Cold-Related Injuries
Original Editor - Puja Gaikwad
Top Contributors - Puja Gaikwad, Kim Jackson, Reem Ramadan, Vidya Acharya and Wanda van Niekerk
Introduction[edit | edit source]
Cold injuries are a result of exposure to cold environments during physical activity. Many athletes participate in fitness pursuits and physical activity year-round in environments with cold, wet, or windy conditions or a combination of these, thereby putting themselves in danger of cold-related injuries. Cold exposure can be uncomfortable, it can impair performance and it can be life-threatening.[1] Cold injuries and illnesses usually affect military personnel, traditional winter-sport athletes, and outdoor-sport athletes, like those involved in running, cycling, mountaineering, and swimming etc.[2][3] Traditional team sports like football, baseball, softball, soccer, lacrosse, and track and field have seasons that stretch into late fall or early winter or begin in early spring when weather conditions may rise vulnerability to cold injuries.[4]
The NATA position statement states that the occurrence of these injuries depends on low air or water temperatures (or both) and the influence of wind on the body's ability to take care of a normothermic core temperature, due to localized exposure of the extremities to cold air or surfaces.[5]
Alpine Environments[edit | edit source]
Cold conditions are often expected in alpine environments. Furthermore, open exposed areas, like mountain peaks, mean that windy conditions are also commonplace in these environments and may contribute significantly to cold temperatures (also referred to as the 'wind chill factor').[6] The collective effect of those conditions is heat loss, which places extra demands on the body. For instance, a decrease in core body temperature of just 1°C causes the muscles to shiver, which in turn can lead to low blood glucose levels (hypoglycaemia) and thereby reduced sporting performance.[4]
Types[edit | edit source]
Cold injuries are classified into three broad categories:
- Decreased core temperature (Hypothermia)
- Freezing-tissue injuries of the extremities
- Non-freezing injuries of the extremities[4]
Hypothermia[edit | edit source]
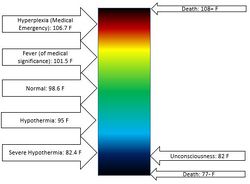
Hypothermia is a significant drop in body temperature [below 95°F (35°C)] as the body’s heat loss exceeds its production. thereby the body is not able to maintain a normal core body temperature. This can occur quickly within a couple of hours or gradually over days and weeks. Conditions which will cause hypothermia are cold temperatures, insufficient clothing and equipment, wetness, poor nutrition, duration of the event and exposed/uncovered skin.
Wind-Chill temperature index (WCT) demonstrates how cold an individual feels when exposed to a combination of cold air and wind. This index is a very useful and necessary tool to monitor the conditions individuals are exposed to during events held in colder weather calculated through a formula, but multiple graphs and apps are available for quick reference. As the Wind-Chill Equivalent Index (WCEI) indicates, wind speed interacts with ambient temperature to significantly increase body cooling. If the body and clothing are wet because of sweat, rain, snow or immersion, the cooling is even more pronounced due to evaporation of the water held close to the skin by wet clothing.[4][6]
The signs and symptoms of hypothermia can vary with each individual, depending upon previous cold weather injury (CWI), race, geological origin, ambient temperature, medications, clothing, fatigue, hydration, age, activity levels and others. Hypothermia is typically classified as mild, moderate, or severe, depending upon measured core temperature. Initially, the athlete may feel cold, begin to shiver and be not able to perform motor function leading to impaired athletic and mental performance. Early recognition of these symptoms is key to preventing more severe hypothermia. If early symptoms of hypothermia are not recognized or treated, the core body temperature will continue to decrease.[4][7]
Freezing Injuries of the Extremities[edit | edit source]
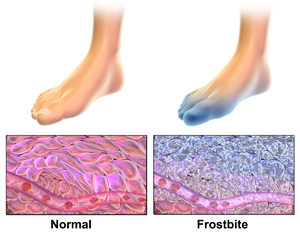
In conditions of prolonged cold exposure, the body sends signals to the blood vessels of hands and feet to constrict so as to preserve blood flow to vital organs. This helps the body by preventing a further drop in internal body temperature by exposing less blood to the outside cold. As this happens, toes and fingers become colder and colder eventually resulting in the injury of the involved tissues. Damage to the frostbitten tissue happens due to electrolyte concentration changes within the cells, leading to water crystallization within the tissue. For cells to freeze, the tissue temperature must be below 28°F (−2°C). The severity of frostbite is directly associated with the time of exposure and is divided into three degrees based on the depth of the injured tissue.[4]
Frostnip[edit | edit source]
Frostnip is the stage before frostbite and occurs when the superficial skin cools below 50°F (10°C). The skin becomes cold and red, and individuals feel a tingling painful sensation. It usually occurs in the nose, ears, cheeks, fingers, and toes and does not cause long term damage.[1]
Mild/superficial frostbite[edit | edit source]
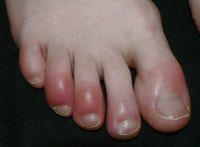
This occurs when skin temperature drops below 28°F (-2°C) and superficial tissues freeze. Initially, skin appears reddened and then turns white or pale. Individuals can experience stinging, burning, and swelling at the site of injury. A fluid-filled blister can be seen 12 to 36 hours after rewarming.[8][9]
Deep/severe frostbite[edit | edit source]
It occurs when deep layers of skin are affected. Skin looks white or blueish-grey and individuals experience numbness. Large blisters can develop 24-48 hours after rewarming. Later the injured area will turn black and hard as tissue dies. Medical attention for frostbite is needed when there are signs and symptoms of superficial or deep frostbite.[1]
In mountaineers, reported rates of hypothermia and frostbite include 3% to 5% respectively of all injuries and 20% of all injuries in Nordic skiers. Cold injury frequency in military personnel is reported to range from 0.2 to 366 per 1000 exposures.[8][10]
Non-freezing Injuries of the Extremities[edit | edit source]
Chilblain[edit | edit source]
Chilblain a nonfreezing cold injury also referred to as pernio, is an injury associated with extended exposure (1–5 hours) to cold, wet conditions. Chilblain severity is time and temperature related. The higher the temperature of the water (generally ranging from 32°F [0°C] to 60°F [16°C]), the longer the duration of exposure required to develop chilblain.[11] Exposure time is usually measured in hours or even days, rather than the minutes or hours associated with frostbite. It is an exaggerated or uncharacteristic inflammatory response to cold exposure. Prolonged constriction of the skin blood vessels leads to hypoxemia and vessel wall inflammation; oedema in the dermis can also be present. It may occur with or without freezing of the tissue. The hands and feet are most commonly affected sites, but chilblain of the thighs has also been reported. Situations during which this will happen include alpine sports, mountaineering, hiking, endurance sports, and team sports in which footwear and clothing remain wet for prolonged periods due to water exposure or sweating.[12][13][14]
Immersion (Trench) Foot[edit | edit source]
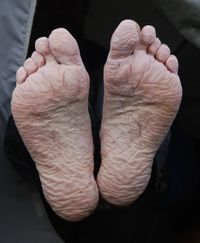
Immersion foot typically occurs with prolonged exposure (12 hours to 4 days) to a cold environment, wet conditions, usually in temperatures ranging from 32°F to 65°F (0°C–18°C). It usually affects primarily the soft tissues, including nerves and blood vessels, due to an inflammatory response leads to high levels of extracellular fluid. The foremost common mechanism for developing trench foot is the continued wearing of wet socks or footwear (or both).[13][15]
Signs and Symptoms[edit | edit source]
| Conditions | Signs and Symptoms |
| Hyperthermia
Mild |
Core temperature 98.6°F to 95°F (37°C -35°C)
Amnesia, Lethargy Vigorous shivering Impaired fine motor control Cold extremities Polyuria Typically conscious Blood temperature within normal limits |
| Moderate | Core temperature 94°F to 90°F (34°C -32°C)
Depressed respiration and pulse Cardiac arrhythmias Cyanosis Cessation of shivering Impaired mental function Slurred speech Impaired gross motor control Loss of consciousness Muscle rigidity Dilated pupils Blood pressure decreased or difficult to measure |
| Severe | Core temperature below 90°F (32°C)
Rigidity Bradycardia Severely depressed respiration Hypotension, pulmonary oedema Spontaneous ventricular fibrillation or cardiac arrest Usually comatose |
| Frostbite
Mild/superficial |
Dry, waxy skin
Erythema Oedema Transient tingling or burning sensation The skin contains white or blue grey-coloured patches Affected skin feels cold and firm to touch Limited movements of the affected area |
| Deep | Skin is hard and cold
The skin may be waxy and immobile Skin colour is white, grey, black or purple Vesicles present Burning aching, throbbing, or shooting pain Poor circulation in the affected area Progressive tissue necrosis Neurapraxia Hemorrhagic blistering develops within 36 to 72 hours Muscle, peripheral nerve, and joint damage likely |
| Chilblain/Pernio | Red or cyanotic lesions
Swelling Increased temperature Tenderness Itching, numbness, burning or tingling Skin necrosis Skin sloughing |
| Immersion (trench) foot | Burning, tingling or itching
Loss of sensation Cyanotic or blotchy skin Swelling Pain/ sensitivity Blisters Skin fissures or maceration |
Risk Factors[edit | edit source]
The risk of cold injuries increases when the blood flow is impeded when food intake is inadequate, or when insufficient oxygen is available, as occurs at high altitudes. It is divided into two categories as follows:
- Non-environmental: Athletes are often predisposed to cold-weather injuries before going outside. Risk factors for increased susceptibility to cold-weather injuries include Nutrition and hydration, age, medications, body size and composition, fitness level, and clothing. Certain medical conditions can predispose athletes to cold injuries, including Exercise-Induced Bronchospasm (EIB), Raynaud syndrome and cardiovascular disease.[4][16]
- Environmental: Environmental conditions like cold temperatures and weather conditions may put added stress on the body. Before training or competing outside, review various environmental conditions such as air temperature, humidity, rain, snow and wind to determine if it is safe for athletes.[16]
Management[edit | edit source]
Hypothermia (Mild)[edit | edit source]
- Identify the signs and symptoms of hypothermia, which include vigorous shivering, increased blood pressure, rectal temperature < 98.6°F (37°C) but > 95°F (35°C), fine motor skill impairment, lethargy, apathy, and mild amnesia.
- The rectal temperature obtained using a thermometer (digital or mercury) which will read below 94°F (34°C) is the preferred method for assessing core temperature in an individual suspected of being hypothermic.
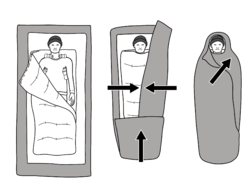
- Begin by removing wet or damp clothing; insulating the athlete with warm, dry clothing or blankets (including covering the head); and moving the athlete to a warm environment with shelter from the wind and rain.
- When rewarming, apply heat only to the trunk and other areas of heat transfer, including the axilla, chest wall, and groin. Rewarming the limbs can produce after drop, which is caused by dilation of peripheral vessels in the arms and legs when warmed, this dilation sends cold blood, often with a high level of acidity and metabolic byproducts, from the periphery to the core. This blood cools the core, resulting in a drop in core temperature, and can lead to cardiac arrhythmias or even death.
- Provide warm, nonalcoholic fluids and foods containing 6% to 8% carbohydrates to help sustain shivering and maintain metabolic heat production.[18][19]
Hypothermia (Moderate/Severe)[edit | edit source]
- Identify the signs and symptoms of moderate and severe hypothermia, which can include cessation of shivering, very cold skin on palpation, depressed vital signs, rectal temperature between 90°F (32°C) and 95°F (35°C) for moderate hypothermia or below 90°F (32°C) for severe hypothermia, impaired mental function, slurred speech, loss of consciousness, and gross motor skill impairment.
- If an athlete with suspected hypothermia having signs of cardiac arrhythmia, they should be moved very gently to prevent paroxysmal ventricular fibrillation.
- Begin with a primary evaluation to determine the need for cardiopulmonary resuscitation (CPR) and activation of the EMS. Remove wet or damp clothing; insulate an individual with warm, dry clothing or blankets covering the head and move them to a warm environment with shelter from the wind and rain.
- immediately initiate rewarming strategies and continue rewarming during transport and at the hospital. During the treatment and/or transport, continually examine vital signs and be prepared for airway management. When rewarming, provide heat only to the trunk and other areas of heat transfer, including the axilla, chest wall, and groin along with more aggressive rewarming procedures, including inhalation rewarming, heated intravenous fluids, peritoneal lavage, blood rewarming, and use of antiarrhythmic drugs.
- When immediate management is complete, keep a check on post-rewarming complications, including infection and renal failure.[1][20]
Frostbite (Superficial)[edit | edit source]
- Recognise the signs and symptoms of superficial frostbite, which include oedema, redness or mottled grey skin appearance, stiffness, and transient tingling or burning.
- Rule out the presence of hypothermia by evaluating observable signs and symptoms and measuring core body temperature.
- The choice to rewarm an athlete is contingent upon resources available and therefore the likelihood of refreezing. Rewarming can occur at room temperature or by placing the affected tissue against another individual's warm skin. Rewarming should be performed slowly, and water temperatures > 98°F to 104°F (37°C–40°C) should be avoided. If rewarming is not undertaken, protect the affected area from additional damage and further tissue temperature decreases and consult with a medical professional or transport to a medical facility.
- Avoid applying transverse friction to tissues and leave any vesicles (fluid-filled blisters) intact.
- Once rewarming has initiated, it is imperative that affected tissue not be allowed to refreeze, as it can result in tissue necrosis.[18][21][22]
Frostbite (Deep)[edit | edit source]
- Recognise the signs and symptoms of deep frostbite, which include oedema, mottled or grey skin appearance, the tissue that feels hard and does not rebound, vesicles, and numbness.
- Eliminate the presence of hypothermia by assessing observable signs and symptoms and measuring core temperature.
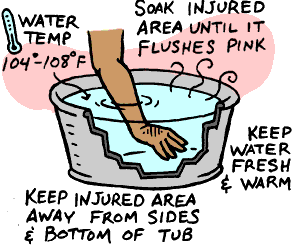
- To rewarm, the affected part should be immersed in a warm (98°F–104°F [37°C–40°C]) water bath. Water temperature should be monitored and maintained. Remove any constrictive clothing and submerge the whole affected area. The water will need to be gently circulated, and therefore the area should be immersed for 15 to 30 minutes. Thawing is complete when the tissue is pliable and colour and sensation have returned back to normal. Rewarming may result in significant pain, so a medical professional may prescribe appropriate analgesic medication.
- Not to use dry heat or steam to rewarm affected tissue also, avoid friction massage or vigorous rubbing to the affected tissues and leave any vesicles or fluid-filled blisters intact. If the vesicles rupture, they must be treated to stop the infection.
- Tissue plasminogen activators (tPA) may be administered to enhance tissue perfusion. These agents have been shown to limit the necessity for subsequent amputation due to tissue death.
- Once rewarming has started, it is imperative that the affected tissue not be allowed to refreeze, as tissue necrosis can result. Also, weight-bearing should be avoided when feet are involved. If the likelihood of refreezing exists, rewarming should be delayed until advanced medical aid is often obtained.
- If tissue necrosis occurs and tissue sloughs off, debridement and infection control measures are necessary.[19][21][22]
Chilblain[edit | edit source]
- Identify the signs and symptoms which include exposure to cold, wet conditions for > 60 minutes at temperatures < 50°F (16°C) and therefore the presence of small erythematous papules, with oedema, tenderness, itching, and pain. Upon rewarming, the skin can exhibit inflammation, redness, swelling, itching, or burning and increased temperature.[23]
- Remove wet or constrictive clothing, wash and dry the area gently, elevate the affected part and cover with warm, loose, dry clothing or blankets.
- Do not disturb blisters, apply friction massage, apply creams or lotions, use high levels of heat, or allow weight bearing on the affected area.
- During treatment, continually examine the affected part for the return of circulation and sensation.[11][12]
Immersion Foot[edit | edit source]
- Early detection of the signs and symptoms which include exposure to cold, wet environments for 12 hours to 3 or 4 days, burning, tingling or itching, loss of sensation, cyanotic or blotchy skin, swelling, pain or sensitivity, blisters, and skin fissures or maceration.[24]
- For treatment, thoroughly clean and dry the feet, then treat the affected part by applying warm packs or soaking in warm water (102°F–110°F [39°C–43°C]) for approximately 5 minutes. Replace wet socks with a clean, dry pair, and rotate footwear or allow footwear to dry before reusing.
- Use a risk management process that involves strategies for preventing, recognizing, and treating cold injuries during events. These strategies can then be used for preparing and devising risk management protocols and plans when cold injuries could also be a possibility.[1][25]
Prevention Strategies[edit | edit source]
Many cold-related injuries are often prevented with planning, adequate preparation and using proper equipment. These strategies have been discussed below.
- Education: Educating athletes about prevention is the key to reducing the possibility of cold exposure injury or illness. Prior to the sports season, individuals should be educated on prevention, risks related to the cold-environment activity, and early recognition and treatment of the cold injury. The sports medical staff and coaches should recognise individuals with conditions that can place members of their teams at greater risk (e.g., predisposing medical conditions, physiological factors, mechanical factors, environmental conditions etc.)[1]
- Hydration: Athletes are more susceptible to dehydration in cold-weather sports as the thirst reflex and desire to drink liquids could also be lowered even though the hydration needs remain the same as training in optimal temperatures. Pre-practice or post-practice hydration is essential and should focus more on carbohydrate-based snacks. Depending on the outdoor winter activity, warm liquids served during a short break may help rewarm the body from the inside out.[26]
- Nutrition: Proper nutrition is equally important in cold-weather activities as training in cold-weather environments place an added stress on the body. Encouraging proper nutrition is vital to maintaining optimal performance in cold-weather sports. Exposure to cold and shivering during activity is fueled mostly by glycogen. This results in additional carbohydrate and caloric demands for athletes.[27]
- Clothing: Wearing sufficient layers of clothing around the body core are one of the most important considerations for preventing cold-related injuries and it should not be overlooked. Individuals should be advised to dress in layers and try to stay dry. Moisture, whether from perspiration or precipitation, remarkably increases body heat loss. Layers could be added or removed depending on temperature, activity levels and wind chill.
- Energy: Maintain energy levels via the use of meals, energy snacks and carbohydrate/electrolyte sports drinks. as negative energy balance increases the susceptibility to hypothermia.
- Warm-Up: Warm-up thoroughly and keep warm throughout the practice or competition to minimise a decrease in muscle or body temperature. Time the warm-up to lead almost immediately to the competition. After the competition, add clothing to avoid rapid cooling.[3][5][18]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Long III WB, Edlich R, Winters KL, Britt LD. Cold injuries. Journal of long-term effects of medical implants. 2005;15(1).
- ↑ Candler WH, Ivey H. Cold weather injuries among US soldiers in Alaska: a five-year review. Military medicine. 1997 Dec 1;162(12):788-91.
- ↑ 3.0 3.1 Castellani JW. Running in Cold Weather: Exercise Performance and Cold Injury Risk. Strength & Conditioning Journal. 2020 Feb 1;42(1):83-9.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Nagpal BM, Sharma R. Cold injuries: The chill within. Medical Journal, Armed Forces India. 2004 Apr;60(2):165.
- ↑ 5.0 5.1 Cappaert TA, Stone JA, Castellani JW, Krause BA, Smith D, Stephens BA. National Athletic Trainers' Association position statement: environmental cold injuries. Journal of Athletic Training. 2008 Nov;43(6):640-58.
- ↑ 6.0 6.1 Osczevski R, Bluestein M. The new wind chill equivalent temperature chart. Bulletin of the American Meteorological Society. 2005 Oct;86(10):1453-8.
- ↑ Ulrich AS, Rathlev NK. Hypothermia and localized cold injuries. Emergency Medicine Clinics. 2004 May 1;22(2):281-98.
- ↑ 8.0 8.1 Kroeger, Janssen, Niebel. Frostbite in a mountaineer. Vasa. 2004 Aug 1;33(3):173-6.
- ↑ Nandini M. Frostbite: A Winter Disaster. Asian Journal of Nursing Education and Research. 2020 Jul;10(3):380-3.
- ↑ Imray C, Richards P, Greeves J, Castellani JW. Nonfreezing cold-induced injuries. BMJ Military Health. 2011 Mar 1;157(1):79-84.
- ↑ 11.0 11.1 AlMahameed A, Pinto DS. Pernio (chilblains). Current treatment options in cardiovascular medicine. 2008 Apr 1;10(2):128-35.
- ↑ 12.0 12.1 Koca T, Bağlan T, Saraç G, Arslan A. Cold Injury and Perniosis (Chilblain). Arşiv Kaynak Tarama Dergisi.;24(4):463-71.
- ↑ 13.0 13.1 Hamlet MP. Non-freezing cold injuries. Wilderness medicine. 1995 Aug 8:129-34.
- ↑ Longman DP, Brown EL, Imray CH. Nonfreezing cold injuries among long-distance polar rowers. Wilderness & Environmental Medicine. 2020 Apr 16.
- ↑ Golant A, Nord RM, Paksima N, Posner MA. Cold exposure injuries to the extremities. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 2008 Dec 1;16(12):704-15.
- ↑ 16.0 16.1 16.2 Ingram BJ, Raymond TJ. Recognition and treatment of freezing and nonfreezing cold injuries. Current Sports Medicine Reports. 2013 Mar 1;12(2):125-30.
- ↑ Norman JN. Environmental The Heat Physical and Cold Environment Medicine:—. Remote Medicine: A Textbook For Trainee And Established Remote Healthcare Practitioners. 2020 Jul 13.
- ↑ 18.0 18.1 18.2 Giesbrecht GG, Wilkerson JA. Hypothermia, Frostbite and other cold injuries: prevention, survival, rescue, and treatment. The Mountaineers Books; 2006.
- ↑ 19.0 19.1 Biem J, Koehncke N, Classen D, Dosman J. Out of the cold: management of hypothermia and frostbite. Cmaj. 2003 Feb 4;168(3):305-11.
- ↑ Aslam AF, Aslam AK, Vasavada BC, Khan IA. Hypothermia: evaluation, electrocardiographic manifestations, and management. The American journal of medicine. 2006 Apr 1;119(4):297-301.
- ↑ 21.0 21.1 Hallam MJ, Cubison T, Dheansa B, Imray C. Managing frostbite. Bmj. 2010 Nov 19;341.
- ↑ 22.0 22.1 Murphy JV, Banwell PE, Roberts AH, McGrouther DA. Frostbite: pathogenesis and treatment. Journal of Trauma and Acute Care Surgery. 2000 Jan 1;48(1):171.
- ↑ Rathjen NA, Shahbodaghi SD, Brown JA. Hypothermia and cold weather injuries. American family physician. 2019 Dec 1;100(11):680-6.
- ↑ Bush JS, Watson S. Trench Foot. InStatPearls [Internet] 2020 Feb 3. StatPearls Publishing.
- ↑ Hall A, Sexton J, Lynch B, Boecker F, Davis EP, Sturgill E, Steinmetz M, Shackelford S, Gurney J, Stockinger Z, King B. Frostbite and immersion foot care. Military medicine. 2018 Sep 1;183(suppl_2):168-71.
- ↑ Roberts DE, Hamlet MP. Prevention of cold injuries. Medical Aspects of Harsh Environments, Borden Institute, Washington. 2001:411-27.
- ↑ Seiffert R, Szymski D. Sports in Hot and Cold Environments. InInjury and Health Risk Management in Sports 2020 (pp. 413-415). Springer, Berlin, Heidelberg.