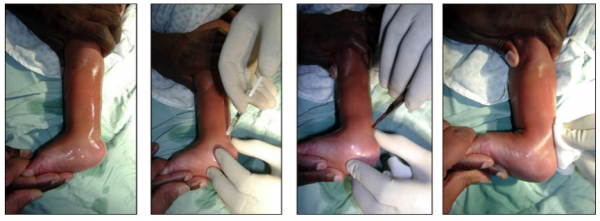
Achilles Tenotomy
Original Editor - Africa Clubfoot Training Team as part of ICRC and GCI Clubfoot Content Development Project
Top Contributors - Naomi O'Reilly, Daniele Barilla, Kim Jackson, Rucha Gadgil, Rachael Lowe, Simisola Ajeyalemi, Meaghan Rieke, Chelsea Mclene and Olajumoke Ogunleye
Introduction[edit | edit source]
Clubfoot is one of the commonest congenital deformities in children. More than 100,000 babies are born worldwide each year with congenital clubfoot. Around 80% of the cases occur in developing nations[1]. Ponseti method of serial manipulation and casting comes closest to of achieving the ultimate goal of treatment i.e. to achieve a functional, pain-free, plantigrade foot with good mobility and without calluses overcoming the issues of extensive scarring, residual pain and inadequate correction as seen with the other procedures such as bandages by Hippocrates and plaster casts by Kite and surgical treatment.[1]
After the final manipulation in management of clubfoot,there is some equinus deformity at ankle which persists. At this stage the total midfoot Pirani score is usually 0, the cavus, adductus, and varus are all corrected, the lateral head of talus is fully covered, and the foot is 50 - 70° abducted. In a few cases the equinus can be corrected by manipulation, but in 90% the Achilles Tendon is too tight and a tenotomy is needed. Over 90% of cases need a tenotomy[2]. Achilles Tenotomy is also called as percutaneous tenotomy, a tendo-Achilles lengthening tenotomy, or a heel cord lengthening/tenotomy.
The tenotomy corrects the rigid equinus. It is a complete cut through of the Achilles tendon, not a tendon lengthening. It creates a very small incision - it is known as a percutaneous (“through the skin”) tenotomy. It is necessary because although tissues yield to gentle stretch, collagen of the achilles tendon is more restrictive than the joint capsule and ligaments and does not respond to stretching as predictably. [2] In infants the tendon heals sufficiently in 3 weeks.
Remember: In most cases after the Ponsetti Method, tenotomy is still needed.
Indication for Tenotomy[edit | edit source]
Are the following all present?
- Talar Head Covered (Pirani Midfoot Score Usually = 0)
- Foot Abducts to 50 - 70 Degrees
- Heel in Valgus or at least Neutral
If yes, proceed to tenotomy.
If no, the foot may need more manipulation and casting.
In some rare cases when the above criteria are reached, the achilles tendon will not be tight, and if it allows Dorsiflexion to greater than 15° then tenotomy can be avoided.
Remember: Cover Talus before Tenotomy
Considerations[edit | edit source]
- Communicate with surgeon BEFORE tenotomy.
- Anticipate date through Pirani Scores, using graph if possible.
- Allow time for questions from parents.
- Decide on holding / casting roles.
- Measure the foot to organize a brace, which will be needed next visit.
- Paperwork and informed consent of parent or caregiver.
- Clinic environment: calm, quiet, baby feeding [2]
Equipment Required[edit | edit source]
Achilles tenotomy can be done in the Ponseti clinic under local anaesthetic, some teams opt to perform achilles tenotomy in theatre. The following equipment is required:
- Sterile Area, linen or paper sterile field
- Antiseptic
- Small Syringe with small gauge needle (25g or Smaller - An insulin syringe is perfect)
- Local anaesthesia Lignocaine 1 - 2% (inject 0.5–1ml)
- Gloves
- #15 Blade
- Sterile Gauze
- Timer to time 5 minutes (Pressure over Wound), or until Bleeding Stops
- The right size underwrap and padding need to be ready
- 2 Trained People: 1 to perform the tenotomy and 1 to Assist [2]
Procedure[edit | edit source]
This may be done in the clinic by an orthopaedic surgeon or an experienced and trained clinician. Two people are required, one person to hold the foot and one person to perform the tenotomy. The person holding the foot grips the leg below the knee and the midfoot, with the child’s knee in extension. A generous antiseptic prep of the heel and ankle is applied, extending medially and laterally. A small amount of local anaesthetic is placed medial to the achilles tendon 1cm proximal to its insertion. If too much anaesthetic is used the tendon is difficult to feel.
Insert the knife (a number 15 scalpel or beaver blade works well) on the medial side, parallel to and beneath (anterior to) the tendon approximately 1cm above its insertion into the calcaneum. Turn the sharp edge of the knife to the tendon and perform the tenotomy. The “release” obtained after a complete tenotomy is easily felt. Often there is a “pop” sound. 10 - 20 degrees of additional dorsiflexion will be obtained.
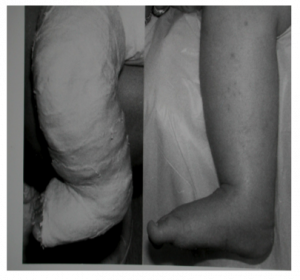
Clean skin with alcohol to remove the betadine. Place a sterile dressing over the wound. Apply firm pressure for 5 mins (or until bleeding stops) over the incision site. Apply the post-tenotomy cast: keep knee in 90 degrees flexion. Wrap with under-cast padding. Place a well-moulded above-knee plaster cast with the foot in maximum dorsiflexion (at least 15 degrees) and 50-70 degrees of abduction (with no eversion). This last cast should be worn for 3 weeks. The patient should remain in the department for 1 hour to check for bleeding and circulation.[2]
Effectiveness of Tenotomy[edit | edit source]
Some clinicians have expressed concerns about performing a complete tenotomy (completely severing) of the Achilles tendon, fearing this procedure will cause damage. However, an ultrasound study on children who had undergone Achilles tenotomy as part of their clubfoot treatment showed tendon re-growth; most tendons were clinically intact after 3 weeks and after 6 weeks all were intact.[3] Percutaneous tendo Achilles tenotomy is safe, inexpensive, effective, and an easy office procedure used to expedite the correction of equinus deformity in idiopathic clubfeet with a very low complication rate.[4]
Tenotomy in older children is a controversial area. A study of older children (7-11 years old) who had achilles tenotomies performed reported that none of the participants had weakness of the gastrocnemius or soleus muscles.[5] However, the maximum age when tenotomy can be used has not been established, it has been suggested that a lengthening procedure using three incisions could be used in place of complete tenotomy in older children.[5] This topic needs further investigation.
Errors During Tenotomy[edit | edit source]
Premature equinus correction - Attempts to correct the equinus before the heel varus and foot supination are corrected will result in a rocker-bottom deformity. Equinus through the subtalar joint can be corrected only if the calcaneus abducts. Tenotomy is indicated after cavus, adductus, and varus are fully corrected.
Failure to perform a complete tenotomy - The sudden lengthening with a “pop” or “snap” signals a complete tenotomy. Failure to achieve this may indicate an incomplete tenotomy. Repeat the tenotomy maneuver to ensure a complete tenotomy if there is no “pop” or “snap.” [6]
Management Post-Tenotomy[edit | edit source]
The cast after tenotomy stays on for 3 weeks. Prior to the tenotomy it is important to ensure to order the brace and book a the brace fitting. The foot must be in a dorsiflexed and abducted position to fit into brace. The last cast is applied with the foot in 50-70 degrees of abduction and at least 15 degrees of dorsiflexion. After removal of the last cast 3 weeks later there is correction of cavus, adductus, varus, and equinus (CAVE).
Post Casting, a foot abduction orthosis (FAO) brace, which consisted of a pair of straight high-top shoes and a connected bar, is prescribed to prevent the relapse of deformity.
Physiotherapy Post Tenotomy:[edit | edit source]
The goal should be to restore each child to their maximal functional ability[7].
- Range of Motion exercises :
- at proximal joints of hip and knee.
- gradual from passive to active at ankle -forefoot and midfoot (in consultation with the procedure performing surgeon)
- Weight bearing exercises:
- Focus on sensory input and feedback through feet, and provide child ability to maintain contact with surface with full plantar surface.
- Try to position child into neutral foot position prior to weight bearing.
- Strengthening: Start strengthening the proximal as well as distal muscles of the lower limbs.
- allow for play activities like kicking a ball.
- allow for play activities like kicking a ball.
- Tactile/ Proprioceptive re-education:
- Introduce different textured surfaces to child, placing under feet to allow child to feel and engage with them (soft blanket, rubber mat, dyna disc).
- Promote weight bearing with different surfaces underneath as well.
- Gait training.
- Counsel the parents regarding requirement of appropriate orthotics to maintain the correction.
References[edit | edit source]
- ↑ 1.0 1.1 Pulak S, Swamy M. Treatment of idiopathic clubfoot by ponseti technique of manipulation and serial plaster casting and its critical evaluation. Ethiop J Health Sci. 2012;22(2):77–84.
- ↑ 2.0 2.1 2.2 2.3 2.4 Africa Clubfoot Training Project. Chapter 7 Africa Clubfoot Training Basic & Advanced Clubfoot Treatment Provider Courses - Participant Manual. University of Oxford: Africa Clubfoot Training Project, 2017.
- ↑ Barker S, Lavy C (2006) Correlation of clinical and ultrasonographical findings after Achilles tenotomy in idiopathic club foot. The Journal of Bone and Joint Surgery 88-B (3): 377-379
- ↑ Riyaz Ahmad Dar, Mohd Shafi Bhat, Mohmad Yaseen Rather, Ansar ul Haq, Shera Ifran Ali. Percutaneous Tendo Achilles Tenotomy in the management of Equinus Deformity in conservatively treated CTEV. SEAJCRR 2015, JAN-FEB 4, 1
- ↑ 5.0 5.1 Khan S & Kumar A (2010) Ponseti’s manipulation in neglected clubfoot in children more than 7 years of age: a prospective evaluation of 25 feet with long term follow-up. Journal of Pediatric Orthopedics B 19: 385-389
- ↑ Lynn Staheli, Ignacio Ponseti, & Others. Clubfoot: Ponseti Management, 3rd Edition. Global Help, 2009. p13-15
- ↑ Ponseti I. Treatment of congenital clubfoot. J Bone Joint Surg Am 1992; 3: 448e54.