Rhizarthrosis: Difference between revisions
No edit summary |
No edit summary |
||
| Line 9: | Line 9: | ||
=== Stages of CMC === | === Stages of CMC === | ||
The CMC stages are usually classified according to the Eaton-Litter Classification | The CMC stages are usually classified according to the Eaton-Litter Classification which is obtained through radiological procedures or arthroscopy <ref>Bilge O, Karalezli N. Current review of trapeziometacarpal osteoarthritis (rhizarthrosis). World Journal of Rheumatology. 2015 Jul 12; 5(2):90-5. </ref>. It's a staging protocol with four different stages based on synovitis, joint space, and the laxity of the capsule <ref>Trapeziometacarpal osteoarthritis. Available from: https://en.wikipedia.org/wiki/Trapeziometacarpal_osteoarthritis (Accessed, 18 October 2020) | ||
</ref>. | </ref>. | ||
The four stages of Eaton--Litter Classification <ref>Thumb CMC Joint Arthroplasty. Available from:https://www.touchsurgery.com/simulations/thumb-cmc-joint-arthroplasty (Accessed 15 October 2020)</ref> | The four stages of Eaton--Litter Classification <ref>Thumb CMC Joint Arthroplasty. Available from:https://www.touchsurgery.com/simulations/thumb-cmc-joint-arthroplasty (Accessed 15 October 2020)</ref> | ||
Stage 1: Synovitis Phase | ''Stage 1: Synovitis Phase'' | ||
* Articular contours normal | * Articular contours normal | ||
* Norma Joint, mild narrowing or joint widening suggestive of joint effusion or ligament laxity | * Norma Joint, mild narrowing or joint widening suggestive of joint effusion or ligament laxity | ||
| Line 20: | Line 20: | ||
* No osteophyte formation | * No osteophyte formation | ||
Stage 2: Significant Capsular Laxity | ''Stage 2: Significant Capsular Laxity'' | ||
* Narrowing of CMC joint | * Narrowing of CMC joint | ||
* Mild subchondral sclerotic changes | * Mild subchondral sclerotic changes | ||
| Line 26: | Line 26: | ||
* No or 1/3rd CMC joint subluxation | * No or 1/3rd CMC joint subluxation | ||
Stage 3: Significant Joint Destruction | ''Stage 3: Significant Joint Destruction'' | ||
* Further joint space narrowing with cystic changes and sclerotic bone | * Further joint space narrowing with cystic changes and sclerotic bone | ||
* Prominent osteophytes at the ulnar border of distal trapezium | * Prominent osteophytes at the ulnar border of distal trapezium | ||
| Line 32: | Line 32: | ||
* Mild arthrosis of the scaphotrapezial joint | * Mild arthrosis of the scaphotrapezial joint | ||
Stage 4: Pantrapezial Arthritis | ''Stage 4: Pantrapezial Arthritis'' | ||
* Major subluxation of the joint | * Major subluxation of the joint | ||
* Narrowing of the joint space as in stage 3 | * Narrowing of the joint space as in stage 3 | ||
Revision as of 07:56, 19 October 2020
Introduction[edit | edit source]
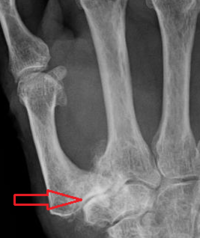
Trapeziometacarpal (TMC) arthritis ( also known as Rhizarthrosis ) is arthritis of the first carpometacarpal (CMC) joint of the thumb. The CMC joint of the thumb, or TMC joint plays a critical role in the normal functioning of the thumb. It is the most important joint connecting the wrist to the metacarpus. Osteoarthritis of the TMC is a severely disabling condition; up to twenty times more common among elderly women than in average.[1]
Stages of CMC[edit | edit source]
The CMC stages are usually classified according to the Eaton-Litter Classification which is obtained through radiological procedures or arthroscopy [3]. It's a staging protocol with four different stages based on synovitis, joint space, and the laxity of the capsule [4].
The four stages of Eaton--Litter Classification [5]
Stage 1: Synovitis Phase
- Articular contours normal
- Norma Joint, mild narrowing or joint widening suggestive of joint effusion or ligament laxity
- Possible mild Suchondral sclerosis
- No osteophyte formation
Stage 2: Significant Capsular Laxity
- Narrowing of CMC joint
- Mild subchondral sclerotic changes
- Small osteophyte formation at the ulnar side of the distal trapezial articular surface
- No or 1/3rd CMC joint subluxation
Stage 3: Significant Joint Destruction
- Further joint space narrowing with cystic changes and sclerotic bone
- Prominent osteophytes at the ulnar border of distal trapezium
- Moderate subluxation radially and dorsally at the base of the first metacarpal
- Mild arthrosis of the scaphotrapezial joint
Stage 4: Pantrapezial Arthritis
- Major subluxation of the joint
- Narrowing of the joint space as in stage 3
- Cystic and sclerotic subchondral bone changes
- Significant erosion and destruction of scaphotrapezial joint
<section> Stage 2: Significant Capslar Laxity
- Narrowingof CMC Joint
- Mild Subchondral sclerotic changes
- Small ( < 2mm) osteophyte formation commonly at the distal trapezial articular surface
- No or < 1/3 CMC joint sbluxation in any projection
</section>
Etiology[edit | edit source]
Causes of TMC arthritis are:
- Excessive repetitive use of the CMC joint of the thumb
- Subluxation
- Lesion of the ligaments or a fracture.
- Laxity of the CMC joint can be hereditary, increased risk for ligament injuries, a primary stimulus in the development of arthritis. Also causes a hyperextension, which is another primary stimulus for the development of arthritis.[6]
- Weakness of the cross links of the fingers (ligament oblique anterior). These ligaments are the most important stabilisers of the fingers. [7]
- Using thumb in occupation, For example, Work-related thumb pain in physiotherapists is a prevalent problem among physiotherapists who administer manual techniques. Factors that appear to be associated with thumb pain include CMC mobility and thumb strength[8].
Signs and Symptoms[edit | edit source]
The first signs of arthritis in the thumb are
- pain, tenderness, and stiffness at the base of your thumb. This occurs with gripping, pinching, or clasping something between the thumb and index fingers or when a mild force, such as when you twist a key in a lock or turn a door handle. An ache after activity can also be a feature.
- Decreased strength and range of motion, For example, opening jars or doing up buttons may become difficult.
- Appearance. The joint may become swollen or develop a bony bump. The joint may appear squarish and enlarged.[9]
Diagnosis[edit | edit source]
- Noticeable lumps or swelling on the first CMC joint
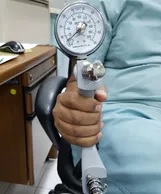
- Thumb CMC grind test
- Plain radiographs showing degenerative changes (bone spurs, thinning of cartilage, loss of joint space) in affected joints are usually diagnostic.[10]
Treatment[edit | edit source]
Conservative measures are the first options for CMC arthritis and can ameliorate symptoms in most cases. These include
Behaviour modification[edit | edit source]
For example, Try to avoid: clenching your hands when carrying things; repetitive movements that involve pinching or twisting
Physiotherapy[edit | edit source]
Techniques include
- range-of-motion and stretching exercises to improve thumb motion.
- Advance to include strength exercise for the thump and fingers.
- Dexterity and fine motor exercises for the hand and thumb. [13]
- Application of therapeutic heat or cold
- Application of electro therapeutic techniques, For example, Therapeutic Ultrasound, TENS. Ultrasound has been found to have the ability to evoke a broad range of therapeutically beneficial such as improved pain and functional outcomes, positive cartilage healing properties and positive phonophoresis for hyaluronan. [14]
- Acupuncture. May work in pain relief for some people.[15]
- Splinting, designed to help reduce pain, prevent deformity, or prevent deformity from getting worse. To wear at night, during flare ups and when doing heavy work with hand.[13]
- Clinical trials have provided evidence that a combination of joint mobilization, neural mobilization, and exercise helps with CMC joint pain.[16]
Pain relief[edit | edit source]
Options include
- Topical medications, such as capsaicin or diclofenac, which are applied to the skin over the joint
- Over-the-counter pain relievers, such as acetaminophen, ibuprofen or naproxen sodium
- Prescription pain relievers, such as celecoxib (Celebrex) or tramadol (Conzip, Ultram)
- Injections. Corticosteroid injections can offer temporary pain relief and reduce inflammation.[10]
.
Surgery [edit | edit source]
If the diagnosis of ‘rhizarthrosis’ is determined too late, none of the above treatments will be helpful. Because of severe pain and movement restriction, surgery could be inevitable.
References[edit | edit source]
- ↑ Wikipedia. CMC joint. Available from: https://en.wikipedia.org/wiki/Carpometacarpal_joint (last accessed 13.4.2019)
- ↑ Mayo clinic. Causes remedies for thumb arthritis. Available from: https://www.youtube.com/watch?v=iVbOPCu5Ius. (last accessed 13.4.2019)
- ↑ Bilge O, Karalezli N. Current review of trapeziometacarpal osteoarthritis (rhizarthrosis). World Journal of Rheumatology. 2015 Jul 12; 5(2):90-5.
- ↑ Trapeziometacarpal osteoarthritis. Available from: https://en.wikipedia.org/wiki/Trapeziometacarpal_osteoarthritis (Accessed, 18 October 2020)
- ↑ Thumb CMC Joint Arthroplasty. Available from:https://www.touchsurgery.com/simulations/thumb-cmc-joint-arthroplasty (Accessed 15 October 2020)
- ↑ Wolf JM, Schreier S, Tomsick S, Williams A, Petersen B. Radiographic laxity of the trapeziometacarpal joint is correlated with generalized joint hypermobility. The Journal of hand surgery. 2011 Jul 1;36(7):1165-9. Available from: https://www.jhandsurg.org/article/S0363-5023(11)00353-4/abstract (last accessed 14.4.2019)
- ↑ A. Gondim Teixeira, Pedro & Omoumi, Patrick & J Trudell, Debra & Ward, Samuel & Blum, Alain & L Resnick, Donald. (2010). High-resolution ultrasound evaluation of the trapeziometacarpal joint with emphasis on the anterior oblique ligament (beak ligament). Skeletal radiology. 40. 897-904. 10.1007/s00256-010-1068-0. Available from: https://www.researchgate.net/publication/49647832_High-resolution_ultrasound_evaluation_of_the_trapeziometacarpal_joint_with_emphasis_on_the_anterior_oblique_ligament_beak_ligament
- ↑ Snodgrass SJ, Riyett DA, Chiarelli P, Bates AM, Rowe LJ. Factors related to thumb pain in physiotherapists. Australian Journal of Physiotherapy. 2003 Jan 1;49(4):243-50. Available from:https://www.sciencedirect.com/science/article/pii/S0004951414601409 (last accessed 10.4.2020)
- ↑ Healthline. Basal joint arthritis. Available from: https://www.healthline.com/health/basal-joint-arthritis#symptoms (last accessed 14.4.2019)
- ↑ 10.0 10.1 Mayo clinic. Thumb arthritis. Available from: https://www.mayoclinic.org/diseases-conditions/thumb-arthritis/diagnosis-treatment/drc-20378344 (last accessed 14.4.2019)
- ↑ Healing hands rehab. CMC arthritis. Available from: https://www.youtube.com/watch?v=wCIA1_tksjA&feature=youtu.be (last accessed 14.4.2019)
- ↑ LB hand therapy. Thumb stability exercises. Available from: https://www.youtube.com/watch?v=rf4R7udarNg&feature=youtu.be
- ↑ 13.0 13.1 Central physiotherapy. Arthritis of the thumb. Available from: https://www.centralphysicaltherapy.com/Injuries-Conditions/Hand/Hand-Issues/Arthritis-of-the-Thumb/a~282/article.html (last accessed 14.4.2019)
- ↑ Srbely JZ. Ultrasound in the management of osteoarthritis: part I: a review of the current literature. The Journal of the Canadian Chiropractic Association. 2008 Mar;52(1):30. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2258240/ (last accessed 15.4.2019)
- ↑ Arthritis Foundation. Acupuncture and osteoarthritis. Available from: https://www.arthritis.org/living-with-arthritis/treatments/natural/other-therapies/mind-body-pain-relief/oa-acupuncture.php (last accessed 15.4.2019)
- ↑ Jospt. The Effectiveness of a Manual Therapy and Exercise Protocol in Patients With Thumb Carpometacarpal Osteoarthritis: A Randomized Controlled Trial. Available from: ☀https://www.jospt.org/doi/full/10.2519/jospt.2013.4524 (last accessed 14.4.2019)
- ↑ Dartmouth-Hitchcock. Basal joint arthritis. Available from: https://www.youtube.com/watch?v=iSA1BSSQLPA (last accessed 15.4.2019)