Turf toe
Original Editors - Charlotte Sirago
Top Contributors - Charlotte Sirago, Kim Jackson, Admin, Shaimaa Eldib, Fasuba Ayobami, Simisola Ajeyalemi, WikiSysop, Claire Knott, Wanda van Niekerk, Jess Bell, Khloud Shreif, 127.0.0.1, Rachael Lowe, Evan Thomas, Oyemi Sillo and Naomi O'Reilly
Definition/Description[edit | edit source]
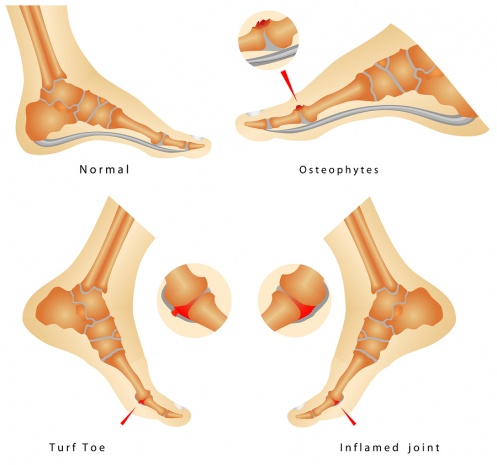
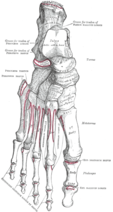
Turf toe is an injury of the first metatarsophalangeal(MTP) articulation, due to hyperextension of the big toe, which leads to damage of the plantar capsuloligamentous complex. It may cause tearing or complete disruption of these structures.
Clinically Relevant Anatomy[edit | edit source]
The slightly concave shape of the proximal phalanx with which the first metatarsal articulates creates little joint stability. The plantar capsule is thicker on the proximal phalanx and finishes in a thinner part on the metatarsal head. It supports the under-surface of the metatarsal head and resists hyperextension of the metatarsophalangeal joint.[1] Additionally to the plantar capsule and the collateral ligaments, the MTP joint is dynamically stabilized by the flexor hallucis brevis (FHB)(the hallucal sesamoids embedded in the FHB tendons), the adductor hallucis and the abductor hallucis tendons.[2]
Epidemiology /Etiology[edit | edit source]
In 1976 turf toe was, for the first time, described by Bowers and Martin. They studied the soccer players at the University of West Virginia and ascertained that during one season there was an average of 5,4 turf toe injuries.[2][3] Further studies showed that the injury occurred more frequently when soccer was played on artificial turf surfaces.
It is caused by an overload on the hallux MTP joint in hyper-dorsiflexion position as happens when one player falls on another players’ heel. Too strong adhesion at the surface so that the shoe sticks, while the bodyweight moves forwards when the player tries to stop quickly may cause an acute turf toe. A chronical condition is mostly caused by frequent running and jumping with extremely flexible shoes.[2][4][5] [6] The injury results very often not due only to hyperextension but also to a degree of valgus stress.
Characteristics/Clinical Presentation[edit | edit source]
It is characterized by pain as a first symptom, localized swelling, ecchymosis and stiffness of the joint. With an appropriate evaluation, we can divide the disease into three grades, each with its own symptoms and treatment protocols.
- Grade I injury symptoms include:
- Local swelling
- Plantar structures attenuation or stretching
- Minimal ecchymosis.
- Grade II injury symptoms include:
- Moderate swelling
- Partial tear of plantar structures
- Restricted motion as a result of pain.
- Grade III injury symptoms include:
Differential Diagnosis[edit | edit source]
- Reverse turf toe
- Soccer toe
- Hallux rigidus
- Hallux limitus
- Hallux valgus
Examination[edit | edit source]
The physical examination starts with observation and palpation of the sensitivity on the hallux MTP joint, evaluating the stability and the flexion strength. The palpation focuses primarily on the collateral ligaments, dorsal capsule and the plantar sesamoid complex.[2]
If pain is localized on the proximal sesamoids it indicates a strain of the flexor hallucis brevis musculotendinous junction, while turf toe injury is located distal to the sesamoids.
Various range of motion manoeuvres of the joint can also be used to identify different injuries. Comparing the active flexion strength with the contralateral side, may reveal a disruption of the FHB or plantar plate.[2]
Applying a varus and/or valgus stress to the collateral ligaments should also be performed:
- Dorsoplantar drawer test (Thompson and Hamilton)[7][8] - this tests the competence of the plantar plate
- Active flexion and extension at the MTP and interphalangeal joints - this tests the extensor and flexor tendons and the plantar plate.
Medical Management[edit | edit source]
Conservative management will always be the first line of intervention and may include Injection therapy.[9] If conservative management is not successful then surgical intervention may be considered. The main criteria for surgical interventions are[2]:
- Large capsular avulsion with unstable MTP joint
- Diastasis of bipartite sesamoid
- Diastasis of sesamoid fracture
- Retraction of sesamoid
- Traumatic hallux valgus deformity
- Vertical instability (positive Lachman test result)
- Loose body in MTP joint
- Chondral injury in MTP joint
- Failed conservative treatment
Physical Therapy Management[edit | edit source]
The three grades of the injury each have a different physical therapy approach although the initial treatment intervention for all three consists of the RICE protocol (rest, ice, compression, elevation).
Interventions for a Grade I Injury[edit | edit source]
Once the acute phase is over, taping in slight plantar flexion, limits movement, protecting the toe from excessive range of motion and also provides compression. Rehabilitation can begin 3 to 5 days after the injury starting with gentle, passive plantarflexion and a gradual increase in strengthening exercises. Distraction and dorsal and proximal sliding of the proximal phalanx on the first metatarsal can help to restore normal ROM and strength.[10]
The patient may participate in non-weight bearing athletic activities such as bicycling, pool therapy and elliptical training.[2] It’s advisable that the athlete wears stiff-soled shoes limiting the motion of the hallux.[2][3]
Interventions for a Grade II Injury[edit | edit source]
A grade II turf toe injury needs at least 2 weeks before returning to activity, although the time will depend on the sport that the athlete plays. The first aim of treatment will focus on increasing the range of motion and reducing the pain, and if the athlete can tolerate it, passive joint mobilizations are indicated.
Only after the symptoms, such as pain and swelling, have been reduced can more intensive rehabilitation begin. However, care must be taken to protect the toe, either by using a turf toe plate or a Morton’s extension orthotic.
Pulsed ultrasound or ionophoresis can be applied to manage inflammation and assist the healing of the soft tissues. Active exercises can also be introduced to encourage toe extension and flexion, such as toe crunches, curling up a towel with the toes, moving the toes in a bucket of sand and short foot exercises.[10] As progress is made the athlete can progress to higher impact activities (jogging, running, cutting and jumping).[2][4]
Interventions for a Grade III Injury[edit | edit source]
The nonsurgical management of a grade III injury requires 8 weeks of recovery and immobilization in plantar flexion. Before restarting sport activity, the hallux MTP joint should return to a 50° to 60° painless, passive dorsiflexion motion. Complete rehabilitation can take up to 6 months.[2]
The most important part of the treatment for turf toe is physical therapy rehabilitation and prevention by using toe protectors/orthotics, but in certain cases a surgical intervention may be necessary.[2]
References[edit | edit source]
- ↑ Yao L, Do HM, Cracchiolo A, Farahani K.- Plantar plate of the foot: findings on conventional arthrography and MR imaging, AJR Am J Roentgenol. 1994 Sep;163(3):641-4.fckLRBooks
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 Jeremy J., McCormick, MD, Robert B. Anderson, MD -Turf Toe: Anatomy, Diagnosis, and Treatment, Clin Sports Med. 2010 Apr;29(2):313-23 Levels of evidence : A
- ↑ 3.0 3.1 3.2 Robert B. Anderson, MD, Kenneth J. Hunt, MD, Jeremy J. McCormick, MD -Management of Common Sports-related Injuries About the Foot and Ankle, Journal of the American Academy of Orthopaedic Surgeons 2010; 18: 546-556 Levels of evidence: A
- ↑ 4.0 4.1 Lisa Chin, MS, ATC and Jay Hertel, PhD, ATC -Rehabilitation of Ankle and Foot Injuries in Athletes, Clin Sports Med. 2010 Jan;29(1):157-67 Levels of evidence: C
- ↑ Ashman CJ, Klecker RJ, Yu JS.- Forefoot Pain Involving the Metatarsal Region: Differential diagnosis with MR Imaging, Radiographics. 2001 Nov-Dec;21(6):1425-40. Levels of evidence: A
- ↑ Freddie H. FU, M.D , David A.Stone, M.D. –Sports Injuries Mechanisms Prevention Treatment – Williams & Wilkins (1994) p. 620 Levels of evidence: D
- ↑ Thompson FM, Hamilton WG – Problems of the second metatarsophalangeal joint,Orthopedics 10:83, 1987
- ↑ Gerard V.YU, Molly S.Judge, Justin R. Hudson, Frank E. Seidelmann- Predislocation Syndrome Progressive Subluxation/dislocation of the Lesser Metatarsophalangeal JointJournal of the American Podiatric Medical Association 2002 April;92(4): 182- 199 Levels of evidence : A
- ↑ Alfred F. Tallia, MD., M.P.H., and Dennis A. Cardone. D.O., C.A.Q.S.M. -Diagnostic and Therapeutic Injection of the Ankle and Foot, American Academy of family Physicians 2003;68:1356-62 Levels of evidence: A
- ↑ 10.0 10.1 Paul K. Canavan – Rehabilitation in Sports Medicine A comprehensive guide – Appleton & Lange (1998) p. 376-377 Levels of evidence : D