Noonan Syndrome
<div class="noeditbox">This article or area is currently under construction and may only be partially complete. Please come back soon to see the finished work! ({{REVISIONDAY}}/{{REVISIONMONTH}}/{{REVISIONYEAR}})</div>
Top Contributors - Kirenga Bamurange Liliane, Lucinda hampton, Chelsea Mclene, Naomi O'Reilly, Kim Jackson, Rucha Gadgil and Leana Louw
Definition[edit | edit source]
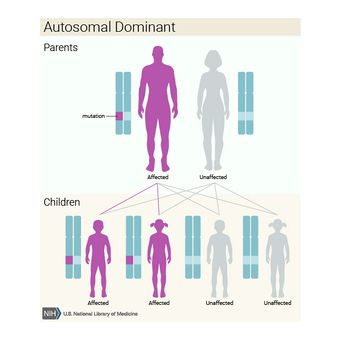
Noonan Syndrome (NS) is an autosomal dominant condition or a genetic mutation that prevents the normal development of different parts of the body. [1]
Noonan Syndrome is a genetic condition that affects both girls an boys in so many ways including:
- distinctive facial features such as broad or webbed neck, drooping eyelids and a wider-than-usual distance between the eyes
- heath problems such as short stature
- chest deformity,
- congenital heart disease
- pulmonary stenosis,
- physical problems
- and possible developmental delays
Noonan and Ehmke were the first to describe a succession of patients with same similarities including unusual faces and multiple malformations like congenital heart disease. As a result, these patients were previously thought to have a form of Turner syndrome, with has a lot of similarities in its clinical features with Noonan Syndrome.[1]
The eponym “Noonan syndrome” was then adopted in recognition of Dr. Jacqueline Noonan who was the first to indicate that this condition occurs in both genders; could be associated with normal chromosomes included congenital heart defects and could be familial.[2]
Epidemiology / Pathological Process[edit | edit source]
The Noonan Syndrome is caused by a mutation of a gene or a faulty gene that is usually inherited from one of the parents. The most commonly altered genes are:
- the PTPN11 gene
- the SOS1 gene
- the RIFT1 gene
- the KRAS
Even though the symptoms are usually the same for all different genes, two of them are associated to specific conditions. The faulty PTPN11 gene is commonly associated with pulmonary stenosis characterized by a narrowed heart valve and the faulty RAF1 gene, associated with cardiomyopathy which is a disease of the heart muscle.
Noonan Syndrome can be caused by mutations in multiple genes. Mutations in the altered genes occur at different degrees. The mutations in the PTPN11 gene cause about half of all cases. SOS1 gene mutations seem to be the second biggest with an additional 10 to 15 percent, followed by the genes RAF1 and RIT1 that account each for about 5 percent of cases. Mutations in other genes each account for a small number of cases. The cause of Noonan syndrome in 15 to 20 percent of people with this disorder is unknown. No matter how they acquired the gene mutation, people with Noonan syndrome have a 50% (1 in 2) chance of passing it on to their children.[3]
There are 2 types of mutations that cause Noonan syndrome:
- Inherited. Children who have one parent with Noonan syndrome who carries the defective gene (autosomal dominant) have a 50 percent chance of developing the disorder.
- Random. Noonan syndrome can develop because of a new mutation in children who don't have a genetic predisposition for the disorder (de novo).[4]
The condition is present from before birth, although milder cases may not be diagnosed until a child gets older. It is believed that 1 in 1000 to 1 in 2500 children.[5]
Clinical Presentation[edit | edit source]
NS is most often characterized by facial and musculoskeletal features. Although these features are more present during early childhood, they change over the time and appear less characteristic during adulthood:
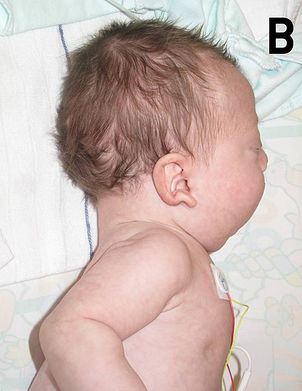
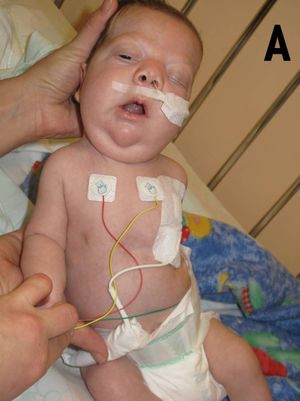
- In the newborn infant, the head is large with :a small face, a tall forehead, wide-spaced eyes, short nose, low set ears, and a broad or webbed neck
Many infants with NS also have heart (cardiac) defects such as
- Pulmonary valvular stenosis
- Hypertrophic cardiomyopathy
- Septal defects
The following characteristics are also seen among individuals with NS:
- Short stature: up to 83% of people with NS have a short stature
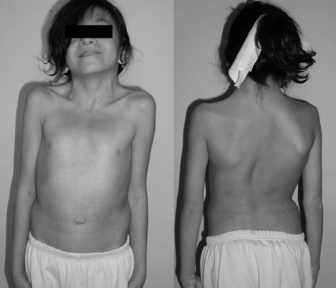
- Pectus deformity of the chest with pectus carinatum (protrusion of sternum an rib) and pectus excavatum (hollow chest)
- Kyphosis
- Scoliosis
- Cubitus valgus (outward deviation of the elbows)
- Rounded shoulders
- Rib abnormalities
- Genu valgum ( Knock knees)
Individuals with NS may also present less common problems including:
- Leaning disability: children with NS tend to often have a mild learning disability due to a lower IQ average
- Feeding problems: children with NS may have problems with sucking and chewing
- Speech problems: articulation difficulty due to a high arched palate and weak muscles
- behavioral problems: some children with NS may have attention problems or difficulty to describe their or people emotions
- Eyes condition such as squint, lazy eye, astigmatation
- Hearing loss
- Hypotonia: decreased muscle tone will make children with NS reach early milestones later compared to other children
- Undescended testicles: one or or both testicles may fail to drop into the scrotum in boys with NS
- Infertitility can be diagnose in boys if undescended testicles are not corrected at an early age
- Lymphoedema
- Bone marrow problems
- Skin problems such as dystrophic nails; extra prominence on pads of fingers and toes; follicular keratosis; hyperelastic skin; moles; thick curly hair or thin sparse hair.[5]
Diagnostic Procedures[edit | edit source]
NS maybe suspected before birth based on the results of a fetal ultrasonography which is used to create an image of the developing fetus.[6] Diagnosis of Noonan syndrome can be made clinically by observing the specific characteristics associated to the condition. These specific characteristics include congenital heart defect; developmental delay that may vary depending on people; short stature; chest malformations as well as facial features.[7] However, because these symptoms can have different causes, further testing is suggested. These tests will help to determine the extent of the symptoms and may include:
- Genetic Testing
- Electrocardiogram (ECG)
- Echocardiogram
- Blood Tests
- Educational Assessment
- Eye Test
- Hearing Test.[8]
- Plotting of growth parameters on NS growth charts
- Renal ultrasound examination
- Clinical and radiographic assessment of spine an rib cage
- Brain and cervical spine MRI if neurologic symptoms are present
- Multidisciplinary developmental evaluation[6].
Management / Interventions[edit | edit source]
Although it's possible to treat many aspects of NS, there is no typical treatment of NS.[9] Because presentation can be mild and the typical facial features recede with age, the diagnosis might be overlooked. Regular detailed follow-up with a multidisciplinary approach is often needed to address the medical and developmental complications of Noonan syndrome.
Differential Diagnosis[edit | edit source]
Several conditions have been found to have similarities with Noonan Syndrome. Noonan syndrome is one of a group of related conditions identified as RASopathies. These conditions all have similar signs and symptoms and are caused by changes in the same cell signaling pathway. Besides Noonan syndrome, the RASopathies consist of cardiofaciocutaneous syndrome, Costello syndrome, neurofibromatosis type 1, Legius syndrome, and Noonan syndrome with multiple lentigines.[10] The differential diagnosis therefore includes Williams syndrome, intrauterine exposure to primidone, fetal alcohol syndrome and Aarskog syndrome. Other cardiocutaneous syndromes such as LEOPARD syndrome, neurofibromatosis and Watson syndrome have a markedly overlapping phenotype.[11]
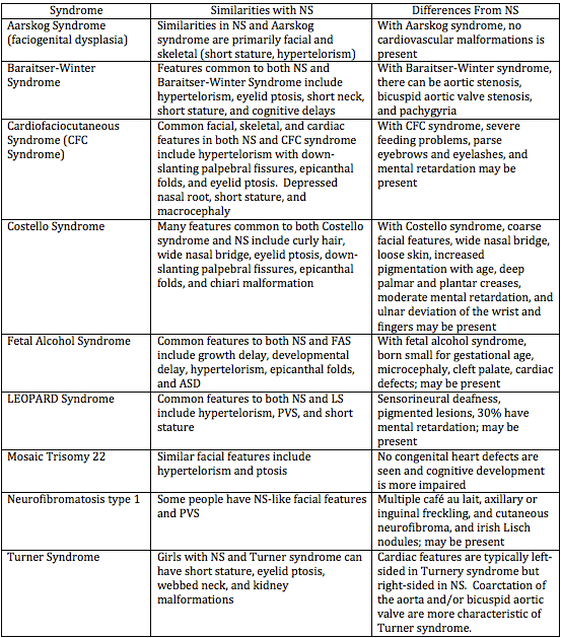
Similarities and Differences between NS and Other Disorders[edit | edit source]
Resources[edit | edit source]
add appropriate resources here
References[edit | edit source]
- ↑ 1.0 1.1 https://emedicine.medscape.com/article/947504-overview#a4
- ↑ https://emedicine.medscape.com/article/947504-overview
- ↑ Noonan Syndrome. Available from https://www.stjude.org/disease/noonan-syndrome.html ( accessed 22September, 2020)
- ↑ Noonan Syndrome. Available from:https://www.mayoclinic.org/diseases-conditions/noonan-syndrome/symptoms-causes/syc-20354422 ( accessed 15 September, 2020)
- ↑ 5.0 5.1 Bhambhani V, Muenke M. Noonan syndrome. Am Fam Physician. 2014; 89(1):37-43.
- ↑ 6.0 6.1 Noonan Syndrome. Judith, E. Allanson and Amy, E. Roberts. Available from: https://www.ncbi.nlm.nih.gov/books/NBK1124/ (accessed 17 September, 2020)
- ↑ Noonan Syndrome Diagnosis. Available from: https://www.news-medical.net/health/Noonan-Syndrome-Diagnosis.aspx ( accessed 20 September, 2020)
- ↑ Noonan syndrome. Available from: https://www.nhs.uk/conditions/noonan-syndrome/diagnosis/#:~:text=You%20may%20be%20referred%20to,t%20rule%20out%20Noonan%20syndrome.( accessed 16 September, 2020)
- ↑ Tafazoli A, Eshraghi P, Koleti ZK, Abbaszadegan M. Noonan syndrome - a new survey. Arch Med Sci. 2017;13:215–222. doi: 10.5114/aoms.2017.64720. Published online 2016 Dec 19.
- ↑ Noonan Syndrome - Genetics Home Reference. U.S National Library of Medicine. Available from: https://ghr.nlm.nih.gov/condition/noonan-syndrome#sourcesforpage (accessed 19 September, 2020)
- ↑ Allanson, JE. Noonan Syndrome. Journal of Medical Genetics,1987, 4: 9-13