Patellofemoral Pain Syndrome and Runners’ Interaction with the Health System
Top Contributors - Oyemi Sillo, Kim Jackson and Kapil Narale
Introduction[edit | edit source]
What is patellofemoral pain syndrome?[edit | edit source]
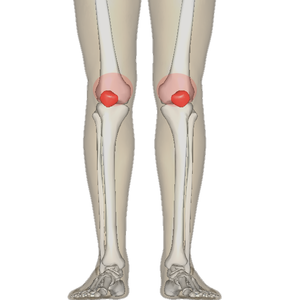
Running is a very common form of physical activity. There are many different types of injuries that can occur. One form of pain that can develop at the knee and the kneecap is patellofemoral pain syndrome (PFPS), anterior knee pain, or ‘runner’s knee’, all terms used interchangeably. PFPS is a very common injury, with a high prevalence in runners, non-runners, male and female adolescents, teens, and adults.[1]
Patellofemoral pain is generally felt at the front, around, or on the backside of the patella.[2][3] Symptoms of PFPS are characterized by pain that is produced with activities, which increase the load on the patellofemoral joint with a flexed knee, such as running, going up and down stairs, squatting, and prolonged sitting.[2][1][3] [4] Crepitus may also be felt at the joint, in addition to tenderness on palpation of the small facets, and some effusion.[1]
PFPS should be detected, managed, and treated early, as long-term treatment outcomes of patellofemoral pain might be quite poor in people who may report symptoms 5 years after diagnosis. This type of pain may also align with patellofemoral osteoarthritis, patellar fracture, or osteochondritis.[1][3]
This page will outline the common forms of treatment for runners with Patellofemoral Pain Syndromeand how it relates to the different levels and stages of healthcare.
Mechanism of Injury / Pathological Process
[edit | edit source]
How does PFPS occur in runners?[edit | edit source]
There are many different possible mechanisms which cause PFPS in runners. PFPS can be caused by various internal and external factors. Internal factors can encompass muscle and joint force imbalances and weakness, and anatomical and biomechanical abnormalities. External factors can be caused by overuse and overloading of the patellofemoral joint, which can occur by overuse from inadequate terrain and environment, training load, running method and gait, and a decrease in grade of incline (downhill running).[6]
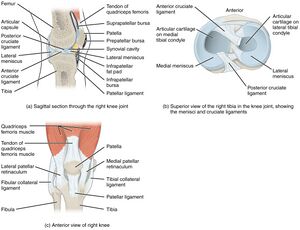
Muscular weakness in the quadriceps, patellar tendon, vastus medialis obliquus, medial patellofemoral ligament, medial patellotibial ligament, patellotibial band, and epicondylopatellar bands[2] can jeopardize the stability of the patella within the patellofemoral joint and can lead to altered patellar tracking or lateral translation of the patella within the femoral groove. Patellar tracking can also increase with load-bearing positions [2][1][4] Altered patellar tracking leads to increased compressive and shearing forces, patellofemoral joint contact pressure, and thus can cause patellofemoral pain.[1]
With running, the quadriceps’ control of the knee occurs mainly via the vastus lateralis oblique muscle and the vastus medialis oblique muscle, however it is noted that the lateral soft tissue of the knee structures can easily become tight.[7] With the vastus lateralis oblique in this state, there will be an imbalance of forces acting upon the patella, which would result in poor movement and coordination of the knee, and possible tracking of the patella. In such a case, if the vastus medialis oblique is weak, and the vastus lateralis oblique is tight, excessive load would be placed on the knee while running, and pain would be an outcome due to excessive imbalanced pressures at the patella.[6][4] This can also occur with stiffness of the iliotibial band.[4]
During running, the hamstrings are specifically important for extending the hip and controlling the movement of the tibia via minimizing knee flexion near the end of swing phase. Tight hamstrings have been associated with patellofemoral pain, possibly because of the co-contraction of the hamstrings and quadriceps, causing increased forces at the knee. Tight hamstrings can be assessed using the passive knee extension test.[2]
Dynamic valgus positioning of the knee can also cause PFPS. This is a position where the knee collapses medially, with internal rotation of the femur, which increases the lateral forces on the patella, contributing to tracking of the patella, leading to patellofemoral pain.[2]
Rearfoot eversion and pes pronatus, which lead to internal rotation of the tibia, can also contribute to dynamic valgus.[2][6] Reduced foot pronation during the stance/loading phase of the running gait can be noted with a shorter time to maximal pressure on the 4th metatarsal. This would reduce the load that is absorbed, and therefore greater transfer of forces toward the patellofemoral joint, leading to patellofemoral pain.[1]
As an interesting fact, especially for runners, excess wear-and-tear patterns on the medial aspect of one’s shoe could indicate the presence of pes pronatus or rearfoot eversion, as can be seen in these clips:[2]
An increase in Q-angle, can lead to Patellofemoral pain; flexion of the knee causes the patella to move medially, allowing it to sit properly in the intercondylar notch until a knee flexion angle of 130o is reached.[7] The patella will subsequently slide back laterally. If this cannot happen smoothly, it will lead to an increased tracking of the patella, and thus cause pain at the patellofemoral joint.[6]
Factors contributing to an improper Q-angle include the drop of the pelvis, increased hip abduction, and increased internal rotation of the hip. During running, this would lead to the patellofemoral joint being overloaded on the lateral aspect. Weak hip abductor muscles, such as the gluteus maximus and gluteus medius muscles, have been associated with increased hip adduction during running.[10] This would contribute to an increased Q-angle, and therefore patellofemoral pain during running.[4][6]
In relation to the hip, individuals with PFPS were seen to have decreased hip abduction, extension, and external rotation strength, with reduced gluteal muscle activity during functional tasks. It was noted that patellofemoral pain was more likely to occur in people with an increased peak hip adduction and internal rotation during running, with the symptoms becoming more pronounced after initial onset.[1][4]
All these factors may cause patellofemoral pain in a runner, but those that may not directly stem from the knee, include weakness at the hip, improper foot positioning, and improper gait biomechanics, which can all lead to problems along the kinetic chain.[4][6]
With respect to gender differences, female runners are more likely to have PFP through a hip biomechanical malingment, while male runners with are seen to have PFP with an increased peak knee adduction.[6]
A non-physical mechanism of injury may occur through one’s psychological beliefs, affecting their training patterns and performance. Individuals with patellofemoral pain may be seen to consciously climb stairs with a reduced peak knee flexion as a fear-avoidance mechanism, to avoid any symptoms, and to minimize patellofemoral joint and quadriceps loading.[1][4]
Where would runners with PFPS turn to for assistance with reducing, minimizing, and eliminating pain, and being able to get back to their lifestyle of running? This is explored below.
Treatments and Interventions available[edit | edit source]
Depending on the type of injury, whether it is an acute injury, like a blow to the knee, or a chronic injury like overloading and overusing, different forms of medical management can be utilized. Physiotherapy and Exercise Therapy, Education, and Foot Orthoses are some of the modalities used to help a person recover from PFPS.[6]
The types of care that are experienced throughout the health system are mapped and outlined below. The Rehabilitation Phases span from Primary Care, Secondary Care, Tertiary Care and Quaternary Care. The levels of healthcare that are generally experienced with a running injury would be Acute Care and Long-Term care.
Primary (or Acute) Care[edit | edit source]
Primary care is usually one’s initial contact with the health system. It usually involves seeing the Family Physician or General Practitioner, but can also involve seeing a pharmacist, physiotherapist, sports trainer, field or event EMS, or even a paramedic.[11]
If a blow to the knee is sustained, immediate acute primary care would be provided by Emergency Medical Services (via paramedics). For runners training in their own chosen environment, such a service may not be instantly available. But during a race or an organized setting, primary care can be provided to a direct blow to the knee by any first aid or medical response personnel on site.
Secondary Care[edit | edit source]
Secondary Care would include planned operations and other medical treatments. It can also include physiotherapy treatment as a referral from a primary physician. If Physiotherapy was the patient’s initial point of contact with the health system, the physiotherapist would be their primary health care practitioner.[12]
Secondary Care through medical treatments would not be needed for people with PFPS, especially if the pain and biomechanical issues can be resolved through Physiotherapy interventions such as exercise therapy or external interventions. Such a treatment would be done through correcting and adjusting the abnormal patellofemoral kinematics, and the alignment of the patellofemoral joint.[6]
Aside from Physiotherapy, Podiatrists and/or Orthotists can help with pain management through correcting biomechanical problems via prescribing appropriate shoes and orthoses.[13] This can also be considered Secondary Care, and they would help runners with any foot alignment problems.[6]
Tertiary or Quaternary Care[edit | edit source]
This type of care would be more specialized than primary or secondary health care, and would not be involved with assessing, evaluating, diagnosing, or treating PFPS, unless there are extenuating circumstances, or long-term pain that is not subsiding with conservative treatments.
Long Term Care [edit | edit source]
Long Term Care would involve any interventions that would be carried out for a longer period, aiding the runner to get back to their activity, helping to reduce pain, and increase function. According to a scoping review conducted by Kunene[6] after reviewing a series of studies, it was concluded that education, gait re-training, exercise, foot orthoses, and multimodal rehabilitation were the most useful forms of rehabilitation interventions for runners to resume and continue their activity.[6]
Education[edit | edit source]
Education would include providing knowledge about the symptoms of PFPS and management of training loads. A study found that education itself was as efficient and effective as education, and exercises or gait retraining, in reducing patellofemoral pain symptoms and functional limitations.[14] Education encompasses managing patient expectations, advising about load management with running, exercising, and activities of daily living, ensuring self-management, teaching the importance of adherence to exercise-therapy, and implementing strategies to address possible fears of movement.[1] In addition to providing education to runners, aggravating activities should be avoided, however activity levels should be maintained to ensure health and fitness.[2]
Education helps equip the runners to prevent and manage the possible symptoms of PFPS and pay attention to their training load. Providing education is a person-centered approach. As the patient becomes involved in their treatment, they have an active role in resolving and preventing any symptoms and improving their running form.[6]
Gait Retraining[edit | edit source]
Gait retraining is an important component for helping patients who have adapted an incorrect gait pattern due to their imbalance or injury. This would help them return to proper, injury free running.
A study of mirror gait retraining in females found that this was an effective rehabilitation method. Gait retraining helped reduce pain, improve function, and body mechanics, which had a long-term effect.[15] A case report mentioned that two weeks of mirror gait retraining addressed pain, function, hip mechanics, gluteus medius control, and hip-abductor strength.[16] This helps reduce excessive hip adduction, contributing to reduced patellofemoral pain. Mirror gait training is seen to help improve hip biomechanics and knee function, and therefore reduces pain levels during running.[6]
Kunene[6] referenced two studies (Roper et al, 2016; Chung and Davis, 2011) that found that altering one’s running gait pattern from heel strike to forefoot strike improved the runners’ symptoms of PFPS, reducing knee pain, and improving biomechanics at the knee and ankle, and thus adapting a forefoot strike would be an effective rehabilitation technique.[6] Gait retraining helps reduce the peak vertical impact while running, and pain and functional limitations, therefore helping to improve running performance.[6] It is seen that the adjustment of biomechanical issues in runners with patellofemoral pain helps to reduce such symptoms.
Here is a video explaining the difference between a heel strike and a forefoot strike:
In addition, this video explains how to switch from a heel strike to a forefoot strike:
Exercise Therapy[edit | edit source]
An important rehabilitation intervention involves exercise therapy, which includes muscle strengthening at the hip, trunk, and knee.[2] This would help strengthen weaker imbalanced areas that are contributing to patellofemoral pain. This helps with overcoming pain in the short-term and long-term, during rest and during activity.[2] Proximally targeted exercises, carried out early in rehabilitation, at the hip, in addition to knee-targeted exercises, will help with reducing symptoms and improve function. Proximal muscles targeted include gluteus maximus and gluteus medius, which would contribute to improving hip strength and mobility. Such exercises should be carried out sooner, especially if knee targeted exercises produce pain.[1]
A weakened vastus medialis oblique and a tight vastus lateral oblique can lead to patellofemoral pain. Pain can be reduced or eliminated by improving the strength of the vastus medialis oblique, its activation, and timing, and the flexibility of the shortened soft tissue structures such as the vastus lateralis oblique, and by correcting patellar alignment.[6] A 3-week hip abductor strengthening program would be recommended as it would help with reducing knee pain and improving knee stability in people with PFPS.[6]
The following video shows an example of hip abductor strengthening exercise:
Here is another video showing a sample programme and progression of hip and knee strengthening and stretching exercises:
With a patient-personalized program of muscle strengthening via exercise therapy, increased response of the vasti muscles, quadriceps isometric strength, hip strength, and reduced knee valgus was noted during running.[1] Without these, a tight iliotibial band, a weak and unstable core, hamstrings, hip internal rotators, and adductor longus and brevis, can contribute to patellofemoral pain, and therefore should be stretched, stabilized, and strengthened, accordingly.[21]
Home exercise programs, which include resistance band training, and body weight exercises were seen to be effective, early on in rehabilitation. Moving from a home-based exercise program to a gym-based exercise program is effective for higher intensity activities such as running, as it will allow for progressive overload and improvements in muscle function.[1] All strengthening exercises should be continued for long-term pain relief and improved functionality for running.[2]
Orthoses [edit | edit source]
Foot orthoses can also be used to help mitigate the pain, correct foot posture, and overall biomechanics of the lower limb, thus minimizing the effects of PFPS.[1]
A study found that the insertion of medially wedged orthotics helped to reduce pain in runners who experienced increased foot pronation and patellofemoral pain.[22] The medially wedged insole was also shown to improve running mechanics at the hip and knee.[1][6] While weight bearing, runners can be seen to have increased compensatory pronation movements of the subtalar and/or midtarsal joint. This would work its way up the kinetic chain, and causes biomechanical problems at the patellofemoral joint, thus resulting in patellofemoral pain. An insertion of a medial wedge orthoses would help with mitigating such a biomechanical issue, and pain at the patellofemoral joint.[6]
Taping[edit | edit source]
Although taping can be done by a Physiotherapist or an Athletic Therapist in a primary care setting, it is outlined here since it is not an instant or urgent fix and can help with biomechanical issues in the long-term. Taping is another technique that helps with correcting biomechanical impairments of PFPS, specifically lateral tracking of the patella. There are two main taping techniques - McConnell Medial Glide and Kinesiotaping.
McConnell Medial Glide taping helps with activating the vastus medialis,[2] thus repositioning the patella medially within the femoral trochlea. This helps with altering its joint contact pressure and joint reaction force, therefore decreasing the applied load and patellofemoral pain symptoms, while improving quadriceps and patellofemoral kinematics.[2][3] This type of taping helps with increasing knee flexion during running, walking, and stair climbing.[2]
A very nice demonstration of McConnell Medial Glide taping is shown below:
Kinesiotape can be used in a Mechanical Correction with Tension in the Base arrangement. In the context of running or walking, the application of kinesiotape allows for more knee flexion at initial contact. This allows for increased activation of the quadriceps and gluteal muscles, thus allowing for a greater force absorption and reduced stress on the patellofemoral joint. With the support of kinesiotape, and the reduced stress at the patellofemoral joint, shorter swing durations can be achieved, with an improvement in running efficiency.[4]
This video carefully explains and shows how kinesiotaping is applied for PFPS:
It should be noted that taping techniques in isolation do not provide the rehabilitation that is needed to effectively reduce the pain symptoms of PFPS. Exercise itself, however, is a very effective rehabilitation intervention for pain relief from PFPS. However, the taping techniques used in combination with exercise and/or physiotherapy are helpful in the reduction in patellofemoral pain, on a short-term basis.[3] [25]
Multimodal Rehabilitation[edit | edit source]
Regardless of all interventions that can be individually carried out, it is shown that a combination of interventions, specifically multimodal rehabilitation, is an effective way to manage pain and increase function with PFPS. An 8-week program involved strengthening of the lower limb and core muscles, exercises to improve motor control, and advice on running gait, symptom management, and a training regimen. This program concluded to have an improvement in pain and function among runners with PFPS.[26] In addition, many studies cited by Kunene[6] mention that multimodal approaches are the most effective way for improving function and quality of life for runners with PFPS.
Type of Community and Healthcare Accessibility[edit | edit source]
The methods of treatment described above would be readily available and accessible in developed countries, with a higher-resource setting, and a well-established healthcare system. There would be various healthcare professionals within differing disciplines, each set out to assist rehabilitation in a different way, and each creating a part of the rehabilitation team.
A team-work approach among professionals has been shown to result in successful outcomes in rehabilitation. Interdisciplinary teams are very beneficial, however, sports clubs, gyms, or facilities in low-resource communities would not have access to complete rehabilitation services, with limited professionals and rehabilitation teams available.[4][6]
Running is a very popular form of physical activity, which is affordable to almost everyone, to those in high-resource settings and those in low-resource settings.[21] Musculoskeletal running injuries are also quite prevalent in all settings, however rehabilitation services for such injuries are “inaccessible, unaffordable, unavailable, inadequate”,[21] and are poorly managed in low-resource communities. With a high prevalence of 40%, PFPS is being seen to lower these runners’ quality of life, in physical, mental, social, emotional wellbeing.[21] Thus, resources need to be in place for the rehabilitation services of such injuries.[6][21] Very similar to the definition of ‘Rehabilitation’ within a Universal Health Care context, “Rehabilitation services should be available, accessible, affordable, adequate, and appropriate to all people, irrespective of their age, gender, race, and socio-economic status”.[21] However, this is not seen in lower-resource communities.
Recommended rehabilitation methods in under-resourced communities include community-based rehabilitation, transdisciplinary rehabilitation, and task-shifting approaches.[21] Referring more complex cases to secondary and tertiary institutions, would subsequently be recommended. Foot orthosis, physiological rehabilitation, medical treatment, radiological services, or surgical needs may be managed, in these cases. The World Health Organization (WHO) recommends- the implementation of community-based rehabilitation approaches as a strategy increase access to rehabilitation services in underserved communities.[11] This is proposed to be supplied at a ‘low-level’, or with no cost involved.[21] Transdisciplinary approaches incorporate the knowledge and expertise of various disciplines of rehabilitation and is especially helpful and useful in low-resource settings.[4][21] The transdisciplinary teams would be at secondary or tertiary healthcare centers or at academic institutes, to provide outreach to respective communities. The team would be responsible for injury screening, planning, monitoring, and evaluating the rehabilitation services. Task-shifting involves enhanced training of existing professionals or clinicians, who may have less or similar training. Such providers would be community healthcare workers, assistant therapists, and club trainers, where the training would be carried out by the transdisciplinary team of healthcare professionals. This would be a suitable rehabilitation framework to address the needs of various runners in these low-resource communities.[21]
The lack of resources, in lower-resourced communities, prevents runners from accessing services previously mentioned such as patient education, running gait training, exercise, use of orthoses, and multimodal rehabilitation,[6][21] thus it is vital to implement these in such communities.
Conclusion[edit | edit source]
As PFPS is a very common injury in runners, there are many modes of treatment available. This page explored the different types of treatments recommended for PFPS, and outlined how they all fit into the long-term care context of rehabilitation. It also outlined that these types of treatments may not be available or accessible in low-resource communities, and to accommodate runners in these communities, such rehabilitation services should be developed and operational in these geographical areas.
Resources[edit | edit source]
- Patellofemoral Pain Syndrome - Physiopedia
- Patellofemoral Pain Syndrome - OrthoInfo
- Patellofemoral Pain Syndrome - Mayo Clinic
- Runner’s Knee: What you need to know – WebMD
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 Lack S, Neal B, De Oliveira Silva D, Barton C. How to manage patellofemoral pain - Understanding the multifactorial nature and treatment options. Phys Ther Sport. 2018
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 Gaitonde DY, Ericksen A, Robbins RC. Patellofemoral Pain Syndrome. Am Fam Physician. 2019 Jan 15;99(2):88-94.
- ↑ 3.0 3.1 3.2 3.3 3.4 Logan CA, Bhashyam AR, Tisosky AJ, Haber DB, Jorgensen A, Roy A, Provencher MT. Systematic Review of the Effect of Taping Techniques on Patellofemoral Pain Syndrome. Sports Health. 2017 Sep/Oct;9(5):456-461.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 Marshall R, Hasnan N. Team Based Care. In: Chhabra, HS editor. ISCoS Textbook on Comprehensive Management of Spinal Cord Injuries. New Delhi : Wolters Kluwer, 2015
- ↑ MedStar Health. Ready to Race: Patellofemoral Syndrome. Available from: http://www.youtube.com/watch?v=hsn532wcB9k [last accessed 09/11/2021]
- ↑ 6.00 6.01 6.02 6.03 6.04 6.05 6.06 6.07 6.08 6.09 6.10 6.11 6.12 6.13 6.14 6.15 6.16 6.17 6.18 6.19 6.20 6.21 6.22 6.23 6.24 Kunene SH, Taukobong NP, Ramklass S. Rehabilitation approaches to anterior knee pain among runners: A scoping review. S Afr J Physiother. 2020 Jan 27;76(1):1342.
- ↑ 7.0 7.1 Brukner P, Khan K. Brukner & Khan's Clinical Sports Medicine: Injuries, Volume 1, 5e. North Ryde NSW: McGraw-Hill Education, 2017. Print.
- ↑ JoggingRevival.com. What Is Overpronation. Available from: http://www.youtube.com/watch?v=Wxx7O8HoOzI [last accessed 09/11/2021]
- ↑ LBG Medical. Foot with Large Range of Rearfoot Eversion. Available from: http://www.youtube.com/watch?v=fiHX1ZWUl6c [last accessed 09/11/2021]
- ↑ Dierks TA, Manal KT, Hamill J, Davis IS. Proximal and distal influences on hip and knee kinematics in runners with patellofemoral pain during a prolonged run. J Orthop Sports Phys Ther. 2008 Aug;38(8):448-56.
- ↑ 11.0 11.1 World Health Organisation. Primary Health Care. Available from: https://www.who.int/health-topics/primary-health-care#tab-tab_1 (accessed 30 June 2021)
- ↑ New World Encyclopedia. Health Care – Secondary Care. (accessed on 26 June 2021)
- ↑ King JC, Nelson TR, Blankenship KJ, Turturro TC, Beck AJ. Rehabilitation Team Function and Prescriptions, Referrals, and Order Writing. Rehabilitation Medicine: Principles and Practice (ed by Delisa JA). 4th Ed, Lippincott Williams & Wilkins, Philadelphia. 2005:1051-72.
- ↑ Esculier JF, Bouyer LJ, Dubois B, Fremont P, Moore L, McFadyen B, Roy JS. Is combining gait retraining or an exercise programme with education better than education alone in treating runners with patellofemoral pain?A randomised clinical trial. Br J Sports Med. 2018 May;52(10):659-666.
- ↑ Willy RW, Scholz JP, Davis IS. Mirror gait retraining for the treatment of patellofemoral pain in female runners. Clin Biomech (Bristol, Avon). 2012 Dec;27(10):1045-51.
- ↑ Willy RW, Davis IS. Varied response to mirror gait retraining of gluteus medius control, hip kinematics, pain, and function in 2 female runners with patellofemoral pain. J Orthop Sports Phys Ther. 2013 Dec;43(12):864-74.
- ↑ James Dunne. Running Footstrike - Breaking your injury cycle. Available from: http://www.youtube.com/watch?v=guCQpGF7nrg [last accessed 09/11/2021]
- ↑ LIVESTRONG.COM. How to Change From Heel to Forefoot Strike. Available from: http://www.youtube.com/watch?v=HP9mQrC3iVo [last accessed 09/11/2021]
- ↑ Medical City Dallas. Hip Abduction - Strengthening Exercise. Available from: http://www.youtube.com/watch?v=CP4LjhZ_Wq0 [last accessed 09/11/2021]
- ↑ Loyola Medicine. Loyola Medicine's Patellofemoral Pain Syndrome Home Exercise Program. Available from: http://www.youtube.com/watch?v=XMfZT9Hysnc [last accessed 09/11/2021]
- ↑ 21.00 21.01 21.02 21.03 21.04 21.05 21.06 21.07 21.08 21.09 21.10 Kunene ST, Taukobong N, Ramklass S. Community-based rehabilitation implementation framework to address patellofemoral pain amongst runners in under-resourced communities: Delphi consensus. South African Journal of Physiotherapy. 2021;77(1):7.
- ↑ Shih YF, Wen YK, Chen WY. Application of wedged foot orthosis effectively reduces pain in runners with pronated foot: a randomized clinical study. Clin Rehabil. 2011 Oct;25(10):913-23.
- ↑ McConnell Physiotherapy Group. MCCONNELL KNEE TAPING (OFFICIAL). Available from: http://www.youtube.com/watch?v=WbHXYnwUwws [last accessed 09/11/2021]
- ↑ John Gibbons. Kinesiology taping for patellofemoral syndrome (Knee pain). Available from: http://www.youtube.com/watch?v=s4i8njZ0WNE [last accessed 09/11/2021]
- ↑ Pelletier A, Sanzo P, Kivi D, Zerpa C. The effect of patellar taping on lower extremity running kinematics in individuals with patellofemoral pain syndrome. Physiother Theory Pract. 2019 Aug;35(8):764-772.
- ↑ Esculier, JF., Bouyer, L.J., Dubois, B. et al. Effects of rehabilitation approaches for runners with patellofemoral pain: protocol of a randomised clinical trial addressing specific underlying mechanisms. BMC Musculoskelet Disord 17, 5 (2016).