Psychosocial Considerations in Patellofemoral Pain: Difference between revisions
Carin Hunter (talk | contribs) No edit summary |
Carin Hunter (talk | contribs) No edit summary |
||
| Line 19: | Line 19: | ||
== Mindfulness == | == Mindfulness == | ||
Wride<ref>Wride J, Bannigan K. [https://www.degruyter.com/document/doi/10.1515/sjpain-2018-0347/html Investigating the prevalence of anxiety and depression in people living with patellofemoral pain in the UK: the Dep-Pf Study.] Scandinavian Journal of Pain. 2019 Apr 1;19(2):375-82.</ref>'s work shows | Wride<ref name=":2">Wride J, Bannigan K. [https://www.degruyter.com/document/doi/10.1515/sjpain-2018-0347/html Investigating the prevalence of anxiety and depression in people living with patellofemoral pain in the UK: the Dep-Pf Study.] Scandinavian Journal of Pain. 2019 Apr 1;19(2):375-82.</ref>'s work shows two important correlations with regards to anxiety and depression | ||
# The prevalence of anxiety and/or depression is higher in the patellofemoral population than the normal population. <ref name=":2" /> | |||
# The prevalence of anxiety and/or depression is higher in young females <ref name=":2" /> | |||
# and we know that a lot of patellofemoral pain is in females, but given that still, the rates are much, much higher.<ref>Boling M, Padua D, Marshall S, Guskiewicz K, Pyne S, Beutler A. [https://onlinelibrary.wiley.com/doi/abs/10.1111/j.1600-0838.2009.00996.x Gender differences in the incidence and prevalence of patellofemoral pain syndrome.] Scandinavian journal of medicine & science in sports. 2010 Oct;20(5):725-30.</ref> | |||
patients | When patients had patellofemoral pain, many of them experienced a sense of loss of identity and a loss of social interactions. When an individual has patellofemoral pain which limits them from participating in their sport of choice, we need to consider that it is not only the activity they are suddenly unable to participate in. They also often loose the sense of wellbeing and social interaction that the sport offered. | ||
A few patients have even been known the change career aspirations and housing choices because of their patellofemoral pain. These types of large lifestyle adaptations, due to a belief regarding their knee pain can | |||
insidious onset, | Patients can battle with their understanding of the causes of their knee pain, especially when it is of insidious onset. Unlike a traumatic injury, knee pain of insidious onset is not marked by an event which the pain can be attributed to. This can be influential to the incorrect assumption that exercise can worsen the pain. When a physical therapist then prescribes exercise based treatment, a patient can be hesitant and non-compliant due to their beliefs. The patient should be educated on the effects of load, repetitive volume, warm up, cool down, footwear, and many other facets vital to understanding exercise. Treatments that patients felt were of benefit to patellofemoral pain where often passive, primarily painkillers, knee supports, and rest. While these might help the pain temporarily, they will not be beneficial to the patient in the long term. | ||
A study by Selhorst <ref>Selhorst M, Fernandez-Fernandez A, Schmitt L, Hoehn J. [https://pubmed.ncbi.nlm.nih.gov/33838141/ Effect of a Psychologically Informed Intervention to Treat Adolescents With Patellofemoral Pain: A Randomized Controlled Trial.] Archives of Physical Medicine and Rehabilitation. 2021 Jul 1;102(7):1267-73.</ref> showed that a short educational video shown to a group of adolescents can reduce kinesiophobia, catastrophisation, pain scores, immediately and at two weeks. This shows the significance of education in patellofemoral pain. | |||
sleep | Another factor to consider is the patients sleep. We should look at the only the quantity or duration of sleep but the quality as well. We should be asking questions such as, How many times does someone wake up in the night? How long does it take to get to sleep? | ||
Bagheri<ref>Bagheri S, Naderi A, Mirali S, Calmeiro L, Brewer BW. [https://meridian.allenpress.com/jat/article/56/8/902/448491/Adding-Mindfulness-Practice-to-Exercise-Therapy Adding mindfulness practice to exercise therapy for female recreational runners with patellofemoral pain: A randomized controlled trial.] Journal of Athletic Training. 2021 Aug 1;56(8):902-11.</ref>'s work showing that physical treatment, sort of standardised typical patellofemoral treatments, with mindfulness was more effective at pain reduction, catastrophisation, kinesiophobia than the same physical treatment. Mindfulness, that's great to see that paper. That's the first paper I've ever seen on, and I'm sure it is, on mindfulness and patellofemoral pain, but why not? It's all around stress reduction, being able to take control of the situation, stay in control, and not be overly alarmed by it | Bagheri<ref>Bagheri S, Naderi A, Mirali S, Calmeiro L, Brewer BW. [https://meridian.allenpress.com/jat/article/56/8/902/448491/Adding-Mindfulness-Practice-to-Exercise-Therapy Adding mindfulness practice to exercise therapy for female recreational runners with patellofemoral pain: A randomized controlled trial.] Journal of Athletic Training. 2021 Aug 1;56(8):902-11.</ref>'s work showing that physical treatment, sort of standardised typical patellofemoral treatments, with mindfulness was more effective at pain reduction, catastrophisation, kinesiophobia than the same physical treatment. Mindfulness, that's great to see that paper. That's the first paper I've ever seen on, and I'm sure it is, on mindfulness and patellofemoral pain, but why not? It's all around stress reduction, being able to take control of the situation, stay in control, and not be overly alarmed by it | ||
| Line 66: | Line 58: | ||
Patients with a high anxiety score were more likely to be female. | Patients with a high anxiety score were more likely to be female. | ||
==== Tampa Scale of Kinesiophobia ==== | |||
The original Tampa Scale of Kinesiophobia is (TSK) was first developed in 1991 by R. Miller, S. Kopri, and D. Todd. TSK is 17 items a self-reporting questionnaire based on evaluation of fear of movement, fear of physical activity, and fear avoidance. It was first developed to distinguish between non-excessive fear and phobia in patients with chronic musculoskeletal pain, specifically the fear of movement in patients with chronic low back pain then widely used for different parts of the body. The questionnaire using 4 points to assess that are based on; the model of fear-avoidance, fear of work-related activities, fear of movement, and fear of re-injury.<ref>Hudes K. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3154068/ The Tampa Scale of Kinesiophobia and neck pain, disability and range of motion: a narrative review of the literature.] The Journal of the Canadian Chiropractic Association. 2011 Sep;55(3):222.</ref> | |||
'''Links:''' | |||
*[[Tampa Scale of Kinesiophobia]] | |||
* [https://novopsych.com.au/wp-content/uploads/2020/05/tsk_assessment.pdf Tampa Scale of Kinesiophobia (TSK) pdf] | |||
* [https://www.mdapp.co/tampa-scale-for-kinesiophobia-tsk-calculator-465/#:~:text=all%2017%20items.-,TSK%20scores%20range%20from%2017%20to%2068%2C%20where%20scores%20of,below%20this%20value%20considered%20low. MDApp, Tampa Scale of Kinesiophobia] | |||
== Key Questions to ask and why == | == Key Questions to ask and why == | ||
Revision as of 17:21, 31 July 2022
Top Contributors - Carin Hunter, Jess Bell, Ewa Jaraczewska, Kim Jackson and Wanda van Niekerk
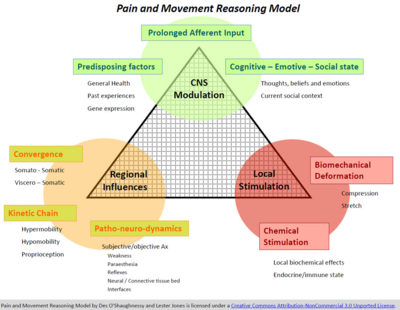
Pain and Movement Reasoning Model , (Jones & O’Shaughnessy,2014)[edit | edit source]
When considering the psychosocial factors affecting the patellofemoral joint, even though the pain and movement reasoning model was not designed for patellofemoral pain, the theory can be effectively applied.
Factors in the Pain and Reasoning Model[edit | edit source]
- Local Stimulation[1][2]
- Biomechanical Stimulation - Bone oedema, fat pad swelling, effusion, retinacular ischaemic changes, bone bruising, or anything local at the knee.
- Chemical Stimulation
- Regional Influences[1][2]
- Kinetic Chain - Excessively pronating foot, anteverted femoral neck or poor control of their hip abduction
- Patho-neuro-dynamics
- Convergence
- Central Nervous System Modulation[1][2] - Minimal research on this area
- Prolonged Afferent Input
- Predisposing Factors
- Cognitive - Emotive - Social state
Mindfulness[edit | edit source]
Wride[3]'s work shows two important correlations with regards to anxiety and depression
- The prevalence of anxiety and/or depression is higher in the patellofemoral population than the normal population. [3]
- The prevalence of anxiety and/or depression is higher in young females [3]
- and we know that a lot of patellofemoral pain is in females, but given that still, the rates are much, much higher.[4]
When patients had patellofemoral pain, many of them experienced a sense of loss of identity and a loss of social interactions. When an individual has patellofemoral pain which limits them from participating in their sport of choice, we need to consider that it is not only the activity they are suddenly unable to participate in. They also often loose the sense of wellbeing and social interaction that the sport offered.
A few patients have even been known the change career aspirations and housing choices because of their patellofemoral pain. These types of large lifestyle adaptations, due to a belief regarding their knee pain can
Patients can battle with their understanding of the causes of their knee pain, especially when it is of insidious onset. Unlike a traumatic injury, knee pain of insidious onset is not marked by an event which the pain can be attributed to. This can be influential to the incorrect assumption that exercise can worsen the pain. When a physical therapist then prescribes exercise based treatment, a patient can be hesitant and non-compliant due to their beliefs. The patient should be educated on the effects of load, repetitive volume, warm up, cool down, footwear, and many other facets vital to understanding exercise. Treatments that patients felt were of benefit to patellofemoral pain where often passive, primarily painkillers, knee supports, and rest. While these might help the pain temporarily, they will not be beneficial to the patient in the long term.
A study by Selhorst [5] showed that a short educational video shown to a group of adolescents can reduce kinesiophobia, catastrophisation, pain scores, immediately and at two weeks. This shows the significance of education in patellofemoral pain.
Another factor to consider is the patients sleep. We should look at the only the quantity or duration of sleep but the quality as well. We should be asking questions such as, How many times does someone wake up in the night? How long does it take to get to sleep?
Bagheri[6]'s work showing that physical treatment, sort of standardised typical patellofemoral treatments, with mindfulness was more effective at pain reduction, catastrophisation, kinesiophobia than the same physical treatment. Mindfulness, that's great to see that paper. That's the first paper I've ever seen on, and I'm sure it is, on mindfulness and patellofemoral pain, but why not? It's all around stress reduction, being able to take control of the situation, stay in control, and not be overly alarmed by it
And, you know, the irony is if we do great physical treatments, maybe someone is more flexible or stronger, their foot sorted out with an orthotic or whatever it may be, we may think - and even their pain might be less - we might feel oh, you know, I've done a good job there. But if they leave your room and they still avoid the stairs because their belief is that it's harmful to them if their knee is noisy on the stairs, or if they still feel highly anxious about doing their sport, or they still avoid going back to their running club because they feel that running bought it on in the first place and that pain meant damage, we have not addressed those psychosocial considerations that really are absolutely as big an issue as any physical thing around the knee.
Ben Smith's fantastic qualitative work and Wride's work in 2018
Bagheri et al., 2021. PFP exs vs exs+mindfulness.
Mindfulness aimed at increasing awareness of thoughts, sensations, emotions all with an attitude of acceptance, curiosity and openness.
Better pain, less catastrophizing, less kinesiophobia w mindfulness.
There is little written about anxiety and depression in PFP but Wride et al., 2019 work in the UK reveals the following key facts regarding the prevalence of anxiety and depression in the PFP population, (n=400):
49.5% demonstrated anxiety.
20.8% indicated depressive symptoms.
When combined, 53% were living with anxiety +/or depression.
Patients with a high anxiety score were significantly younger.
Patients with a high anxiety score were more likely to be female.
Tampa Scale of Kinesiophobia[edit | edit source]
The original Tampa Scale of Kinesiophobia is (TSK) was first developed in 1991 by R. Miller, S. Kopri, and D. Todd. TSK is 17 items a self-reporting questionnaire based on evaluation of fear of movement, fear of physical activity, and fear avoidance. It was first developed to distinguish between non-excessive fear and phobia in patients with chronic musculoskeletal pain, specifically the fear of movement in patients with chronic low back pain then widely used for different parts of the body. The questionnaire using 4 points to assess that are based on; the model of fear-avoidance, fear of work-related activities, fear of movement, and fear of re-injury.[7]
Links:
- Tampa Scale of Kinesiophobia
- Tampa Scale of Kinesiophobia (TSK) pdf
- MDApp, Tampa Scale of Kinesiophobia
Key Questions to ask and why[edit | edit source]
| Question | Reason | Treatment Implication |
| Duration of symptoms | The longer the duration the more likely there will be central pain changes. | Assess for central changes |
| Alteration in sleep quality? | Serotonin (natural painkiller) production suppressed with poor sleep | Recommend re-establishing routine. Non-painful exercise.
Decrease anxiety through education |
| Change in exercise profile? | Can affect sleep, mood, self-esteem, social interactions and conditioning. | Consider exercise programmes for non-painful body parts initially.
Education to minimise fear-avoidance. |
| Can they tolerate the sense of clothing on their knee, eg skinny jeans/tights? | Some patients cannot bear the feeling of material on their knee. Highly suggestive of non-mechanical pain. | Graduated exposure. May need medical management to de-sensitise. |
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Jones LE, O'Shaughnessy DF. The pain and movement reasoning model: introduction to a simple tool for integrated pain assessment. Manual therapy. 2014 Jun 1;19(3):270-6.
- ↑ 2.0 2.1 2.2 O’Shaughnessy D, Jones LE. Making sense of pain in sports physiotherapy: applying the Pain and Movement Reasoning Model. A Comprehensive Guide to Sports Physiology and Injury Management: an interdisciplinary approach. 2020 Nov 13:107.
- ↑ 3.0 3.1 3.2 Wride J, Bannigan K. Investigating the prevalence of anxiety and depression in people living with patellofemoral pain in the UK: the Dep-Pf Study. Scandinavian Journal of Pain. 2019 Apr 1;19(2):375-82.
- ↑ Boling M, Padua D, Marshall S, Guskiewicz K, Pyne S, Beutler A. Gender differences in the incidence and prevalence of patellofemoral pain syndrome. Scandinavian journal of medicine & science in sports. 2010 Oct;20(5):725-30.
- ↑ Selhorst M, Fernandez-Fernandez A, Schmitt L, Hoehn J. Effect of a Psychologically Informed Intervention to Treat Adolescents With Patellofemoral Pain: A Randomized Controlled Trial. Archives of Physical Medicine and Rehabilitation. 2021 Jul 1;102(7):1267-73.
- ↑ Bagheri S, Naderi A, Mirali S, Calmeiro L, Brewer BW. Adding mindfulness practice to exercise therapy for female recreational runners with patellofemoral pain: A randomized controlled trial. Journal of Athletic Training. 2021 Aug 1;56(8):902-11.
- ↑ Hudes K. The Tampa Scale of Kinesiophobia and neck pain, disability and range of motion: a narrative review of the literature. The Journal of the Canadian Chiropractic Association. 2011 Sep;55(3):222.