Essentials of Patient Safety in Physical Therapy Practice
Top Contributors - Sivapriya Ramakrishnan, Shaimaa Eldib and Kim Jackson
Introduction[edit | edit source]
Patient safety is defined as a commitment from the healthcare team member in providing the patient with safe techniques and procedures that reduces the risks and errors and maximize the recovery of the patient[1]. The WHO Global Safety Action Plan 2021-2030[2] emphasizes various action from the stakeholders to promote zero harm for the patients. The patient safety curriculum guide given by WHO- multidisciplinary edition does not provide information specifically from the perspectives of Physiotherapy practice[3]. Physiotherapists as a healthcare team member must be aware about patient safety protocols[4][5] and they must be trained in this area to improve their competencies[6] and hence the patient safety.[7]
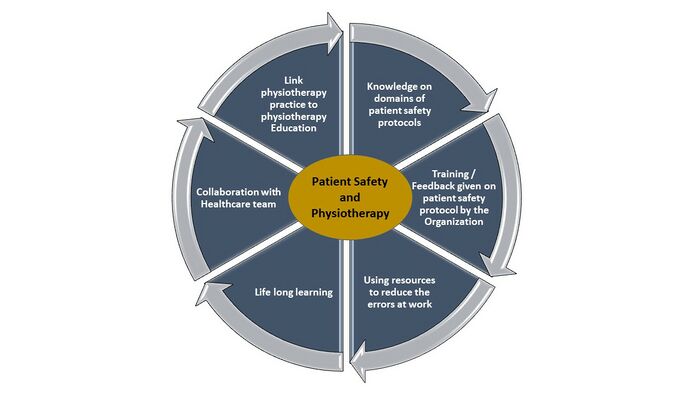
Domains of patient safety practices[edit | edit source]
- Knowledge about the adverse events and the system involved in patient safety[8]: The physical therapist must have knowledge on factors such as Infection control procedures [3], near misses, errors and risk mitigation strategies[9] and the patient safety assessment manual used at their place of work like hospitals[10] and primary care[11].
- Communication[12][13][14]: Communicating with the patient is one of the essential competencies across the globe. Communication with the patient, family members and team members will begin from informed consent[15], history taking[16], providing knowledge to the patient[17] about the condition and action taken plan, giving instructions while treatment, explaining the home exercise program to the patient and caregivers and it may extend up to negotiation of in terms of long-term care requirement for the patient. Collaboration with the team members[18][19].[20]
- Managing and acting at the moment[21]: According to Endsley's theory of situational awareness, the therapist must be aware of how to tackle the situation. It involves three phases perception, understanding and prediction.
- Perception[21]: The therapist is being aware of the situation around, which includes people, environment, modalities, team members action, patient details, medical records, family members etc.
- Understanding[21]: Once the stage of perception has completed, the therapist must now act in a way to integrate these details to practice and understand how one factor can affect all other factors[22].
- Prediction[21]: As the phase of perception and understanding shall pass, now the therapist must be in a scenario to anticipate that may happen and act ahead of time to create check list and incident management plan. Checklist[23] is considered as one of the important resources to be used in critical situations, to reduce human errors. Physical therapist in collaboration with the healthcare team members shall create a checklist to be used to address the patient safety concerns across different situations eg- safety considerations while transferring the patient, pulling up the bed rails after treatment to prevent patient falls, crutch height considerations to prevent axillary nerve injury etc. This can be utilized either in the form of physical checklist or using technology an automated one to be chosen according to the case. This requires meticulous practice and training with the organization considering the legislative and socio-cultural norms involved within.
- Information technology to reduce risks: Using information technology can enhance patient safety in physical therapy practice like, Electronic Medical Records (EMR), Electronic Physician's orders, Clinical Decision Support (CDS) tools, Asynchronous and Synchronous Telerehabilitation[24], Patient Handover[25].
- Being a life-long learner: Physical therapist must seek to enhance knowledge by participating in formal and informal opportunities of learning. Formal opportunities includes presenting their cases in the departmental meetings, participating in competency based continuous professional development[26] activities i.e pertaining to attend seminars, workshops and conferences that improve the knowledge, skills, approaches and attitude in their practice[27] and so does the patient centered care. Organizations/Institutions must take up some responsibilities in organizing professional development activities based on the needs analysis of the employees that will benefit both the parties[28].
- Collaborator[29]: Patient safety is shared amongst all healthcare professionals[30]. Decision making process involves clinical reasoning across the healthcare team to ensure patient safety is a priority[31][32].
Linking Physiotherapy practice to Physiotherapy Education[edit | edit source]
Patient safety can no longer be a part of the hidden curriculum, but it has to emphasized to embedded across the curriculum[33]. There is limited evidence to showcase the same and research are less in this area, which questions the actual implementation of the patient safety curriculum in physiotherapy education and the limited knowledge about patient safety for physiotherapists.[34] The patient safety framework provided by the Australian Patient Safety Education Framework (APSEF) and Canadian safety competency framework emphasizes various domains and in a programmatic method to be introduced in the curriculum [3]. Integrating the physiotherapy education[35] with practice with experiential learning strategies [36]on patient safety can promote the domains addressed[37][38].
Methods to inculcate Patient Safety in the physiotherapy education[edit | edit source]
Simulation- Simulated environment and standardized patient is one of the methods to expose the students in an unfamiliar environment, which let the students to gain confidence before approaching a real working situations[39].
Project Based Learning- Assigning the final year students to prepare the project considering the real-world working systems quality in mind to promote patient safety[40].
Interprofessional Problem Based Learning & Team Based Learning- Providing the students with the problem pertaining to the errors and risk mitigation and facilitate the process of learning through inquiry has an impact on the retention of the concept applied [41]and it is enhanced more if the students are working in groups of various health care professionals[42].
References[edit | edit source]
- ↑ Henriksen K, Battles JB, Keyes MA, Grady ML. Advances in patient safety: new directions and alternative approaches. AHRQ Publication. 2008 Aug(08-0034).[1]
- ↑ World Health Organization. Global patient safety action plan 2021–2030: towards eliminating avoidable harm in health care.
- ↑ 3.0 3.1 3.2 Safety WP, World Health Organization. Patient safety curriculum guide: multi-professional edition.[2]
- ↑ Scheirton LS, Mu K, Lohman H, Cochran TM. Error and patient safety: ethical analysis of cases in occupational and physical therapy practice. Medicine, Health Care and Philosophy. 2007 Sep;10(3):301-11.
- ↑ HaCP C. Standards of proficiency for physiotherapists. NHS, editor. 2013:20.
- ↑ Pearson P, Steven A, Dawson P. Patient safety in health care professional educational curricula: examining the learning experience.
- ↑ Gonzalez-Caminal, G. , Gomez, A. C. , Gomar-Sancho, C. . Patient Safety in Physiotherapy: Are Errors that Cause or Could Cause Harm Preventable?. In: Salen, P. , Stawicki, S. P. , editors. Contemporary Topics in Patient Safety - Volume 2 [Working Title] [Internet]. London: IntechOpen; 2022 [cited 2022 Nov 27]. Available from: https://www.intechopen.com/online-first/83873 doi: 10.5772/intechopen.107847
- ↑ Lawati MH, Dennis S, Short SD, Abdulhadi NN. Patient safety and safety culture in primary health care: a systematic review. BMC family practice. 2018 Dec;19(1):1-2.
- ↑ Hughes R, editor. Patient safety and quality: An evidence-based handbook for nurses.
- ↑ World Health Organization. Patient safety assessment manual.
- ↑ World Health Organization. Patient safety assessment manual for primary care.
- ↑ Hiller A, Delany C. Communication in physiotherapy: Challenging established theoretical approaches. Manipulating practices: A critical physiotherapy reader. 2018:308-33.
- ↑ World Confederation of Physical Therapy, European Region. Euro-pean physiotherapy benchmark statement. Barcelona: WCPT; 2003. Available at: http://www.physio-europe.org/pdf/Benchmark.pdf (last accessed 11/09/2008)
- ↑ King J, Anderson CM. Patient safety and physiotherapy: what does it mean for your clinical practice?. Physiotherapy Canada. 2010 Jul;62(3):172-5.
- ↑ Copnell G. Informed consent in physiotherapy practice: it is not what is said but how it is said. Physiotherapy. 2018 Mar 1;104(1):67-71.
- ↑ Ladyshewsky R, Baker R, Jones M, Nelson L. Reliability and validity of an extended simulated patient case: a tool for evaluation and research in physiotherapy. Physiotherapy Theory and Practice. 2000 Jan 1;16(1):15-25.
- ↑ Worum H, Lillekroken D, Ahlsen B, Roaldsen KS, Bergland A. Bridging the gap between research-based knowledge and clinical practice: a qualitative examination of patients and physiotherapists’ views on the Otago exercise Programme. BMC geriatrics. 2019 Dec;19(1):1-8.
- ↑ Ajjawi R. Learning to communicate clinical reasoning in physiotherapy practice.
- ↑ Aggarwal D, Ploderer B, Vetere F, Bradford M, Hoang T. Doctor, can you see my squats? Understanding bodily communication in video consultations for physiotherapy. InProceedings of the 2016 ACM conference on designing interactive systems 2016 Jun 4 (pp. 1197-1208).
- ↑ Wloszczak-Szubzda A, Jarosz MJ. Professional communication competences of physiotherapists–practice and educational perspectives. Annals of Agricultural and Environmental Medicine. 2013;20(1).
- ↑ 21.0 21.1 21.2 21.3 Endsley MR, Garland DJ, editors. Situation awareness analysis and measurement. CRC Press; 2000 Jul 1.
- ↑ Hignett S, Lang A. Human factors for health & social care.
- ↑ Hales BM, Pronovost PJ. The checklist—a tool for error management and performance improvement. Journal of critical care. 2006 Sep 1;21(3):231-5.
- ↑ Alotaibi YK, Federico F. The impact of health information technology on patient safety. Saudi medical journal. 2017 Dec;38(12):1173.
- ↑ Lau PM, DHSca RM, DHScb AC, DHScc MW. Clinical handover in physiotherapy enhanced safety and continuity of patient care for transfer from acute to rehabilitation hospitals. Hong Kong Physiotherapy Journal. 2015 Dec 1;2(33):101.
- ↑ Campbell C, Silver I, Sherbino J, Cate OT, Holmboe ES, International CBME Collaborators. Competency-based continuing professional development. Medical teacher. 2010 Aug 1;32(8):657-62.
- ↑ Schostak J, Davis M, Hanson J, Schostak J, Brown T, Driscoll P, Starke I, Jenkins N. ‘Effectiveness of continuing professional development’project: a summary of findings. Medical teacher. 2010 Jul 1;32(7):586-92.
- ↑ Alsiö Å, Pettersson A, Silén C. Health Care Leaders' Perspectives on How Continuous Professional Development Can Be Promoted in a Hospital Organization. Journal of Continuing Education in the Health Professions. 2022 Jul 1;42(3):159-63.
- ↑ Fewster-Thuente L, Velsor-Friedrich B. Interdisciplinary collaboration for healthcare professionals. Nursing administration quarterly. 2008 Jan 1;32(1):40-8.
- ↑ Ballard KA. Patient safety: A shared responsibility. Online Journal of issues in nursing. 2003 Sep 30;8(3):4.
- ↑ Trede F, Higgs J. Collaborative decision making. Clinical reasoning in the health professions. 2008 Feb 14:43-54.
- ↑ Jones MA, Jensen G, Edwards I. Clinical reasoning in physiotherapy. Clinical reasoning in the health professions. 2008 Feb 14:245-56.
- ↑ Cresswell K, Howe A, Steven A, Smith P, Ashcroft D, Fairhurst K, Bradley F, Magnusson C, McArthur M, Pearson P, Sheikh A. Patient safety in healthcare preregistration educational curricula: multiple case study-based investigations of eight medicine, nursing, pharmacy and physiotherapy university courses. BMJ Quality & Safety. 2013 Oct 1;22(10):843-54.
- ↑ Howarth SD, Fielden SA, O’Hara JK. How do we educate medical students interprofessionally about patient safety? A scoping review. Journal of Interprofessional Care. 2022 Mar 4;36(2):259-67.
- ↑ Martensen A, Grønholdt L. Quality in higher education: linking graduates' competencies and employers' needs. International Journal of Quality and Service Sciences. 2009 Mar 20.
- ↑ Tolsgaard MG, Kulasegaram KM, Ringsted C. Practical trials in medical education: linking theory, practice and decision making. Medical Education. 2017 Jan;51(1):22-30.
- ↑ Milligan FJ. Establishing a culture for patient safety–The role of education. Nurse education today. 2007 Feb 1;27(2):95-102.
- ↑ Ebright P, Kooken W, Moody R, Al-Ishaq MA. Mindful attention to complexity: Implications for teaching and learning patient safety in nursing. New York, NY: Springer Publishing Company; 2006.
- ↑ Phillips AC, Mackintosh SF, Bell A, Johnston KN. Developing physiotherapy student safety skills in readiness for clinical placement using standardised patients compared with peer-role play: a pilot non-randomised controlled trial. BMC medical education. 2017 Dec;17(1):1-0.
- ↑ Gleason KT, VanGraafeiland B, Commodore-Mensah Y, Walrath J, Immelt S, Ray E, Dennison Himmelfarb CR. The impact of an innovative curriculum to introduce patient safety and quality improvement content. BMC medical education. 2019 Dec;19(1):1-8.
- ↑ Madigosky WS, Headrick LA, Nelson K, Cox KR, Anderson T. Changing and sustaining medical students' knowledge, skills, and attitudes about patient safety and medical fallibility. Academic Medicine. 2006 Jan 1;81(1):94-101.
- ↑ Leotsakos A, Ardolino A, Cheung R, Zheng H, Barraclough B, Walton M. Educating future leaders in patient safety. Journal of multidisciplinary healthcare. 2014;7:381.