Fetal Alcohol Spectrum Disorder (FASD)
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kirenga Bamurange Liliane and Kim Jackson
Introduction[edit | edit source]
Fetal alcohol spectrum disorder (FASD) refers to a range of problems caused by exposure of a fetus to alcohol during pregnancy. FASD is the most common preventable cause of developmental disability.[1]
- FASD affects children and youth across all races, ethnicities, cultures and socioeconomic status.
- There is no cure for FASD and its effects last a lifetime. eg behavioural, intellectual, neurological and mental health difficulties.
- A person with FASD can get help with their learning and behaviour to maximise their independence and achievements.
- Not drinking alcohol during pregnancy is the safest option[2]. See also Preconceptual Care
What is FASD[edit | edit source]
Fetal alcohol spectrum disorder (FASD) refers to the range of problems caused by prenatal exposure to alcohol (exposure to alcohol during pregnancy).
If a woman drinks alcohol while she is pregnant, the alcohol crosses the placenta from her blood into the baby’s bloodstream and the baby is exposed to similar concentrations of alcohol as the mother. Babies severely affected by FASD are at risk of dying before they are born.[2]
The effects of alcohol on a fetus include:
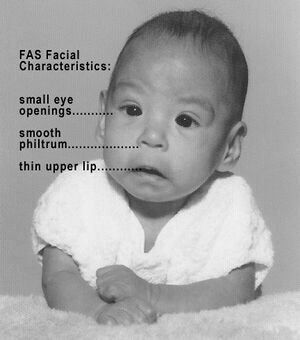
- Facial/oral: short palpebral fissures; mid facial hypoplasia; long thin upper lip
- Cranial/CN: microcephaly; intellectual impairment; corpus callosum agenesis/ dysgenesis; focal cortical thickening
- Skeletal: delayed bone development; pectus excavatum; vertebral segmental anomalies: congenital scoliosis; limb anomalies; fusion of upper limbs: radio-ulnar synostoses
- Cardiac: septal defects[3]
Not all babies exposed to alcohol develop FASD. The risk of harm to the fetus is highest when prenatal exposure to alcohol occurs regularly or due to frequent binge drinking.[2]
Epidemiology[edit | edit source]
Prenatal alcohol exposure is the leading cause of preventable congenital disabilities[3]. The estimated incidence in the western world is at around ~10% for FASD. It may affect up to 20-40% of pregnancies in mothers with chronic alcohol abuse.[4]
In many cases, prenatal alcohol exposure is unintentional because women continue their normal drinking patterns before they know they are pregnant. Most women stop drinking alcohol once made aware of their pregnancy. Despite this fact, 7.6% of women report continued drinking during pregnancy.[3]
Pathophysiology[edit | edit source]
The exact mechanism by which alcohol causes its teratogenic (causing congenital anomalies or birth defects) effects is not known. For obvious ethical reasons, formal studies on the effects of alcohol on human brain development are limited. Most of our data come from animal models and associations with alcohol exposure.
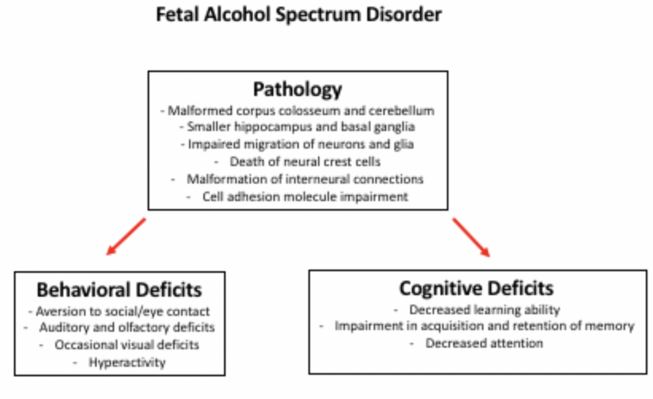
We do know that alcohol is a teratogen that causes irreversible damage to the central nervous system (CNS). From associations with alcohol exposure, we are aware that damage is widespread, causing not only a decrease in brain volume but also damage to structures within the brain.
We also know from associations that:
- High levels of alcohol consumption in the first trimester resulted in an increased likelihood of facial and brain anomalies.
- High levels of alcohol consumption in the second trimester are associated with increased incidences of spontaneous abortions.
- High levels of alcohol consumption in the third trimester are associated with decreased height, weight, and brain volume.
Associations with alcohol exposure show that the neurobehavioral deficits associated with fetal alcohol spectrum disorders can occur within a wide range of exposure to alcohol and at any point in the pregnancy[3].
Management[edit | edit source]
CNS damage from prenatal alcohol exposure is permanent, there is no cure for fetal alcohol spectrum disorders. However, treatment to mitigate the effects of fetal alcohol spectrum disorders is available. Given the extensive variation in presentation and damage that prenatal exposure to alcohol can cause, treatment for fetal alcohol spectrum disorders is often tailored and specific to individuals.
- One of the most common treatment approaches is using the medical home to coordinate developmental and educational resources.
- Treatment methodology seeks to tailor specific therapies to reinforce and address any delays or deficiencies with additional education, practice, and reminders[3].
Physiotherapy[edit | edit source]
Although there are many consequences of FASD, the focus for physical therapy is the neuromotor abnormalities associated with F AS, that may require consultation or intervention.
There are two elements in the management of FASD.
- An appropriate treatment program that addresses specific symptoms must/be designed.
- The treatment program and outcomes with respect to the child with FAS must be monitored carefully.
Treatment programs for children with FAS should address impairments with intellectual, behavior, and social functioning , as well as deficits[5]
Examples of treatments include:
- Working on achieving developmental milestones with these children. eg: work on rolling over, sitting balance, crawling, walking, climbing stairs, standing balance, coordination, or any other activity that they haven’t yet performed that is age-appropriate ; manual facilitation helping them practice those movements and learn how to move their body in new ways.
- Motor planning (older children), eg creating games to help them work on their balance and coordination, like creating obstacle courses, pretending that the floor is lava, and stepping on pillows to get across the room.
- Children with FASD tend to have difficulty filtering out all of the sensory input around them, like lights, noises, smells, and focusing on one task. Work on processing sensory information and perform task-focused activities.
- Aquatic therapy, teaching children how to swim and helping them exercise and improve their physical function in the water.[6]
See Motor Control and Learning
References[edit | edit source]
- ↑ The Conversation The truth about fetal alcohol spectrum disorder. Available from: https://theconversation.com/the-truth-about-fetal-alcohol-spectrum-disorder-103240 (Accessed, 16.10.2021)
- ↑ 2.0 2.1 2.2 Fetal alcohol spectrum disorder (FASD). Available from: https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/fetal-alcohol-spectrum-disorder-fasd#bhc-content (Accessed, 16.10.2021).
- ↑ 3.0 3.1 3.2 3.3 3.4 Vorgias D, Bernstein B. Fetal Alcohol Syndrome. StatPearls [Internet]. 2020 Aug 23.
- ↑ Fetal alcohol syndrome. Available from: https://radiopaedia.org/articles/fetal-alcohol-syndrome (Accessed, 16.10.2021).
- ↑ Emerson ML. Fetal alcohol syndrome: physical therapy implications and treatment strategies. Available from:https://commons.und.edu/pt-grad/128/ (Accessed, 16.10.2021).
- ↑ Physical Therapy Fetal Alcohol Spectrum Disorders: an Overview. Available from: https://katiegpt.com/blog/fetal-alcohol-spectrum-disorders (Accessed, 16.10.2021).