Stanmore Classification of Shoulder Instability
Original Editors - Ammar Suhail
Top Contributors - Ammar Suhail and Christopher Nyunt
Introduction[edit | edit source]
Shoulder instability is the symptomatic abnormal motion of the glenohumeral joint (GHJ), which can present as pain or a sense of displacement either as a subluxation or a dislocation. The patient usually reports abnormal motions and sense of apprehension while doing Activities of daily living (ADLs). Shoulder being a mobile joint has a high predisposition for Instability.[1]
Classification[2][edit | edit source]
The classification suggests that for the symptoms to occur there has to be a disturbance of one or more of the following factors, in isolation or together:
- the capsulolabral complex and its proprioceptive mechanism
- the rotator cuff
- the surface arc or area of contact between the glenoid and humeral head
- the central/peripheral nervous system.
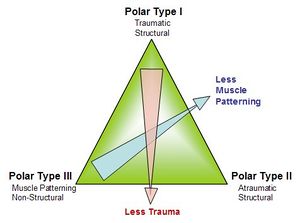
Stanmore classification system proposes three types of shoulder instability recognising the structural and non-structural components and that a continuum exists between pathologies. The concept of instability being caused by a combination of structural (traumatic and atraumatic) and neurological system disturbances has led to the classification of instability as a continuum of pathologies. The system also proposes that direction of instability is not as relevant to effective management as whether the instability is structural, non-structural or both The following are the three different forms of Instabilities according to Jaggi and Lambert, 2010 (Stanmore Classification):
- Polar Type I (Structural Instability)
- Polar Type II (Atraumatic Instability)
- Polar Type III (neurological dysfunctional or muscle patterning)
Clinical Presentation[edit | edit source]
Polar Group I[edit | edit source]
These group patients usually present with a positive apprehension (anterior direction) associated with rotator cuff weakness. Subscapularis shows deficits on either the belly-press or modified lift-off tests [3]. Global posture, single leg balance and scapular control are often undisturbed in these patients[2]. As these patients move towards either the type II or III poles, patients begin to exhibit signs of poor scapular control, abnormal muscle activation, altered trunk stability and balance, indicating non-structural comorbidity. The imaging is only used in cases suspected of structural abnormality. Arthroscopy is useful to look for the subtleties of internal lesions of occult instability, such as bicipital and deep surface cuff lesions, soft tissue Broca defects, internal impingement and external impingement lesions.
Polar Group II[edit | edit source]
Patients in this group present with positive anterior apprehension test with signs of increased capsular laxity, excessive external rotation and a sulcus sign. There may also be an associated glenohumeral internal rotation deficit (GIRD). The abnormal anterior translation of the GHJ within this group can be due to a combination of several factors: excessive anterior capsular laxity, scapular dyskinesis, tight posterior capsule, muscular imbalance (increased ratio of internal rotator/external rotator strength) and congenital labral pathology. The Presentation usually varies in individuals from different sports[2].
Polar Group III[edit | edit source]
Patients lying in this spectrum of the pathology shows aberrant activation large muscles and simultaneous suppression of the rotator cuff. Dynamic EMG has characterised latissimus dorsi, pectoralis major and anterior deltoid among the large muscles, and only infraspinatus of the rotator cuff. If there is no clinically or electrophysiologically proven aberrant muscle activation then the condition is labelled type II. Polar III patients will have a history of ‘party tricking’ the shoulder. This will often occur in the midranges of movement or with the arm-dependent by the side indicating a muscular control problem. These patients need a thorough assessment of the muscle activation pattern as well as the resting position of the GHJ (Glenohumeral Joint)[2].
References[edit | edit source]
- ↑ Kim SH, Ha KI, Jung MW, et al. Accelerated rehabilitation after arthroscopic Bankart repair for selected cases: a prospective randomized clinical study. Arthroscopy 2003;19:722–31.
- ↑ 2.0 2.1 2.2 2.3 Jaggi A, Lambert S. Rehabilitation for shoulder instability. British journal of sports medicine. 2010 Apr 1;44(5):333-40.
- ↑ Tennent TD, Beach WR, Meyers JF. A review of the special tests associated with shoulder examination. Part II: laxity, instability, and superior labral anterior and posterior (SLAP) lesions. Am J Sports Med 2003;31:301–7