TNM Staging System
Original Editor - Riccardo Ugrin
Top Contributors - Riccardo Ugrin, Kim Jackson and Sehriban Ozmen
Introduction[edit | edit source]
Staging a tumor is the process of finding out the cancer in a patient. A cancer’s stage can also be used to help predict the course of the cancer, as well as how likely it is that treatment will be successful. It is used in almost every oncological patient to describe the tumor, regardless of the localisation of the primary cancer.
In most cases the biopsy exam do not modified the TNM[1] stage system: infact the biopsy finds out if a disease is present and, if so, it precisely and accurately classifies the disease according to the cells differentiation. TNM system could stage both benign or malign tumors. Because of that in case of benign tumors, the N and M letters would be follow by 0.
In the TNM system, the overall stage is determined after the cancer is assigned a letter or number to describe the tumor (T), node (N), and distant metastasis (M) categories[2].
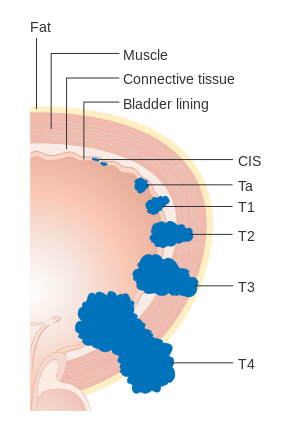
T: Tumor Size[edit | edit source]
T describes the original (primary) tumor. The T determine the size of the tumor according to the physical assessment or imaging and endoscopy exams.
- TX means there’s no information about the primary tumor, or it can’t be measured.
- T0 means there is no evidence of a primary tumor (it cannot be found).
- Tis means that the cancer cells are only growing in the layer of cells where they started, without growing into deeper layers. This may also be called in situ cancer or pre-cancer.
- T1-T4 describe the size and/or the extension of the tumor. The higher the T number, the larger the tumor and/or the more it has grown into nearby tissues.
N: Lymph Nodes[edit | edit source]
N describes the degree of spread to regional lymph nodes. The N describe the size, location, and/or the number of nearby lymph nodes affected by cancer. The higher the N number, the greater the cancer spread to nearby lymph nodes.
- Nx: lymph nodes cannot be assessed
- N0: no regional lymph nodes metastasis
- N1: regional lymph node metastasis present; at some sites, tumor spread to closest or small number of regional lymph nodes
- N2: tumor spread to an extent between N1 and N3 (N2 is not used at all sites)
- N3: tumor spread to more distant or numerous regional lymph nodes (N3 is not used at all sites)
M: Metastasis[edit | edit source]
M describes the presence of distant metastasis in other parts of the body. If the tumor spread to other organs the malignacy of the tumor is higher and indicates a negative prognostic factor. The M describes only the presence or the absence of distant metastasis:
- M0: no distant metastasis
- M1: metastasis to distant organs (beyond regional lymph nodes)
The Mx designation was removed from the 7th edition of the AJCC/UICC system, but referred to cancers that could not be evaluated for distant metastasis.
TNM reassessment[edit | edit source]
The cancer stage is also a way for doctors to describe the extent of the cancer and the aggravation during time. When a cancer is staged again after the initial staging, it is sometimes referred to as restaging. Infact the first clinical stage (cTNM) is often reassessed by the surgeon during surgery. Because of that the new reassessement is called the pathological stage (pTNM). The uTNM stage is determined by ultrasonography or endosonography.
Other reassessment of the TNM staging are made in case of radiotherapy or chemotherapy. In case of adjuvant therapy the ycTNM defines the stage after the radiotherapy or chemotherapy but before surgery. If the patient underwent surgery after the adjuvant therapy, the TNM stadiation is referred to ypTNM.
In case of secondary tumors or relapsed cancers the staging is added to the previous primary classification. It is defined as rTNM when its new stadiation is only clinical, or rpTNM when the new stadiation had a pathological examination. Ther mTNM tumor staging is a multifocal cancer(more than 1 tumors).
The TNM staging system could also be used for an autopsy re-examination of the cancer. In that cases is defined as aTNM.
Other parameters[edit | edit source]
For most cancers other factors could be included in the stadiation process. The better treatment option for the patient could be determined also by the grade of differentiation of the tumor's cells or by the spread of the tumor in vassels. Because of that other parameters can be used:
- G: describes the grade of differentiation of the cancer cells. In lower grade (G1-G2) cancers, the cancer cells look well-differentiated under the microscope. In general, these low-grade cancers tend to grow slowly and often have a better prognosis. In higher grade (G3-G4) cancer the cells look poorly differentiated and more abnormal. High-grade cancers often tend to grow quickly and have higher malignacy, so it may be needed different treatments options than low-grade cancers.
- S (0–3): elevation of serum tumor markers. Some tumors with high blood antigenic markers can be defined during the stadiation process. For example, the level of prostate-specific antigen (PSA) in the blood is taken into account in assigning a stage in prostate cancer.
- R (0–2): describes the completeness of the operation. Free surgical margins are the main oncological prognostic factor in patients underwent surgery.
Other specific parameters in lymphoma or blood cancer:
- L (0–1): invasion into lymphatic vessels
- V (0–2): invasion into vein (no, microscopic, macroscopic)
Examples[edit | edit source]
| Stage of the tumor | TNM |
|---|---|
| STAGE 0 | Tumor in situ |
| STAGE I | T1-2 N0 M0 |
| STAGE II | T1-2 N1 M0
T3 N0 M0 |
| STAGE III | T1-2 N2-3 M0
T3 N1-3 M0 T4 N0-3 M0 |
| STAGE IV | T1-4 N0-3 M1
(or every cancer with distant metastasis) |
References[edit | edit source]
- ↑ Lydiatt WM, Patel SG, O'Sullivan B, Brandwein MS, Ridge JA, Migliacci JC, et al. . "Head and Neck cancers-major changes in the American Joint Committee on cancer eighth edition cancer staging manual". CA: A Cancer Journal for Clinicians. 2017; 67 (2): 122–137
- ↑ American Cancer Society. Overview: Testicular Cancer, What is Testicular Cancer? American Cancer Society, Inc.; 2009-08-28; 2010-02. Available from: http://www.cancer.org/docroot/CRI/content/CRI_2_2_1x_What_Is_Testicular_Cancer_41.asp?sitearea=