Proliferative Myositis
Original Editors - Billie Rehberg from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Billie Rehberg, Admin, 127.0.0.1, Elaine Lonnemann, WikiSysop, Kim Jackson and Wendy Walker
Definition/Description [edit | edit source]
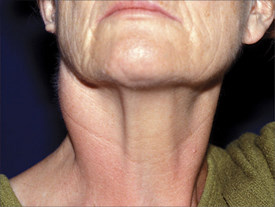
Proliferative myositis (PM) is a benign tumor which grows in skeletal muscle[1]. It is usually 3-4 cm in diameter[2], and is often mistaken for sarcomas (especially rhabdomyosarcoma)[3]. The tumor is formed by ganglion-like cells, fibroblasts, and myofibroblasts which increase the spaces between muscle fibers[2]. While etiology is unknown, it may result from injury to the muscle, fascia, or vasculature (resulting in ischemia) of the associated area[4]. PM generally presents in the upper extremity or trunk regions[2]. Median age of onset is 50 years[5], with rare cases reported in children[2]. [Photo: PM of the SCM muscle[1]]
Prevalence
[edit | edit source]
According to an article written by Fauser et. al in 2008, approximately 100 cases of PM had been published in the literature[1]. According to Jassar and Kumar (2005), approximately 1000 cases have been reported[6].
Characteristics/Clinical Presentation[1][6][7][8] [edit | edit source]
- Solid tumor within skeletal muscle
- Rapidly enlarging (often noticeably larger within several days time)
- Localized inflammation
- No lymph node enlargement
- No significant laboratory results
- Possible localized pain
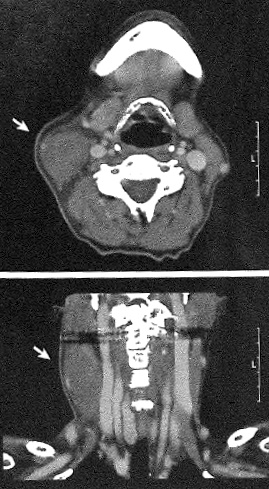
[Photo: Computerized Tomography of PM of the SCM muscle[1]]
Associated Co-morbidities[edit | edit source]
No associated co-morbidities have been reported.
Medications[edit | edit source]
Ibuprofen and other NSAIDs may be beneficial in decreasing pain and inflammation.
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
Proliferative Myositis is diagnosed based on biopsy[1]. The following list, taken directly from the Stanford University School of Medicine page on PM, are histologic and immunologic characteristics of PM which are used in its diagnosis:
o Relatively normal muscle fibers separated by expanded myxoid connective tissue
o Produces distinctive checkerboard pattern
o No evidence of muscle damage
o No sarcolemmal proliferation
o No multinucleation
o No nuclear enlargement
o No necrosis
o Connective tissue space between fibers contains reactive cells resembling those seen in nodular fasciitis and proliferative fasciitis
o Spindled and stellate fibroblasts and myofibroblasts
o Vesicular nuclei
o No cytologic atypia
o Actin positive
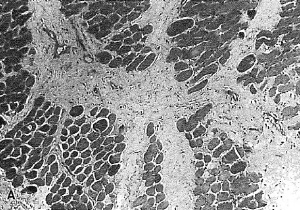
o CD68 variable [Image: "checkerboard" arrangement
o S100, desmin negative of cells often seen in PM biopsies[5]]
o Ganglion-like cells
o Characteristic feature of this process
o Large round regular nuclei
o Occasional binucleate and trinucleate cells may be seen
o Prominent nucleoli
o Dispersed chromatin
o Basophilic to amphophilic cytoplasm
o May be clustered and may mold each other
o Factor XIIIa positive
o Actin, CD68 negative to focal/weak
o Desmin, keratin, S100, neuron specific enolase negative
o Mitotic figures frequent
o No atypical mitotic figures [2]
Etiology/Causes[edit | edit source]
While etiology is unknown, PM may result from injury to the muscle, fascia, or vasculature (resulting in ischemia) of the associated area[4].
Systemic Involvement[edit | edit source]
Mulier et. al reported a case in which one patient had a mild fever (37.5 degrees C or 100 degrees F)[5]. No other cases of systemic symptoms have been reported.
Medical Management (current best evidence)[edit | edit source]
Proliferative Myositis is a self-limiting pathology, meaning that the growth of the tumor will eventually stop. While spontaneous resolution of the tumor has been reported[1][8][5], surgical excision is the only treatment and recurrence following excision is rare[2].
Physical Therapy Management (current best evidence)[edit | edit source]
No formal reports of the physical therapy treatment of PM have been published. However, it has been theorized that PM is a precursor to heterotopic ossification or myositis ossificans[6]. Thus, aggressive range of motion and strengthening exercises should be avoided to prevent possible aggravation of the condition while the tumor is still enlarging. Following surgical excision, ROM and strengthening exercises and modalities to regain normal muscular function and decrease pain may be beneficial.[5]
- Myositis Ossificans
- Neoplasms (especially rhabdomyosarcomas)
- Proliferative fasciitis
- Nodular fasciitis
- Fibromatosis
- Ganglioneuroblastoma or ganglioneuroma
Case Reports/ Case Studies[edit | edit source]
PM in the bicep of a 65 year-old female. Access this study in Radiology[9].
PM in the sternocleidomastoid of a 64 year-old female. Access this study in the Archives of Otolaryngology[1].
PM in the paraspinal muscles of a 14 year-old male. Access this study in Skeletal Radiology[5].
PM in the chest wall of a 48 year-old male. Access this study in The Annals of Thoracic Surgery[10].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Fauser C, Nahrig J, Niedermeyer H, Arnold W. Proliferative myositis: a rare pseudomalignant tumor of the head and neck. Archives of Otolaryngology - Head & Neck Surgery [serial online]. Apr 2008; 134(4): 437-440. Available from: CINAHL with Full Text.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Stanford University. Proliferative Myositis. Available at http://surgpathcriteria.stanford.edu/softfib/proliferative_myositis/printable.html. Accessed April 4, 2011
- ↑ Meis J, Enzinger F. Proliferative fasciitis and myositis of childhood. The American Journal Of Surgical Pathology [serial online]. Apr 1992; 16(4): 364-372. Available from: MEDLINE.
- ↑ 4.0 4.1 Dent C, DeBoom G, Hamlin M. Proliferative myositis of the head and neck. Report of a case and review of the literature. Oral Surgery, Oral Medicine, And Oral Pathology [serial online]. Sep 1994; 78(3): 354-358. Available from: MEDLINE.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 Mulier S, Stas M, Delabie J, Lateur L, Gysen M, De Wever I, et al. Proliferative myositis in a child. Skeletal Radiology [serial on the Internet]. Dec 1999; 28(12): 703-709. Available from: MEDLINE.
- ↑ 6.0 6.1 6.2 Jassar A, Kumar V. Proliferative myositis--a case report. Indian Journal Of Pathology & Microbiology [serial online]. January 2005;48(1):33-35. Available from: MEDLINE, Ipswich, MA. Accessed April 5, 2011.
- ↑ Sharma S and Banerjee AK. Proliferative Myositis: Report of Two Cases. Indian Journal of Pathology & Microbiology; an Official Organ of Indian Association of Pathologists and Microbiologists [serial online]. 1985;28(3):273-276.
- ↑ 8.0 8.1 Turner R, Robson A, Motley R. Proliferative myositis: an unusual cause of multiple subcutaneous nodules. Clinical and Experimental Dermatology 1997;22:101-103
- ↑ Demir MK, Beser M, and Akinci O. Case 118: Proliferative Myositis. Radiology [serial online]. August 2007 244:613-616.
- ↑ Kent MS, Flieder DB, Port JL and Altorki NK. Proliferative myositis: a rare pseudosarcoma of the chest wall. Annals of Thoracic Surgery [serial online]. 2002;73:1296-1298.