Wound Care Terminology
Top Contributors - Stacy Schiurring and Kim Jackson
Introduction[edit | edit source]
The terminology is listed in alphabetical order. This is a living document, terminology will be added as wound care/integumentary courses are created.
A[edit | edit source]
- Angiogenesis: the formation of new blood vessels from existing vasculature.[1]
- Anhidrosis: Dry skin.[2]
- Antimicrobials: a group of agents and substances which reduce the possibility of infection and sepsis.[3]
- Antibiotics: naturally derived from other microorganisms or synthetically created agents which are absorbed into the body for the purpose of killing or preventing bacterial multiplication. These substances can be given parenterally (intramuscularly, intravenously), orally, or applied topically to the skin.[3]
- Antifungals agents are agents that slow or halt the growth of fungi, including yeasts. These substances can be given intravenously, orally or topically.[3]
- Antiseptics: chemical agents that slow or halt the growth of microorganisms on external body surfaces, including wounds, and aid in preventing infection.[4] These substances are non-damaging to living tissue and skin.[5] When applied to the skin antiseptics are not absorbed in a significant quantity into the body.[3]
- Apoptosis: the process of programmed cell death.
- Aseptic technique: utilises measures to prevent the transfer of microorganisms from a healthcare provider and/or the environment to the patient during a wound care procedure.[6]
- Atrophie blanche: a chronic condition that presents as reoccurring, painful, ulcers of the lower leg, ankle, or dorsal foot which result in scar formation. The scars appear as white star-shaped scar radiating out from the healed ulcer. The term atrophie blanche is used to describe the result of the healed ulcer.[7]
B[edit | edit source]
- Bioburden: includes all of the dimensions of wound microbiology involved in the development of wound infection. This can include microbial load, microbial diversity, and the presence of pathogenic organisms.[8]
- Biofilm: a microbial colony encased in a polysaccharide matrix attached to a wound surface. Biofilms can affect the healing of chronic wounds due to the production of destructive enzymes and toxins which can keep the wound in a chronic inflammatory state.[9]
- Biopsy: the skilled removal of cells or tissues for the purpose to determine a diagnosis or infection.
- Blanchable erythemia: redness of the skin which blanches (turns white when pressed with a fingertip) and then quickly returns to the original redness once the pressure is removed.
- Burn wound: a wound caused by heat or due to radiation, radioactivity, electricity, friction or contact with chemicals.[10]
- Burn wound conversion: phenomenon where superficial burns that appear to retain the ability to spontaneously heal, convert later into deeper wounds in need of surgical intervention.[11]
C[edit | edit source]
- Callus: (also known as hyperkeratosis) an area of thickened skin caused by friction, pressure, or other physical or chemical irritation.[12]
- Cellular senescence: the process of cellular aging, meaning a cell permanently stops dividing but does not die.
- Charcot foot syndrome: a serious limb-threatening lower-extremity complication of diabetes characterized by varying degrees of bone and joint disorganization due to underlying neuropathy, trauma, and changes in bone metabolism.[13]
- Clean technique: utilises measures to reduce the numbers of microorganisms to minimize the risk of microorganism transmission from healthcare provider and/or the environment to the patient during a wound care procedure.[6]
- Colonization: the presence of multiplying microorganisms on the surface of a wound which does not cause an immune response from the host.
- Contamination: the beneign presence of bacteria within a wound without any host immune reaction.
- Cyanotic: tissue which has become blue in colour due to lack of oxygenation.
- Cytotoxic: the ability of a substance or process to damage cells and cause cell death, including the death of healthy cells and viable tissue in a wound bed.[14]
D[edit | edit source]
- Debridement: the removal of nonviable tissue using sharp surgical instruments, mechanical (wiping), autolytic (breakdown by natural processes of the body), enzymatic (use of a topical agent) means.
- Dehiscence: a partial or complete separation of approximated wound edges due to a failure of proper wound healing.[15]
- Dependent rubor: an red discolouration of the limbs which occurs when in a gravity dependent position, most commonly associated with peripheral artery disease.[16]
- Desiccation: tissue which has become dried out.
- Devitalised tissue: necrotic or dead tissue within the wound bed. It must be removed for proper healing to occur and to decrease infection risk. Also known as non-viable or necrotic tissue.
- Disinfectants: destroy microorganisms on non-living objects or surfaces.[3]
E[edit | edit source]
- Epibole: rolled or curled-under wound edges
- Epithelial bridging: incomplete wound epithelialisation presenting as strands or patches of tissue which form 'bridges' across the wound bed secondary to infection.
- Epithelial cells: the outer layer of cells which form the skin and line the alimentary canal. It is pink or red in colour and has the appearance of "new skin."
- Erythemia: red colouration of the skin, often as a result of injury or irritation or infection.
- Eschar: non-viable tissue that presents as dry, adhered to the wound bed, and has a spongy or leather-like appearance. It indicates deeper tissue damage and can be black, grey, or brown. It must be removed in order for healing to occur. Eschar is not synonymous with a scab.
- Exudate: drainage from a wound. Types of exudate include: serous (thin, watery, and straw-coloured), sanguineous (bloody), serosanguineous (a mixture of serous and sanguineous), purulent (distinctively thick and yellow, grayish or green in colour), seropurulent (a mixture of serous and purulent), and autolytic (the result of the liquifaction of necrotic tissue and phagocytosis of bacteria, typically thick and milky-white to tan in colour).
F[edit | edit source]
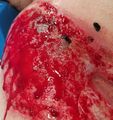
- Friable: bleeds easily with very little contact pressure.
G[edit | edit source]
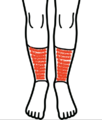
- Gaiter area: area located circumferentially around the lower leg from the mid calf to just below the medial and lateral malleoli, common location for venous wounds.[16]
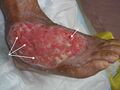
- Granulation tissue: new growth of small blood vessels and connective tissue. It is soft and spongy, and may bleed when touched. Granulation tissue is usually pale pink initially, and then beefy red as it is vascularised.[16]
H[edit | edit source]
- Haemosiderin staining: presents as brownish speckled staining of the skin, common with venous wounds.[16]
- Hemostasis: the first stage of wound healing, involves clot and scab formation.[17]
- Hydrotherapy: involves the use of water for soothing pains and treating certain medical conditions using equipment ranging in size from swimming pools to whirlpool tanks.[18]
- Hypergranulation: an overgrowth of granulation tissue that rises above the level of the wound surface. It is irregular in shape and has large or swollen granules. Hypergranulation is typically due to maceration, infection, or friction on the wound bed. It must be removed for proper healing to occur.[19]
- Hypertrophic nails: thickened, brittle, crumbly, and or ragged nails.[16]
I[edit | edit source]
- Iatrogenic: describes a medical disorder, illness, or injury caused in the process of medical treatment.[20]
- Induration: abnormal firmness of tissue with margins and sometimes has an orange peel appearance.[19]
- Infection: "wound infection is the invasion of a wound by proliferating microorganisms to a level that invokes a local, spreading and/or systemic response in the host. Microorganisms multiply within the wound, developing a range of virulence factors to overcome the host defences leading to local tissue damage and impeding wound healing."[21]
- Ischaemia: decreased or lack of blood supply to a part of the body.
J[edit | edit source]
K[edit | edit source]
L[edit | edit source]
M[edit | edit source]
- Maceration: softening of tissue caused by excessive moisture. This tissue appears white due to a loss of pigmentation, and it is often soft and soggy.[16]
N[edit | edit source]
- Necrosis: death of body tissue.
- Non-viable tissue: necrotic or dead tissue within the wound bed. It must be removed for proper healing to occur and to decrease infection risk. Also known as necrotic or devitalised tissue.
O[edit | edit source]
- Oedema: a collection of fluid in an area of the body, it is a normal response seen in the inflammatory phase. Types include: pitting oedema (assessed by pressing your finger into the skin for five seconds and then releasing your finger, indention remains in place once pressure is removed) and non-pitting oedema (stretched skin that is shiny and hard).[19]
- Onychomycosis: a fungal infection that presents as a yellowish or brownish nails, the nail may separate from the nail bed.[16]
P[edit | edit source]
- Periwound: the area around a wound that may be affected by "wound-related factors and/or underlying pathology." [22]
- Petechiae: small, red or purple spots of bleeding under the skin formed by ruptured capillaries.[23]
- Primary intention: wounds which have been closed with external force using sutures, staples, adhesive strips or glue.[17]
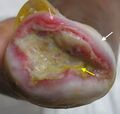
- Pseudo-Eschar: A thick gelatinous yellow or tan film that forms with silver sulfadiazine cream combining with wound exudate. It can often be mistaken for eschar, but it can be removed with mechanical debridement.[23]
Q[edit | edit source]
R[edit | edit source]
- Re-epithelialization: migration of new skin cells over the surface of the wound.[17]Also known as resurfacing.
S[edit | edit source]
- Scab: a collection of dried blood cells, platelets, and serum on top of the skin surface. Wound healing occurs beneath the scab.
- Secondary intention: wounds which heal as a result of the body's inflammatory response, formation of new granulation tissue to fill the empty space, and then closure via re-epithelialisation.[24]
- Sepsis: a life-threatening medical emergency where the body undergoes an extreme response to an infection. It is a life-threatening medical emergency. Sepsis occurs when an infection triggers a chain reaction throughout the body.[25]
- Slough: non-viable subcutaneous tissue and by-products. It is usually yellow to tan in colour and can be mucousy or stringy, and is a result of the body breaking down dead cells and ranges from non-adherent to loosely adherent to tissue.
- Sterile: free of germs or infectious agents
- Surfactant: a primary component of cleaning detergents and means surface active agent. It acts to remove containments from the wound surface.
T[edit | edit source]
- Trophic changes: changes in skin texture, changes in nail beds, loss of hair, shiny skin
U[edit | edit source]
V[edit | edit source]
W[edit | edit source]
- Wound bed: the base or open area of a wound.
- Wound border/edges/margins: the place where the wound bed meets the periwound skin surface.
- Wound cleansing: removal of surface contaminants, loose debris, slough, softened necrosis, microbes and/or remnants of previous dressings from the wound surface and from the periwound skin.[26]
X[edit | edit source]
Y[edit | edit source]
Z[edit | edit source]
References[edit | edit source]
- ↑ National Library of Medicine. Overview of Angiogensis. Available from: https://www.ncbi.nlm.nih.gov/books/NBK53238/ (accessed 27/July/2023).
- ↑ Merwarth, D. Understanding the Foot Programme. Introduction to Foot Neuropathy. Physioplus. 2023.
- ↑ 3.0 3.1 3.2 3.3 3.4 Nankervis H, Thomas KS, Delamere FM, Barbarot S, Rogers NK, Williams HC. Antimicrobials including antibiotics, antiseptics and antifungal agents. InScoping systematic review of treatments for eczema 2016 May. NIHR Journals Library.
- ↑ DermNet. Antiseptics. Available from: https://dermnetnz.org/topics/antiseptic (accessed 26 March 2023).
- ↑ Suzuki JB, Misch CE. Periodontal and maintenance complications. InMisch's Avoiding Complications in Oral Implantology 2018 Jan 1 (pp. 771-826). Mosby.
- ↑ 6.0 6.1 Brigham and Woman's Hospital. Aseptic versus Clean Technique. Available from: https://www.brighamandwomens.org/assets/BWH/pediatric-newborn-medicine/pdfs/aseptic-technique.pdf (accessed 29/May/20123).
- ↑ StatPearls. Atrohpie blanche. Available from: https://www.statpearls.com/ArticleLibrary/viewarticle/417 (accessed 29/May/2023).
- ↑ Gardner SE, Frantz RA. Wound bioburden and infection-related complications in diabetic foot ulcers. Biological research for nursing. 2008 Jul;10(1):44-53.
- ↑ Rajpaul K. Biofilm in wound care. British journal of community nursing. 2015 Mar 1;20(Sup3):S6-11.
- ↑ World Health Organization. Burns. Available from: https://www.who.int/news-room/fact-sheets/detail/burns (accessed 29/May/2023).
- ↑ Palackic A, Jay JW, Duggan RP, Branski LK, Wolf SE, Ansari N, El Ayadi A. Therapeutic strategies to reduce burn wound conversion. Medicina. 2022 Jul 11;58(7):922.
- ↑ Britannica. Callus. Available from: https://www.britannica.com/science/callus-dermatology (accessed 29/May/2023).
- ↑ Rogers LC, Frykberg RG, Armstrong DG, Boulton AJ, Edmonds M, Van GH, Hartemann A, Game F, Jeffcoate W, Jirkovska A, Jude E. The Charcot foot in diabetes. Journal of the American Podiatric Medical Association. 2011 Sep 1;101(5):437-46.
- ↑ Merwarth, D. Management of Burn Wounds Programme. Burn Wound Cleansing and Solutions. Physioplus. 2023.
- ↑ Rosen RD, Manna B. Wound dehiscence. InStatPearls [Internet] 2022 May 8. StatPearls Publishing.
- ↑ 16.0 16.1 16.2 16.3 16.4 16.5 16.6 Palmer, D. Characteristics and Identification of Wound Types. Physiotherapy Wound Care Programme. Plus. 2022.
- ↑ 17.0 17.1 17.2 Palmer, D. Skin Anatomy, Physiology, and Healing. Physiotherapy Wound Care Programme. Plus. 2022.
- ↑ Centers for Disease Control and Prevention. Water Use in Hydrotherapy Tanks. Available from: https://www.cdc.gov/healthywater/other/medical/hydrotherapy.html (accessed 21 March 2023).
- ↑ 19.0 19.1 19.2 Palmer, D. Integumentary Physiotherapy Programme. Basic Wound Assessment. Physioplus. 2023.
- ↑ Dictionary.com. Iatrogenic. Available from: https://www.dictionary.com/browse/iatrogenic (accessed 31/May/20123).
- ↑ Wounds International. Wound Infection In Clinical Practice: Principles of best practice. Available from: https://www.woundsinternational.com/resources/details/wound-infection-in-clinical-practice-principles-of-best-practice (accessed 26/11/2022).
- ↑ LeBlanc K, Beeckman D, Campbell K et al (2021) Best practice recommendations for prevention and management of periwound skin complications.
- ↑ 23.0 23.1 Merwarth, D. Management of Burn Wounds Programme. Burn Wound Assessment. Physioplus. 2023
- ↑ Palmer, D. Skin Anatomy, Physiology, and Healing. Physiotherapy Wound Care Programme. Plus. 2022.
- ↑ Centers for Disease Control and Prevention. What is Sepsis. Available from: https://www.cdc.gov/sepsis/what-is-sepsis.html#:~:text=Sepsis%20is%20the%20body%27s%20extreme,%2C%20skin%2C%20or%20gastrointestinal%20tract. (accessed 30/May/2023).
- ↑ Hayek S, El Khatib A, Atiyeh B. Burn wound cleansing-a myth or a scientific practice. Annals of burns and fire disasters. 2010 Mar 3;23(1):19.