focused on general clinical experience than on specific researched evidence.
It is well accepted that a comprehensive management programme of elbow pain and dysfunction requires a multi-modal approach. Active management of musculoskeletal pain disorders involving self-management is more supported by evidence than passive management strategies.[19] Treatment should be aimed not only at the local elbow structures found on assessment but at all the contributing factors identified during the examination.
Management of Lateral Elbow Tendinopathy (LET)[edit | edit source]
Pharmacotherapy[20]
NSAIDs- possibly more useful in reactive tendinopathy than a degenerative tendinopathy
Corticosteroid medication- the evidence shows short term relief but outcomes are worse at 6-12 months compared to wait and see or physiotherapy management. Corticosteroid injections may not be appropriate as a first-line intervention for lateral elbow tendinopathy
Centrally Acting Analgesics- may be appropriate for patients with central sensitisation
Prolotherapy and Nitric Oxide patches- possibly more beneficial in patients with more chronic LET of more than 3 months
Manual Therapy[20]
There is moderate evidence that manual therapy can have immediate beneficial effects on pain and grip strength. Mulligan mobilisations which are aimed at pain-free movement during a mobilization technique have been shown to be beneficial. Manual therapy at the cervical and thoracic regions have also shown to provide clinical benefits in LET management
Education[20]
As in any condition education around the pathophysiology of the condition and symptom modification, stages of healing and general self-management are important.
Exercise Therapy[20]
Exercise therapy has the best evidence for good treatment outcomes in lateral epicondylalgia. Optimal loads have not yet been established and various subgroups of patients may benefit from different loading strategies. Isometrics may produce an analgesic effect and in general, exercises that are centred around loading the tendon should not aggravate the pain.
Tendon neuroplastic training
Tendon neuroplastic training as descrived by Rio et al has been shown to be an effective management programme for lower limb tendinopathies.[21] It has not been studied in upper limb tendinopathies in detail. Welsh (2018) published a case report with a TNT programme being applied to 2 separate patients with lateral elbow tendinopathy with promising results.[22] More research is needed in this field
Conclusion[edit | edit source]
Physiotherapists are integral in the management of conditions around the elbow. Physiotherapists can provide a detailed assessment and comprehensive multimodal management strategy that takes into account the complex anatomy and biomechanics of the elbow as well as the contributing factors from structures distant to the elbow,
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Bryce CD, Armstrong AD. Anatomy and biomechanics of the elbow. Orthopedic Clinics of North America. 2008 Apr 1;39(2):141-54.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Alcid JG, Ahmad CS, Lee TQ. Elbow anatomy and structural biomechanics. Clinics in sports medicine. 2004 Oct 1;23(4):503-17.
- ↑ Akhtar A, Hughes B, Watts AC. The post-traumatic stiff elbow: A review. J Clin Orthop Trauma. 2021 May 19;19:125-31.
- ↑ Umur LF, Surucu S. Association between increased elbow carrying angle and lateral epicondylitis. Cureus. 2022 Mar 9;14(3):e22981.
- ↑ 5.0 5.1 5.2 5.3 5.4 Smith JM, Bell JE. Anatomy of the Elbow. InThe Unstable Elbow 2017 (pp. 3-11). Springer, Cham.
- ↑ 6.0 6.1 Brukner P. Brukner & Khan's Clinical sports medicine. North Ryde: McGraw-Hill; 2012.
- ↑ Viswanathan S, Shanker H. Long-term functional outcomes following radiofrequency microtenotomy for lateral epicondylitis of elbow. Cureus. 2022;14(10): e30317.
- ↑ Karabinov V, Georgiev GP. Lateral epicondylitis: New trends and challenges in treatment. World J Orthop. 2022 Apr 18;13(4):354-64.
- ↑ Berglund KM, Persson BH, Denison E. Prevalence of pain and dysfunction in the cervical and thoracic spine in persons with and without lateral elbow pain. Manual therapy. 2008 Aug 1;13(4):295-9.
- ↑ Zunke P, Auffarth A, Hitzl W, Moursy M. The effect of manual therapy to the thoracic spine on pain-free grip and sympathetic activity in patients with lateral epicondylalgia humeri. A randomized, sample sized planned, placebo-controlled, patient-blinded monocentric trial. BMC Musculoskelet Disord. 2020 Mar 24;21(1):186.
- ↑ 11.0 11.1 Suzuki H, Swanik KA, Huxel KC, Kelly JD, Swanik CB. Alterations in upper extremity motion after scapular-muscle fatigue. Journal of Sport Rehabilitation. 2006 Feb 1;15(1):71-88.
- ↑ Lucado AM, Kolber MJ, Cheng MS, Echternach Sr JL. Upper extremity strength characteristics in female recreational tennis players with and without lateral epicondylalgia. journal of orthopaedic & sports physical therapy. 2012 Dec;42(12):1025-31.
- ↑ 13.0 13.1 Sahrmann S. Movement system impairment syndromes of the extremities, cervical and thoracic spines-e-book. Elsevier Health Sciences; 2010 Nov 19.
- ↑ Degen RM, MacDermid JC, Grewal R, Drosdowech DS, Faber KJ, Athwal GS. Prevalence of symptoms of depression, anxiety, and posttraumatic stress disorder in workers with upper extremity complaints. journal of orthopaedic & sports physical therapy. 2016 Jul;46(7):590-5.
- ↑ 15.0 15.1 15.2 Coombes BK, Bisset L, Vicenzino B. Cold hyperalgesia associated with poorer prognosis in lateral epicondylalgia: a 1-year prognostic study of physical and psychological factors. The Clinical journal of pain. 2015 Jan 1;31(1):30-5.
- ↑ Maxwell S, Sterling M. An investigation of the use of a numeric pain rating scale with ice application to the neck to determine cold hyperalgesia. Manual therapy. 2013 Apr 1;18(2):172-4.
- ↑ Evans JP, Porter I, Gangannagaripalli JB, Bramwell C, Davey A, Smith CD, Fine N, Goodwin VA, Valderas JM. Assessing patient-centred outcomes in lateral elbow tendinopathy: a systematic review and standardised comparison of English language clinical rating systems. Sports medicine-open. 2019 Dec 1;5(1):10.
- ↑ 18.0 18.1 Chourasia AO, Buhr KA, Rabago DP, Kijowski R, Lee KS, Ryan MP, Grettie-Belling JM, Sesto ME. Relationships between biomechanics, tendon pathology, and function in individuals with lateral epicondylosis. journal of orthopaedic & sports physical therapy. 2013 Jun;43(6):368-78.
- ↑ Hutting N, Johnston V, Staal JB, Heerkens YF. Promoting the use of self-management strategies for people with persistent musculoskeletal disorders: the role of physical therapists. journal of orthopaedic & sports physical therapy. 2019 Apr;49(4):212-5.
- ↑ 20.0 20.1 20.2 20.3 Coombes BK, Bisset L, Vicenzino B. Management of lateral elbow tendinopathy: one size does not fit all. journal of orthopaedic & sports physical therapy. 2015 Nov;45(11):938-49.
- ↑ Rio E, Kidgell D, Moseley GL, Gaida J, Docking S, Purdam C, Cook J. Tendon neuroplastic training: changing the way we think about tendon rehabilitation: a narrative review. British journal of sports medicine. 2016 Feb 1;50(4):209-15.
- ↑ Welsh P. Tendon neuroplastic training for lateral elbow tendinopathy: 2 case reports. The Journal of the Canadian Chiropractic Association. 2018 Aug;62(2):98.