Anterior Interosseous Nerve
Introduction[edit | edit source]
The anterior interosseous nerve, also known as the volar interosseous nerve, is a motor branch that comes off of the median nerve in the proximal forearm. Anterior interosseous nerve syndrome, also known as anterior interosseous nerve compressive syndrome, refers to a motor neuropathy from compression of the anterior interosseous nerve. Compression can occur at various sites along the nerves course in the forearm , which is key to understanding the clinical implications [1].
Structure & Origin[edit | edit source]
The anterior interosseous nerve arises off the median nerve in the proximal forearm, approximately 5-8cm distal to the lateral epicondyle of the humerus. A 2018 cadaver study (n=50) summarized that the anterior interosseous nerve branched from the median nerve anywhere from 1.5 to 7.5 cm (mean = 5.2 cm) distal to the intercondylar line[2].
It is comprised of the C5-T1 spinal nerve roots.
Course[edit | edit source]
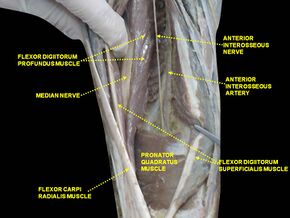
After branching off the median nerve in the proximal forearm, the anterior interosseous nerve courses distally between the two heads (superficial & deep) of the pronator teres muscle, deep to the flexor digitorum superficialis. It continues its descent along the anterior aspect of the interosseous membrane, between the flexor digitorum profundus and flexor pollicis longus muscles.
The anterior interosseous nerve passes deep to the pronator quadratus muscle, terminating close to the wrist joint[2].
Branches & Supply[edit | edit source]
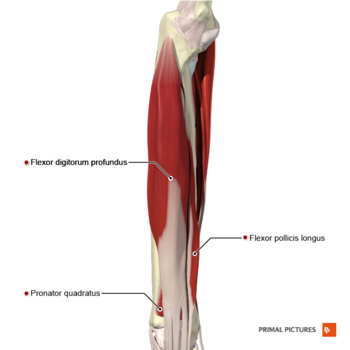
The anterior interosseous nerve provides motor innervation to the deep muscles in the anterior compartment of the forearm, including:
- Flexor pollicis longus
- Flexor digitorum profundus - lateral aspect only (the medial aspect of this muscle is supplied by the ulnar nerve)
- Pronator quadratus
The terminal branch of the anterior interosseous nerve travels through the posterior surface of the pronator quadratus, where it also provides sensory branches to the carpal bones of the wrist [2].
Relations[edit | edit source]
Initially, the anterior interosseous nerve sits parallel to the median nerve. As it travels into the distal forearm, it is positioned between two muscles: the flexor pollicis longus laterally and the flexor digitorum profundus medially. The anterior interosseous nerve continues to descend along the anterior aspect of the interosseous membrane where it is accompanied by the anterior interosseous artery and correlating veins [2].
Variants[edit | edit source]
Research suggests that the degree to which the median and ulnar nerves innervate the flexor digitorum muscle is variable[2].
Clinical Significance[edit | edit source]
Due to its deep location in the forearm, lesions to the anterior interosseous nerve are deemed rare however the overlying structures may cause compression in some cases[2].
The anterior interosseous nerve may be compressed by the following structures:
- Struthers ligament
- Bicipital aponeurosis
- Fibrous arch of the pronator teres muscles (between the superficial & deep heads)
- Fibrous arch at the origin of the flexor digitorum muscle
- Anamalous muscles. i.e., Gantzer muscle
The most common structural site of compression is anywhere from the origin of the deep head of the pronator teres muscle to the brachialis fascia. Conversely, compression from "fibrous bands from the superficial head of the pronator teres, bands from the superficialis arcade, the nerve running deep to both heads of the pronator and compression by a double lacterus fibrosus" are deemed to be less common causes[3].
Other causes of compression include the following:
- Trauma i.e., supracondylar humeral fracture, fracture of the forearm (proximal third)
- Vascular disease. i.,.e thrombosis, vessel hypertrophy
- Cysts
- Abscesses
- Hematomas
- Tumors
- Iatrogenic. i.e., forearm drug injections, fracture reduction
Anterior Interosseous Nerve Compressive Syndrome[edit | edit source]
This is a rare compressive neuropathy of the upper extremity that results in paralysis of the following: flexor digitorum profundus of the index finger, flexor pollicis longus as well the pronator quadratus[3]. This is characterized by the"inability to flex the distal interphalangeal joints of the thumb and index finger, causing an inability to make a pulp pinch, hyperextension of the distal interphalangeal joint, and flexion of the proximal interphalangeal joint; in the thumb, there is flexion of the metacarpophalangeal joint and hyperextension of the interphalangeal joint, which results in a contact area of the thumb pulp with the indicator much more proximal than normal"[2].
The pronator quadratus muscle can be tested by asking the patient to resist pronation of the forearm with the elbow in a fully flexed position in order to reduce activation of the pronator teres muscle [2].
Sensory examination of the hand & forearm will be unremarkable in anterior interosseous nerve compressive syndrome[2].
Incomplete anterior interosseous nerve syndrome refers to paresis or paralysis of the flexor pollicis longus or the flexor digitorum profundus of the index finger, resulting in compromised flexion of the distal phalanx of the thumb or index finger[2] [3]. Differential diagnoses of incomplete anterior interosseous nerve syndrome, related to the flexor tendon, include rupture, adherence or adhesion and stenosing tenosynovitis[3].
References[edit | edit source]
- ↑ Harris WH, Heaney RP. Skeletal renewal and metabolic bone disease. New England Journal of Medicine. 1969 Jan 23;280(4):193-202.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 2.9 Caetano EB, Vieira LA, Sabongi Neto JJ, Caetano MB, Sabongi RG. Anterior interosseous nerve: anatomical study and clinical implications. Revista brasileira de ortopedia. 2018 Oct;53(5):575-81.
- ↑ 3.0 3.1 3.2 3.3 Hill NA, Howard FM, Huffer BR. The incomplete anterior interosseous nerve syndrome. The Journal of hand surgery. 1985 Jan 1;10(1):4-16.