Post-traumatic Arthritis
Original Editors - Lynn Leemans Top Contributors - Lynn Leemans, Leana Louw, Admin, Anthonia Abraham, Lucinda hampton, Laura Ritchie, WikiSysop and Kim Jackson
Definition/Description[edit | edit source]
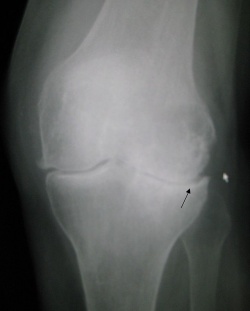
Post-traumatic arthritis is a condition triggered by an acute joint trauma that can lead to osteoarthritis or chronic inflammatory arthropathies.[1] Image is of Knee osteoarthritis, possible a PTA.
Joint injuries, with or without associated disruption of the articular surface, frequently lead to a progressive process of severe debilitating condition known as acute post-traumatic arthritis (PTA). PTA can occur at any age, in any joints and may develop from any kind of acute physical trauma, such as sports, vehicle accident, fall or military injury. Although a single trauma may sometimes be sufficient to induce arthropathy, repeated injuries and excess body weight are known to increase the risk for PTA.[1]
Inflammatory events in the initial phase after injury, such as the increased release of inflammatory cytokines, can predispose to the development of OA or inflammatory arthritis[1].
Clinically Relevant Anatomy [edit | edit source]
Trauma can cause damage to the articular cartilage of the joint, which results in weakening cartilage that is not able to withstand the stress. The articular cartilage layer start to break down as a result of this.[2]
Epidemiology/Etiology [edit | edit source]
Any injury to any joint can lead to traumatic arthritis. It is important to differentiate between regular arthritis and post-traumatic arthritis. Post-traumatic arthritis develops as a result of a trauma, while regular arthritis develops gradually without any apparent outside reason.[3][4] Post-traumatic arthritis makes out about 12% of osteoarthritis cases.[1] Symptom onset can be as long ago as 2-5 years after an injury to the joint was sustained.[3][4] The cartilage can be bruised when too much pressure is exerted on it. This can happen without any superficial appearance of damage. The injury to the joint does not show up until months later. More severe injury to the cartilage can cause loose fragments when the cartilage comes loose from the bone. These loose pieces are not able to heal, and move around in the joint, and can result into catching and subsequent pain. These defects does not heal as with bone, but are instead filled with scar tissue. Broken off cartilage need to be surgically removed from the joint.[5]
Characteristics/Clinical presentation [edit | edit source]
There are several symptoms that can indicate a case of post-traumatic arthritis. It includes the following:[1]
- Swelling of the joint
- Synovial effusion
- Pain in the joint
- Intolerance to weight-bearing activities
- Joint instability
A diagnose of post-traumatic arthritis can be considered, even more when this condition develops at an early age. Post-traumatic arthritis normally recovers spontaneously, but if the symptoms are still present after 6 months, it is seen as chronic.[1] Sometimes pain comes and goes over a long period of time. The pain may or may not be accompanied by inflammation of the joint or surrounding area. Often the symptoms would disappear without any major medical intervention, these symptoms may re-appear after a while. [2]
Risk Factors[edit | edit source]
- Age: The risk of developing post-traumatic arthritis increases with age. This is because the cartilage in the joints becomes more susceptible to damage as we age.
- Gender: Men are more likely to develop post-traumatic arthritis than women. This is thought to be due to the fact that men are more likely to participate in activities that can lead to joint injuries, such as contact sports.
- Genetics: Some people are more genetically predisposed to developing post-traumatic arthritis than others. This is because certain genes may make the cartilage in the joints more susceptible to damage.
- Body weight: People who are overweight or obese are more likely to develop post-traumatic arthritis. This is because excess weight puts more stress on the joints.
- Joint injury: The severity of the joint injury is a major risk factor for developing post-traumatic arthritis. The more severe the injury, the greater the risk of developing arthritis.
- Joint instability: If a joint is unstable, it is more likely to be injured and more likely to develop arthritis. This is because the joint is not properly supported and is more susceptible to wear and tear.
- Occupational exposure: People who are exposed to repetitive motion or vibration at work are more likely to develop post-traumatic arthritis. This is because these activities can put stress on the joints and damage the cartilage.
- Other medical conditions: Some medical conditions, such as rheumatoid arthritis and lupus, can increase the risk of developing post-traumatic arthritis. These conditions can damage the cartilage in the joints, making them more susceptible to injury.
It is important to note that not everyone who experiences a joint injury will develop post-traumatic arthritis. However, the presence of one or more of the risk factors listed above can increase the likelihood of developing this condition.[6]
Differential diagnosis[edit | edit source]
- Osteoarthritis
- Rheumatoid arthritis
- Juvenile rheumatoid arthritis
- Various pathologies related to specific joints
Diagnostic procedures[edit | edit source]
Outcome Measures[edit | edit source]
- Hip Disability and Osteoarthritis Outcome Score
- Knee Injury and Osteoarthritis Outcome Score
- Western Ontario and McMaster universities osteoarthritis index (WOMAC) WOMAC Osteoarthritis Index,
- Algofunctional index (AFI)
- Intermittent and constant osteoarthritis pain index (ICOAP)
- West-Haven-Yale Multidimensional Pain Inventory (Assesses chronic pain in individuals and Recommended for use in conjunction with behavioral and psycho-physiological strategies)
- Oxford Hip Scale
- Oxford Knee Score
- McGill Pain Questionnaire Short-Form
Medical management[edit | edit source]
The primary goals of treating patients with PTA are to minimise the symptoms and loss of function and reduce pain. Currently, treatment for PTA includes anti-inflammatory drugs (non-steroidal anti-inflammatory drugs or intra-articular injections of cortisone), low impact exercise and lifestyle changes, for example, losing weight if necessary.[1]
Conservative management is the treatment of first choice, and surgery is only considered when this fails. Surgical management will determine on the joint affected, as well as the extent of damage to the joint. For example, post-traumatic hip arthritis might be managed with a hip replacement when conservative management fails. Medical management can not stop the disease process of post-traumatic arthritis, but it can be used to manage the symptoms. Supplemental glucosamine and anti-inflammatory pain medications are normally prescribed to patients.[5] Management will be very similar to that of osteoarthritis.
Physiotherapy management [edit | edit source]
Conservative management includes:[5]
- Activity modification
- Unloading the joint with a mobility assistive device
- Exercise program aimed at regaining range of motion, strength and coordination
- Weight management
Physiotherapy also plays a big role in the post-surgical management of these patients. The type of surgery will determine the physiotherapy approach.[5]
Other approaches include
- Joint injections: Corticosteroid injections can help to reduce inflammation and pain in the joint.
- Platelet-rich plasma (PRP) injections: PRP is a concentrated form of platelets that can help to promote healing in the joint.
- Stem cell therapy: Stem cell therapy is a newer treatment option that involves injecting stem cells into the joint. Stem cells have the potential to repair damaged tissue in the joint.
Clinical Bottom Line[edit | edit source]
Post-traumatic arthritis is secondary osteoarthritis that forms after a specific injury to a joint. Symptom can present as long as 2-5 years post injury. Conservative management includes analgesia, as well as physiotherapy. Surgical management is considered when conservative management fails, and again physiotherapy plays a critical part in the post-operative rehabilitation of these patients.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Punzi L, Galozzi P, Luisetto R, Favero M, Ramonda R, Oliviero F, Scanu A. Post-traumatic arthritis: overview on pathogenic mechanisms and role of inflammation. RMD open 2016;2(2):e000279.
- ↑ 2.0 2.1 Brugioni DJ, Falkel J. Total knee replacement rehabilitation: The knee owner’s manual. Alameda CA: Hunter House Inc, 2004.
- ↑ 3.0 3.1 3.2 Ombregt L, Bisschop P, Ter Veer HJ. A system of orthopaedic medicine. Elsevier Limited, 2003.
- ↑ 4.0 4.1 Saltzman CL, Salamon ML, Blanchard GM, Huff T, Hayes A, Buckwalter JA, Amendola A. Epidemiology of ankle arthritis: report of a consecutive series of 639 patients from a tertiary orthopaedic center. The Iowa orthopaedic journal 2005;25:44.
- ↑ 5.0 5.1 5.2 5.3 5.4 Cleveland Clinic. Post-Traumatic Arthritis: Diagnosis and Tests. Available from: https://my.clevelandclinic.org/health/diseases/14616-post-traumatic-arthritis/diagnosis-and-tests (accessed 6 April 2019).
- ↑ Lübbeke A, Salvo D, Stern R, Hoffmeyer P, Holzer N, Assal M. Risk factors for post-traumatic osteoarthritis of the ankle: an eighteen year follow-up study. Int Orthop. 2012 Jul;36(7):1403-10. doi: 10.1007/s00264-011-1472-7. Epub 2012 Jan 17. PMID: 22249843; PMCID: PMC3385887.