Intravenous Lines: Difference between revisions
No edit summary |
(add PIV picture) |
||
| Line 13: | Line 13: | ||
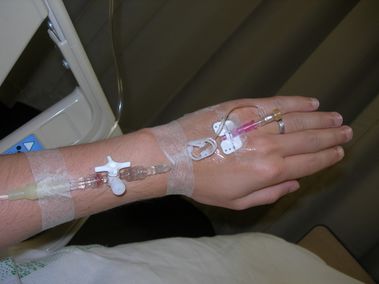
== Peripheral IV (PIV) == | == Peripheral IV (PIV) == | ||
[[File:Peripheral IV.JPG|thumb|379x379px|PIV]] | |||
Overview: | Overview: | ||
* Common and preferred method for short-term therapy (< 6 days) | * Common and preferred method for short-term therapy (< 6 days) | ||
Revision as of 04:21, 18 April 2019
Original Editor - Jin Yoo Top Contributors - Jin Yoo and Kim Jackson
Introduction [1][edit | edit source]
In the acute care setting, intravenous (IV) lines have varied functions:
- to infuse fluids, nutrients, electrolytes, and medication
- to obtain venous blood samples
- to insert catheters into the central circulatory system
Common areas of placement are in the forearm or back of the hand.
Types of Venous Access [2][edit | edit source]
Peripheral IV (PIV)[edit | edit source]
Overview:
- Common and preferred method for short-term therapy (< 6 days)
- A short intravenous catheter is inserted by percutaneous venipuncture into a peripheral vein
- Held in place with a sterile transparent dressing to keep site sterile and prevent accidental dislodgement
- Upper extremities are the preferred sites for insertion
- Usually attached to IV extension tubing with a positive pressure cap
Complications:
- Chemical and mechanical complications include phlebitis, infiltration, extravasation, hemorrhage, and local infection.
- Systemic complications include pulmonary edema, air embolism, catheter embolism, and catheter-related bloodstream infection.
Safety Considerations:
- Increased risk of systemic complications in cardiac and renal patients as well as pediatric patients, neonates, and the elderly
Central Venous Catheter (CVC)[edit | edit source]
Overview:
- Also known as a central line or central venous access device
- Inserted into a large vein in the central circulation system (guided by ultrasound)
- Tip of catheter terminates in the superior vena cava leading to an area just above the right atrium
- Can remain in place for more than a year
Sub-types:
- Peripherally inserted central catheter (PICC)
- Subcutaneous or tunneled central venous catheter ("Hickman", "Broviac", "Groshong")
- Implanted central venous catheter (ICVC, or port-a-cath)
Commonly seen in patients who:
- require antineoplastic medications
- are seriously/chronically ill
- require vesicant/irritant medications
- require toxic medications/multiple medications
- require central venous pressure monitoring
- require long-term venous access/dialysis
- require total parenteral nutrition
- require medications with a pH greater than 9 or less than 5 OR osmolality of greater than 600mOsm/L
- have poor vasculature
- have had multiple PIV insertions/attempts
Safety Considerations:
- Heightened risk for developing a nosocomial infection (need strict adherence to aseptic technique)
- Assessment should include :
- type of CVC and insertion date
- dressing is dry and intact
- lines and sutures are secure
- insertion site is free from redness, pain, or swelling
- positive pressure cap is attached securely
- IV fluids are running through IV pump
- number of lumens and type of fluid running through each lumen
- vital signs
- respiratory/cardiovascular examination to check for signs and symptoms of fluid overload
Complications:
- pulmonary edema
- mechanical complications
- catheter-related bloodstream infection
- infection at insertion site
- air embolism
- occlusion of CVC (mechanical or thrombus)
- damage to CVC line
- Catheter migration
Administration Equipment [2][edit | edit source]
References[edit | edit source]
- ↑ Dutton M. Introduction to Physical Therapy and Patient Skills. New York: McGraw Hill; 2014.
- ↑ 2.0 2.1 Doyle GR, McCutcheon. Clinical Procedures for Safer Patient Care. Victoria, BC: BC Campus; 2015 Available from: https://opentextbc.ca/clinicalskills/ [Accessed 18th April 2019].