Hypokalemia: Difference between revisions
No edit summary |
No edit summary |
||
| Line 3: | Line 3: | ||
'''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} | '''Top Contributors''' - {{Special:Contributors/{{FULLPAGENAME}}}} | ||
</div> | </div> | ||
== Definition/Description == | == Definition/Description == | ||
One of the most common electrolyte disturbances seen in clinical practice is hypokalemia. Hypokalemia is known as a electrolyte imbalance that is lower than normal level of potassium in your bloodstream.<ref name=":0">Castro D, Sharma S. [https://www.ncbi.nlm.nih.gov/books/NBK482465/ Hypokalemia]. 2018 Available: https://www.ncbi.nlm.nih.gov/books/NBK482465/<nowiki/>(accessed 18.9.2021)</ref> | One of the most common electrolyte disturbances seen in clinical practice is hypokalemia. Hypokalemia is known as a electrolyte imbalance that is lower than normal level of potassium in your bloodstream.<ref name=":0">Castro D, Sharma S. [https://www.ncbi.nlm.nih.gov/books/NBK482465/ Hypokalemia]. 2018 Available: https://www.ncbi.nlm.nih.gov/books/NBK482465/<nowiki/>(accessed 18.9.2021)</ref> | ||
| Line 31: | Line 27: | ||
== Characteristics/Clinical == | == Characteristics/Clinical == | ||
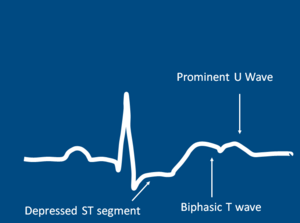
Image 1: ECG Pattern Of Hypokalemia | |||
[[File:Hypokalemia.png|right|frameless]] | |||
An individual with Hypokalemia may exhibit signs of the following: | An individual with Hypokalemia may exhibit signs of the following: | ||
Revision as of 06:37, 18 September 2021
Original Editors - Kara Lawless from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Kara Lawless, Elaine Lonnemann, Lucinda hampton, Admin, Kim Jackson, Wendy Walker and WikiSysop
Definition/Description[edit | edit source]
One of the most common electrolyte disturbances seen in clinical practice is hypokalemia. Hypokalemia is known as a electrolyte imbalance that is lower than normal level of potassium in your bloodstream.[1]
- A normal blood potassium is 3.6 to 5.2 mmol/L.
- Severe and life threatening hypokalemia level is known as <2.5mmol/L. [2]
Potassium helps control how our muscles, heart, and digestive system work. Hypokalemia occurs when your body loses too much potassium or does not absorb enough from food[3].
Etiology[edit | edit source]
A variety of etiologies can result in hypokalemia. These etiologies can be placed into the following categories:
- Decreased potassium intake
- Transcellular shifts (increased intracellular uptake)
- Increased potassium loss (skin, gastrointestinal, and renal losses)[1]
Epidemiology[edit | edit source]
In general, hypokalemia is associated with diagnoses of cardiac disease, renal failure, malnutrition, and shock. Hypothermia and increased blood cell production (for example, leukemia) are additional risk factors for developing hypokalemia[1].
- Hypokalemia is more common in hospitalized patients, up to 15%, as a result of other pathologies.
- Only 3% of the outpatient population is found to have Hypokalemia.
- There has been no significant difference in prevalence between gender and race. [4]
Characteristics/Clinical[edit | edit source]
Image 1: ECG Pattern Of Hypokalemia
An individual with Hypokalemia may exhibit signs of the following:
- Abnormal heart rhythyms
- Constipation
- Fatigue
- Muscle Damage
- Muscle Weakness or spasms
- Paralysis[2]
- Nausea and vomiting
- Polyuria, nocturia or polydipsia
- Altered mental status
- Signs of Ileus
- Hypotension
- Cardia arrest
- Bradycardia or Tachycardia
- Premature atrial or ventricular beats
- Hypoventilation/Respiratory distress
- Respiratory failure
- Lethargy
- Edema (Cushingoid appearance)[5]
Associated Co-morbidities[edit | edit source]
Hypokalemia may present as a result of:
- Chronic Kidney Failure
- Diabetic Ketoacidosis
- Diarrhea/Vomiting
- Excessive Sweating
- Excessive use of laxatives
- Prescription Diuretic Pills
- Primary Aldosteronism [2]
- Liddle Syndrome
- Cushing Syndrome
- Bartter Syndrome
- Fanconi Syndrome
- Bulimia [6]
- Eating large amounts of licorice, herbal teas or chewing tobacco
- Magnesium Deficiency
- Glue Sniffing
- Alcoholism (poor appetite and/or vomiting)
- Amphotericin B therapy
- Hypothermia [4]
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
Hypokalemia is commonly found in a blood test, with <3.5mmol/L as mild hypokalemia and <2.5mmol/L as severe hypokalmia.[2]
In severe cases, a 12-lead electrocardiogram may be necessary if to check for cardiac arrythymias. Findings such as T-wave flattening or prominent U waves will result in hospital admission.[4] Other tests may include:
- arterial blood gas
- basic or comprehensive metabolic panel
Blood tests will also be administered to check the following:
- glucose
- magnesium
- calcium
- sodium
- phosphorus
- thyroxine
- aldosterone levels.[6]
Systemic Involvement[edit | edit source]
| Systems | Impairments |
| Cardiovascular | Cardiac Arrythmias, Hypotension, Premature Artrial or Ventricular Contractions, Bradycardia/Tachycardia/3 |
| Pulmonary | Respiratory Failure or complete paralysis in cases <2.5mmol/L |
| Musculoskeletal |
Muscle weakness, cramping or paralysis. |
| Genitourinary | Polyuria or sexual dysfunction.[2] |
Management[edit | edit source]
The overarching goals of therapy for hypokalemia are to prevent or treat life-threatening complications, replace the potassium deficit, and to diagnose and correct the underlying cause.[1]
Management of the underlying disease or contributing factors constitutes the cornerstone of therapeutic approach. Potassium should be gradually replaced, preferably by oral administration if clinically feasible. In cases of severe/symptomatic hypokalemia and cardiac complications, i.v. administration with continuous ECG monitoring is recommended. In some patients, such as in endocrine related hypokalemia cases, multidisciplinary diagnostic and therapeutic approach is needed.[7]
Physical Therapy Management[edit | edit source]
Hypokalemia is not managed primarily by a physical therapist. Physical therapists should be mindful of common signs of symptoms of hypokalemia when working with patients.
- Potassium levels < 3.2 mEq/L is contraindicated for physical therapy intervention due to the potential for arrhythmia . Due to muscle weakness and cramping, exercise is not effective during the state of hypokalemia.
- Patients should be monitored for potassium levels in order to determine the appropriate time to participate in Physical Therapy.[8]
Differential Diagnosis[edit | edit source]
- Bartter syndrome
- Hyperthyroidism and thyrotoxicosis
- Hypocalcemia
- Hypochloremic alkalosis
- Hypomagnesemia
- Iatrogenic Cushing syndrome
- Metabolic alkalosis
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Castro D, Sharma S. Hypokalemia. 2018 Available: https://www.ncbi.nlm.nih.gov/books/NBK482465/(accessed 18.9.2021)
- ↑ 2.0 2.1 2.2 2.3 2.4 Low Potassium(hypokalemia)[Internet]. 2012 August 10 [cited 2013 March 27] Available from:http://www.mayoclinic.com/health/low-potassium/MY00760
- ↑ Drugs.com Hypokalemia Avaulable: https://www.drugs.com/cg/hypokalemia.html(accessed 18.9.2021)
- ↑ 4.0 4.1 4.2 Hypokalemia [Internet]. 2012 [cited 2013 March 27] Available from:https://www.clinicalkey.com/topics/nephrology/hypokalemia.html#720089
- ↑ Garth D.,Schraga E.Hypokalemia in emergency medicine.[homepage on the Internert]2012 April 13 [cited 2013 March 27] Available from: http://emedicine.medscape.com/article/767448-overview
- ↑ 6.0 6.1 Hypokalemia [Internet]. 2013 March 22 [cited 2013 March 27] Available from: http://www.nlm.nih.gov/medlineplus/ency/article/000479.htm
- ↑ Kardalas E, Paschou SA, Anagnostis P, Muscogiuri G, Siasos G, Vryonidou A. Hypokalemia: a clinical update. Endocrine connections. 2018 Apr 1;7(4):R135-46. Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5881435/ (accessed 18.9.2021)
- ↑ Goodman CC. Fuller KS. In K Falk editor. Pathology: Implications for the Physical Therapist. St. Louis: Saunders Elsevier; 2009. pp.150, 157, 187-189, 480, 558, 927, 1243, 1640-1641
see adding references tutorial.