Pneumocystis Jirovecii Pneumonia
Introduction[edit | edit source]
Pneumocystis Jirovecii Pneumonia (PJP) was previously called as Pneumocystis Carinii Pneumonia (PCP), it is one of the most common opportunistic fungal infection in immuno-compromised conditions such as haematological malignancy, congenital immunodeficiency, organ transplantation, immunosuppressive therapy, under medication and predominantly in Human Immunodeficiency Virus (HIV). [1]
Epidemiology[edit | edit source]
PJP has a high incidence before the advent of prophylaxis treatment and highly active antiretroviral therapy (HAART). A study about the epidemiology of PJP showed that the incidence has significantly decreased both for the adult and pediatric population.[2] However, the same study showed that there is difference with the prevalence of PJP in industrialized countries, such as those in Europe and North America, and in developing countries , such as in Southeast Asia and Sub-Saharan Africa, wherein the former has a continuous decline while the latter is at a greater risk of incidence.[2]
A recent nationwide study in Spain, conducted by Pereira-Diaz et al, reported that PJP is an emerging disease in patients without HIV infection of which risk factors include haematological neoplasms, chronic lung diseases and, non-hematological cancers with high mean mortality and hospitalization costs.[3]
Etiology[edit | edit source]
The pathogen responsible for PJP is Pneumocystis Jirovecii, an organism classified as a fungus.
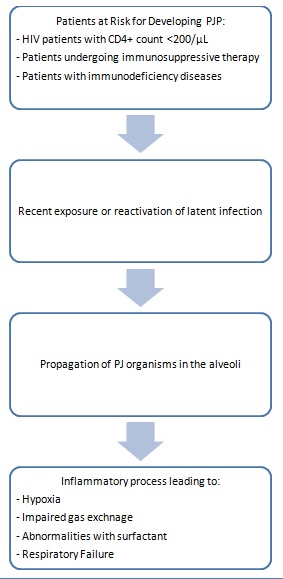
Pathophysiology[edit | edit source]
PJP Pathophysiology
Signs and Symptoms[edit | edit source]
- Subacute onset exertional dyspnea[4]
- Dry and non-productive cough[4]
- Fever or subfebrile temperatures[4]
- Chest pain
- Tachypnea
- Tachycardia
- Cyanosis
- Weight loss
Diagnostic Procedures[edit | edit source]
Diagnosis of PJP relies on combination of laboratory findings and diagnostic imaging together with physical examination and history-taking.
Laboratory procedures and findings pertinent to PJP diagnosis include:[edit | edit source]
- Quantitative polymerase chain reaction (qPCR)- more accurate way to diagnose PJP[5]
- (1–3)-β-d-glucan (BG) -most reliable serologic biomarker for PJP diagnosis[6]
- Krebs von den Lungen-6 antigen (KL-6)- together with BG, is the most accurate serologic apptoach for PJP diagnosis[6]
- Lactate dehydrogenase (LDH)[6]
- S-adenosyl methionine (SAM)[6]
- Sputum induction
Imaging studies used in the diagnosis of PJP include:[edit | edit source]
Chest CT Scan- most pertinent finding is ground glass opacity (GGO) indicative of alveolar subtotal consolidation[7]
Chest Radiography- nonspecific, can be normal, less common patterns have been reported, including lobar infiltrates, pulmonary nodules, and pneumatoceles and other cystic changes.[8]
Differential Diagnosis[edit | edit source]
Thorough evaluation that includes physical examination, laboratory findings and/or imaging studies are warranted in order to make a specific diagnosis of PJP and to differentiate it from other conditions with similar presentation, which include but not limited to:
- Bacterial pneumonia[8]
- Acute Respiratory Distress Syndrome[1]
- Viral pneumonia
- Pulmonary Tuberculosis[8]
- Pulmonary Embolism[1]
- Mycobacterium Avium Complex[1]
- Cytomegalovirus[8]
- Histoplasmosis
Prognosis[edit | edit source]
A meta-analysis conducted by Liu et al, stated that risk factors associated with increased mortality rate including old age, female sex, longer time from onset of symptoms to diagnosis, respiratory failure, solid tumors, high lactate dehydrogenase, low serum albumin, bacterial, and aspergillus co-infection, etc.[9] The findings of their study revealed that even in non-HVI patients, mortatlity rate for PJP infection is high.[9]
A predictive model to evaluate mortality in HIV/AIDS patients with PCP was constructed by Wu L. et al, based on routine laboratory and clinical parameters, which may be a simple tool for physicians to assess the prognosis in HIV/AIDS patients with PCP in China. [10] This includes 7 predictors, including LDH >350U/L, HR>130 times/min, room air PaO2 <70mmHg, later admission to ICU, Anemia (HGB≤90g/L), CD4<50cells/ul, and development of a pneumothorax. [10]
Pharmacological Management[edit | edit source]
- Trimethoprim/sulfamethoxazole (TMP-SMX)- first-line agent for the treatment of mild to severe PJP[8]
- Atovaquone- one of the oral treatment alternatives for mild and moderate PCP[8]
- Pentamidine isethionate- preferred alternative drug regimen to TMP-SMX[1][8]
- Clindamycin and Primaquine-good alternative choice for treatment of mild to moderate PJP[1]
- Caspofungin[1]
Prophylaxis[edit | edit source]
Physiotherapy Intervention[edit | edit source]
Physiotherapy interventions for the treatment of PJP would be the same as treating Pneumonia. This includes:
- Modified postural drainage
- Shaking, vibrations and percussion
- Coughing and huffing exercises
- Segmental and Diaphragmatic breathing exercises
- Mobilization of the patient
- General body conditioning exercises
See also Pulmonary Rehabilitation
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Kante, Meenakshi & Racherla, Rishi & Usha, Kalawat. (2019). Pneumocystis jirovecii Pneumonia: A Revisit to the Old Malady. JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH retrieved fromhttps://www.researchgate.net/publication/337105006_Pneumocystis_jirovecii_Pneumonia_A_Revisit_to_the_Old_Malady doi:10.7860/JCDR/2019/42636.13318
- ↑ 2.0 2.1 Morris A, Lundgren JD, Masur H, et al. Current epidemiology of Pneumocystis pneumonia. Emerg Infect Dis. 2004;10(10):1713–1720 retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3323247/ doi:10.3201/eid1010.030985
- ↑ Pereira-Díaz E, Moreno-Verdejo F, de la Horra C, Guerrero JA, Calderón EJ, Medrano FJ. Changing Trends in the Epidemiology and Risk Factors of Pneumocystis Pneumonia in Spain. Front Public Health. 2019;7:275. Published 2019 Oct 4 retrieved fromhttps://www.ncbi.nlm.nih.gov/pmc/articles/PMC6788256/ doi:10.3389/fpubh.2019.00275
- ↑ 4.0 4.1 4.2 Salzer H, J, F, Schäfer G, Hoenigl M, Günther G, Hoffmann C, Kalsdorf B, et al: Clinical, Diagnostic, and Treatment Disparities between HIV-Infected and Non-HIV-Infected Immunocompromised Patients with Pneumocystis jirovecii Pneumonia. Respiration 2018;96:52-65 retrieved fromhttps://www.karger.com/Article/FullText/487713# doi: 10.1159/000487713
- ↑ Alanio A, Bretagne S. Pneumocystis jirovecii detection in asymptomatic patients: what does its natural history tell us?. F1000Res. 2017;6:739. Published 2017 May 23 retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5464226/ doi:10.12688/f1000research.10619.1
- ↑ 6.0 6.1 6.2 6.3 Esteves F., Calé S. S., Badura R., De Boer M. G., Maltez F., Calderon E. J., et al. (2015). Diagnosis of Pneumocystis pneumonia: evaluation of four serologic biomarkers. Clin. Microbiol. Infect. 21:379.e1–e10 retrieved from https://www.sciencedirect.com/science/article/pii/S1198743X14001116 doi: 10.1016/j.cmi.2014.11.025
- ↑ Ebner L, Walti LN, Rauch A, et al. Clinical Course, Radiological Manifestations, and Outcome of Pneumocystis jirovecii Pneumonia in HIV Patients and Renal Transplant Recipients. PLoS One. 2016;11(11):e0164320. Published 2016 Nov 8 retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5100884/ doi:10.1371/journal.pone.0164320
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 Tasaka, S. (2015). Pneumocystis Pneumonia in Human Immunodeficiency Virus–infected Adults and Adolescents: Current Concepts and Future Directions. Clinical Medicine Insights: Circulatory, Respiratory and Pulmonary Medicine retrieved from https://journals.sagepub.com/doi/full/10.4137/CCRPM.S23324#articleCitationDownloadContainer doi: 10.4137/CCRPM.S23324
- ↑ 9.0 9.1 Liu Y, Su L, Jiang SJ, Qu H. Risk factors for mortality from pneumocystis carinii pneumonia (PCP) in non-HIV patients: a meta-analysis. Oncotarget. 2017;8(35):59729–59739. Published 2017 Aug 4 retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5601772/ doi:10.18632/oncotarget.19927
- ↑ 10.0 10.1 Wu L, Zhang Z, Wang Y,Hao Y, Wang F, Gao G, et al. A Model to Predict In-Hospital Mortality in HIV/AIDS Patients with Pneumocystis Pneumonia in China: The Clinical Practice in Real World retrieved from https://www.hindawi.com/journals/bmri/2019/6057028/#abstract doi: 10.1155/2019/6057028