Implementation Science: Pre-Implementation Stage
Top Contributors - Stacy Schiurring, Jess Bell, Tarina van der Stockt and Kim Jackson
Introduction[edit | edit source]
"Pre-implementation work is an important element of the early phase of preparing the setting for the introduction of an intervention, and the factors contributing towards the creation of an optimal pre-implementation community context are under-acknowledged."[1]
As rehabilitation is recognised as a complex multi-disciplinary process with many moving parts, within complex multi-level healthcare systems and involving multiple professionals, patients, families and care-providers[2] pre-implementation efforts are important than ever. Adopting, implementing or sustaining any new rehabilitation interventions is challenging. Have you ever wondered why some professionals seem to adopt these interventions more easily, when others do not and why this intervention works in some settings and not in others? When rehabilitation professionals implement new interventions in lower middle-income countries, they can experience a wide range of challenges at a systems, healthcare provider and or at a patient level. While many implementation challenges exist, implementation science can provide a way of thinking about these challenges and can facilitate implementation efforts.
This article can serve as a guide on how to plan implementation process efforts to adopt, adapt, spread or sustain new interventions.
What is implementation science? Watch this short video for a summary of this field of study.
Building Implementation Science Capability[edit | edit source]
The need to build implementation science expertise is recognised as urgently required to bridge the gap between evidence and practice, particularly in resource-poor or low-middle income countries (LMICs).[4][5] [6]
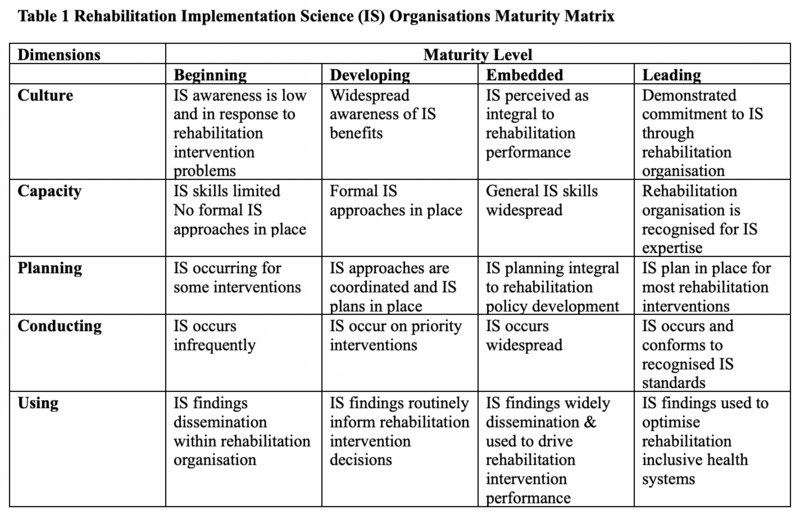
All rehabilitation leaders and stakeholders and their organisations have differing implementation science capability. Thus, it is important to reflect upon the implementation science maturity of an organisation to establish a baseline, then set about identifying implementation science strengths, gaps, readiness and priorities.
Challenges to Implementing Evidenced-Based Interventions in LMICs[edit | edit source]
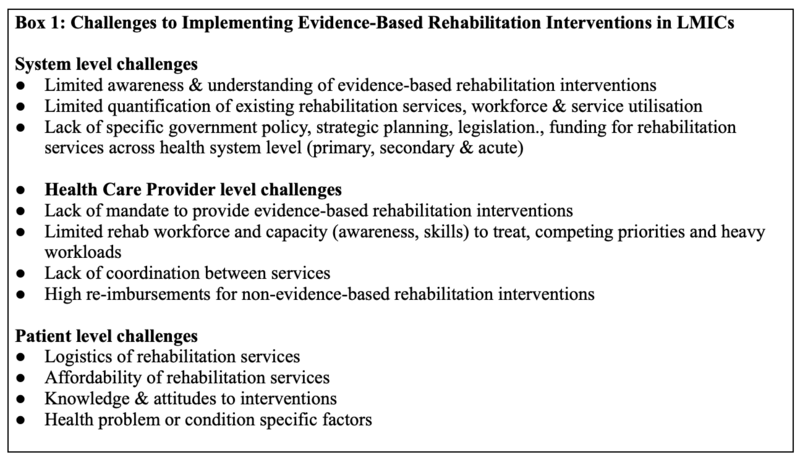
Please read this page to review the challenges of implementing evidence-based rehabilitation interventions that are known to exist in LMICs.
Challenges exist at a:
- System level: lack of specific government policy, strategic planning, legislation and funding for rehabilitation services across all health system level
- Healthcare provider level: limited rehabilitation workforce, capacity, competing priorities and heavy workloads
- Patient level: knowledge and attitudes about interventions

Implementation Science Terms[edit | edit source]
Below are listed many terms that are used in the field of implementation science, please review and reflect upon these key implementation terms and definitions, as they are key thinking about facilitating the implementation of evidence-based rehabilitation interventions.
Understanding the Intervention[edit | edit source]
The questions in Box 3 were designed to encourage thought about evidence-based rehabilitation interventions, irrespective of whether you are referring to adopting, implementing or sustaining a new rehabilitation intervention.
Rehabilitation intervention evidence is growing every day. Principles and guidance on rehabilitation interventions are increasingly available such as:
- NHS Commissioning Guidance for Rehabilitation
- World Health Organization Package of Rehabilitation Interventions Information Sheet
Despite the wealth of information, the uptake of this evidence into practice is a slow process, especially in lower-middle income countries. The translation from clinical research to clinical practice can take anywhere between 10-20 years.[9] With so much available information, it is easy to become overwhelmed when deciding what interventions to implement. It is of great benefit to utilise a comprehensive approach to explore and understand the chosen intervention. This is done by focusing on six key intervention topics:
- Needs
- Fit
- Resources
- Evidence
- Usability
- Capacity
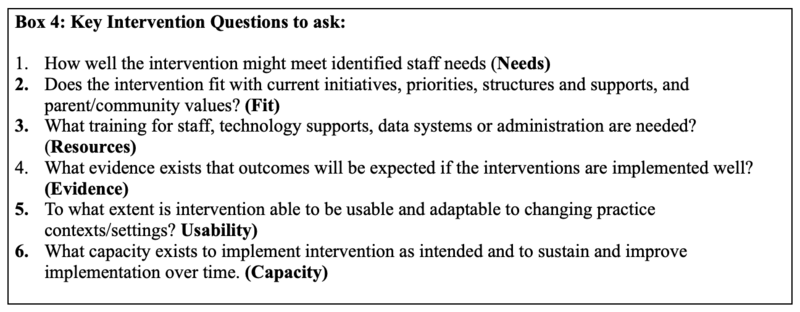
These six questions are based upon an existing implementation science exploration and planning tool that can also inform evaluation: the Hexagon Discussion and Analysis Tool.
Hexagon Tool[edit | edit source]
The Hexagon Discussion and Analysis Tool is used by organisations to evaluate the fit and feasibility of implementing programmes within a given context. This tool facilitates team discussion and ensures that diverse perspectives are represented in a discussion of the six contextual fit and feasibility indicators (please see Box 4).[10]
The Hexagon Tool can be used at any stage in the implementation process to determine its fit with the local context. When used early in the process, it can help identify possible new programmes or practices to implement. When used later in the process, it can help diagnose implementation challenges related to contextual fit.[10]
Understanding Context[edit | edit source]
In implementation science, the term context is used to describe and refer to all the potential factors or challenges that may influence adoption, effectiveness and sustainability of interventions. The questions in Box 5 were designed to encourage thinking about the context within which the evidence-based rehabilitation intervention is designed to help patients address the impact of physical, cognitive, psychosocial and mental health problems and conditions.
There are multiple contextual factors and levels (inner and outer) related to the organisation that are instrumental to implementation. For example, the inner context is comprised of internal organisation characteristics that drive implementation, such as the institution’s leadership, structures, resources, internal policies, staffing, practices, and provider factors (e.g., attitudes, beliefs). The outer context refers to the external environment that influences organisational implementation. These include policies outside the organisation, consumers, relationships across organisations such as funding agencies, health departments, and advocacy groups.[11]
These inner and outer setting factors also interact with one another and the intervention itself (i.e., how it fits within the organisation and culture) to influence implementation. Evidence is also building about ‘Bridging factors’ that refer to the relationships between the inner and outer contexts to guide implementation (e.g., academic-community partnerships).[11]
Given the increasing information about the Contextual challenges to implementing rehabilitation interventions, it is easy to become overwhelmed when assessing what may be affected by the new implementation intervention. It is beneficial to use a more comprehensive approach to explore and understand the inner and outer contextual factors or challenges across the three implementation phases: Pre-Implementation, Implementation and Sustainment.
Box 6 provides examples of key inner and outer contextual factors (barriers or facilitators) at the individual and organisational level – framed as questions that are known to influence implementation outcomes, such as: feasibility, acceptability, appropriateness and fidelity of implementation.
These six questions are based upon several existing implementation science exploration and planning or determinants frameworks that can also inform evaluation. Listed below are commonly used implementation planning frameworks that can identify barriers and facilitators to key implementation outcomes, namely feasibility, acceptability, uptake, and fidelity.
Please follow the listed links for more information on these implementation planning frameworks:
Stakeholders[edit | edit source]
In rehabilitation, multiple key stakeholders are essential to the implementation process and can include: staff within a clinic or service, such as frontline rehabilitation professionals who deliver services; organisational managers and administration staff who support the delivery of rehabilitation services; clients who receive services; or staff external to the clinic or service such as policymakers who fund and make decisions that can support the implementation of interventions.[12]
Stakeholder engagement at the beginning and throughout the implementation process can enhance the acceptability of interventions to rehabilitation clients and providers and improve reach (the number of eligible people taking part in the intervention) and sustainability (changes over time in numbers of eligible people taking part in the intervention).[12]
Understanding Key Stakeholders[edit | edit source]
It is important to understand the key stakeholders, including their knowledge, beliefs and capacity to adopt them.
The questions in Box 7 were designed to help understand the key Stakeholders who are key to implementing the evidence-based rehabilitation interventions, irrespective of whether you are referring to adopting, implementing or sustaining a new rehabilitation intervention.
Engaging Key Stakeholders[edit | edit source]
Engaging key stakeholders is a critical part to successful implementation of evidence-based interventions. It is firstly important to recognise that, just as there are multiple stakeholders potentially key to implementation, the timing and nature of stakeholder engagement and engaging stakeholders across multiple levels of an implementation is recommended best practice for implementation.[12]
Engagement is a process, with differing phases that align and fit with the stakeholder’s differing roles, interests and influence and the implementation process itself. Stakeholders can be engaged by informing, involving, consulting, collaborating, or empowering them into the implementation process. These different levels or phases of engagement is based upon the International Association for Public Participation (IAP2) spectrum. Thinking about stakeholder engagement in this way allows for the use an implementation science mindset to successfully engage multiple stakeholders across multiple levels of an implementation ecosystem (e.g., policy/legislative, funders, community, organisational, provider, client/patient).
These five questions are based upon the International Association of Public Participation (IAP2) stakeholder engagement framework and the CFIR framework.
Conclusion[edit | edit source]
The pre-implementation stage of implementation science uses a comprehensive approach to explore and understand the intervention to be implemented in a given situation. This stage focusses on six key intervention topics: needs, fit, resources, evidence, usability and capacity to implement.
Given the multiple challenges to implementing rehabilitation interventions, a comprehensive approach is needed to explore and understand the inner (organisational setting) and outer (external to the organisation) factors across the implementation phases: Pre-Implementation, Implementation and Sustainment.
It is essential to consider who is needed to engage in what is implemented, and that engaging the key stakeholders throughout the implementation process can enhance the acceptability, reach and sustainability of interventions to rehabilitation clients.
Optional Resources[edit | edit source]
Optional Video:
Please view this approximately 13-minute video for a detailed discussion on engaging stakeholders.
Recommended Reading:
- Bauer MS, Damschroder L, Hagedorn H, Smith J, Kilbourne AM. An introduction to implementation science for the non-specialist. BMC psychology. 2015 Dec;3(1):1-2.
- Holcomb J, Ferguson GM, Sun J, Walton GH, Highfield L. Stakeholder engagement in adoption, implementation, and sustainment of an evidence-based intervention to increase mammography adherence among low-income women. Journal of Cancer Education. 2021 Mar 22:1-0.
- Paré G, Sicotte C, Poba-Nzaou P, Balouzakis G. Clinicians' perceptions of organizational readiness for change in the context of clinical information system projects: insights from two cross-sectional surveys. Implementation Science. 2011 Dec;6(1):1-4.
References[edit | edit source]
- ↑ Ellis J, Band R, Kinsella K, Cheetham-Blake T, James E, Ewings S, Rogers A. Optimising and profiling pre-implementation contexts to create and implement a public health network intervention for tackling loneliness. Implementation Science. 2020 Dec;15(1):1-1.
- ↑ Morris JH, Bernhardsson S, Bird ML, Connell L, Lynch E, Jarvis K, Kayes NM, Miller K, Mudge S, Fisher R. Implementation in rehabilitation: a roadmap for practitioners and researchers. Disability and rehabilitation. 2020 Oct 22;42(22):3265-74.
- ↑ YouTube. Implementation Science Introduction | Implementation Scientists. Available from: https://www.youtube.com/watch?v=i_l5OsxAxao [last accessed 23/04/2022]
- ↑ Alonge O, Rodriguez DC, Brandes N, Geng E, Reveiz L, Peters DH. How is implementation research applied to advance health in low-income and middle-income countries?. BMJ Global Health. 2019 Mar 1;4(2):e001257.
- ↑ Ridde V. Need for more and better implementation science in global health. BMJ Global Health. 2016 Aug 1;1(2):e000115.
- ↑ Semeere AS, Semitala FC, Lunkuse O, Katahoire A, Sewankambo NK, Kamya MR. An assessment of implementation science research capacity in Uganda. Health research policy and systems. 2021 Dec;19(1):1-0.
- ↑ Grimmer K, Louw Q, Dizon JM, Brown SM, Ernstzen D, Wiysonge CS. A South African experience in applying the adopt–contextualise–adapt framework to stroke rehabilitation clinical practice guidelines. Health Research Policy and Systems. 2019 Dec;17(1):1-4.
- ↑ 8.0 8.1 Leonard E, de Kock I, Bam W. Barriers and facilitators to implementing evidence-based health innovations in low-and middle-income countries: a systematic literature review. Evaluation and Program Planning. 2020 Oct 1;82:101832.
- ↑ Novak I, te Velde A, Hines A, Stanton E, Mc Namara M, Paton MC, Finch-Edmondson M, Morgan C. Rehabilitation Evidence-Based Decision-Making: The READ Model. Frontiers in Rehabilitation Sciences. 2021:51.
- ↑ 10.0 10.1 National Implementation Research Network. The Hexagon: An Exploration Tool. Available from: https://nirn.fpg.unc.edu/sites/nirn.fpg.unc.edu/files/imce/documents/NIRN%20Hexagon%20Discussion%20Analysis%20Tool_September2020_1.pdf (accessed 23/04/2022).
- ↑ 11.0 11.1 Paré G, Sicotte C, Poba-Nzaou P, Balouzakis G. Clinicians' perceptions of organizational readiness for change in the context of clinical information system projects: insights from two cross-sectional surveys. Implementation Science. 2011 Dec;6(1):1-4.
- ↑ 12.0 12.1 12.2 Holcomb J, Ferguson GM, Sun J, Walton GH, Highfield L. Stakeholder engagement in adoption, implementation, and sustainment of an evidence-based intervention to increase mammography adherence among low-income women. Journal of Cancer Education. 2021 Mar 22:1-0.
- ↑ Youtube. Implementation Strategies | IRL. Available from: https://www.youtube.com/watch?v=eMesZs9R0L8[last accessed 11/05/2022]