Thermotherapy
Original Editor - Kirianne Vander Velden
Lead Editors - Bianca Geeroms, Anja Vanroelen, Charles Senay, Robert Wright, Kirianne Vander Velden, Admin, Kim Jackson, Daiton Wells, Ella Rubbens, Oyemi Sillo, WikiSysop, Tony Varela, 127.0.0.1, Hau Nguyen, Scott Buxton, Claire Knott, Chelsea Mclene, Aminat Abolade, Laura Ritchie and Evan ThomasWelcome to Arkansas Colleges of Health Education School of Physical Therapy Musculoskeletal 1 Project. This space was created by and for the students at Arkansas Colleges of Health Education School in the United States. Please do not edit unless you are involved in this project, but please come back in the near future to check out new information!!
Definition/Description [edit | edit source]
Thermotherapy consists of application of heat or cold (cryotherapy) for the purpose of changing the cutaneous, intra-articular and core temperature of soft tissue with the intention of improving the symptoms of certain conditions. Cryotherapy and thermotherapy are useful adjuncts for the treatment of musculoskeletal injuries and soft tissue injuries. Using ice or heat as a therapeutic intervention decreases pain in joint and muscle as well as soft tissues and they have opposite effects on tissue metabolism, blood flow, inflammation, oedema and connective tissue extensibility. Thermotherapy can be used in rehabilitation facilities or at home. [1] [2] [3] [4]
Purpose[edit | edit source]
The goal of thermotherapy is to alter tissue temperature in a targeted region over time for the purpose of inducing a desired biological response. The majority of thermotherapies are designed to deliver the thermal therapy to a target tissue volume with minimal impact on intervening or surrounding tissues.
Heat[edit | edit source]
By increasing the temperature of the skin/soft tissue, the blood flow increases by vasodilatation. The metabolic rate and the tissue extensibility will also increase. Heat increases oxygen uptake and accelerates tissue healing, it also increases the activity of destructive enzymes, such as collagenase, and increases the catabolic rate.
Cold[edit | edit source]
By decreasing the temperature of the skin/soft tissue, the blood flow decreases by vasoconstriction. It will be followed by a vasodilatation which will prevent against hypoxic damage (hunting reflex: If the cold pack is left on the skin for more than 10 minutes, the blood vessels will dilatate). The tissue metabolism will decrease just like the neuronal excitability, inflammation, conduction rate and tissue extensibility. At joint temperatures of 30°C or lower, the activity of cartilage degrading enzymes, including collagenase, elastase, hyaluronidase, and protease, is inhibited. the decreased metabolic rate limits further injury and aids the tissue in surviving the cellular hypoxia that occurs after injury.
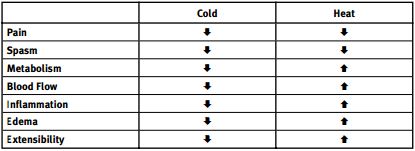
Figure 1:Pathophysiologic effects of topical modalities [4]
Both applications can reduce the pain, but the question of when to use which application is still debated. Therefore, patient’s preference can be taken into consideration when deciding which thermotherapy tool to use. [1] [5] [6] [7]
Application[edit | edit source]
Heat[edit | edit source]
Heating of superficial tissues can be achieved using hot packs, wax baths, towels, sunlight, saunas, heat wraps, steam baths/rooms. Heat can be induced in the deeper tissues through electrotherapy (ultrasound, shockwave and infrared radiation).
Exercise in warm water, usually called hydrotherapy, aqua therapy or balneotherapy, is a popular and effective treatment[8] with a pain relief effect for many patients with painful neurologic or musculoskeletal conditions. The warmth of water may block nociception by acting on thermal receptors and mechanoreceptors, thus influencing spinal segmental mechanisms. It gives positive effects on cutaneous barrier homeostasis and a anti-inflammatory activity. In addition, the warmth may enhance blood flow and muscle relaxation. The hydrostatic effect may also relieve pain by reducing peripheral oedema and by dampening sympathetic nervous system activity. [9] [10] [8]
Cold[edit | edit source]
Cooling is achieved using ice packs, ice baths, cooling gel packs, cold air and sprays. [1] [2]
In the literature, cryotherapy (ice application) is described as an effective treatment for soft tissue injuries. [11] [12] [4] It reduces the swelling, and improves the range of motion[13]. However, there are still some doubts whether it is actually effective for chronic pain relief. The application of ice may be useful for a variety of musculoskeletal pains, yet the evidence for its efficacy should be established more convincingly. [14] [15]
Mechanism of Action[edit | edit source]
Skin blood flow is controlled by two branches of the sympathetic nervous system: a noradrenergic vasoconstrictor system and a cholinergic active vasodilator system. These dual sympathetic neural control mechanisms affect the major aspects of thermoregulatory responses over most of the human body’s surface.
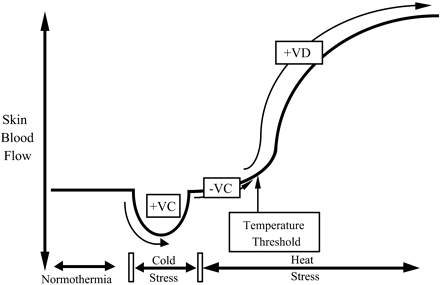
Figure 2:Skin blood flow responses to cold stress and heat stress. [5]
VC = vasoconstriction, VD = vasodilatation
During periods of hypothermia, falling core and skin temperatures lead to reflexive increases in sympathetic active vasoconstrictor nerve activity to reduce skin blood flow and conserve body heat. During periods of heat stress, increasing core and skin temperatures lead to reflexive increases in sympathetic active vasodilator nerve activity to increase skin blood flow.
The effect of heat on pain is mediated by heat sensitive calcium channels. These channels respond to heat by increasing intracellular calcium. This generates action potentials that increases stimulation of sensory nerves and causes the feeling of heat in the brain. These channels are part of a family of receptors called TRPV receptors. TRPV1 and TRPV2 channels are sensitive to noxious heat, while TRPV4 channels are sensitive to normal physiological heat. Their multiple binding sites allow a number of factors to activate these channels. Once activated, they can also inhibit the activity of purine pain receptors. These receptors, called P2X2 and P2Y2 receptors, are mediated pain receptors and are located in the peripheral small nerve endings. For example, with peripheral pain, heat can directly inhibit pain. However, when pain is originating from deep tissue, heat stimulates peripheral pain receptors which can alter what has been termed gating in the spinal cord and reduce deep pain.
Previous studies have suggested that temperature can affect the exchange between Ca2+ and Na+ in neural cells. They have documented an increase in both pain threshold (PTH) and pain tolerance (PTO) with the use of cooling. [16] [15] [5] [3]
Increased superficial tissue temperature results in the release of chemical mediators, such as histamine and prostaglandins, which result in vasodilation. These vasodilatory mechanisms do not significantly affect blood flow in skeletal muscle since skeletal muscle blood flow is heavily influenced by other physiologic and metabolic factors. Exercise is the best means to increase blood flow to skeletal muscle. [17] [7]
Treatment[edit | edit source]
Evidence surrounding the use of thermotherapy is mostly limited to the reduction of pain in conditions such as osteoarthritis, rheumatoid arthritis, primary dysmenorrhea and low back pain. [18][19][20][2]However, the use of those modalities can facilitate the efficacy of other treatments such as therapeutic exercises by reducing nociceptive signals and reducing joint stiffness (improved range of motion).
As for healing properties, the new guidelines suggest avoiding the use of thermotherapy during the stages of healing (see Peace and Love Principle). There are 4 phases of the healing process: the hemostasis phase, the inflammatory phase, the proliferation phase and the remodeling phase.[21]These phases hold their purposes and should only be altered in case of abnormal or extreme symptoms.
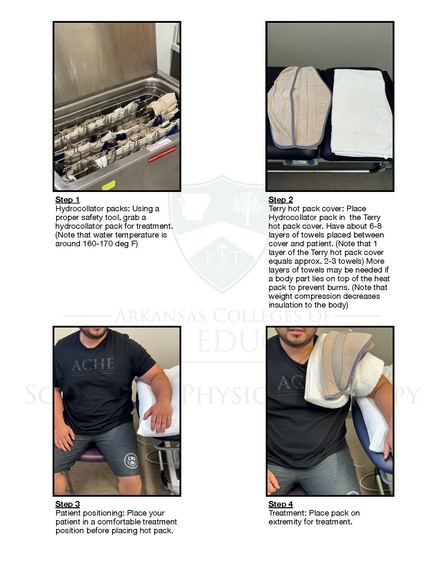
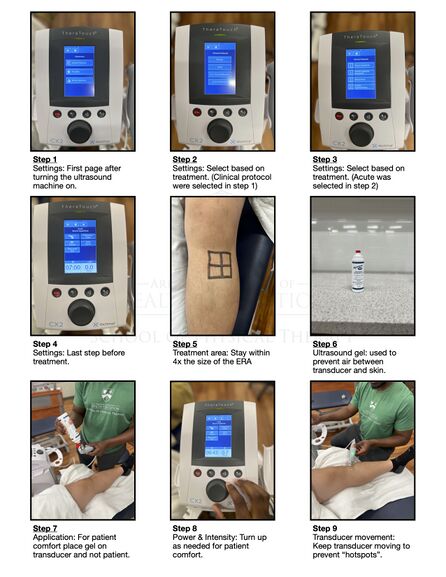
Below are instructions on how to use various thermotherapy modalities.
Physiological Effects[edit | edit source]
Many of the local physiologic effects of heat and cold have been studied thoroughly. For instance, heat increases skin and joint temperature, improves blood circulation and muscle relaxation and decreases joint stiffness. Cold numbs the pain, decreases swelling, constricts blood vessels and blocks nerve impulses to the joints. [23] [24] [2]
Deep heating is thought to lessen nerve sensitivity, increase blood flow, increase tissue metabolism, decrease muscle spindle sensitivity to stretch, cause muscle relaxation, and increase flexibility. Heat stimulates the cutaneous thermoreceptors that are connected to the cutaneous blood vessels, causing the release of bradykinin which relaxes the smooth muscle walls resulting in vasodilation. Muscle relaxation occurs as a result of a decreased firing rate of the gamma efferents, thus lowering the threshold of the muscle spindles and increasing afferent activity. There is also a decrease in firing of the alpha motor neuron to the extrafusal muscle fiber, resulting in muscle relaxation and decrease in muscle tone. [25] [26]
Indications, Precautions, Contraindications, and Adverse Effects[edit | edit source]
There are indications, precautions, contraindications, and adverse effects surrounding the use of thermotherapy, that needs to be taken with different clienteles such as children and older people (due to depleted temperature control capacities), and individuals with deprived sensations. Below are some indications, precautions, contraindications, and adverse effects for cryotherapy and thermotherapy. [1] [27]
Cold[edit | edit source]
Cryotherapy is indicated for various conditions including chronic pain, acute contusions, acute swelling, muscle spasms, and other things. Precautions should be taken to avoid tissue damage, nerve damage, and to help prevent frostbite. To help avoid the previous list, here are some precautions to consider: tissue damage may result when tissue temperature reaches 59 degrees F, frostbite may result if tissue temperature reaches below 39 degrees F. Contraindications to cryotherapy include conditions like sensory disorders, cold intolerance, and paroxysmal cold hemoglobinuria, where exposure could cause harm to the individual or an increase in symptoms. Adverse effects to cryotherapy could include any of the following: Tissue death due to prolonged vasoconstriction, ischemia, and thromboses in smaller vessels, tissue death from freezing, also appearance of wheals would indicate an adverse response to cryotherapy application.[22][28]
Heat[edit | edit source]
Indications:
- Subacute and chronic inflammatory condition
- Subacute or chronic pain
- Decreased range of motion
- Facilitate healing
- Muscle guarding
- Muscle spasm
- Myofascial trigger points
- Subacute muscle strain
- Subacute ligament sprain
Precautions:
- Pregnancy
- Impaired Circulation
- Cardiac Insufficiency
- Poor Thermal Regulation
- Edema
Contraindications:
- Acute musculoskeletal conditions
- Recent or potential hemorrhage
- Thrombosis
- Impaired sensation
- Impaired mentation
- Malignant tumor
- Infrared irradiation of the eyes
- Over an open wound
Adverse Effects:
Effectiveness[edit | edit source]
There are still contradictions whether the use of thermotherapy is effective or not. However, it is still used worldwide to reduce acute pain and improve mobility - where most of its evidence stands.
While there is good evidence that exercise relieves pain, improves function, and is cost-effective, evidence supporting the use of non-exercise physio-therapeutic interventions is much weaker. There is some support for the efficacy of thermotherapy, transcutaneous electrical neuromuscular stimulation (TENS), and massage, but there is little evidence to support the efficacy of electrotherapy, acupuncture or manual therapy.
For knee osteoarthritis (OA), ice massage is reported to improve joint mobility, pain and function; ice packs can reduce swelling and improve movement but may not relieve pain. In rheumatoid arthritis (RA), heat or cold packs are reported to have no effect on oedema, pain, movement, strength or function.
Cost effectiveness[edit | edit source]
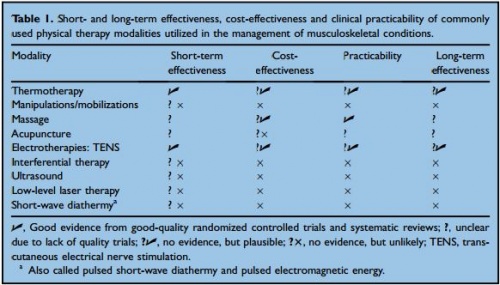
Despite conflicting evidence, the simple form of thermotherapy is widely recommended for many musculoskeletal conditions because it is a safe, effective, easy-to-apply and well-liked therapy based on anecdotal reports, expert opinion and patient preferences. Interventions that can be self-administered (thermotherapy, TENS, massage) are more likely to be cost-effective and less burdensome and hence much more attractive long-term management options. Complex thermal therapeutic modalities (heating deeper tissues) require special equipment, supervision and need to be delivered by a therapist, making them less accessible, more costly and higher risk.
Figure 3:Short- and long-term effectiveness, cost-effectiveness and clinical practicability of commonly
used physical therapy modalities utilized in the management of musculoskeletal conditions. [1]
level of evidence: 1C
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Hurley MV, Bearne LM. Non-exercise physical therapies for musculoskeletal conditions. Best Practice & Research Clinical Rheumatology. 2008 Jun 1;22(3):419-33.
- ↑ 2.0 2.1 2.2 2.3 Brosseau L, Yonge KA, Welch V, Marchand S, Judd M, Wells GA, Tugwell P. Thermotherapy for treatment of osteoarthritis. Cochrane Database of Systematic Reviews. 2003(4).
- ↑ 3.0 3.1 Petrofsky J, Berk L, Bains G, Khowailed IA, Hui T, Granado M, Laymon M, Lee H. Moist heat or dry heat for delayed onset muscle soreness. Journal of clinical medicine research. 2013 Dec;5(6):416.
- ↑ 4.0 4.1 4.2 Nadler SF, Weingand K, Kruse RJ. The physiologic basis and clinical applications of cryotherapy and thermotherapy for the pain practitioner. Pain physician. 2004 Jul 1;7(3):395-400.
- ↑ 5.0 5.1 5.2 Kellogg Jr DL. In vivo mechanisms of cutaneous vasodilation and vasoconstriction in humans during thermoregulatory challenges. Journal of applied physiology. 2006 May;100(5):1709-18.
- ↑ Hendee W.R., Physics of Thermal Therapy, Fundamentals and Clinical applications, By Taylor and Francis group, 2013.
- ↑ 7.0 7.1 Heinrichs K. Superficial thermal modalities. InCanine rehabilitation and physical therapy 2004 Jan 1. Saunders Elsevier, St Louis (MO).
- ↑ 8.0 8.1 Choi YJ, Lee HJ, Do Hyun Lee SY, Lee KH, Yun ST, Kim JM, Kim HJ, Kim JW. Therapeutic effects and immunomodulation of suanbo mineral water therapy in a murine model of atopic dermatitis. Annals of dermatology. 2013 Nov;25(4):462.
- ↑ Kamioka H, Tsutani K, Okuizumi H, Mutoh Y, Ohta M, Handa S, Okada S, Kitayuguchi J, Kamada M, Shiozawa N, Honda T. Effectiveness of aquatic exercise and balneotherapy: a summary of systematic reviews based on randomized controlled trials of water immersion therapies. Journal of epidemiology. 2010 Jan 5:0910270113-.
- ↑ Eversden L, Maggs F, Nightingale P, Jobanputra P. A pragmatic randomised controlled trial of hydrotherapy and land exercises on overall well being and quality of life in rheumatoid arthritis. BMC musculoskeletal disorders. 2007 Dec;8(1):1-7.
- ↑ Bleakley C, McDonough S, MacAuley D. The use of ice in the treatment of acute soft-tissue injury: a systematic review of randomized controlled trials. The American journal of sports medicine. 2004 Jan;32(1):251-61.
- ↑ Hubbard TJ, Denegar CR. Does cryotherapy improve outcomes with soft tissue injury?. Journal of athletic training. 2004 Jul;39(3):278.
- ↑ Adie, S., Kwan, A., Naylor, J. M., Harris, I. A., & Mittal, R. (2012). Cryotherapy following total knee replacement. The Cochrane database of systematic reviews, (9), CD007911. https://doi.org/10.1002/14651858.CD007911.pub2
- ↑ Ernst E, Fialka V. Ice freezes pain? A review of the clinical effectiveness of analgesic cold therapy. Journal of pain and symptom management. 1994 Jan 1;9(1):56-9.
- ↑ 15.0 15.1 Algafly AA, George KP. The effect of cryotherapy on nerve conduction velocity, pain threshold and pain tolerance. British journal of sports medicine. 2007 Jun 1;41(6):365-9.
- ↑ Holowatz LA, Thompson CS, Minson CT, Kenney WL. Mechanisms of acetylcholine‐mediated vasodilatation in young and aged human skin. The Journal of physiology. 2005 Mar;563(3):965-73.
- ↑ Swenson, C., Swärd, L., & Karlsson, J. (1996). Cryotherapy in sports medicine. Scandinavian journal of medicine & science in sports, 6(4), 193–200. https://doi.org/10.1111/j.1600-0838.1996.tb00090.x
- ↑ Jo, J., & Lee, S. H. (2018). Heat therapy for primary dysmenorrhea: A systematic review and meta-analysis of its effects on pain relief and quality of life. Scientific reports, 8(1), 16252. https://doi.org/10.1038/s41598-018-34303-z
- ↑ Freiwald, J., Hoppe, M. W., Beermann, W., Krajewski, J., & Baumgart, C. (2018). Effects of supplemental heat therapy in multimodal treated chronic low back pain patients on strength and flexibility. Clinical biomechanics (Bristol, Avon), 57, 107–113. https://doi.org/10.1016/j.clinbiomech.2018.06.008
- ↑ Robinson, V., Brosseau, L., Casimiro, L., Judd, M., Shea, B., Wells, G., & Tugwell, P. (2002). Thermotherapy for treating rheumatoid arthritis. The Cochrane database of systematic reviews, (1), CD002826. https://doi.org/10.1002/14651858.CD002826
- ↑ Wound Source. Wound Healing. Available from:https://www.woundsource.com/blog/four-stages-wound-healing
- ↑ 22.0 22.1 22.2 Prentice W.E. Cryotherapy and thermotherapy. Therapeutic Modalities in Rehabilitation, 5e. McGraw-Hill Education. 2017;(9):336-436
- ↑ Sluka KA, Christy MR, Peterson WL, Rudd SL, Troy SM. Reduction of pain-related behaviors with either cold or heat treatment in an animal model of acute arthritis. Archives of physical medicine and rehabilitation. 1999 Mar 1;80(3):313-7.
- ↑ Oosterveld FG, Rasker JJ. Effects of local heat and cold treatment on surface and articular temperature of arthritic knees. Arthritis & Rheumatism: Official Journal of the American College of Rheumatology. 1994 Nov;37(11):1578-82.
- ↑ Prentice Jr WE. An electromyographic analysis of the effectiveness of heat or cold and stretching for inducing relaxation in injured muscle. Journal of Orthopaedic & Sports Physical Therapy. 1982 Jan 1;3(3):133-40.
- ↑ Peres SE, Draper DO, Knight KL, Ricard MD. Pulsed shortwave diathermy and prolonged long-duration stretching increase dorsiflexion range of motion more than identical stretching without diathermy. Journal of athletic training. 2002 Jan;37(1):43.
- ↑ Oosterveld FG, Rasker JJ. Treating arthritis with locally applied heat or cold. InSeminars in arthritis and rheumatism 1994 Oct 1 (Vol. 24, No. 2, pp. 82-90). WB Saunders.
- ↑ 28.0 28.1 Cameron MH. Physical Agents in Rehabilitation. 6e. Elsevier Health Sciences; 2021.p.123-223