Gluteal Fibrosis
Original Editor - Khloud Shreif
Top Contributors - Khloud Shreif
Clinically Relevant Anatomy[edit | edit source]
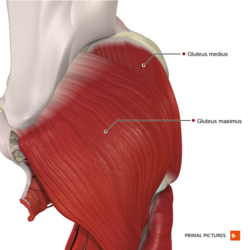
Gluteal muscles/ buttock muscles are muscles at the back of the thigh and formed of three layers; gluteus maximus, the superficial layer and the largest muscle, it is important as one of hip extensors and to maintain erect posture. Gluteus medius the middle layer on the lateral aspect of the pelvis below the iliac crest and it is important as a main hip abductor muscle. Gluteus minimus the deep layer and the smallest one of the gluteal muscles and helps with hip abduction and internal rotation.
Mechanism of Injury / Pathological Process[edit | edit source]
Gluteal fibrosis/ gluteal contracture was reported early in 1970s by Valderrama, defined as fibrotic infiltration changes of gluteal muscles, most commonly associated with intramuscular injections that may cause serious functional limitation of hip joint movements[1], patients with gluteal contracture will present with hip abducted and externally rotated[2]. Acquired gluteal fibrosis/ contracture is the most common type, the prevalence increase when the injection was in younger ages.
The mechanism / pathophysiology of GF/ GMC seems to have more than one hypothesis; congenital, idiopathic that usually associated with some diseases such as cerebral palsy, brain atrophy, poliomyelitis[3], or acquired that is the most common type and happen because of intramuscular gluteal injection it known as “Injection-Contracture”, or injuries around the hip[2].
Classifications of GMC/ GF[edit | edit source]
The classifications bases on anatomical changes and clinical manifestations, classified into three levels and three types as following:[4]
| Classifications according to the level. | |
| Level I
(mild) |
Outward rotation of the lower limb is mild, the abduction contracture is less than 15° with 90° flexion of both hip and knee joints or adduction range is less than 20° with no flexion. Ober's sign and frog squatting sign are weakly positive. The limp gait is not obvious and lateral pelvic inclination on the anteroposterior radiograph is less than 10° |
| Level II
(moderate) |
Outward rotation of the lower limb is moderate, the abduction contracture ranges from 15° to 60°with 90° flexion of both hip and knee joints, or the adduction range is less than 10° with no flexion. Ober's sign and frog squatting sign are positive. The limp gait is obvious and the lateral pelvic inclination on the anteroposterior radiograph is less than 20° |
| Level III
(server) |
Outward rotation of the lower limb is severe, the abduction contracture is more than 60° with 90° flexion of both hip and knee joints or the adduction range is less than 0° with no flexion. Ober's sign and frog squatting sign is strongly positive. The limp gait is more obvious and lateral pelvic inclination on the anteroposterior radiograph is more than 20° |
| Classification according to type | |
| Type MA | Gluteus maximus contraction type |
| Type MEI | Gluteus medius and minimus contraction type |
| Type AGM | Gluteus maximus, medius and minimus contraction type (All gluteal muscle contraction type |
Prevalence[edit | edit source]
GF/ GMC reported worldwide we can find it in Turkey, Iraq, England, Spain, Germany, Italy, Poland, Belgium, Uganda, the U.S, China, South Korea, India[5], but in china the incidence rate of childhood range from 1–2.5% from overall childhood and that a high percentage. In Africa the injection of quinine (used to treat malaria) intramuscular is the reported cause for GF[6].
Clinical Presentation[edit | edit source]
- Toe- out gait.
- Awkward gait be more obvious with running.
- Positive ober's test.
- Excessive hip external rotation and abduction when the hip is flexed.
- Frog leg posture at squatting or sitting.
- Difficulty in crossing legs.
- leg length discrepancy, the affected leg will be the longer it may be due to pelvic obliquity or prolonged traction of contracture bands.
- Palpable contracture bands.
- Skin dimples over the buttocks[5] or cone shaped buttocks[2].
- Usually there may be snapping sound at squatting because of the gliding movement of fibrotic bands over the greater trochanter[7].
Diagnostic Procedures[edit | edit source]
At first we need to exclude first poliomyelitis and other diseases; cerebral palsy, neuromuscular disorders, or other hip abnormalities are important to be ruled out through imaging and clinical examination.
Diagnostic ultrasound: it will show stripes of condensed sound waves (hyperechoic muscles) it had 88.9%sensitivity and 83.3% for specificity.
Magnetic Resonance Imaging MRI: it will show intramuscular atrophic changes and fibrotic cord that will be more common in the upper-third of the gluteus maximus, the fibrotic change may extend to the muscle's tendon, groove depression at the musculotendinous junction and external rotation of the proximal femur because of medial retraction of the muscle[8].
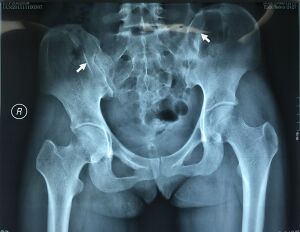
Radiography X- ray: early stage there will be no obvious changes but, with disease progression there will be iliac hyperdense line over the posterior iliac spine, pelvic obliquity, or coxa valga are other signs may be visible on x ray[2].
Outcome Measures[edit | edit source]
Ober's test, used during surgeries to assess and evaluate the release of tissue.
Management / Interventions[edit | edit source]
Surgical management[edit | edit source]
Surgical intervention is the gold standard for GF/GMC management there are different operative methods. Arthroscopic intervention
New minimally invasive surgery
It was introduced in 2012 and one of it's benefits, it can be used for all levels of injury. It is performed through small incisions around greater trochanter. It is effective for deeper contracted tissues. Physical examination to detect the borders of the contracture is important to be done before surgery[9].
Endoscopic release
That was first carried by Liu in 2009 [10]by using radiofrequency ablation to release the contracted tissue. At first detecting the important anatomical landmark; borders of contracted glutei, greater trochanter, and sciatic nerve. It is mainly used for level I and level II, and may be used for level III[11].
Conventional open release
The surgical approach include releasing of soft tissue until the contraction region of the gluteus maximus, then Ober's test used to reassess if it is positive, release of Gluteus medius, and minimus will be done.
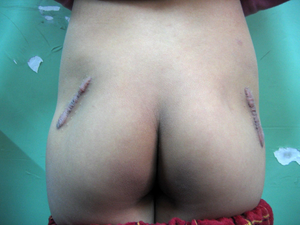
The release done through a lateral skin incision in the lower part of the line between greater trochanter and posterior superior iliac spine. This surgical approach has excellent results for level I injury, for level II the adduction angle improved> 45°, and 60° for level III[4].
However, on medium- term follow up arthroscopic release of GMC has a quick recovery and high success rate after surgery in adult[12], conventional open surgery and arthroscopic are both effective surgical interventions for GF[13].
Non- surgical management[edit | edit source]
It is the option of choice for children or who wait for surgery, used mainly for level I.
The program will include massage, a source for deep heat as shortwave diathermy, stretching exercise, gait training like walking straight in a line, and squatting or couching with both knees together[4].
Post- operative rehabilitation program
It is better to be done as early as possible for better outcomes, they can start the rehabilitation program 24-48h after operation. After elimination of pain we can start active or passive movement for hip and knee joint, walking, gait training, and progress to crunching with both closed knee, squatting, and sitting with crossed legs. At first the patient should be advised to lie side lying to allow provide support for wound compression, and if the contracture was on both sides, the patient will change position every11-2 hour for each side[2].
References[edit | edit source]
- ↑ Reilly AL, Owori FR, Obaikol R, Asige E, Aluka H, Penny N, Olupot R, Sabatini CS. Surgical release of gluteal fibrosis in children results in sustained benefit at 5-year follow-up. Journal of Pediatric Orthopaedics. 2021 Mar 11;41(3):e240-5.
- ↑ 2.0 2.1 2.2 2.3 2.4 Rai S, Meng C, Wang X, Chaudhary N, Jin S, Yang S, Wang H. Gluteal muscle contracture: diagnosis and management options. SICOT-J. 2017;3.
- ↑ Lixihua L, Zhangqing Z, Shengpingquan S, Zhaolei Z, Zhaoli Z, Cuixuee C, Liuxiaoqin L. P1. 43 The clinical and pathological analysis of the uniform type l fiber myopathy with brain atrophy and gluteal muscle contractures. Neuromuscular Disorders. 2010 Oct 1;20(9):613.
- ↑ 4.0 4.1 4.2 Zhao CG, He XJ, Lu B, Li HP, Wang D, Zhu ZZ. Classification of gluteal muscle contracture in children and outcome of different treatments. BMC Musculoskeletal Disorders. 2009 Dec;10(1):1-7.
- ↑ 5.0 5.1 Alves K, Katz JN, Sabatini CS. Gluteal fibrosis and its surgical treatment. The Journal of Bone and Joint surgery. American Volume. 2019 Feb 20;101(4).
- ↑ Nikolaou S, Asige E, Francis O, Abaikol R. Gluteal fibrosis: A case series in eastern Uganda. Could our malarial treatment be causing long-term disability?. International Journal of Surgery. 2014 Nov 1;12:S64.
- ↑ Lewis CL. Extra-articular snapping hip: a literature review. Sports health. 2010 May;2(3):186-90.
- ↑ Chen CK, Yeh L, Chang WN, Pan HB, Yang CF. MRI diagnosis of contracture of the gluteus maximus muscle. American Journal of Roentgenology. 2006 Aug;187(2):W169-74.
- ↑ Ye B, Zhou P, Xia Y, Chen Y, Yu J, Xu S. New minimally invasive option for the treatment of gluteal muscle contracture. Orthopedics. 2012 Dec 1;35(12):e1692-8.
- ↑ Liu YJ, Wang Y, Xue J, Lui PP, Chan KM. Arthroscopic gluteal muscle contracture release with radiofrequency energy. Clinical orthopaedics and related research. 2009 Mar;467(3):799-804.
- ↑ Fu D, Yang S, Xiao B, Wang H, Meng C. Comparison of endoscopic surgery and open surgery for gluteal muscle contracture. Journal of Pediatric Orthopaedics. 2011 Jul 1;31(5):e38-43.
- ↑ Gao SG, Liu WJ, Yang M, Li JP, Su C, Kuang SD, Xiong JP, Chou K, He ZY, Li LJ. Clinical results of arthroscopic tight fibrous band release for adult moderate-to-severe gluteal fibrosis using anterior and posterior portals: a retrospective analysis of 118 consecutive cases. BMC Musculoskeletal Disorders. 2021 Dec;22(1):1-0.
- ↑ Rai S, Jin S, Meng C, Chaudhary N, Tamang N, Wang X, Liu X, Wang H, Yang S. Arthroscopic release using F and C method versus conventional open release method in the treatment of gluteal muscle contracture: a comparative study. BMC Musculoskeletal Disorders. 2017 Dec;18(1):1-0.