Acromioclavicular Joint
Original Editor - Tyler Shultz, Mathilde De Dobbeleer as part of the Vrije Universiteit Brussel Evidence-Based Practice Project
Top Contributors - Admin, Tyler Shultz, Venus Pagare, Kim Jackson, Laura Ritchie, Scott Buxton, Rachael Lowe, Redisha Jakibanjar, Tony Lowe, Olajumoke Ogunleye, Rujuta Naik, Naomi O'Reilly, Scott Cornish, Shaimaa Eldib, Abdelrahman Elaraby, Mathilde De Dobbeleer, Amanda Ager, Evan Thomas, Kai A. Sigel and WikiSysop
Description[edit | edit source]
The Acromioclavicular Joint, or AC Joint, is one of four joints that comprises the Shoulder complex. The AC Joint is formed by the junction of the lateral clavicle and the acromion process of the scapula and is a gliding, or plane style synovial joint. The AC Joint attaches the scapula to the clavicle and serves as the main articulation that suspends the upper extremity from the trunk[1].
The primary function of the AC Joint is:
- To allow the scapula additional range of rotation on the thorax.
- Allow for adjustments of the scapula (tipping and internal/external rotation) outside the initial plane of the scapula in order to follow the changing shape of the thorax as arm movement occurs.
- The joint allows the transmission of forces from the upper extremity to the clavicle[2].
Anatomy[edit | edit source]
Articulating Surface[edit | edit source]
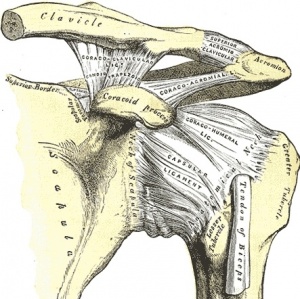
The AC Joint is the articulation between the lateral end of the clavicle and a small facet on the acromion of the scapula. The articular facets are considered to be incongruent, in that they vary in configuration. They may be flat, reciprocally concave-convex, or reversed (reciprocally convex-concave). The inclination of the articulating surfaces varies from individual to individual. 3 joint types are described in which the angle of inclination of the contacting surfaces varied from 16 to 36 degrees from vertical. The closer the surfaces were to the vertical, the more prone the joint was to the wearing effects of shear forces. Given the variable articular configuration, intra-articular movements for this joint are not predictable.[2][4]
Ligaments and Joint Capsule[edit | edit source]
The AC joint capsule and ligaments surrounding the joint work together to provide stability and to keep the clavicle in contact with the acromion process of the scapula.
Joint Capsule[edit | edit source]
The AC Joint has a thin capsule lined with synovium. The capsule is weak and is strengthened by capsular ligaments both inferiorly and superiorly, which in turn are reinforced through attachments from the deltoid and trapezius[4]. Without the superior and inferior capsular ligaments, the AC Joint capsule would not be strong enough to maintain the integrity of the joint.[2]
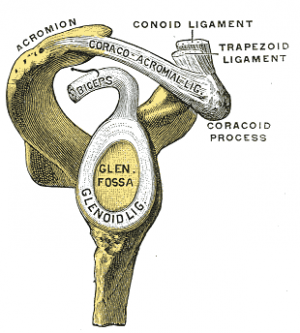
Ligaments[edit | edit source]
- Coracoclavicular Ligaments[2]: Composed of the conoid and trapezoid ligaments (which do not actually come in contact with the joint). This combined ligament is the primary support ligament of the AC Joint. The Coracoclavicular ligaments run from the coracoid process to the underside of the clavicle, near the AC Joint. These ligaments contribute to horizontal stability, making them crucial for preventing superior dislocation of the AC Joint. Both portions also limit the rotation of the scapula. The most critical role of the coracoclavicular ligament is in producing the longitudinal rotation of the clavicle necessary for full ROM during the elevation of the upper extremity.
- The conoid ligament is the fan-shaped component of the coracoclavicular ligament. It is located more medially than the trapezoid ligament.
- The trapezoid ligament is the more lateral portion of the coracoclavicular ligament, and is quadrilateral in shape.
- The acromioclavicular ligament serves to reinforce the joint capsule and serves as the primary restraint to posterior translation and posterior axial rotation at the AC joint.[5]
Joint Disc[edit | edit source]
The disc of the AC Joint is variable in size between individuals, at various ages within an individual and between sides of the same individual. Through the 1st 2 years of age, the joint is actually a fibro-cartilaginous union. With the use of the upper extremity, a joint space develops at each articulating surface that may leave a meniscoid fibrocartilage remnant within the joint.[2]
Muscles[edit | edit source]
The clavicle serves as an attachment for many of the muscles that act on the upper extremity and head, these include:
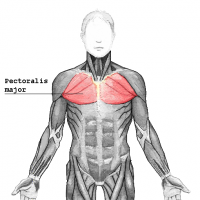
- Pectoralis Major (Clavicular Head)
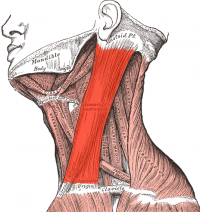
- Sternocleidomastoid
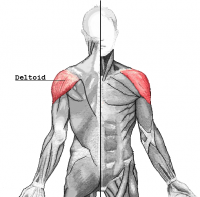
- Deltoid
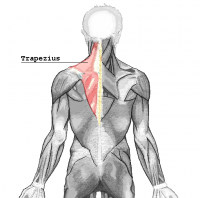
- Trapezius
Function[edit | edit source]
Movement of the Scapulothoracic Joint is generally considered to be a combination of Sternoclavicular and Acromioclavicular motion.[6] Motion of the AC Joint is described as a scapular movement with respect to the clavicle, including[7]:
- Upward/Downward Rotation about an axis directed perpendicular to the scapular plane facing anteriorly and medially. During abduction and flexion, the scapula moves in upward rotation in relation to acromion about 30 degrees, And during adduction and extension the scapula moves in downward rotation relative to the acromion about 30 degrees.[4]
- Internal/External Rotation about an approximately vertical axis. During protraction, the scapula internally rotates on the AC level to fit on the contour of the postero-lateral thorax while during retraction, the scapula externally rotates. [4]
- Anterior/Posterior tipping or tilting about an axis directed laterally and anteriorly. During elevation, the scapula moves in anterior tilting, and during the depression, the scapula moves in posterior tilting in relation to the AC to adjust itself on the dome-shaped thorax.[4]
Closed Packed Position[edit | edit source]
The closed packed position of the AC Joint occurs when the Glenohumeral Joint is abducted to 90 degrees.
Open Packed Position[edit | edit source]
The open packed position of the AC Joint is undetermined.
Pathology/Injury[edit | edit source]
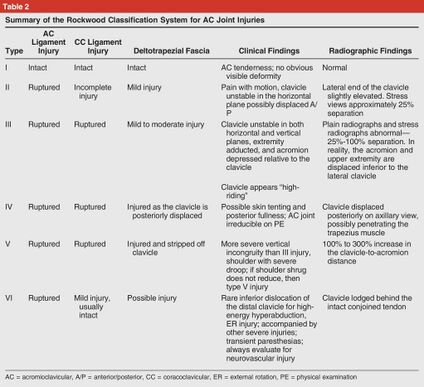
The Rockwood classification of ACJ injuries can be used to plan the management of the patients. For type I and II AC joint pathologies, conservative management is recommended and for injuries graded from IV-VI are recommended to undergo surgical interventions. However, type III injury management remains to be controversial. [9]
Acromioclavicular Stress Tolerance[edit | edit source]
The AC Joint is extremely susceptible to both trauma and degenerative change. This is due to its small and incongruent surfaces that result in large forces per unit area. Degenerative change is common from the 2nd decade on, with the joint space itself commonly narrowed by the 6th decade.[2]
Why are the Acromioclavicular Joint Injuries Relatively Common?[edit | edit source]
The acromioclavicular joint injuries are relatively common accounting for about 40%[10] of all shoulder injuries in contact sports[4], due to the nature of its surface which is highly sloped. Striking the tip of the shoulder over any hard surface will lead to the dislocation of the joint due to the medially and inferiorly directed force toward the shoulder. The loads over the joint will be resisted primarily by the joint’s superior and inferior capsular ligaments, and if the loads exceed the ability of the later two ligaments, the coracoclavicular ligament will offer a secondary resistance to horizontal shear[11], which if failed to endure this great load, its disruption will occur and the AC joint will dislocate or subluxate depending on the intensity of the loads. [4]
References[edit | edit source]
- ↑ Dutton, M. Orthopaedic: Examination, evaluation, and intervention (2nd ed.). New York: The McGraw-Hill Companies Inc, 2008.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Levangie PK, Norkin CC. Joint structure and function. 5th ed. Philadelphia: F.A. Davis Company; 2011. 624 p.
- ↑ Catalyst University. The Acromioclavicular (AC) Joint | Anatomy and Function. Available from: https://youtu.be/WlhtjcLIqDg [last accessed date: 2020/05/31]
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Neumann DA. Kinesiology of the musculoskeletal system: Foundations for Physical Rehabilitation. Elsevier Health Sciences, 2009.
- ↑ Turnbull JR. Acromioclavicular joint disorders. Med Sci Sports Exerc.1998;30:S26-32.
- ↑ Inman VT, Saunders JB, Abbott LC. Observations of the function of the shoulder joint. 1944. Clin Orthop Relat Res. 1996;(330):3-12.
- ↑ Teece, RM, Lunden JB, Lloyd AS, Kaiser AP, Cieminski CJ, Ludewig PM. Three-dimensional acromioclavicular motions during the elevation of the arm. J Orthop Sports Phys Ther. 2008;38(4),181-90.
- ↑ mcp2187. 3D Shoulder. Available from: http://www.youtube.com/watch?v=Jmxz3bEjjGM [last accessed 01/12/12]
- ↑ 9.0 9.1 Frank RM, Cotter EJ, Leroux TS, Romeo AA. Acromioclavicular joint injuries: evidence-based treatment. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 2019 Sep 1;27(17):e775-88.
- ↑ Dragoo JL, Braun HJ, Bartlinski SE, Harris AH. Acromioclavicular joint injuries in National Collegiate Athletic Association football: data from the 2004-2005 through 2008-2009 National Collegiate Athletic Association Injury Surveillance System. Am J Sports Med. 2012;40(9):2066-2071.
- ↑ Fukuda K, Craig EV, An KN, et al: Biomechanical study of the ligamentous system of the acromioclavicular joint. J Bone Joint Surg Am 1986; 68:434–440.