Skin Microbiome
Original Editor - Oyemi Sillo
Top Contributors - Oyemi Sillo and Aminat Abolade
Introduction[edit | edit source]
The skin is the largest organ of the human body and it serves as a physical barrier that protects the body from invasion by foreign organisms.[1] The skin is colonized by millions of microorganisms, which make up the skin microbiome. These include bacteria, fungi, viruses, and mites. As with the gut, the microbiome of the skin plays a role in immunity, healing and health.
Composition of the Skin Microbiome[edit | edit source]
The composition of the skin microbiome varies among individuals and between body parts, and it is influenced by several intrinsic and extrinsic factors.[1]
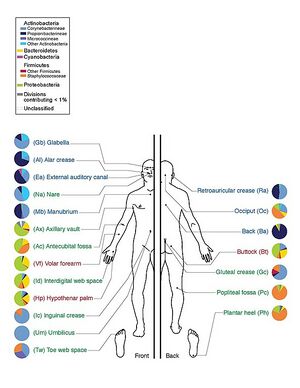
The site of the skin significantly influences the composition of microorganisms; for example, the arm was observed to have a greater diversity of microbial species than the scalp or axilla.[3] Also, Staphylococci and Propionibacteria species are the most prevalent at oily skin sites, Corynebacteria species predominate moist sites with some representation of Staphylococci species, and dry sites have a mixed population of bacteria but β-Proteobacteria and Flavobacteriales are the most prevalent.[4]Ethnicity is another intrinsic factor that has been found to influence variations in skin microbiome.[3][5] Gender may also influence the composition of skin microbiome at specific ages and skin sites due to the physiological variations between male and female skin environments, such as hormone metabolism, perspiration rate, and skin surface pH.[6]Aging is another factor that influences the skin microbiome composition, due to skin changes (e.g. changes to sebaceous gland activity) that affect the ecological conditions of the skin.[7]
The extrinsic factors that influence the composition of the skin microbiome include the delivery mode during childbirth;[8] the type of living environment, including the presence of domestic animals;[9][10] [11] the use of hygiene and cosmetic products;[12] and geographical factors like climate, seasons, and levels of pollution and radiation.[13][14] Also, the use of oral and topical antibiotics have been found to alter skin microbiome composition.[15] [16]
Aside from host factors, interactions between microorganisms also influence the composition and function of the skin microbiome. Microbial interactions can be competitive, where the presence of one diminishes the presence of another, or synergistic, where their presence is mutually beneficial. For instance, Staphylococcus aureus colonizes the nostrils of about a third of the population and is harmless most of the time, however, it is a major risk factor for serious infection. Certain strains of Staphylococcus epidermidis have been reported to inhibit S. aureus colonization.[17]
Role of Skin Microbiome on Immunity[edit | edit source]
The skin microbiome helps to prime the cells of the immune system for response to attacks by pathogens.[1] Commensal microorganisms interact closely with the host immune cells, training T cells to respond to potential pathogen.[18] Staphylococcus epidermidis colonizes the skin during the neonatal period, possibly establishing immune tolerance by the accumulation of commensal-specific regulatory T cells following another exposure later in life.[19] Current evidence suggests that disease states are the results of microbial dysbiosis, which lead to aberrant immune responses both locally and systemically.[20] Atopic Dermatitis is an immune-mediated inflammatory disease of the skin, in which commensal bacteria of the Staphylococcus species - particularly Staphylococcus aureus - are implicated.[20]P. acnes is a commensal skin bacterium that is associated with acne, while Malassezia spp. are skin fungi that are associated with seborrhoeic dermatitis.[1]
Role of Skin Microbiome on Wound Healing[edit | edit source]
The skin microbiome has been found to play a role in wound healing. Staphylococcus epidermidis produces a secretion that reduces inflammation and speeds wound healing by binding to an immune-system receptor. There have been a lot of research into the role of the skin microbiome in the healing of chronic wounds, especially in people with diabetes. People with poorly controlled glucose levels have relatively greater abundance of Staphylococcus spp. and Streptococcus spp. Colonization. Also, studies have shown that more than half of diabetic foot ulcers are infected, with associations between the clinical features and the colonizing bacterial communities. For instance, Staphylococcus spp., particularly S. aureus, are associated with shallow ulcers and ulcers of short duration; whereas, ulcers that are deep or of long duration tend to have more diverse microbial community, with the presence of anaerobic bacteria and Gram-negative Proteobacteria spp.[17]
Physiological stressors, like metabolic disease, and psychological stressors, such as depression, can modify microbial physiology in a way that increases their virulence, causing nonpathogenic microbes to transit to a pathogenic state. This impairs the body’s wound healing responses, and promotes infections.[18] Studies on the role of microbes in wound healing have yielded contradictory results, hence there is need for more research.[21] A 2014 study found that skin wounds had accelerated and scarless healing when commensal microbes were completely absent.[22] In contrast, another study found that decrease in commensal skin bacteria following oral antibiotic use reduced wound healing rates.[15]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Grice EA, Segre JA. The skin microbiome. Nature reviews microbiology. 2011 Apr;9(4):244-53.
- ↑ nature video. The skin microbiome: a healthy bacterial balance. Available from: http://www.youtube.com/watch?v=MWE3U3FItlc [last accessed 30/12/2022]
- ↑ 3.0 3.1 Perez Perez GI, Gao Z, Jourdain R, Ramirez J, Gany F, Clavaud C, Demaude J, Breton L, Blaser MJ. Body site is a more determinant factor than human population diversity in the healthy skin microbiome. PloS one. 2016 Apr 18;11(4):e0151990.
- ↑ Grice, E. A., Kong, H. H., Conlan, S., Deming, C. B., Davis, J., Young, A. C., NISC Comparative Sequencing Program, Bouffard, G. G., Blakesley, R. W., Murray, P. R., Green, E. D., Turner, M. L., & Segre, J. A. (2009, May 29). Topographical and temporal diversity of the human skin microbiome. Science (New York, N.Y.).
- ↑ Leung MH, Tong X, Wilkins D, Cheung HH, Lee PK. Individual and household attributes influence the dynamics of the personal skin microbiota and its association network. Microbiome. 2018 Dec;6(1):1-5.
- ↑ Zhai W, Huang Y, Zhang X, Fei W, Chang Y, Cheng S, Zhou Y, Gao J, Tang X, Zhang X, Yang S. Profile of the skin microbiota in a healthy Chinese population. The Journal of Dermatology. 2018 Nov;45(11):1289-300.
- ↑ Bonté F, Girard D, Archambault JC, Desmoulière A. Skin changes during ageing. Biochemistry and Cell Biology of Ageing: Part II Clinical Science. 2019:249-80.
- ↑ Chu DM, Ma J, Prince AL, Antony KM, Seferovic MD, Aagaard KM. Maturation of the infant microbiome community structure and function across multiple body sites and in relation to mode of delivery. Nature medicine. 2017 Mar;23(3):314-26.
- ↑ Ying S, Zeng DN, Chi L, Tan Y, Galzote C, Cardona C, Lax S, Gilbert J, Quan ZX. The influence of age and gender on skin-associated microbial communities in urban and rural human populations. PloS one. 2015 Oct 28;10(10):e0141842.
- ↑ McCall LI, Callewaert C, Zhu Q, Song SJ, Bouslimani A, Minich JJ, Ernst M, Ruiz-Calderon JF, Cavallin H, Pereira HS, Novoselac A. Home chemical and microbial transitions across urbanization. Nature microbiology. 2020 Jan;5(1):108-15.
- ↑ Song SJ, Lauber C, Costello EK, Lozupone CA, Humphrey G, Berg-Lyons D, Caporaso JG, Knights D, Clemente JC, Nakielny S, Gordon JI. Cohabiting family members share microbiota with one another and with their dogs. elife. 2013 Apr 16;2:e00458.
- ↑ Bouslimani A, da Silva R, Kosciolek T, Janssen S, Callewaert C, Amir A, Dorrestein K, Melnik AV, Zaramela LS, Kim JN, Humphrey G. The impact of skin care products on skin chemistry and microbiome dynamics. BMC biology. 2019 Dec;17(1):1-20.
- ↑ van Mierlo MM, Totté JE, Fieten KB, van den Broek TJ, Schuren FH, Pardo LM, Pasmans SG. The influence of treatment in alpine and moderate maritime climate on the composition of the skin microbiome in patients with difficult to treat atopic dermatitis. Clinical & Experimental Allergy. 2019 Nov;49(11):1437-45.
- ↑ Li H, Wang Y, Yu Q, Feng T, Zhou R, Shao L, Qu J, Li N, Bo T, Zhou H. Elevation is associated with human skin microbiomes. Microorganisms. 2019 Nov 24;7(12):611.
- ↑ 15.0 15.1 Zhang M, Jiang Z, Li D, Jiang D, Wu Y, Ren H, Peng H, Lai Y. Oral antibiotic treatment induces skin microbiota dysbiosis and influences wound healing. Microbial ecology. 2015 Feb;69(2):415-21.
- ↑ SanMiguel AJ, Meisel JS, Horwinski J, Zheng Q, Grice EA. Topical antimicrobial treatments can elicit shifts to resident skin bacterial communities and reduce colonization by Staphylococcus aureus competitors. Antimicrobial agents and chemotherapy. 2017 Sep 1;61(9):e00774-17.
- ↑ 17.0 17.1 Byrd Allyson L, Yasmine B, Segre Julia A. The human skin microbiome [J]. Nat Rev Microbiol. 2018;16:143-55.
- ↑ 18.0 18.1 Holmes CJ, Plichta JK, Gamelli RL, Radek KA. Dynamic role of host stress responses in modulating the cutaneous microbiome: implications for wound healing and infection. Advances in wound care. 2015 Jan 1;4(1):24-37.
- ↑ Nakatsuji T, Cheng JY, Gallo RL. Mechanisms for control of skin immune function by the microbiome. Current Opinion in Immunology. 2021 Oct 1;72:324-30.
- ↑ 20.0 20.1 Park YJ, Lee HK. The role of skin and orogenital microbiota in protective immunity and chronic immune-mediated inflammatory disease. Frontiers in immunology. 2018 Jan 10;8:1955.
- ↑ Johnson TR, Gómez BI, McIntyre MK, Dubick MA, Christy RJ, Nicholson SE, Burmeister DM. The cutaneous microbiome and wounds: new molecular targets to promote wound healing. International Journal of Molecular Sciences. 2018 Sep 11;19(9):2699.
- ↑ Canesso MC, Vieira AT, Castro TB, Schirmer BG, Cisalpino D, Martins FS, Rachid MA, Nicoli JR, Teixeira MM, Barcelos LS. Skin wound healing is accelerated and scarless in the absence of commensal microbiota. The Journal of Immunology. 2014 Nov 15;193(10):5171-80.