Lower Leg and Foot Regional Pain and Gait Deviations
Top Contributors - Stacy Schiurring, Kim Jackson, Lucinda hampton and Jess Bell
Introduction[edit | edit source]
"The kinesiopathologic model was designed specifically to describe the mechanically related processes proposed to contribute to the development and course of low back pain (LBP). The basic premise is that LBP results from the repeated use of direction-specific (flexion, extension, rotation, lateral bending, or a combination of these) stereotypic movement and alignment patterns in the lumbar spine. The model proposes that the patterns begin as the result of adaptations of the musculoskeletal and neural systems due to repeated use of specific movements and alignments during daily activities. The nature and rate of the adaptations can be modified by intrinsic and extrinsic characteristics of the individual, for example, sex, anthropometrics, or typical activities of the person. The typical pattern is one in which, during performance of a movement (eg, forward bending) or assumption of a posture (eg, sitting), the lumbar spine moves into its available range in a specific direction more readily than other joints, such as the knees, hips, or thoracic spine."[1]
With the patient's pain as a guide, a goal of musculoskeletal physiotherapy is to identify the anatomical structures associated with the reported pain. Physiotherapists utilise orthopaedic tests to assist in symptom source identification. However, these clinical tests are often inconsistent in their ability to accurately identify the anatomical source of the patient's symptoms. Additionally, there is a poor correlation between imaging results and symptom source identification in the absence of trauma or pathology. These two statements suggest that musculoskeletal pain may often be anatomically and structurally indeterminable. The kinesiopathological approach is an alternative to these more traditional methods of diagnosis. This method calls for clinical practice to be guided by the identification and modification of kinematic or motor control impairments within a musculoskeletal function. By correcting deviant movement patterns to a more idealised movement pattern unique to a particular individual, subjective pain can be improved and function can be reestablished.[2]
Lower Leg Regional Pain[3][edit | edit source]
| Region of Pain | Relavent Diagnoses | Expected Gait Deviations |
|---|---|---|
| Calf |
| |
| Achilles |
|
|
Foot Regional Pain[3][edit | edit source]
| Region of Pain | Relavent Diagnoses | Expected Gait Deviations |
|---|---|---|
| Plantar heel |
(for more information, please see special topics at the end of this article) |
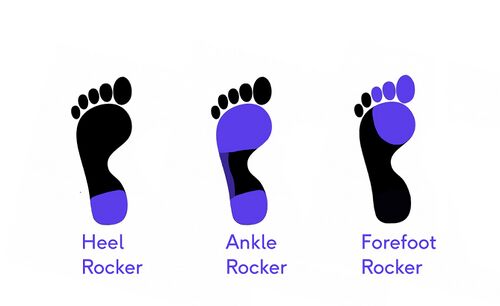
First period "heel rocker" ( heel contact):
Second period "ankle rocker" (transition from whole foot contact to forefoot contact only):
Third period "forefoot rocker" (during terminal stance):
|
| Great toe |
|
|
|
| |
| Forefoot |
|
|
Lower Leg and Foot Region Special Topics[edit | edit source]
Plantar heel pain syndrome[edit | edit source]
Special considerations for plantar heel pain syndrome:[3][7][8]
- Professional guidelines and or protocols do not include recommendations for gait analysis and training
- Available professional guidelines and protocols describe evaluation and treatment procedures which are clinically effective for plantar heel pain syndrome. However, they do not recommend gait analysis as part of the evaluation process or gait training. For physiotherapists, plantar heel pain syndrome is associated with gait therefore gait analysis and training should be part of a physiotherapy plan of care.
- Plantar heel pain syndrome differential diagnosis should include tendinopathy of intrinsic plantar flexor muscles
- Pain is NOT an indication for stretching exercises
- Limited range of motion is an indication for stretching exercises
It is possible to develop a sub-classification of plantar heel pain syndrome based on the movements that occur during the three periods of stance phase. This sub-classification is created using gait analysis.[3]
According to Dr Jacquelin Perry, the three time periods during stance include:[9]
- Heel rocker: the period of stance with only heel contact with the ground. Can also be called foot strike or impact loading.
- Ankle rocker: the period of stance when the whole foot is in contact with the ground. Can also be called mid-stance.
- Forefoot rocker: the period of stance with only forefoot contact with the ground. Can also be called terminal stance.
The sub-classification can be based on force per area per contact time during stance phase:[3]
- Force: Estimated to be 1.5 times body weight when walking. When running, that force is estimated to increase to be three times body weight.
- Time: During ambulation, single-limb support is two-thirds of stance; one-third of that period could be double support. Depending on ambulation velocity, single limb support occurs in roughly 0.6 seconds. If single limb stance phase is 0.6 seconds, divide that into three and each period of stance would be very quick, approximately 0.2 seconds each.
- Period of heel rocker: 1.5 body weight going into a relatively small area of the heel for a very brief period of time.
- Period of ankle rocker: the force per unit area of the foot is relatively lower because it is spread out over the forefoot and the hindfoot, a larger area, for a very short period of time.
- Period of forefoot rocker: the force per unit of area is going into a relatively small area of the forefoot for a very brief period of time.
- The first and last periods of stance are associated with greater risks as they have the greatest amount of force over a smaller body area.
| Stance time period | Possible gait deviations |
|---|---|
| Heel rocker |
|
| Ankle rocker |
|
| Forefoot rocker |
|
Windlass Effect[edit | edit source]
According to a 2004 study[10] published in the Journal of Athletic Training:
- A “windlass” is the tightening of a rope or cable.
- The plantar fascia "simulates a cable" attached between the calcaneus and the metatarsophalangeal (MTP) joints.
- Dorsiflexion during the propulsion phase of gait tightens the plantar fascia around the head of the metatarsal. This tightening of the fascia shortens the distance between the calcaneus and metatarsals to elevate the medial longitudinal arch. This shortening of the plantar fascia is the hallmark of the windlass mechanism principle.
- From heel strike to weight acceptance: foot pronation increases the distance between the calcaneus and metatarsals. This lengthening applies tension stress to the plantar fascia.
- From midstance through the propulsive phase (i.e. the period from the end of midstance when the heel lifts to toe off[11]): foot supination occurs causing the foot to become a rigid lever arm, using the windlass mechanism to propel gait. As with pronation, forces generated during supination also apply tension to the plantar fascia.[10][12]
The windlass test:[3]
- A length test for the plantar fascia, a passive structure
- A length test for the the intrinsic foot muscles, active structures
- When performing the test will see: (1) the arch rising, (2) slight supination of the forefoot, (3) slight external rotation of the tibia
- When performing the test, monitor for the presence or absence of joint crepitation
- Test in both weight bearing and non-weight bearing
You might like to view the following short video for more information on the windlass mechanism, and to see the windlass test performed in both weight bearing and non-weight bearing positions.
Leg length discrepancy[edit | edit source]
Two types of leg length discrepancy:[3]
- Anatomical leg length discrepancy: due to a physical osseous shortening of one of the lower limbs
- Functional leg length discrepancy: a unilateral asymmetry of one lower extremity without any shortening of the osseous components. The deformity is derived from admirable movements at the hip, knee, and or ankle.
Anatomical leg length differences can be measured both statically and dynamically. Gait analysis should also be performed to determine how the individual accommodates for that structural variation. Noting and assessing compensatory movements will help develop a physiotherapy plan of care and treatment interventions.
Possible expected gait deviations and or compensatory movements of leg length discrepancy:
| Longer leg | Shorter leg | |
|---|---|---|
| Foot | Pronation | Supination |
| Ankle | Dorsiflexation | Plantarflexion |
| Knee | Flexion | Extension |
| Hip |
|
|
| Pelvis/Ilium |
|
|
Resources[edit | edit source]
Optional Recommended Reading:
- Bramah C, Preece SJ, Gill N, Herrington L. Kinematic characteristics of male runners with a history of recurrent calf muscle strain injury. International Journal of Sports Physical Therapy. 2021;16(3):732.
- Cholewicki J, Breen A, Popovich Jr JM, Reeves NP, Sahrmann SA, Van Dillen LR, Vleeming A, Hodges PW. Can biomechanics research lead to more effective treatment of low back pain? A point-counterpoint debate. journal of orthopaedic & sports physical therapy. 2019 Jun;49(6):425-36.
- Lehman GJ. The role and value of symptom-modification approaches in musculoskeletal practice. journal of orthopaedic & sports physical therapy. 2018 Jun;48(6):430-5.
References[edit | edit source]
- ↑ Cholewicki J, Breen A, Popovich Jr JM, Reeves NP, Sahrmann SA, Van Dillen LR, Vleeming A, Hodges PW. Can biomechanics research lead to more effective treatment of low back pain? A point-counterpoint debate. journal of orthopaedic & sports physical therapy. 2019 Jun;49(6):425-36.
- ↑ Lehman GJ. The role and value of symptom-modification approaches in musculoskeletal practice. journal of orthopaedic & sports physical therapy. 2018 Jun;48(6):430-5.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 Howell, D, Lower Leg and Foot Regional Pain and Gait Deviations. Gait Analysis. Plus. 2022
- ↑ Bramah C, Preece SJ, Gill N, Herrington L. Kinematic characteristics of male runners with a history of recurrent calf muscle strain injury. International Journal of Sports Physical Therapy. 2021;16(3):732.
- ↑ Wang J, Mannen EM, Siddicky SF, Lee JM, Latt LD. Gait alterations in posterior tibial tendonitis: A systematic review and meta-analysis. Gait & Posture. 2020 Feb 1;76:28-38.
- ↑ Van Der Vlist AC, Breda SJ, Oei EH, Verhaar JA, de Vos RJ. Clinical risk factors for Achilles tendinopathy: a systematic review. British journal of sports medicine. 2019 Nov 1;53(21):1352-61.
- ↑ Shane McClinton PT, Bryan Heiderscheit PT, McPoil TG, Flynn TW. Physical therapist decision-making in managing plantar heel pain: cases from a pragmatic randomized clinical trial. Physiotherapy Theory and Practice. 2018 Jul 6.
- ↑ Riel H, Plinsinga ML, Delahunt E, Jensen MB, Landorf KB, van Middelkoop M, Roddy E, Rathleff MS, Vicenzino B, Olesen JL. Large variation in participant eligibility criteria used in plantar heel pain research studies-a systematic review. Journal of foot and ankle research. 2022 Dec;15(1):1-8.
- ↑ Perry, J. and Burnfield, J. (1992) Gait Analysis: Normal and Pathological Function. SLACK Incorporated, New Jersey.
- ↑ 10.0 10.1 Bolgla LA, Malone TR. Plantar fasciitis and the windlass mechanism: a biomechanical link to clinical practice. Journal of athletic training. 2004 Jan;39(1):77.
- ↑ Kawalec JS. 12 - Mechanical testing of foot and ankle implants. In Friss E, editor. Mechanical testing of orthopaedic implants. Woodhead Publishing, 2017. p231-53.
- ↑ Williams LR, Ridge ST, Johnson AW, Arch ES, Bruening DA. The influence of the windlass mechanism on kinematic and kinetic foot joint coupling. Journal of Foot and Ankle Research. 2022 Dec;15(1):1-1.
- ↑ YouTube. What is The Windlass Mechanism of The Foot? | James Dunne. Available from: https://www.youtube.com/watch?v=vzTdSXgTCsY [last accessed 29/06/2022]