Paraneoplastic Syndrome: Difference between revisions
m (Text replace - '- Your name will be added here if you are a lead editor on this page.' to ' ') |
Rujuta Naik (talk | contribs) No edit summary |
||
| (33 intermediate revisions by 12 users not shown) | |||
| Line 1: | Line 1: | ||
<div class="editorbox"> | <div class="editorbox"> | ||
'''Original Editors '''- Brittany Chorley & Seth Chorley [[Pathophysiology of Complex Patient Problems|from Bellarmine University's Pathophysiology of Complex Patient Problems project.]] | '''Original Editors '''-[[User: Brittany Chorley|Brittany Chorley]] &[[User: Seth Chorley|Seth Chorley]][[Pathophysiology of Complex Patient Problems|from Bellarmine University's Pathophysiology of Complex Patient Problems project.]] | ||
''' | '''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} | ||
</div> | </div> | ||
== | == Introduction == | ||
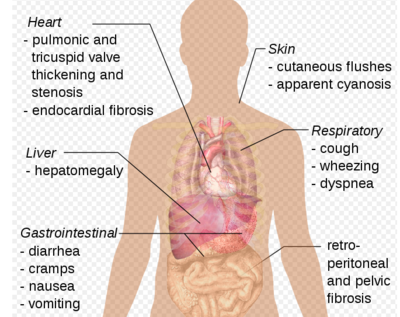
[[File:Paraneoplastic syndrome.png|400x400px|alt=|thumb|Paraneoplastic syndrome]] | |||
Paraneoplastic syndromes (PNS) occur due to the systemic effect of a malignancy and occur remotely to the primary malignancy. Symptoms are brought about by [[cytokines]], [[hormones]] or [[Immune System|immune]] cross-reactivity. These syndromes can cause a manifold of symptoms and can affect numerous systems.<ref name=":2">Radiopedia [https://radiopaedia.org/articles/paraneoplastic-syndromes Paraneoplastic syndromes] Available: https://radiopaedia.org/articles/paraneoplastic-syndromes<nowiki/>(accessed 24.1.2023)</ref> PNS can occur concurrently with tumour diagnosis before a tumour is diagnosed and even after tumours have been resected<ref name=":0">Henry K. [https://www.sciencedirect.com/science/article/abs/pii/S0740257019300097 Paraneoplastic syndromes: definitions, classification, pathophysiology and principles of treatment.] InSeminars in diagnostic pathology 2019 Jul 1 (Vol. 36, No. 4, pp. 204-210). WB Saunders.Available from:https://www.sciencedirect.com/science/article/abs/pii/S0740257019300097 (last accessed 15.7.2020)</ref>. The symptoms typically present in the middle-aged to [[Older People - An Introduction|older]] population. Also, it is common in individuals with [[Lung Cancer|lung]], [[Ovarian Cancer|ovarian]], [[Acute Lymphoblastic Leukemia|lymphatic]], or [[Breast Cancer|breast]] cancer. The most common cancer associated with paraneoplastic syndrome is small-cell cancer of the lungs. <ref name="p2">National Institute of Neurological Disorders and Stroke. NINDS Paraneoplastic Syndromes Information Page. http://www.ninds.nih.gov/disorders/paraneoplastic/paraneoplastic.htm. (accessed 18 March 2013).</ref> | |||
There is no cure for paraneoplastic syndromes and the treatment does not stop neurological damage.<ref name=":3">NIH [https://www.ninds.nih.gov/health-information/disorders/paraneoplastic-syndromes Paraneoplastic Syndrome]s Available:https://www.ninds.nih.gov/health-information/disorders/paraneoplastic-syndromes (accessed 24.1.2023)</ref> | |||
== Aetiology == | |||
PNS are largely due to two main causes: | |||
# Those due to tumour secretions of hormones, functionally active peptides, enzymes cytokines | |||
# Those due to tumours operating through auto-immune/immunological mechanisms with cross-reacting antibodies between neoplastic and normal tissues. Nb Remission of symptoms often follows resection of humoral secretory tumours but not always of tumours due to immunological mechanisms<ref name=":0" />. | |||
== | == Types of Paraneoplastic Syndrome == | ||
The Paraneoplastic Syndromes are classified based on the organ systems involved or on the etiological groups and are as follows<ref>Henry K. Paraneoplastic syndromes: Definitions, classification, pathophysiology and principles of treatment. InSeminars in diagnostic pathology 2019 Jul 1 (Vol. 36, No. 4, pp. 204-210). WB Saunders.</ref> : | |||
* Lambert-Eaton Myasthenic Syndrome | |||
* Stiff-Person Syndrome | |||
* Encephalomyelitis | |||
* Myasthenia Gravis | |||
* Cerebellar Degeneration | |||
* Limbic or Brainstem Encephalitis | |||
* Neuromyotonia | |||
* Opsoclonus | |||
* Sensory Neuropathy | |||
==Epidemiology == | |||
PNS occur in up to 15% of patients with cancer.<ref name=":2" /> Neurological manifestation in the form of neuropathies is common. Males and females are affected equally.<ref name=":1">Thapa B, Ramphul K. [https://www.ncbi.nlm.nih.gov/books/NBK507890/ Paraneoplastic syndromes.] InStatPearls [Internet] 2020 Jun 27. StatPearls Publishing.Available from:https://www.ncbi.nlm.nih.gov/books/NBK507890/ (last accessed 15.7.2020)</ref> | |||
== | ==<u></u>Clinical Presentation == | ||
PNS can affect multiple systems and have various presentations. Symptoms usually start before a tumour is found, slowly developing over a few days or weeks. Some of the more common symptoms include - Difficulty walking or swallowing; Loss of muscle tone; Loss of fine motor coordination; Slurred speech; Memory loss; Vision problems; Sleep disturbances; Dementia; Seizures; Sensory loss in the limbs; Vertigo or dizziness.<ref name=":3" /> | |||
Examples are given below based on the organ system involved. | |||
# Paraneoplastic neurological syndromes: [[encephalitis]] (paraneoplastic rhombencephalitis, [[Limbic System|limbic]] encephalitis); [[Lambert-Eaton Myasthenic Syndrome|Lambert-Eaton myasthenic syndrome]]; [[Optic Nerve|Optic]] neuropathy; [[Cerebellum|Cerebellar]] degeneration. | |||
#Endocrine eg [[Cushing's Syndrome|Cushing]] syndrome; Syndrome of inappropriate antidiuretic hormone secretion (SIADH); Hypercalcemia | |||
#Rheumatologica'''l''' eg Paraneoplastic polyarthritis; [[Polymyalgia Rheumatica|Polymyalgia rheumatica]]; Multicentric reticulohistiocytosis; Hypertrophic osteoarthropathy | |||
[[ | #Paraneoplastic haematologic syndromes: Good syndrome; Polycythaemia<ref name=":2" /> | ||
#Dermatological eg Acanthosis nigricans; Paraneoplastic pemphigus; Sweet syndrome; Leukocytoclastic vasculitis; [[Dermatomyositis]] | |||
#Renal eg Electrolyte imbalance ([[hypokalemia]], hypo or hypernatremia, hyperphosphatemia) causing nephropathy and acid-base disturbance due to ectopic hormones produced by tumour cells such as ACTH and ADH. Nephrotic syndrome can also be one of the manifestations of paraneoplastic syndrome. | |||
#Miscellaneous eg Fever, cachexia, [[Anorexia Nervosa|anorexia]], dysgeusia<ref name=":1" /><sup></sup><sup></sup><sup></sup> | |||
== Management == | |||
[[File:National-cancer-institute-0YBIMOqQzt0-unsplash.jpg|right|frameless]]Management of the patients is based on the type, severity, and location of the paraneoplastic syndrome. First, therapeutic options are to treat underlying malignancy with [[Chemotherapy Side Effects and Syndromes|chemotherapy]], [[Radiation Side Effects and Syndromes|radiation]], or surgery. | |||
* Other therapeutic options are immunosuppression with [[Corticosteroids in the Management of Rheumatoid Arthritis|corticosteroids]] or other immunosuppressive drugs, intravenous immunoglobulins, plasma exchange, or plasmapheresis. | |||
<sup>< | |||
| | |||
| | |||
[[ | |||
== Diagnostic Tests/Lab Tests/Lab Values == | == Diagnostic Tests/Lab Tests/Lab Values == | ||
First, a | First, a healthcare provider will perform a clinical exam that would include a general physical and neurological screening. | ||
# Neurological screening: reflexes, sensation, myotomes, balance, and coordination. | |||
# Laboratory tests that could be utilized to diagnose paraneoplastic syndrome include: [[Blood Tests|Blood tests]], Spinal tap | |||
# Imaging tests that could be utilized to diagnose paraneoplastic syndrome include: [[CT Scans|CT]] Scan; [[MRI Scans|MRI]]; PET Scan; and PET-CT, which may enhance the detection rate of small cancers | |||
= | If the physicians cannot find a malignant tumour, the syndrome may be the cause of a tumour that is too small to locate. In this instance, the physician will continue to have follow-up imaging conducted every three to six months for several years unless the cause is identified. <ref name="p1">Mayo Clinic. Paraneoplastic syndromes of the nervous system. http://www.mayoclinic.com/health/paraneoplastic-syndromes/DS00840. (accessed 18 March 2013).</ref> | ||
< | == Physical Therapy Management == | ||
People with paraneoplastic syndrome can have difficulty with walking, [[balance]], [[Coordination Exercises|coordination]], [[muscle]] tone, sensory of where the body is in space, and vertigo. | |||
* All of these symptoms the physical therapist can treat with traditional therapy. | |||
* Precautions must be taken into account for the cancer or neoplasm that is involved.<ref name="p2" /> | |||
== Conclusion == | |||
The diagnosis and management of paraneoplastic syndromes is difficult. | |||
* In most cases, there is an underlying malignancy responsible. | |||
* Due to the numerous causes, the condition is best managed by an interprofessional team (including a pathologist, oncologist, radiologist, haematologist, nurse specialist, and internist). | |||
* Once the cause is discovered, it needs to be treated. | |||
The management of the patients is based on the type, severity, and location of the paraneoplastic syndrome. | |||
* First, therapeutic options are to treat underlying malignancy with chemotherapy, radiation, or surgery. | |||
* Other therapeutic options are immunosuppression with corticosteroids or other immunosuppressive drugs, intravenous immunoglobulins, plasma exchange, or plasmapheresis.<ref name=":1" /><br> | |||
== References == | |||
<references /> | <references /> | ||
[[Category:Bellarmine_Student_Project]] | [[Category:Bellarmine_Student_Project]] | ||
[[Category:Primary Contact]] | |||
[[Category:Syndromes]] | |||
[[Category:Cardiopulmonary]] | |||
[[Category:Chronic Respiratory Disease - Conditions]] | |||
[[Category:Oncology]] | |||
Latest revision as of 16:08, 30 September 2023
Original Editors -Brittany Chorley &Seth Chorleyfrom Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Seth Chorley, Brittany Chorley, Lucinda hampton, Admin, Kim Jackson, Priya Gulla, Elaine Lonnemann, Rujuta Naik, WikiSysop, Claire Knott, 127.0.0.1, Vidya Acharya, Wendy Walker, Mariam Hashem and Adam Vallely Farrell
Introduction[edit | edit source]
Paraneoplastic syndromes (PNS) occur due to the systemic effect of a malignancy and occur remotely to the primary malignancy. Symptoms are brought about by cytokines, hormones or immune cross-reactivity. These syndromes can cause a manifold of symptoms and can affect numerous systems.[1] PNS can occur concurrently with tumour diagnosis before a tumour is diagnosed and even after tumours have been resected[2]. The symptoms typically present in the middle-aged to older population. Also, it is common in individuals with lung, ovarian, lymphatic, or breast cancer. The most common cancer associated with paraneoplastic syndrome is small-cell cancer of the lungs. [3]
There is no cure for paraneoplastic syndromes and the treatment does not stop neurological damage.[4]
Aetiology[edit | edit source]
PNS are largely due to two main causes:
- Those due to tumour secretions of hormones, functionally active peptides, enzymes cytokines
- Those due to tumours operating through auto-immune/immunological mechanisms with cross-reacting antibodies between neoplastic and normal tissues. Nb Remission of symptoms often follows resection of humoral secretory tumours but not always of tumours due to immunological mechanisms[2].
Types of Paraneoplastic Syndrome[edit | edit source]
The Paraneoplastic Syndromes are classified based on the organ systems involved or on the etiological groups and are as follows[5] :
- Lambert-Eaton Myasthenic Syndrome
- Stiff-Person Syndrome
- Encephalomyelitis
- Myasthenia Gravis
- Cerebellar Degeneration
- Limbic or Brainstem Encephalitis
- Neuromyotonia
- Opsoclonus
- Sensory Neuropathy
Epidemiology[edit | edit source]
PNS occur in up to 15% of patients with cancer.[1] Neurological manifestation in the form of neuropathies is common. Males and females are affected equally.[6]
Clinical Presentation[edit | edit source]
PNS can affect multiple systems and have various presentations. Symptoms usually start before a tumour is found, slowly developing over a few days or weeks. Some of the more common symptoms include - Difficulty walking or swallowing; Loss of muscle tone; Loss of fine motor coordination; Slurred speech; Memory loss; Vision problems; Sleep disturbances; Dementia; Seizures; Sensory loss in the limbs; Vertigo or dizziness.[4]
Examples are given below based on the organ system involved.
- Paraneoplastic neurological syndromes: encephalitis (paraneoplastic rhombencephalitis, limbic encephalitis); Lambert-Eaton myasthenic syndrome; Optic neuropathy; Cerebellar degeneration.
- Endocrine eg Cushing syndrome; Syndrome of inappropriate antidiuretic hormone secretion (SIADH); Hypercalcemia
- Rheumatological eg Paraneoplastic polyarthritis; Polymyalgia rheumatica; Multicentric reticulohistiocytosis; Hypertrophic osteoarthropathy
- Paraneoplastic haematologic syndromes: Good syndrome; Polycythaemia[1]
- Dermatological eg Acanthosis nigricans; Paraneoplastic pemphigus; Sweet syndrome; Leukocytoclastic vasculitis; Dermatomyositis
- Renal eg Electrolyte imbalance (hypokalemia, hypo or hypernatremia, hyperphosphatemia) causing nephropathy and acid-base disturbance due to ectopic hormones produced by tumour cells such as ACTH and ADH. Nephrotic syndrome can also be one of the manifestations of paraneoplastic syndrome.
- Miscellaneous eg Fever, cachexia, anorexia, dysgeusia[6]
Management[edit | edit source]
Management of the patients is based on the type, severity, and location of the paraneoplastic syndrome. First, therapeutic options are to treat underlying malignancy with chemotherapy, radiation, or surgery.
- Other therapeutic options are immunosuppression with corticosteroids or other immunosuppressive drugs, intravenous immunoglobulins, plasma exchange, or plasmapheresis.
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
First, a healthcare provider will perform a clinical exam that would include a general physical and neurological screening.
- Neurological screening: reflexes, sensation, myotomes, balance, and coordination.
- Laboratory tests that could be utilized to diagnose paraneoplastic syndrome include: Blood tests, Spinal tap
- Imaging tests that could be utilized to diagnose paraneoplastic syndrome include: CT Scan; MRI; PET Scan; and PET-CT, which may enhance the detection rate of small cancers
If the physicians cannot find a malignant tumour, the syndrome may be the cause of a tumour that is too small to locate. In this instance, the physician will continue to have follow-up imaging conducted every three to six months for several years unless the cause is identified. [7]
Physical Therapy Management[edit | edit source]
People with paraneoplastic syndrome can have difficulty with walking, balance, coordination, muscle tone, sensory of where the body is in space, and vertigo.
- All of these symptoms the physical therapist can treat with traditional therapy.
- Precautions must be taken into account for the cancer or neoplasm that is involved.[3]
Conclusion[edit | edit source]
The diagnosis and management of paraneoplastic syndromes is difficult.
- In most cases, there is an underlying malignancy responsible.
- Due to the numerous causes, the condition is best managed by an interprofessional team (including a pathologist, oncologist, radiologist, haematologist, nurse specialist, and internist).
- Once the cause is discovered, it needs to be treated.
The management of the patients is based on the type, severity, and location of the paraneoplastic syndrome.
- First, therapeutic options are to treat underlying malignancy with chemotherapy, radiation, or surgery.
- Other therapeutic options are immunosuppression with corticosteroids or other immunosuppressive drugs, intravenous immunoglobulins, plasma exchange, or plasmapheresis.[6]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Radiopedia Paraneoplastic syndromes Available: https://radiopaedia.org/articles/paraneoplastic-syndromes(accessed 24.1.2023)
- ↑ 2.0 2.1 Henry K. Paraneoplastic syndromes: definitions, classification, pathophysiology and principles of treatment. InSeminars in diagnostic pathology 2019 Jul 1 (Vol. 36, No. 4, pp. 204-210). WB Saunders.Available from:https://www.sciencedirect.com/science/article/abs/pii/S0740257019300097 (last accessed 15.7.2020)
- ↑ 3.0 3.1 National Institute of Neurological Disorders and Stroke. NINDS Paraneoplastic Syndromes Information Page. http://www.ninds.nih.gov/disorders/paraneoplastic/paraneoplastic.htm. (accessed 18 March 2013).
- ↑ 4.0 4.1 NIH Paraneoplastic Syndromes Available:https://www.ninds.nih.gov/health-information/disorders/paraneoplastic-syndromes (accessed 24.1.2023)
- ↑ Henry K. Paraneoplastic syndromes: Definitions, classification, pathophysiology and principles of treatment. InSeminars in diagnostic pathology 2019 Jul 1 (Vol. 36, No. 4, pp. 204-210). WB Saunders.
- ↑ 6.0 6.1 6.2 Thapa B, Ramphul K. Paraneoplastic syndromes. InStatPearls [Internet] 2020 Jun 27. StatPearls Publishing.Available from:https://www.ncbi.nlm.nih.gov/books/NBK507890/ (last accessed 15.7.2020)
- ↑ Mayo Clinic. Paraneoplastic syndromes of the nervous system. http://www.mayoclinic.com/health/paraneoplastic-syndromes/DS00840. (accessed 18 March 2013).