Models of Fatigue
Original Editor - Rebecca Willis
Top Contributors - Rebecca Willis and Lucinda hampton
Introduction[edit | edit source]
Exercise causes physiological and biochemical adaptations including the development of fatigue [1]. The development of fatigue is the body's mechanism to protect against the harmful effects of exercise, thus it limits the body's ability to perform [2]. Knowledge of the different models of fatigue, resulting from exercise, is important for physiotherapists to understand the training aims of an athlete's programme when improving performance during return from injury. This page outlines the common models used to explain the mechanisms behind fatigue.
Cardiovascular Model[edit | edit source]
This model suggests that exercise endurance is limited by the heart's ability to pump sufficient blood, and therefore oxygen, to the exercising muscles [3]. When the demand of the skeletal muscle exceeds the cardiac output, fatigue occurs. This is supported by the increase in cardiac output which leads to increases in exercise capacity. However, it is also argued that, if this is the case, then the heart (which also relies on an adequate blood and oxygen supply), would also suffer from oxygen deficiency, which would result in myocardial ischaemia [3]. Therefore, it can be hypothesised that there is a central 'governor' whereby receptors in the heart assess coronary blood flow and oxygen delivery. Before these reach a detrimental limit, the motor cortex reduces skeletal muscle activation, thus resulting in fatigue.
Energy Supply / Energy Depletion Model[edit | edit source]
This model suggests that fatigue is an inability to supply energy (ATP) at a fast enough rate, or a depletion in energy stores [2]. When endogenous carbohydrate stores are depleted, fatigue occurs. But, similar to the cardiovascular model, if muscle ATP stores are fully depleted, rigor occurs. Therefore it is hypothesised that there is a central 'governor' to defend against skeletal muscle rigor.
Biomechanical Model[edit | edit source]
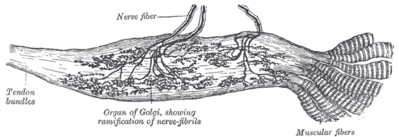
This model suggests fatigue is a result of movement inefficiency which results in increased VO2 requirements, increased metabolic accumulation, depletion of energy stores, and increased core body temperature [2]. It is suggested that muscle damage caused during the stretch-shortening cycle reduces the tolerance to move between muscle stretch and muscle contraction (amortization), thus resulting in a reduced force production. It is also suggested that the central nervous system interprets feedback from Golgi tendon organs to provide this protective mechanism, thus a longer amortization phase is felt as fatigue.
Psychological Model[edit | edit source]
This model suggests exercise is limited by the athlete's conscious effort based on sensory feedback [3]. It is measured by a rating of perceived exertion (RPE) scale and posits that athletes will anticipate the work required and modify their effort accordingly [2] which is supported by the placebo effect [4].
Muscle Recruitment Model / Central (Nervous System) Fatigue[edit | edit source]
This model suggests it is the failure of the central nervous system to recruit skeletal muscle that causes fatigue, as shown by reduced motor neuron output in EMG assessment of working muscles [6].This is brought about by a reduction in excitatory, and/or, an increase in inhibitory neural messaging [7].This change in neural messaging has several sources; changes in central neurotransmitter concentrations [6], feedback from rising body temperature, and feedback from skeletal muscle [3].
Conclusion[edit | edit source]
Different proponents will advocate different models of fatigue dependent upon their background, but fatigue is a result of several physiological processes that reduces the ability of muscle fibres to generate force [6]. It is the result of multiple peripheral systems interacting and integrating with the brain to modulate a response[8]. Specific training will produce physiological adaptations that delays the onset of fatigue; the focus of training will depend upon which model is being targeted. This page looks specifically at models as they relate to athletic performance and training, but the related Physiopedia page, Muscle Fatigue, delves further into fatigue as it relates to pathological conditions and the treatment of fatigue.
References[edit | edit source]
- ↑ Ament W, Verkerke GJ. Exercise and Fatigue. Sports Med [Internet] 2012 Oct 7 [Cited 2023 Apr 24]; 39:389–422.
- ↑ 2.0 2.1 2.2 2.3 Abiss C R, Laursen PB. Models to explain fatigue during prolonged endurance cycling. Sports Med. [Internet] 2005 [Cited 2023 Apr 24]; 35(10):865-98.
- ↑ 3.0 3.1 3.2 3.3 Noakes TD. Physiological models to understand exercise fatigue and the adaptations that predict or enhance athletic performance. Scand. J. Med. Sci. Sports [Internet] 2000 Jun [Cited 2023 Apr 24]; 10(3):123-145.
- ↑ Roelands B, Hurst P. The Placebo Effect in Sport: How Practitioners Can Inject Words to Improve Performance. Int J Sports Physiol Perform. [Internet] 2020 Jun 3 [Cited 2023 Apr 24]; 15(6):765–66.
- ↑ PEER_reviews. Why Do You Get Tired During Exercise? | Your Brain as the 'Central Governor'. Available from https://www.youtube.com/watch?v=FjTbo0twpQw [Last accessed 24/04/2023]
- ↑ 6.0 6.1 6.2 Tornero-Aguilera JF, Jimenez-Morcillo J, Rubio-Zarapuz A, Clemente-Suárez VJ. Central and Peripheral Fatigue in Physical Exercise Explained: A Narrative Review. Int. J. Environ. Res. Public Health [Internet] 2022 Mar 25 [Cited 2023 Apr 24]; 19:3909.
- ↑ Potvin JR, Fuglevand AJ. A motor unit-based model of muscle fatigue. PLoS Comput Biol. 2017 Jun 2 [Cited 2023 Apr 24]; 13(6):e1005581.
- ↑ Lambert, EV., St Clair Gibson, A., Noakes, TD., Complex systems model of fatigue: integrative homoeostatic control of peripheral physiological systems during exercise in humans. Br J Sports Med [Internet]. 2005 [cited 2023 May 22]; 39:52–62