Secondary Progressive Multiple Sclerosis (SPMS) - A Case Study
Abstract[edit | edit source]
Purpose: The purpose of this fictional case study is to outline and examine the presentation of a patient with Secondary Progressive Multiple Sclerosis (SPMS) and highlight research on the effects of treatment by an interdisciplinary health care team with the focus on physiotherapy management. This case spans from initial assessment to the 12-week follow up and discharge.
Case Presentation: This fictional case study focuses on Geraldine Smith, a 35-year-old woman whose diagnosis recently changed from SPMS active without progression to SPMS active with progression. This progression brought on an increase in symptoms that mainly effected her mobility, work, activities of daily living and participation in fun events with her family.
Intervention: Mrs. Smith was prescribed an intervention program focused on balance, strengthening, stretching and gait to help improve or limit her symptoms. She is currently receiving additional treatment from her neurologist, occupational therapist and psychiatrist, while also looking into massage therapy and pelvic floor physiotherapy.
Outcomes: Mrs. Smith's follow-up showed notable improvements in her fatigue level, balance and gait. The prescription of a more appropriate gait aid improved her confidence, balance and gait overall. The additional treatments from the rest of her interdisciplinary health care team have also contributed to improving her quality of life and functional ability. Geraldine’s adherence to her home exercise program and improvements thus far indicate she is on track to meet her goals and can be discharged at this time.
Introduction[edit | edit source]
Multiple Sclerosis (MS)(MS) is an autoimmune inflammatory disease that causes the demyelination of neurons in the Central Nervous System (CNS). It tends to develop in young adults, resulting in considerable deficits in sensory, motor, autonomic, and neurocognitive function[1]. MS can be classified as either Relapsing-Remitting MS (RRMS), or Progressive MS.

The latter can be categorized as Primary or Secondary Progressive MS, and further broken down into active or not active, with or without progression, as seen in Figure 1[2] . There have been several mechanisms proposed to explain the occurrence of Progressive MS, which affects 10-20% of patients. One explanation is that inflammation causes degeneration of the brain, while other theories state that the inflammation and neurodegeneration occur independently[3]. However, the two are not mutually exclusive. In fact, 50% of those diagnosed with RRMS will transition to Progressive MS within 10 years, and 90% will transition within 25 years[4]. Progression is measured through clinical evaluation of the patient’s status and outcome measures, at least once a year. This can be done using the Nine Hole Peg Test (NHPT), Timed 25-Foot Walk (T25FW), and Paced Auditory Serial Addition (PASAT) which give a picture of physical and cognitive function.
This case study tracks the progress of Geraldine Smith, a 35-year-old woman diagnosed with Secondary Progressive Multiple Sclerosis (SPMS) in 2011. She initially reported symptoms of blurred vision, general weakness, and difficulty with balance to her family physician. The presence of low-level lesions and plaque formation in the cerebral white matter were noted through MRI imaging, and Evoked Potential testing was conducted to confirm the diagnosis as MS. The disease has been classified as active without progression for 10 years. However, Mrs. Smith began to notice her symptoms were worsening over the last few months and decided to schedule a visit with her neurologist. MRI imaging confirmed her diagnosis had changed to SPMS active with progression. Her neurologist suggested she visit the Physical Therapy Clinic at Queen’s University to help manage her symptoms and functional abilities. Mrs. Smith was diagnosed with depression five years ago and hypertension four years ago. She is easily fatigued during her job as an online sales representative, even when working from home, where she lives with her husband and daughter.
Studies have researched the benefits of physical therapy management in patients with MS. Kalron et al. (2016) found that standardized physical therapy brings about a significant increase in gait speed and step length in patients at the end of an intervention program[5]. A similar approach can be taken with Mrs. Smith to improve her mobility functions and assist her in reaching her personal goals. The incorporation of a balance rehabilitation program has proven to reduce the fall rate and improve balance skills in subjects with MS, with a statistically significant difference on the Berg Balance Scale[6]. This form of physical therapy would address one of Mrs. Smith’s concerns by reducing her risk of falls.
The purpose of this fictional case study is to present evidence-based research on the effects of physiotherapy management as part of an inter-professional healthcare team on a patient with SPMS. Comparisons are drawn from the patient’s case to existing literature to describe the history of illness, findings from the examination, interventions, and the resultant outcomes.
Client Characteristics[edit | edit source]
Geraldine Smith is a 35-year-old female (DOB: 12/31/1985) who was diagnosed with SPMS active without progression 10 years ago (2011) but whose diagnosis has now developed to SPMS active with progression. Mrs. Smith currently lives with her husband and daughter in Kingston, Ontario and works from home as an online sales representative. Mrs. Smith was diagnosed with depression 5 years ago and hypertension 1 year later. Her neurologist recommended she attend physiotherapy due to her recent change in diagnosis to active with progression and her increasing difficulty with activities of daily living. Mrs. Smith is concerned about her current level of function with this recent decline and hopes that physiotherapy can help prevent further progression of her symptoms and improve her independent function.
Examination Findings[edit | edit source]
Subjective Assessment[edit | edit source]
Chief Complaint[edit | edit source]
Mrs. Smith is concerned with her current functional level because she wants to be “fit enough” to walk around at her daughter’s grade 8 graduation in one year.
History of Present Illness[edit | edit source]
- Medical Diagnosis: SPMS active with progression (2021)
- Treatment to date: no previous history of physiotherapy treatment
- Current symptoms: increased weakness and fatigue in lower extremities, reduced endurance, difficulty with normal gait and impaired balance, difficulty controlling bladder[8]
Past Medical History[edit | edit source]
- Diagnosed with SPMS-Active without Progression in 2011 (10 years ago)
- Comorbidities:
Medications[edit | edit source]
- Baclofen – 10mg 3/day to help muscle spasms[8]
- Dalfampridine – 10mg every 12hrs to help with gait[8]
- Amantadine – 100mg 3/day to help with fatigue[8]
- Fluoxetine – 30mg/day to help with depression symptoms[13]
- Captopril – 25mg every 12hrs to control hypertension[14]
Social History[edit | edit source]
- Home: lives in a bungalow with 4 steps to access the front entrance
- Social Support: lives with her husband Jerry and their 12-year-old daughter, Jane
- Occupation: online sales representative, currently working from home
- Patient reports noticing the need to take more frequent breaks due to fatigue and reduced focus
- Hobbies: baking with her daughter, walking outside with her husband
- Patient reports fatigue and unsteadiness have been limiting her ability to participate in either activity
Family History[edit | edit source]
No previous family members with MS.
Functional History[edit | edit source]
- Previously able to walk with single-point cane for at least 30 minutes without experiencing pain or fatigue.
- Previously able to walk up the 4 front steps with single-point cane and no railing without any difficulties.
- Gradually decreased driving after her initial diagnosis and has not driven in over 2 years.
Current Functional Status[edit | edit source]
- Able to walk for 5 minutes with a single point cane before stopping for a break due to fatigue in the lower extremities.
- Reports difficulties when going from sitting to standing in chairs without armrests.
- Experiencing difficulty getting on and off the toilet
- Waiting for an Occupational Therapist consult for how to adjust home environment
- Currently having difficulty ascending the 4 front steps with single-point cane, even with use of the railing.
- Difficulty walking on the uneven grass to get to her driveway because it feels like her legs will collapse and she will fall.
- Increased dependency on her husband for errands and household chores.
- Feels unsteady when standing and baking due to lack of focus and other arm movements.
- Had 1 fall 2 weeks ago and has had multiple near-falls since.
Patient Goals[edit | edit source]
- Limit further progression of symptoms as much as possible.
- Build up endurance to be able to walk with daughter at Grade 8 graduation.
- Improve balance to be able to stand while baking and be able to walk on uneven surfaces.
- Be able to walk up front steps without having to take a break.
Objective Assessment[edit | edit source]
Range of Motion (ROM)
- UE - WNL
- LE - Table 1
| Joint | Movement | Range (°) |
|---|---|---|
| Hip | Flexion | 110 |
| Hip | Extension | 2 |
| Hip | Abduction | 35 |
| Hip | Adduction | 30 |
| Hip | IR | 30 |
| Hip | ER | 40 |
| Knee | Flexion | 125 |
| Knee | Extension | -5 |
| Ankle | Plantar flexion | 50 |
| Ankle | Dorsiflexion | 0 |
| Ankle | Inversion | 30 |
| Ankle | Eversion | 10 |
Spasticity - Modified Ashworth scale[15]
- UE – WNL (0)
- LE (both sides) - Table 2
| Muscle Group | Score |
|---|---|
| Hip Flexors | 1+ |
| Hip Extensors | 1 |
| Hip Abductors | 0 |
| Hip Adductors | 0 |
| Knee Flexors | 1+ |
| Knee Extensors | 1 |
| Ankle Plantar Flexors | 2 |
| Ankle Dorsiflexors | 1 |
Strength - Manual Muscle Testing (MMT)
- LE (bilateral) - Table 3
| Muscle Group | Score (/5) |
|---|---|
| Hip Flexors | 4 |
| Hip Extensors | 3+ |
| Hip Abductors | 4 |
| Hip Adductors | 4 |
| Hip Internal Rotators | 4 |
| Hip External Rotators | 4 |
| Knee Flexors | 4 |
| Knee Extensors | 4- |
| Ankle Plantar Flexors | 3+ |
| Ankle Dorsiflexors | 3+ |
| Ankle Inverters | 4 |
| Ankle Everters | 4- |
Neurological
- Dermatomes - WNL
- Myotomes - WNL
- Reflexes
- Sensation testing - WNL
Gait[18]
- Decreased ankle dorsiflexion at initial contact, resulting in insufficient heel strike
- Decreased hip extension in terminal stance
- Loss of dorsiflexion and heel raise in terminal stance
- Reduced push off in pre-swing to initial swing
- Incomplete foot clearance in initial swing
- Lack of full knee extension in terminal swing
- Reduced gait speed, step and stride length
- Gait speed 0.5m/s with single point cane
- Difficulty performing dual-tasks
- Reliant on single point cane gait aid
Balance
- Administered Berg Balance Scale(BSS)[19][20]-32/56
- Activities-Specific Balance Scale (ABC) Self Report Outcome Measure[19] -40
Fatigue

Walking Ability
- Disease Steps [23]-4 late cane
- Patient Determined Disease Steps[24] -5 late cane
- Timed up and go (TUG) [19][25](with single point cane) - 17 seconds
- Increased risk of falls
- Requires gait aid
Endurance
- Six-Minute Walk Test (6MWT)[19][26] - 140m
- With single point cane
- Borg Rating of Perceived Exertion (RPE)[27] - 16
Quality of Life and Physical Function
- Multiple Sclerosis Impact Scale (MSIS-29)[19]
- Physical – 46.25
- Psychological – 52.78
Clinical Impression[edit | edit source]
Mrs. Smith is a 35-year-old female whose SPMS symptoms have notably worsened with her change in disease status to active with progression. Mrs. Smith is currently presenting with bilateral lower extremity (LE) fatigue with minimal activity, hypomobility, spasticity, reduced strength, impaired gait and balance, and incontinence. These components are greatly limiting to her mobility, functional ability and confidence in performing daily activities.
Body, Structure and Function
- Decreased sensory and motor conduction rate due to demyelination and axonal degeneration associated with disease.
- Reduced mobility and ambulatory endurance due to increased fatigue, LE and aerobic deconditioning, and impaired gait pattern and impaired balance.
- Impaired gait pattern due to reduced LE strength and range of motion, particularly in plantar flexors (push off), dorsiflexors (foot clearance, heel strike) and hip extensors (terminal stance).
- Deconditioning of LE and aerobic capacity due to increased sedentary behaviours since diagnosis.
- Lack of steadiness due to impaired proprioception and compensatory balance.
- Difficulty with bladder control due to disease progression.
Activity
- Increased difficulty rising from sit to stand, notably when rising from chairs without armrests or the toilet, due to LE deconditioning.
- Reduced independence and ability to perform previously manageable activities of daily living (ADLs) due to quick onset of fatigue in LEs.
Participation
- Difficulty focusing on work for extended periods (e.g. needing to take frequent breaks) due to decreased cognitive attention span and fatigue.
- Has trouble maintaining balance while standing when baking with her daughter.
Personal Factors
- Development of depression in years following diagnosis and loss of ability to participate in activities involving her family.
- Increased fear of falling.
Environmental Factors
- 4 steps to enter front door of house
- Uneven ground to get to her driveway
Interventions[edit | edit source]
Patient Centered Treatment
Short Term Goals:
- Find a group-based exercise class (ex. yoga or swimming) at the discretion of the patient by the end of the first week of treatment.
- Reduce Fatigue Severity Score to a 49/63 in 2 weeks.
- Increase walking tolerance to 8 minutes with her gait aid within 4 weeks.
Long Term Goals:
- Avoid progression past a score of 6 on the EDSS within one year.
- Consistently achieving 150min/week of physical activity within 3 months.[28]
- Able to participate in daughter's Grade 8 Graduation ceremony for the entire evening (~3 hours of intermittent standing, walking and sitting) while not surpassing a 12 on the BORG RPE, in one year from now.
In-Clinic Management
Balance Exercises
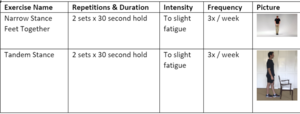
- Begin balance program with undisturbed, static, bilateral support movements. With appropriate progression, change the environment to add perturbations, dynamic components or unilateral components to further challenge balance.
Strengthening Exercises
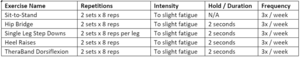
- Begin strengthening exercise program with light functional exercises without resistance. Slowly progress exercises by increasing resistance or adapting the exercise as patient improves.
Gait Training
- Prescribe quad cane gait aid for use instead of single-point cane. Due to the patient’s current status, she would benefit from a more stable gait aid that still allows for mobility.
- Therapist instructed, focusing on;
- Appropriate sequencing through gait stages
- Maintaining symmetry
- Appropriate stride length
- Achieving foot clearance
Education
- Promoting the importance of physical activity in reducing secondary complications
- Fatigue management program
- Strive for a self-modulated management strategy.
- Further elaborate that any activity is better than no activity.
- On good days, try to do more physical activity.
- On bad days, try to do some physical activity.
- On really bad days, it's okay to do no physical activity!
- Strive for a self-modulated management strategy.
Home Exercise Program
- Aerobic Exercise
- Swimming
- Encourage patient to swim. Swimming is a low-impact form of aerobic exercise that is coupled with large range of motions which will help increase her range of motion throughout her body[30].
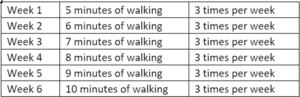
- Walking program
- Start within current functional limits and build up gait tolerance as the weeks progresses.
- Swimming
- Balance
- Complete the same balance exercises performed in clinic to ensure weekly volume is reached.
- Strengthening Exercises
- Complete the same strengthening exercises performed in clinic to ensure weekly volume is reached.
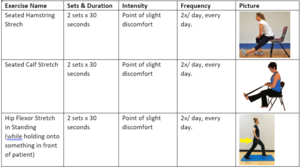
- Stretching Exercises
- Begin stretching program with global stretches to help facilitate overall flexibility of the lower extremities.
Interdisciplinary Treatment
- Massage Therapy
- Referral to massage therapy would benefit patient in increasing lower extremity range of motion, decreasing spasticity and promoting overall relaxation of her body.[31]
- Pelvic Floor physiotherapy specialist
- Referral to a pelvic floor specialist to address bladder control issues. [32]
Outcome[edit | edit source]
Geraldine attended a follow-up appointment 3 months after the initial visit. During the reassessment, the FSS, BSS and TUG were all re-administered. Her FSS score decreased from a 52/63 to a 44/63, her BSS increased from a 32/56 to a 40/56, and her TUG improved from 17 seconds to 14.5. These outcome measure improvements demonstrate reduced fatigue, improved balance, and an increase in walking speed and functional strength, respectively.
Following the home evaluation with the occupational therapist, the Smith family had an assistance bar installed beside the toilets which has provided Geraldine assistance when rising from the toilet on days when she needs it. The occupational therapist also provided Geraldine with strategies to use while baking, such as gathering all the ingredients beforehand, and taking breaks between the recipes' steps.
Geraldine followed up with a pelvic floor therapist and has initiated a pelvic floor strengthening program to improve her bladder control. Geraldine’s depression has continuously improved by attending her CBT sessions with her psychiatrist and getting more social interaction with her exercise class.
Geraldine has been successful with her long-term goal of consistently accumulating >150 minutes of physical activity at the 3 month mark, which is on track with her original timeline. Geraldine has picked up Yoga and Aerobic Swimming classes and is enjoying the social component of both. She appears on track to achieving her main goal of walking with her daughter at her Grade 8 graduation as she can currently walk for 12 minutes without stopping for a break.
At this time, it is appropriate to discharge Geraldine from private practice physiotherapy services. Geraldine will be instructed to continue with her HEP to maintain her current levels of physical function. Following discharge, she will have a 6-week telerehabilitation visit scheduled to ensure she is maintaining her current function and give an opportunity to provide her with any other education she may need.
Discussion[edit | edit source]
Geraldine Smith is a 35-year-old female online sales representative who was recommended physiotherapy to manage her SPMS that, after 10 years, had changed in status from active without progression to active with progression. Since her initial diagnosis, Geraldine's SPMS primarily impacted her bilateral lower extremities. The compounding effects of demyelination associated with the disease and resulting deconditioning from reduced activity levels had led to ongoing challenges with ambulation and balance. The patient's main goals were to be able to better tolerate daily activities, participate in her daughter’s Grade 8 Graduation in one years' time, and minimize the further progression of her disease as much as possible.
In her physiotherapy assessment, both subjective and objective findings demonstrated Geraldine had reduced lower extremity strength, endurance, flexibility, and impaired gait and balance. These presentations were largely attributed to a cycle of reduced activity levels, deconditioning and fear avoidance behaviour, commonly seen in patients with MS. It was determined Geraldine would benefit from a personalized home exercise program to help strengthen her lower extremity muscles, increase her endurance, lessen muscle spasticity and tone, and improve her balance. She was provided specific gait training instructions and prescribed a quad cane as a more appropriate gait aid to provide increased stability and reduce her risk of future falls. Geraldine greatly benefitted from being educated on the importance of physical activity and improved self-efficacy strategies. In addition to her physiotherapist, Geraldine's interdisciplinary team has included her neurologist, family physician, occupational therapist, pelvic floor therapist, massage therapist and psychiatrist. Geraldine's adherence to her home exercise program and improved outcome measures indicate that she is on track to achieving her goals of walking with her daughter at Grade 8 Graduation in one year, and making daily activities more manageable and enjoyable.
The broader implications of this case give rise to the importance of an interdisciplinary team in the assessment and management of patients with SPMS. SPMS presents with multifactorial symptoms which are not just isolated to physical impairments. Thus, it is essential to include a multitude of health care professionals to cover all impairments that are experienced by the patient. This case also highlights the importance of physical activity when dealing with a neurological condition like MS. Although the specific type and amount of activity needs to be tailored to each individual and their specific limitations and goals, physical activity should always be a component of the rehabilitation plan for MS patients[28]. It is also crucial to educate patients on the importance of physical activity in improving their symptoms and limiting secondary complications and comorbidities. This fictional case demonstrates how, with proper management and lifestyle adjustment, individuals with MS can often remain functional and achieve realistic goals.
Self-study Questions[edit | edit source]
1) Which of the following tests would likely be normal in a patient with MS?
a. Achilles Tendon Reflex
b. Clonus
c. C6 Myotome
d. Babinski
2) Which of the following is NOT a type of Multiple Sclerosis diagnosis?
a. Secondary Progressive Multiple Sclerosis
b. Relapsing Remitting Multiple Sclerosis
c. Primary Progressive Multiple Sclerosis
d. Clinically Isolated Syndrome
e. Tertiary Progressive Multiple Sclerosis
3) Which of the following would be the best course of treatment for a patient with MS?
a. Intensive strengthening program
b. Flexibility training twice a week
c. 150 min/week of physical activity
d. Thermal ultrasound
Answers: 1) c , 2) e , 3) c
References[edit | edit source]
- ↑ Sospedra M, Martin R. Immunology of Multiple Sclerosis. Annual Review of Immunology. 2005; 23: 683-747.
- ↑ 2.0 2.1 Lublin FD. New Multiple Sclerosis Phenotypic Classification. European Neurology. 2014Sep;72(s1):1-5.
- ↑ Lassman, H. Multiple Sclerosis Pathology. Cold Spring Harbor perspectives in medicine. 2018; 8(3).
- ↑ Secondary progressive MS (SPMS). National Multiple Sclerosis Society. [cited 2021May13]. Available from: https://www.nationalmssociety.org/What-is-MS/Types-of-MS/Secondary-progressive-MS
- ↑ Kalron A, Rosenblum U, Frid L, Achiron A. Pilates exercise training vs. physical therapy for improving walking and balance in people with multiple sclerosis: a randomized controlled trial. 2016; 31(3): 319-328.
- ↑ Cattaneo D, Jonsdottir J, Zocchi M, Regola A. Effects of balance exercises on people with multiple sclerosis: a pilot study. 2007; 21(9): 771-781.
- ↑ 7.0 7.1 Diagnosis secondary progressive MS (SPMS) [Internet]. National Multiple Sclerosis Society. [cited 2021May10]. Available from: https://www.nationalmssociety.org/What-is-MS/Types-of-MS/Secondary-progressive-MS/Diagnosing-Secondary-Progressive-MS
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 8.7 8.8 8.9 Multiple Sclerosis (MS) - Neurologic Disorders [Internet]. Merck Manuals Professional Edition. Merck Manuals; [cited 2021May9]. Available from: https://www.merckmanuals.com/en-ca/professional/neurologic-disorders/demyelinating-disorders/multiple-sclerosis-ms#v1045158
- ↑ JF. K, BG W, CEP van M. Expanded Disability Status Scale (EDSS) [Internet]. MS Trust. 2020 [cited 2021May10]. Available from: https://mstrust.org.uk/a-z/expanded-disability-status-scale-edss
- ↑ 10.0 10.1 AJMC Perspectives. Comorbidities Management and Lifestyle Modification in... [Internet]. AJMC. [cited 2021 May9]. Available from: https://www.ajmc.com/view/comorbidities-management-and-lifestyle-modification-in-patients-with-multiple-sclerosis
- ↑ 11.0 11.1 Zhang T, Tremlett H, Zhu F, Kingwell E, Fisk JC, Bhan V, et al. Effects of physical comorbidities on disabilty progression in multiple sclerosis. Neurology. 2018;90(5).
- ↑ Chwastiak LA, Ehde DM. Psychiatric Issues in Multiple Sclerosis. Psychiatric Clinics of North America. 2007;30(4):803-17.
- ↑ Fluoxetine: Drug Uses, DOsage & Side Effects [Internet]. Drugs.com [cited 2021May10]. Available from: https://www.drugs.com/fluoxetine.html
- ↑ Capoten, Captoril (captopril) dosing, indications, interactions, adverse effects, and more. 2020 [cited 2021May11]. Availabl from: https://reference.medscape.com/drug/capoten-captoril-captopril-342315
- ↑ Harb A, Kishner S, Modified Ashworth Scale. StatPearls [Internet]. 2020May31 [cited 2021May9]; Available from: https://www.ncbi.nlm.nih.gov/books/NBK554572/
- ↑ Sustained ankle clonus [Internet]. YouTube. YouTube; 2020 [cited 2021May12]. Available from: Sustained ankle clonus
- ↑ Physiotutors. The Babinski Sign or Reflex | Upper Motor Neuron Lesion [Internet]. YouTube. YouTube; 2016 [cited 2021May12]. Available from: The Babinski Sign or Reflex | Upper Motor Neuron Lesion
- ↑ Kempen JC, Doorenbosch CA, Knol DL, Groot VD, Beckerman H. Newly Identified Gait Patterns in Patients with Multiple Sclerosis May Be Related to Push-off Quality. Physical Therapy. 2016;96(11):1744-52.
- ↑ 19.0 19.1 19.2 19.3 19.4 19.5 19.6 Cohen ET, Potter K, Allen DD, Bennett SE, Brandfass KG, Widener GL, et al. Selecting Rehabilitation Outcome Measures for People with Multiple Sclerosis. International Journal of MS Care. 2015;17(4):181-9
- ↑ Berg Balance Scale [Internet]. Physiopedia. [cited 2021May10]. Available from: https://www.physio-pedia.com/Berg_Balance_Scale
- ↑ 21.0 21.1 Fatigue Severity Scale [Internet]. Physiopedia. [cited 2021May11]. Available from: https://physio-pedia.com/Fatigue_Severity_Scale
- ↑ Fatigue Severity Scale [Internet]. Shirley Ryan AbilityLab. [cited 2021May11]. Available from: https://www.sralab.org/rehabilitation-measures/fatigue-severity-scale
- ↑ Guidebook – Disease Steps Form (.pdf) [Internet]. National MS Society. [cited 2021 May 12]. Available from: https://www.nationalmssociety.org/NationalMSSociety/media/MSNationalFiles/Brochures/10-2-3-28-Disease_Steps_Form.pdf
- ↑ Learmonth YC, Motl RW, Sandroff BM, Pula JH, Cadavid C. Validation of patient determined disease steps (PDDS) scale scores in persons with multiple sclerosis. BMC Neurology. 2013;13(1).
- ↑ Timed Up and Go Test (TUG) [Internet]. Physiopedia. [cited 2021May11]. Available from:Timed Up and Go Test (TUG)
- ↑ Wetzel JL, Fry DK, Pfalzer LA. Six-Minute Walk Test for Persons with Mild or Moderate Disabiility from Multiple Sclerosis: Performance and Explanatory Factors. Physiotherapy Canada. 2011;63(2):166-80.
- ↑ Borg Rating of Perceived Exertion Scale [Internet]. HealthLink BC. 2021 [cited 2021 May 10]. Available from: https://www.healthlinkbc.ca/physical-activity/borg-rating-perceived-exertion-scale
- ↑ 28.0 28.1 28.2 Kalb, R., Brown, T. R., Coote, S., Costello, K., Dalgas, U., Garmon, E., Giesser, B., Halper, J., Karpatkin, H., Keller, J., Ng, A. V., Pilutti, L. A., Rohrig, A., Van Asch, P., Zackowski, K., & Motl, R. W. Exercise And Lifestyle Physical Activity Recommendations For People With Multiple Sclerosis Throughout The Disease Course. Multiple Sclerosis Journal. 2020;26(12):1459–1469.
- ↑ Moffat, F., & Paul, L. Barriers And Solutions To Participation In Exercise For Moderately Disabled People With Multiple Sclerosis Not Currently Exercising: A Consensus Development Study Using Nominal Group Technique. Disability and Rehabilitation. 2019;41(23), 2775–2783.
- ↑ Rafeeyan, Z., Azarbarzin, M., Moosa, F. M., & Hasanzadeh, A. Effect Of Aquatic Exercise On The Multiple Sclerosis Patients' Quality Of Life. Iranian Journal Of Nursing And Midwifery Research. 2010;15(1), 43–47.
- ↑ Schroeder, B., Doig, J., & Premkumar, K. The Effects Of Massage Therapy On Multiple Sclerosis Patients' Quality Of Life And Leg Function. Evidence-based Complementary And Alternative Medicine. 2014;640916.
- ↑ Vahtera, T., Haaranen, M., Viramo-Koskela, A. L., & Ruutiainen, J. Pelvic Floor Rehabilitation Is Effective In Patients With Multiple Sclerosis. Clinical rehabilitation. 1997;11(3), 211–219.
'''''