Aetiology, Symptoms and Clinical Classifications of Temporomandibular Disorders
Top Contributors - Jess Bell, Wanda van Niekerk, Kim Jackson and Olajumoke Ogunleye
Introduction[edit | edit source]
The temporomandibular joint (TMJ) is considered one of the most complex joints in the body. It plays a significant role in dental occlusion and the neuromuscular system.[1]
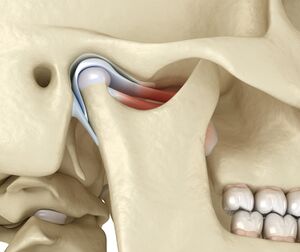
It has been classified as both a compound joint and a double joint. Compound joints typically consist of three or more bones, but the TMJ only has two bones. Instead of a third bone, an articular disc sits between the mandibular fossa and the condyle (Figure 1).[1]
The anatomy, biomechanics and physiology of the TMJ are discussed in detail here and here.
Causes of Facial Pain[edit | edit source]
Temporomandibular disorders (TMDs) are the most common non-dental cause of facial pain. Other acute causes of facial pain are:[2]
- Dental and oral causes
- Maxillary sinusitis
- Salivary gland disorders
- Neuropathic pain (trigeminal nerve region), such as:
- Trigeminal post-herpetic neuralgia
- Post-traumatic trigeminal pain / trigeminal neuropathic pain / atypical odontalgia
- Burning mouth syndrome
- Trigeminal neuralgia and its variants etc
- Vascular causes
- Giant cell arteritis should be considered in individuals aged over 50 years who present with temporal pain that mimics TMD
References[edit | edit source]
- ↑ 1.0 1.1 Chang CL, Wang DH, Yang MC, Hsu WE, Hsu ML. Functional disorders of the temporomandibular joints: Internal derangement of the temporomandibular joint. Kaohsiung J Med Sci. 2018;34(4):223-30.
- ↑ Zakrzewska JM. Differential diagnosis of facial pain and guidelines for management. Br J Anaesth. 2013;111(1):95-104.