Peroneal Tendon Subluxation
Original Editors - Tess Mertens
Top Contributors - Rachael Lowe, Kim Jackson, Tess Mertens, Wajeeha Hassan, Admin, Maarten Cnudde, Patti Cavaleri, Simisola Ajeyalemi, Wanda van Niekerk, 127.0.0.1, Rucha Gadgil, Jess Bell and Pinar Kisacik
Definition/Description[edit | edit source]
Subluxation or dislocation of the peroneal tendons is a disorder involving an elongation, a tear, or an avulsion of the superior peroneal retinaculum[1]. There can be also subluxation of the tendons with an intact superior peroneal retinaculum (SPR) (intrasheath subluxation)[2].
Clinically Relevant Anatomy[edit | edit source]
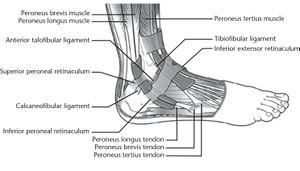
Peroneus brevis and peroneus longus are contained in the retromalleolar sulcus on the fibula. The depth of the sulcus is variable and has been noted to be absent or convex in some[3]. The tendons are stabilized by a superior peroneal retinaculum. The SPR is formed by thickening of the superficial aponeurosis. A small fibrous ridge is occasionally seen originating from the distal fibula close to the origin of the SPR and increases the depth of the fibular groove. Distal to the fibula is the inferior peroneal retinaculum, which covers the tendons for about 2 to 3 cm distal to the tip of the fibula[4].
Epidemiology /Etiology[edit | edit source]
The most common mechanism is a dorsiflexion force on the ankle associated with a rapid, strong contraction of the peroneal tendons and with eversion of the hindfoot[5]. The peroneus longus and brevis tendons sublux or dislocate from the lateral retromalleolar groove. This results from a tear, avulsion or significant laxity of the SPR. Some patients have a more chronic presentation and cannot recall a traumatic episode. Also, congenital factors are reported, for example, the sulcus or the ridge that helps deepen the sulcus can be too shallow or even absent or the SPR can be too loose[5].
Peroneal tendon subluxation is commonly encountered in skiing, but also has been reported in other sports, such as gymnastics, ice skating, and rugby[1][6][7].
Peroneal subluxations account for 0.3-0.5% of traumatic ankle injuries[7].
Characteristics/Clinical Presentation[edit | edit source]
There are three grades to classify the acute peroneal subluxation[8][3][9]
Grade I: The retinaculum, which is confluent with the periosteum on the fibula, is stripped away from the fibula, resulting in dislocation of the tendons.
Grade II: The fibrocartilaginous ridge and the SPR is avulsed from the posterior aspect of the fibula.
Grade III: Bony avulsion of the posterolateral aspect of the fibula containing the cartilaginous rim and a flake of bone permitting the tendon to slide beneath the periosteum.
Grade IV: The SPR elevated from the calcaneus
Patient's with pes cavus feet may be predisposed to peroneal subluxations and lateral ankle instability[7].
- Popping or snapping sensation on the outer edge of the ankle
- Forceful pop in traumatic injuries
- Tendons slip out of place along the lower tip of the fibula
- Pain, swelling or tenderness below/behind the lateral malleolus
- Painful resisted ankle eversion
- Unstable ankle, especially on uneven surfaces
- Chronic retromalleolar pain and/or history of recurrent ankle sprains in those with chronic subluxations
Differential Diagnosis[edit | edit source]
Examination[edit | edit source]
Acute peroneal subluxation is often difficult to appreciate clinically. There is usually edema, ecchymosis and point tenderness in the same distribution than in case of a sprained ankle, therefore making diagnosis difficult[5].
Due to dorsiflexion mechanism of injury, utilization of the squeeze test can help determine if there is a syndesmotic injury component[7].
Subluxation of the peroneal tendon can be replicated with the patient repeatedly dorsiflexing and plantarflexing the foot while the examiner provides a force to resist ankle eversion[7]. A negative on this test does not rule out subluxation injury.
In chronic situations patients frequently complain about a painful windlass mechanism and can typically reproduce the dislocation by active dorsiflexion-eversion of the foot[5]. In most cases, a peroneal tendon snapping around the posterior margin of the lateral malleolus can be palpated and even visualized by the examinator. These clinical findings can be enhanced by applying a slight resistance to the dorsiflexion-eversion.
Acute injuries should be screened for fracture using the Ottawa Ankle Rules to determine if referral for radiography is indicated for assessment of avulsion injury[7].
MRI can show the static anatomy of the peroneal tendons. Ultrasound is becoming a more favored diagnostic imaging tool as it can assess the peroneal tendons in a dynamic environment. Ultrasonography achieved an accuracy of 94%, with 100% sensitivity and 90% specificity, whereas MRI was 66% accurate, with 23% sensitivity and 100% specificity[7].
Management[edit | edit source]
In infants and neonates, conservative management of subluxing peroneal tendon is the rule and spontaneous resolution is extremely high[5],[10].
In adults the treatment can be divided into non-operative and operative when considering acute or chronic injuries[5]. When an acute subluxation is diagnosed, the patient may be consider non-operative treatment[8][3]. If the conservative treatment failed or if there’s a chronic subluxation, surgical treatment is likely indicated[7][8]. Early treatment is critical, since a tendon that continues to sublux (move out of position) is more likely to tear or rupture[11].
Conservative[edit | edit source]
In particular, non-operative treatment is indicated for grade I and possibly grade III injuries, depending on the degree of displacement of the cortical fragment[8]. Conservative treatment is associated with minimal risks but also with a high rate of failure[5].
Non operative treatment consists in applying a non weight bearing cast for 2–6 weeks[8]. This conservative management aims to allow the SPR to re-adhere to the posterolateral aspect of the fibula[5].
Conservative attempts can also include adhesive strapping with a pad to restrict subluxation, J-shaped pads that anchor in front of the fibula and wrap around laterally and posteriorly to hold the tendons in place and non-weight bearing for 2-6 weeks. If the foot is kept relatively stable and the tape restricts the tendon’s movement, scar-tissue formation may allow the tendon to be managed without surgery[12]. Exercises included in rehabilitation after immobilization include proprioception training and range of motion exercises.
Physical therapy management[edit | edit source]
Physical therapy management starts ideally with asking patients to be non-weight bearing for a time period of 2 weeks. After this, the patient is asked to be in walking boots for the next 4 weeks.[13]
Then starting with an active range of motion progression is made to proprioceptive training and then to strength training. Strength training can include resistance band protocol and proprioceptive neuromuscular facilitation.[14]
Use of non weight bearing cast for 6≥ weeks is found to be more effective than taping for 3≥ weeks.[15]
Aerobic exercises such as swimming and cycling are also incorporated into the plan after the strength gains. After getting a full command on functional training, the patient can proceed to sports-specific training. Athletes usually return to play in about 3-4 months.[16]
Physical therapy after surgery
With the exception of the motion precautions, rehabilitation can proceed much like that of the chronic ankle sprain. However, the rehabilitation after surgery is likely to take more time to fully restore motion, strength and function[17]
After surgery, the ankle is maintained for 2 weeks in a non-weight bearing and short leg cast in a slightly inverted position, followed by 4 or more than 4 weeks in a short leg walking cast. During immobilization, cardiovascular conditioning is performed along with proximal muscle strengthening.[18]
The first few physical therapy treatments are designed to help control pain and swelling from the surgery. Ice and electrical stimulation treatments may be used. The therapist may also use massage and other hands-on treatments to ease muscle spasm and pain. Soft tissue mobilization around the scar site can be employed to increase the soft tissue mobility[12].
Treatments are also used to help improve ankle range of motion by progressive resistance and ROM exercises without putting excessive strain on the area[17]. Active and resisted dorsiflexion and eversion are prevented during the early rehabilitation phase to reduce stress on the SPR (approximately 6 to 8 weeks[12].
Patient can run and jog with at 8-10 weeks. At the same time peroneal strengthening is also targeted. [18]
Talar mobilization exercises and active dorsiflexion and eversion begin when the patient can bear weight without pain[12].
The progression of resisted strengthening, proprioception and agility exercises is initiated when the patient can bear weight without pain and without brace. As strength and proprioception improve, the patient can progress through plyometric and functional activities that lead to a return to competition[12].
Surgical[edit | edit source]
Less controversy exists for the management of chronic lesions because surgical repair for peroneal tendon subluxation provides good results in most cases[5].
- Bone block procedure
- Reattachment of the SPR with local tissue augmentation
- Reinforcement of the SPR with local tissue transfer
- Rerouting the tendons behind the calcaneofibular ligament[19]
- Groove-deepening procedures
The surgical approach may differ on the basis of the grade of injury[4].
References [edit | edit source]
- ↑ 1.0 1.1 1.2 Safran MR, O'Malley D. Peroneal tendon subluxation in athletes: new exam technique, case reports, and review. Med Sci Sports Exerc. 1999; 31(Suppl 7): s487-92
- ↑ Raikin SM, Elias I, Nazarian LN: Intrasheath subluxation of the peroneal tendons. JBJS Am. 2008 May;90(5):992-9
- ↑ 3.0 3.1 3.2 Roger A. Mann, Subluxation and dislocation of the peroneal tendons. Operative Techniques in Sports Medicine, Vol 7, No 1 (January), 1999: pp 2-6
- ↑ 4.0 4.1 Rosenberg ZS, Bencardino J, Astion D, Schweitzer ME, Rokito A, Sheskier S: MRI Features of Chronic Injuries of the Superior Peroneal Retinaculum. AJR:181, December 2003
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 Akiki A, Crevoisier X; Peroneal Tendon Dislocation: Schweizerische Zeitschrift für «Sportmedizin und Sporttraumatologie» 55 (1), 26–29, 2007
- ↑ Micheo W: Musculoskeletal, Sports, and Occupational Medicine, Demos Medical New York, 272p
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 7.7 7.8 Roth JA, Taylor WC, Whalen J. Peroneal tendon subluxation: the other lateral ankle injury. Br J Sports Med. 2010 Nov;44(14):1047-53.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 Heckman DS, Reddy S, Pedowitz D, Wapner KL, Parekh SG: Operative Treatment for Peroneal Tendon Disorders Review. JBJS Vol 90-A nr2 February 2008
- ↑ Wade R, Eckert MD, Mammoth L, Earle AD: Acute Rupture of the Peroneal Retinaculum. JBJS, 1976; 58:670-672
- ↑ Siegel MR, Schubiner J, Sammarco VJ: A Nonoperative Treatment Technique for Peroneal Tendon Subluxation; Clinical Pediatrics
- ↑ American College of Foot and Ankle Surgeons (ACFAS): http://www.footphysicians.com/footankleinfo/peroneal-tendon.htm, 12/18/2009
- ↑ 12.0 12.1 12.2 12.3 12.4 Starkey C, PhD, ATC, Johnson G: Athletic training and sports medicine, American Academy of Orthopaedic Surgeons, 713p, 2006
- ↑ Espinosa N, Maurer MA. Peroneal tendon dislocation. European Journal of Trauma and Emergency Surgery. 2015 Dec;41(6):631-7. https://link.springer.com/article/10.1007/s00068-015-0590-0
- ↑ Voss DE. Proprioceptive neuromuscular facilitation. American Journal of Physical Medicine & Rehabilitation. 1967 Feb 1;46(1):838-98. https://meridian.allenpress.com/jat/article/50/1/36/112404/Strength-Training-Protocols-to-Improve-Deficits-in
- ↑ Bakker D, Schulte JB, Meuffels DE, Piscaer TM. Non-operative treatment of peroneal tendon dislocations: A systematic review. Journal of orthopaedics. 2020 Mar 1;18:255-60.https://www.sciencedirect.com/science/article/abs/pii/S0972978X19303009
- ↑ Roth JA, Taylor WC, Whalen J. Peroneal tendon subluxation: the other lateral ankle injury. British journal of sports medicine. 2010 Nov 1;44(14):1047-53. https://bjsm.bmj.com/content/44/14/1047.short
- ↑ 18.0 18.1 Oesman I, Kurniawan D, Wikanjaya R. Peroneal groove deepening as the treatment of peroneal tendon subluxation: a case report. International Journal of Surgery Case Reports. 2019 Jan 1;65:333-8. https://www.sciencedirect.com/science/article/pii/S2210261219306492
- ↑ Wang C-C, Wang S-J, Lien S-B, Lin L-C; A New Peroneal Tendon Rerouting Method to Treat Recurrent Dislocation of Peroneal Tendons. The American Journal of Sports Medicine (2009) Volume: 37, Issue: 3, Pages: 552-557