Spinothalamic tract
Original Editor - Matt Ross
Top Contributors - Matt Ross, Kate Sampson, Aminat Abolade, Kim Jackson, Amanda Ager, Lucinda hampton and WikiSysop
Description[edit | edit source]
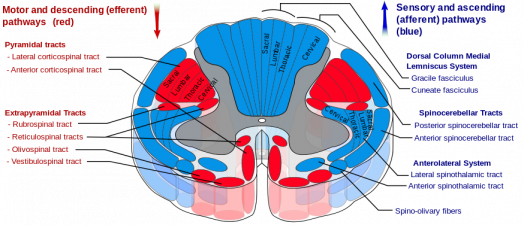
Information from the trunk and limbs is carried to the sensory cortex and the cerebellum. Two systems ascend to the cerebral cortex, the dorsal column-medial lemniscal (DCML) system and the anterolateral (AL) system. These paralleled ascending systems each relay different information, however, there remains redundancy between the two pathways. The anterolateral system consists of the
i) spinothalamic tract
ii) spinoreticular tract and
iii) spinomesencephalic tract.
These tracts (fibers) cross over upon entering the spinal cord and ascend to the brainstem centers.
The spinothalamic tract, one of the most important pathways of the nervous system, lies anteriolaterally to the ventral horn of the spinal grey matter. This pathway comprises of three neutron sets and forms part of the somatosensory system.
1st Order Neurones[edit | edit source]
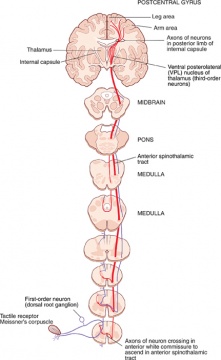
These neurones carry information regarding pain, thermal sensation, course touch and pressure. These primary afferent neurones, also known as nociceptive neurones (read more about nociception), are specialised neurones that can be divided into 4 main modalities; mechanonociceptors (Pressure), Thermal Nociceptors, Chemically sensitive nociceptors or polymodal nociceptors. Their cell bodies reside in the dorsal root ganglion, and synapse onto second order neurones located within the posterior grey horn of the spinal cord[1].
2nd Order Neurones[edit | edit source]
The cell bodies of the second order neurones lie within the posterior grey horn of the spinal cord. Once the second order neurones have synapsed with the first order neurones, they decussate via the ventral commissar at their respective segmental level. The second order neurones now ascend up the spinal cord anteriolaterally now known as the spinothalamic tract - those neurones from the lower spinal cord are more dorsal and lateral while the more rostral levels are ventral and medial. As it enters the region of the head it is joined by the trigeminal afferents as well as accompanying the medial lemniscus pathway. The second order neurones then synapse with the third order neurones in the ventral posterior nucleus of the thalamus [1] [2]
3rd Order Neurones[edit | edit source]
The third order neurones then project from the thalamus to the primary somatosensory cortex (Brodman areas 3, 1 and 2)
Function[edit | edit source]
As previously mentioned, the spinothalamic tract is an afferent sensory pathway and has no motor function. The sensory signal that is sent from the 1st order (nociceptive neurone) depends on what nociceptive fibre was activated [3].
Mechanoreceptors[edit | edit source]
Stimuli are transmitted via the thinly myelinated fast transmitting A Delta fibres. These nociceptors respond to pressure and tissue damaging stimuli.
Thermal Nociceptors[edit | edit source]
Stimuli are carried via the unmyelinated, slow conduction C fibres and are activated when the temperature exceeds 45 degrees.
Chemically Sensitive Nociceptors[edit | edit source]
Like thermal nociceptors, the stimuli are transmitted via the slow conducting C-Fibres. These are activated in response to aligns, pH and irritants.
Polymodal Nociceptors[edit | edit source]
These are the most abundant nociceptor and respond to thermal, mechanical and chemical stimuli. information is also carried via the slow conducting C-fibres.
Clinical relevance[edit | edit source]
The spinothalamic tract can be comprised anywhere along the length of its ascension to the cortex.
peripheral neuropathy[edit | edit source]
Peripheral neuropathy, seen as symmetrical damage to peripheral nerves is relatively common and is usually a result of either toxic, metabolic, inflammatory or infectious causes. Most commonly this is seen in patients with diabetes. Initially, symptoms, in this case, are commonly sensory loss and those nerves which are longest, particularly those that transmit stimuli from the lower limb are affected first later producing the 'stocking-glove' distribution.
Whilst vibration sense is usually the first to be affected, pin-prick, temperature and light touch soon follow.
Radiculopathy[edit | edit source]
Commonly as a result of disk herniation onto a nerve root, the patient will commonly complain of pins and needles and there will only be slight sensory loss due to the vast overlapping nature of the dermatomes.
The sensory loss will usually follow a dermatomal pattern, reflecting the segmental level at which the herniation is occurring.
Spinal Cord[edit | edit source]
Both sensory and motor impairments are witnessed in spinal cord injuries as a result of an insult on both ascending and descending tracts. Sensation is usually affected below the point at which the spinal cord has been damaged. In spinal cord injury patients, the ASIA scale is commonly used to diagnose the severity.
Damage to the spinothalamic tract within the spinal cord, as seen in Brown-Séquard syndrome, results in contralateral loss of pain and temperature whilst vibration and proprioception, transmitted via the dorsal columns, will be affected ipsilaterally.
Cerebral Cortex[edit | edit source]
Cortical lesions, particularly if they have occurred within the parietal lobe, may affect stereognosis and graphesthesia with minimal deficits in pain, temperature and light touch perception. However, this will vary on the size of the lesion.
chronic pain[edit | edit source]
Although further information regarding chronic pain can be read here, it is worth noting that the cell origin within the dorsal horn of the spinal cord receives both inhibitory and excitatory synapses from neurones that lie within the substantia gelatinosa which is important in regulating the pain experience. There is a large evidence base that highlights the link between psychosocial factors (anxiety, depression) that increases the patient's experience of pain.
Assessment[edit | edit source]
The integrity of the spinothalamic tract should be assessed along with other spinal tracts within a neurological assessment. A detailed subjective examination will be required, allowing the patient to describe any sensory deficits they are currently experiencing. When these tests are being performed, the patient should have their eyes closed with comparisons of the left and right sides taking place.
- Pain: Can be examined using neurotips or safety pin, assessing various aspects of the limb comparing left and right. These objects have both a sharp and blunt end, and asking whether the patient is experiencing either sharp or dull pain allows the clinician insight into their ability to discriminate between the two.
- Temperature: Can be examined by using two tubes; one with warm water and one with cold. Testing various aspects of the limb and comparing left to right, can they differentiate between hot and cold?
- Crude Touch: Using cotton wool / a piece of paper towel touch various parts of their extremities again comparing left to right. Ask whether or not they can feel you touching them and if so can they tell you where you are touching them?
Treatment[edit | edit source]
Sensory re-education with various different stimuli to help try to reinforce the sensory pathways that have been damaged.
Resources[edit | edit source]
| [6] | [7] |
References[edit | edit source]
- ↑ 1.0 1.1 Tortora, G.J. and Derrickson, B. (2011). Principles of Anatomy and Physiology. 13th Edition. John Wiley and Sons Inc.
- ↑ Crossman, A.R. and Neary, D. (2015). Neuroanatomy an Illustrated Colour Text. 5th Edition. Churchill Livingstone.
- ↑ Mtui, E., Gruener, G. and Dockery, P. (2016). Fitzgeralds Clinical Neuroanatomy and Neuroscience. 7th Edition. Elsevier. Philadelphia, USA.
- ↑ Merck Manuals. How to do the Sensory Exam | Merck Manual Professional Version. Available from:https://www.youtube.com/watch?v=YDfDG6kgqcE [last accessed 8/7/2022]
- ↑ The Florey Institute of Neuroscience and Mental Health. SENSe: Study of the Effectiveness of Neurorehabilitation on Sensation. Available from:https://www.youtube.com/watch?v=mKkoWCacbgQ [last accessed 8/7/2022]
- ↑ Neuroscientifically Challenged. 2-Minute Neuroscience: Pain and the Anterolateral System. Available from:https://www.youtube.com/watch?v=gcOqv0uzyAQ[last accessed 8/7/2022]
- ↑ Handwritten Tutorials. Spinal Pathways 1 - Spinal Cord Anatomy and Organisation. Available from:https://www.youtube.com/watch?v=5B87zsAKmWc[last accessed 8/7/2022]
- ↑ Handwritten Tutorials. Spinal Pathways 3 - Spinothalamic Tract. Available from:https://www.youtube.com/watch?v=QpoEh9VQ7so[last accessed 8/7/2022]