Interphalangeal Joints of the Hand
Original Editor - Denys Nahornyi
Top Contributors - Denys Nahornyi, Kim Jackson, Lucinda hampton, Shaimaa Eldib and Aminat Abolade
Description[edit | edit source]
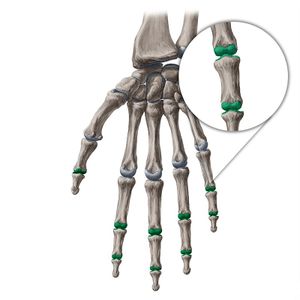
The interphalangeal joints of the hand are the hinge joints between the phalanges of the fingers that provide flexion towards the palm of the hand.[1]
Anatomy[edit | edit source]
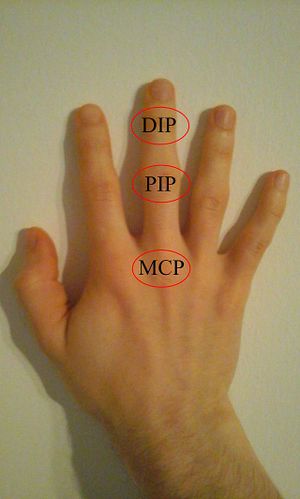
There are two sets in each finger (except in the thumb, which has only one joint)
- Proximal interphalangeal joints" (PIJ or PIPJ), those between the first (also called proximal)
- Distal interphalangeal joints" (DIJ or DIPJ), those between the second (intermediate) third (distal) phalanges
Anatomically, the proximal and distal interphalangeal joints are very similar. There are some minor differences in how the palmar plates are attached proximally and in the segmentation of the flexor tendon sheath, but the major differences are the smaller dimension and reduced mobility of the distal joint.[2]
Articulating Surfaces[edit | edit source]
Each interphalangeal joint is composed of the head of the more proximal phalanx and the base of its distal counterpart. This means that, for example, the proximal interphalangeal joint is formed by the union of the head of the proximal phalanx with the base of the middle phalanx. This same pattern applies to the distal interphalangeal joint, meaning that it is formed by the articulation of the head of the middle phalanx with the base of the distal phalanx.
Closer inspection of the phalangeal head reveals two curved condylar processes with a shallow groove in between. These condyles are received by two concavities of reciprocal size and shape on the base of the distally lying phalanx. Between these two concavities is a raised ridge of bone that glides within the groove of the phalangeal head, promoting intraarticular stability. These joint surfaces are covered by a layer of hyaline cartilage that extends further palmarly than dorsally, creating a proximal articular surface which is greater than the distal surface. Unlike the metacarpophalangeal joints, there is little articular surface on the dorsal aspect, and therefore little hyperextension.
The point of articulation does not occur directly at the apex of the condylar processes, but rather on their inner sloping surfaces. This results in the radii of the condyles of the phalangeal head being greater than that of the convex surfaces of the phalangeal base, leaving the joint markedly incongruent. This incongruency manifests as a small intercondylar joint space in most people.[3]
Ligaments & Joint Capsule[edit | edit source]
Surrounding each interphalangeal joint is a fibrous joint capsule, the inner lining of which is comprised of a synovial membrane. Strengthening each joint capsule are two collateral ligaments and a palmar ligament, also known as a palmar/volar plate. Dorsally, the joint capsule is strengthened by a broadening of the extensor tendons. This extensive ligamentous contribution to each joint capsule increases the articular surface of the phalangeal base, improving joint congruence.
Collateral ligaments[edit | edit source]
The collateral ligaments course on either side of each interphalangeal joint, arising from the head of the more proximal phalanx and extending to the palmar, or volar, aspect of its distal counterpart. Arising from each collateral ligament is an accessory ligament, which extends anteriorly to attach to the fibers of the palmar ligament. These ligaments help to prevent excessive adduction-abduction movements of the interphalangeal joints.
Palmar ligament[edit | edit source]
The palmar ligament (a.k.a palmar/volar plates) is a thick plate of fibrocartilage located on the palmar surface of each interphalangeal joint. This ligament has a characteristic upside down “U” shape, with its distal part arching across the base of the distally lying phalanx to blend with the accessory collateral ligaments. Proximally, the legs of the palmar ligament blend in with the periosteum of the body of the more proximally lying phalanx. These are termed ‘check rein’ ligaments and serve to prevent excessive hyperextension of the joint.[4]
Muscles[edit | edit source]
The extraordinary dexterity exhibited by the fingers is reflected in the number of muscles that can act upon them. Both intrinsic and extrinsic hand muscles are responsible for producing flexion-extension movements at the interphalangeal joints of the hand.
| Muscles acting on the interphalangeal joints of the hand and movements they produce | |
| Flexion | IP joint of thumb - Flexor pollicis longus
PIP joints of digits 2-5 - Flexor digitorum superficialis, flexor digitorum profundus DIP joints of digits 2-5 - Flexor digitorum profundus |
| Extension | IP joint of thumb - Extensor pollicis longus
PIP joints of digits 2-5 - Extensor digitorum, lumbricals, dorsal interossei, extensor indicis (digit 2), palmar interossei (digits 2,4,5) DIP joints of digits 2-5 - Extensor digitorum, lumbricals, dorsal interossei, extensor indicis (digit 2), palmar interossei (digits 2,4,5) |
Flexion of the interphalangeal joint of the thumb is accomplished through the action of the flexor pollicis longus muscle. The proximal interphalangeal joints of digits 2-5, meanwhile, are flexed via the flexor digitorum superficialis and flexor digitorum profundus, the latter of which also extends to the distal phalanx, and is therefore the only muscle capable of flexing the distal interphalangeal joints.
Extension of the interphalangeal joint of the thumb is performed by the extensor pollicis longus. Both the proximal and distal interphalangeal joints of digits 2-5 are extended through the actions of extensor digitorum, lumbricals, and dorsal interossei. Digit 2, the index finger, gets additional extension via the extensor indicis, while the palmar interossei assist with extension of digits 2, 4, and 5. The muscles responsible for extending digits 2-5 do so through their tendinous aponeurotic insertion into the extensor expansion. This hood-like expansion extends down the length of digits 2-5, and is anchored on each side by the palmar ligament. It functions to maintain the direction of pull of the extensor tendons in the midline of each digit.[4]
Function[edit | edit source]
The function of the interphalangeal joints of the hand to permit fine motor movements in the digits. To accomplish this, these joints facilitate movement within only one degree of freedom: flexion - extension.
Motions Available[edit | edit source]
The morphology of the interphalangeal joints of the hand permits flexion and extension as their only active movements. However, a small degree of passive accessory movements is allowed primarily at the distal interphalangeal joints of digits 2-5.
Range of Motion[edit | edit source]
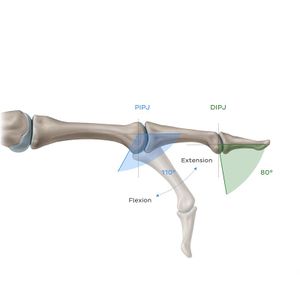
The range of motion of the thumb consists of up to about 90° flexion and 10° extension, with passive hyperextension possible when a large amount of force is applied to the distal phalanx. The degree of flexion of the proximal interphalangeal joints increases slightly across digits 2-5, however, can be generally said to be in the range of 100° to 110°. In the case of the distal interphalangeal joints, digit 3 exhibits the greatest degree of flexion (80°), with digit 5 featuring the least (70°).
Closed Packed Position[edit | edit source]
Full extension
Open Packed Position[edit | edit source]
Slight flexion
Osteokinematics[edit | edit source]
Flexion and extension occur in the thumb about a transverse axis that crosses through the middle of the neck of the proximal phalanx. Strong collateral ligaments prevent any passive accessory rotational or lateral movements of the interphalangeal joint of the thumb. Flexion and extension of digit 2, often referred to as the index finger, occurs entirely in the sagittal plane. More medially lying digits, however, have their flexion and extension occur increasingly obliquely so as to better oppose the thumb.[5]
Pathology/Injury[edit | edit source]
- Osteoarthritis: The distal interphalangeal (DIP) joint is actually the most common location on the body for osteoarthritis (OA). In fact, according to a study evaluating the frequency of hand arthritis, OA at the DIP joint occurs in approximately 58% of individuals age 60 years and older. The visible changes may be due to the formation of a Heberden’s node; a calcified spur or osteophyte that forms on the top or the side of the joint. These symptoms often lead to functional concerns including difficulty with household tasks, opening containers, writing, and manipulating small objects;[6]
- Mallet Finger;
- Swan-Neck Deformity.
Techniques[edit | edit source]
Palpation[edit | edit source]
- Gently squeeze across the joints in a methodical order, assessing for the nature of any swelling present
- Remember that inflamed joints are painful and must be examined gently
- Look at patient’s face if possible while palpating to discern any pain
- Interphalangeal (IP) joint must be palpated in turn and compared to the opposite side. This is best done by holding the joint between your thumb and forefinger and palpating gently
- If the swollen joint feels soft, warm and diffusely tender it is usually due to acute synovitis. If it is hard it is usually due to bony overgrowth.[7]
Examination[edit | edit source]
Active movement[edit | edit source]
- Ask about any pain the patient feels, particularly with which movements
- Pain in most or all directions is the most sensitive sign of synovitis; pain in one plane of movement is more characteristic of a localised intra- or peri-articular lesion.
- Ask about stiffness
- This is related to fluid retention in the peri-articular tissues and is an indication of the inflammatory processes
- Function
- The key to testing active movement is to work out what the patient can and can’t do functionally. Ask what their pain or stiffness stops them doing. To test this more fully you can then ask them to:
- Squeeze your finger (fully flex the hand powerfully)
- Pick up a coin from a table (pincer grip)
- Pretend to lock a door with a key (key grip)
- Do up a button (coordination and fine motor control)
- These movements are common in everyday life so are a useful gauge of what the patient can and can’t do.[7]
- The key to testing active movement is to work out what the patient can and can’t do functionally. Ask what their pain or stiffness stops them doing. To test this more fully you can then ask them to:
Treatment[edit | edit source]
According to research, there is evidence that gentle exercise with osteoarthritis will assist with decreasing pain and increasing grip strength and that joint protection techniques are effective at decreasing pain. Heat or paraffin may also be used to assist with decreasing pain and improving mobility.
Additionally, a splint for the DIP joint is a common recommendation for the treatment of DIP joint arthritis. A cohort study of individuals with DIPJ arthritis had a 66% improvement in pain symptoms with the use of a splint during activity. A more recent study also found that use of a splint at night during sleep, for 3 months, decreased pain and improved the deformity associated with DIP joint arthritis.[6]
Resources[edit | edit source]
| [8] |
[9] |
References[edit | edit source]
- ↑ Peter B, Alain G, Finger bone and joint injuries. London: Taylor & Francis, 1999.
- ↑ Mee SD. Anatomy of the proximal interphalangeal joint and splintage of flexion contracture. British Journal of Therapy and Rehabilitation. 1995 Nov 2;2(11):604-10.
- ↑ Dumont C, Albus G, Kubein-Meesenburg D, Fanghänel J, Stürmer KM, Nägerl H. Morphology of the interphalangeal joint surface and its functional relevance. The Journal of hand surgery. 2008 Jan 1;33(1):9-18.
- ↑ 4.0 4.1 Moore KL, Dalley AF, Agur AMR. Clinically Oriented Anatomy (7th ed.). Philadelphia: Lippincott Williams & Wilkin, 2014.
- ↑ Pang EQ, Yao J. Anatomy and biomechanics of the finger proximal interphalangeal joint. Hand clinics. 2018 May 1;34(2):121-6.
- ↑ 6.0 6.1 3-Point Products. DIP Joint Osteoarthritis: How to Treat this Common Form of Arthritis. Available from: https://www.3pointproducts.com/blog/health-arthritis-finger-and-toe-conditions/dip-joint-osteoarthritis-how-to-treat-this-common-form-of-arthritis#:~:text=The%20distal%20interphalangeal%20(DIP)%20joint,age%2060%20years%20and%20older. (accessed 29 October 2020).
- ↑ 7.0 7.1 Oxford medical education. Hand Examination. Available from: http://www.oxfordmedicaleducation.com/clinical-examinations/rheumatology-examination/hand-examination/ (accessed 29 October 2020).
- ↑ online video, https://www.youtube.com/watch?v=m8tkPnJcLpM, last accessed 29/10/20
- ↑ online video, https://www.youtube.com/watch?v=qHJ-C1MdI3Y, last accessed 29/10/20