Syphilis
Original Editor - Chelsea McLene
Top Contributors - Chelsea Mclene, Lucinda hampton and Nupur Smit Shah
Introduction[edit | edit source]
Syphilis is a contemporary plague that continues to afflict millions of people worldwide. The infection progresses through 4 stages and can affect many organ systems.
Syphilis:
- A highly contagious sexually transmitted infection (STI) infection caused by the bacteria spirochete Treponema pallidum.
- Usually spread through contact with infectious sores on the genitals, anus, rectum, lips or mouth, via blood transfusion, or through mother-to-child transmission during pregnancy.
- Correct and consistent use of condoms significantly decreases the risk of infection.
- Mother-to-child transmission of syphilis (congenital syphilis) is preventable and can be achieved through early screening and treatment.
Uncomplicated syphilis can be easily cured with antibiotics, however if left untreated, the disease last for years and cause serious health problems.[1][2].
- Syphilis is only spread through direct contact with syphilitic chancres.
- It can’t be transmitted by sharing a toilet with another person, wearing another person’s clothing, or using another person’s eating utensils.[3]
- To read about the history of syphilis, click here.
Epidemiology[edit | edit source]
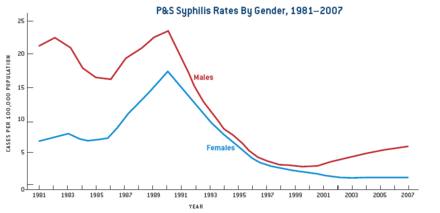
Syphilis continues to cause morbidity and mortality worldwide. While syphilis infection is easily identifiable and treatable, rates of syphilis infection continue to increase among select populations in high-income countries and remain at endemic levels in low- and middle-income counties.
- In 2016, the World Health Organization (WHO) released a new strategy to combat sexually transmitted infections (STIs) from 2016 to 2021. The strategy prioritizes the elimination of congenital syphilis by implementing comprehensive syphilis screening and treatment among pregnant women, as well as in specific populations.
- Despite prior efforts to eliminate syphilis in high-income countries, budget reductions in STI programs and public health surveillance systems have undermined previous elimination and control efforts.
- In Western Europe, the USA, and China, large increases in syphilis have been seen among key populations.
- Key populations are disproportionally affected, and continue to exhibit a high burden of syphilis, which ranges from 1% to 27% in the case of gay men and other men who have sex with men (MSM), and from 0.5% to 14% in female sex workers
- Untreated syphilis increases the risk of transmitting or acquiring HIV by two or three times in some populations[1]
- In low- and middle-income countries (LMICs) , syphilis has remained endemic[5]
Etiology[edit | edit source]
Treponema pallidum was identified as the agent that causes syphilis in 1905. The only host for the organisms are humans, and there is no animal reservoir. Syphilis is considered a sexually transmitted disease, as most cases of syphilis are transmitted through vaginal, anogenital, and orogenital contact. The infection can rarely be acquired via nonsexual contact, such as skin-to-skin contact or via blood transfer (blood transfusion or needle sharing). Vertical transmission occurs transplacentally, resulting in congenital syphilis[2].
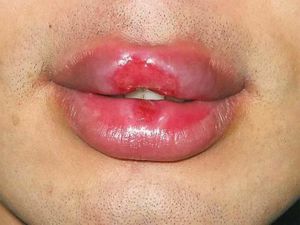
Image 3: Chancre Syphilitic
How It Spreads[edit | edit source]
- By having unprotected vaginal, anal or oral sex.
- By blood products (unclean needles or unscreened blood).
- By mother to baby by pregnancy, labor or nursing.[3]
- can spread during practice of dentistry by direct contact with the mucosal lesions.[6]
Stages and Symptoms[edit | edit source]
There are 4 [4]stages:
- Primary
- Secondary
- Latent
- Tertiary
- Primary syphilis: appears 10 to 90 days after exposure to the infection and comprises a painless, indurated ulcer (chancre) at the site of inoculation with the T. pallidum. HIV patients usually develop multiple chancres. These lesions resolve without treatment in 3-6 weeks. Regional lymphadenopathy is common and consists of rubbery lymph nodes.
- Secondary syphilis: appears 2 to 8 weeks after the disappearance of the chancre and has multiple systemic manifestations that can involve any system and body part. The cutaneous manifestations are also varied (condyloma lata, alopecia, mucous patches, palmar or truncal rash, papulosquamous rash) and because they contain a high load of spirochetes, these lesions are highly contagious.
- Latent syphilis: Untreated primary or secondary syphilis is followed by an early latent phase (one year or less later on) or late latent phase (over 1 year) and is characterized by positive serologic tests, but negative clinical manifestations.
- Tertiary syphilis: late symptomatic syphilis that can manifest months or years after the initial infection as cardiovascular syphilis (an aortic aneurysm, aortic valvulopathy), neurosyphilis (meningitis, hemiplegia, stroke, aphasia, seizures, tabes dorsalis), or gummatous syphilis (infiltration of any organ and its subsequent destruction).
Congenital syphilis: results from transplacental transmission or contact with the infectious lesions during birth and can be acquired at any stage, causing stillbirth or neonate congenital infection. There are many presentations of congenital syphilis, including nasal cartilage destruction (saddle nose), frontal bossing (olympian brow), bowing of the tibia (saber shins), morbilliform rash, rhinitis (snuffles), sterile joint effusion (Clutton joints), peg-shaped upper central incisors (Hutchinson teeth). Many of the neonates born with congenital syphilis are asymptomatic at birth. Early signs can manifest up to 48 months as rash, hepatosplenomegaly, fever, bulging fontanels, seizures, or cranial nerve palsies. Those untreated neonates enter a latent period. Routine screening is recommended at the first prenatal visit and during the third trimester and delivery in high-risk women[2].
Diagnosis[edit | edit source]
Syphilis is easy to detect using:
- a simple blood test
- a swab test – if there are sores present.
The tests ordered are:
Treponemal Test and Non Treponemal Test
- This test is an antibody test and it is done by collecting a sample of the blood from a vein. In the case of syphilis, the most common tests that are used are the nontreponemal antibody test and the treponemal antibody test. In most cases, a positive result from one test is followed by the other so that confirmation of the disease can be made. The nontreponemal antibodies are not specifically directed at the Treponema pallidum bacterium.
- Conditions like pregnancy, Lyme disease, certain types of pneumonia, malaria, tuberculosis, and lupus can generate false-positive results. The Treponemal antibody tests are more specifically directed at the syphilis bacteria and more accurate. But once these antibodies are formed, they remain in the blood for a lifetime and a positive result in the test may not indicate an active state of the disease.[7][8][9][10]
Prevention[edit | edit source]
Syphilis spreads only from sexual contact with someone who has it. So the best way to avoid syphilis and other STDs is to not have vaginal, anal, or oral sex at all.
- always use condoms with water based lubricant during sex.
- always use dental dams for oral sex.
- limit the number of people you have sex with, or just have sex with one partner who isn’t already infected.
- avoid sex with someone infected with syphilis or who has symptoms of syphilis until they have finished treatment.
- have regular STI check-ups.[8][11]
Prognosis[edit | edit source]
The prognosis of syphilis depends on the stage and extent of organ involvement. If left untreated, the organism has significant morbidity and mortality. Patients usually develop cardiovascular and CNS syphilis, which are fatal. Congenital syphilis is associated with spontaneous abortions, stillbirth, and fulminant pulmonary hemorrhage in neonates. Without treatment during pregnancy, syphilis is almost always passed on to the fetus.[2]
Treatment[edit | edit source]
Treatment depends on the disease stage. It can usually be treated with a short course of antibiotics.[8]
- Primary, secondary, or early latent syphilis is treated with a single dose of intramuscular (IM) penicillin G benzathine 2.4 million units.
- Late latent syphilis is treated with IM penicillin G benzathine 2.4 million units once weekly for 3 weeks.
- Tertiary syphilis is treated with IM penicillin G benzathine 2.4 million units once weekly for 3 weeks.
- Neurosyphilis is treated IV penicillin G aqueous 18-24 million units daily for 10 to 14 days[2].
If allergic to penicillin, doxycycline or tetracycline can be administered.[12][13]
Infected person must stop having sex until he is completely healed and the partner must also be treated for the same.
Treatment Guidelines[edit | edit source]
- WHO Guidelines on the Treatment of Syphilis by the World Health Organization
- 2015 STD Treatment Guidelines
- Syphilis During Pregnancy
- Congenital Syphilis
- Clinical Advisory: Ocular Syphilis in the United States
- STD and Pregnancy
- Syphilis treatment protocol
Physiotherapy[edit | edit source]
Patient education is vital, and counsel patients against the use of IV drugs or use clean needles or refer on to relevant professional. eg
- Health nurse to educate on safe sex practices and the importance of regular screening for sexually transmitted diseases. The use of barrier protection (condom) is highly recommended.
- The pharmacist should educate the patient that there are effective treatments for STDs, and the earlier the condition is treated, the better the outcomes.
Only through close collaboration with an interprofessional team can the morbidity of infections like syphilis be lowered.
The outlook for most patients who are compliant with treatment is good, but those who delay or fail to comply with treatment can develop life-threatening complications[2].
References[edit | edit source]
- ↑ 1.0 1.1 PAHO Syphilis Available from:https://www.paho.org/hq/index.php?option=com_content&view=article&id=14869:sti-syphilis&Itemid=3670&lang=en (accessed 13.4.2021)
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Tudor ME, Al Aboud AM, Gossman WG, Haddad LM. Syphilis (Nursing).Available from:https://www.ncbi.nlm.nih.gov/books/NBK534780/ (accessed 13.4.2021)
- ↑ 3.0 3.1 LaFond RE, Lukehart SA. Biological basis for syphilis. Clinical microbiology reviews. 2006 Jan 1;19(1):29-49.
- ↑ 4.0 4.1 Khanacademymedicine. What is syphilis? Available from: http://www.youtube.com/watch?v=IE9hAzVAGeY[last accessed 23/3/2021]
- ↑ Kojima N, Klausner JD. An update on the global epidemiology of syphilis. Current epidemiology reports. 2018 Mar;5(1):24-38.Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6089383/ (accessed 13.4.2021)
- ↑ Little JW. Syphilis: an update. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology. 2005 Jul 1;100(1):3-9.
- ↑ Dr Fact TPAB test Available from:https://factdr.com/diagnostics/blood-tests/treponema-pallidum-antibody-tpab/ (accessed 13.4.2021)
- ↑ 8.0 8.1 8.2 8.3 Raja Narayan. Diagnosis, Treatment, and Prevention of Syphilis. Available from https://www.youtube.com/watch?v=b2twF_jDSQM[last accessed 23/3/2021]
- ↑ Kenyon C, Lynen L, Florence E, Caluwaerts S, Vandenbruaene M, Apers L, Soentjens P, Van Esbroeck M, Bottieau E. Syphilis reinfections pose problems for syphilis diagnosis in Antwerp, Belgium–1992 to 2012. Eurosurveillance. 2014 Nov 13;19(45):20958.
- ↑ Lautenschlager S. Diagnosis of syphilis: clinical and laboratory problems. JDDG: Journal der Deutschen Dermatologischen Gesellschaft. 2006 Dec;4(12):1058-75.
- ↑ Schmid G. Economic and programmatic aspects of congenital syphilis prevention. Bulletin of the World Health Organization. 2004;82:402-9.
- ↑ Clement ME, Okeke NL, Hicks CB. Treatment of syphilis: a systematic review. Jama. 2014 Nov 12;312(18):1905-17.
- ↑ Alexander JM, Sheffield JS, Sanchez PJ, Mayfield J, Wendel Jr GD. Efficacy of treatment for syphilis in pregnancy. Obstetrics & Gynecology. 1999 Jan 1;93(1):5-8.