Ober's Test
Original Editor - Nicole Kluckhohn, Agapi Hakobyan
Top Contributors - {{Special:Contributors/Ober's Test}}
Welcome to Arkansas Colleges of Health Education School of Physical Therapy Musculoskeletal 1 Project. This space was created by and for the students at Arkansas Colleges of Health Education School in the United States. Please do not edit unless you are involved in this project, but please come back in the near future to check out new information!!
Purpose[edit | edit source]
The Ober's test evaluates a tight, contracted or inflamed Tensor Fasciae Latae (TFL) and Iliotibial band (ITB). The Ober’s test must not be confounded with Noble’s test and the Renne test, two other tests that are commonly used to detect iliotibial band syndrome.
Clinically Relevant Anatomy[edit | edit source]
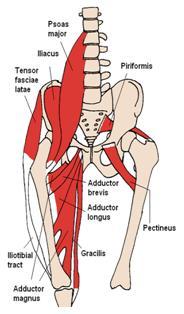
Anatomically, the ITB is a continuation of the tendinous portion of the TFL muscle with some contributions from the gluteal muscles. TFL/ITB is a synergist of the gluteus medius and gluteus minimus muscles in hip abduction[1]. The gluteus maximus muscle is responsible for hip extension, which is the action involved in the Ober test.
Origin:[edit | edit source]
- TFL originates from- the anterior part of the external lip of iliac crest, the outer surface of an anterior superior iliac spine, and the deep surface of fascia lata.[2]
- Iliotibial band (ITB) or tract is a lateral thickening of the fascia lata in the thigh. Proximally it splits into superficial and deep layers, enclosing tensor fasciae lata and anchoring this muscle to the iliac crest. It also receives most of the tendon of the gluteus maximus.[3]
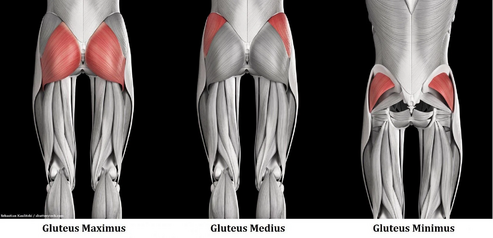
- Gluteus minimus originates on the external surface of the ilium between the anterior and inferior gluteal lines.[4]
- Glute medius begins on the external surface of the ilium between the anterior and posterior gluteal lines.[5]
- Glute maximus originates on the posterior gluteal line of the ilium and sacrotuberous ligament.[6]
Insertion:[edit | edit source]
- TFL inserts into the ITB at the anterolateral thigh at the junction of proximal and middle thirds of the thigh.[2]
- ITB is generally viewed as a band of dense fibrous connective tissue that passes over the greater trochanter of the hip, lateral femoral epicondyle of the knee and attaches to Gerdy's tubercle on the anterolateral aspect of the tibia.[3]
- Gluteus minimus inserts onto the anterior border of the greater trochanter.[4]
- Gluteus medius inserts onto the oblique ridge on the lateral surface of the greater trochanter of the femur.[5]
- Glute maximus also inserts into the ITB and the gluteal tuberosity of the femur.[6]
Action:[edit | edit source]
- TFL flexes, medially rotates, and abducts the hip joint; tenses the fascia lata; and may assist in knee extension.[2] Gluteus medius, gluteus minimus, and upper fibers of the gluteus maximus are the primary synergistic muscles of the hip abductors.
- ITB permits the TFL and Gluteus maximus to influence the stability of the extended knee joint, due to the insertion of these muscles into the ITB.[7]
- Gluteus minimus's main action is abduction and can serve as a hip stabilizer.[8]
- Gluteus medius 's main action main action is abduction. The anterior fibers internally rotate and assist in the flexion of the hip, while the posterior fibers can laterally rotate and assist in extension.[9]
- Gluteus maximus extends and externally rotates the hip. The lower fibers assist in the adduction of the hip, and the upper fibers assist in abduction.[10]
Collagen of the ITB[edit | edit source]
The ITB is composed of dense regular connective tissue. [11] It is also primarily composed of type 1 collagen, which runs in a longitudinal pattern. The longitudinal direction of the type 1 collagen resists stretching or tension forces on the ITB.[11]
Glute Contributions to Ober[edit | edit source]
While the Ober is primarily testing for a tight TFL or ITB, gluteus maximus could contribute to some variations in the test. Due to gluteus maximus attaching to the ITB, tightness of glute max could lead to a posterior pelvic tilt and weakness of glute max could lead to an anterior pelvic tilt. Tightness of the glute maximus could lead to indirect involvement of the ITB, leading to dysfunction due to the ITB inability to resist stretch.[12]
Technique[edit | edit source]
Frank Ober described the test for tightness of TFL and ITB in an article entitled "Back Strain and Sciatica", wherein he discussed the relationship of a contracted TFL and ITB to low backache (May 1935). This was later revised in the year 1937 which cautioned on avoiding hip internal rotation and flexion while carrying out the test.[13]
Test position:[14][15][edit | edit source]
- The patient should be in side-lying with the affected side up.
- Place a pillow between the patient and therapist.
- Bottom knee and hip should be flexed to flatten the lumbar curve.
- Stand behind the patient and firmly stabilize the pelvis to prevent movement in any direction. Try to stabilize above the gluteal muscles.
- Grasp the distal end of the patient’s affected leg with your other hand and flex the leg to a right angle at the knee
Test:[edit | edit source]
- Extend and abduct the hip joint.
- Slowly lower the leg toward the table -adduct hip- until motion is restricted.
- Ensure that the hip does not internally rotate and flex during the test. Additionally, the pelvis must be stabilized. Lacking stabilization and support allows the thigh to drop in flexion and internal rotation, which would 'give in' to the tight TFL and not accurately test the length (false negative).[13]
Results:[edit | edit source]
- If the ITB is normal, the leg will adduct with the thigh dropping down slightly below the horizontal and the patient won't experience any pain; in this case, the test is called negative.
- If the ITB is tight, the leg would remain in the abducted position, in this case, the test is called positive.
- If patient reports knee pain, stop the test and perform the modified ober test. The lateral knee pain could be caused from the ITB attachment to Gerdy's tubercle. Medial knee pain could caused by strain from the Ober test.
Modified Ober Test[13][edit | edit source]
A modification of the Ober test was first recommended by Kendalls in Posture and Pain. In this test, there is less strain on the medial aspect of the knee joint, less tension on the patella, less interference by a tight Rectus Femoris and it provides a complete stretch on TFL. Another reason for modifying the test is if the patient cannot get into the test position.
Test position:[edit | edit source]
- The patient is in a side-lying position with the underneath leg flexed at the hip and knee to flatten the low back.
- The examiner stabilizes the pelvis and keeps the lateral trunk in contact with the table. Stabilization should resemble the stabilization of the Ober.
- Note: Downward lateral tilt is equivalent to the hip abduction and that would "give in " to a tight TFL.
Test:[edit | edit source]
The patient is placed in side-lying and with the bottom leg bent. A pillow is placed between the therapist and the patient. During the modified test, the leg being tested is extended. The therapist will extend and abduct the hip. A negative test will consist of the patient being able to get 10° below parallel to the table.
Results:[edit | edit source]
- With the knee straight and the pelvis in a neutral position, the thigh drops about 10 degrees below the horizontal. It is suggestive of normal length.
- The leg fails to drop indicates tight ITB and TFL.
Evidence[edit | edit source]
- There is a limited number of studies to support the validity of this test.[17] A study by Reese et al shows that the use of an inclinometer to measure hip adduction using both the Ober test and the modified Ober test appears to be a reliable method for the measurement of IT band flexibility, and the technique is quite easy to use. It demonstrated a significant difference in ROM between testing with the affected knee flexed vs. extended, with the reliability of .90 and .91 respectively[18]. The modified Ober test allows a significantly greater hip adduction range of motion than the Ober test, the 2 examination procedures should not be used interchangeably for the measurement of the flexibility of the IT band.
- But the study findings in 'An Anatomic Investigation of the Ober Test' [19] by Willet GM et al refutes the hypothesis that the ITB plays a role in limiting hip adduction during either version of the Ober test and question the validity of these tests for determining ITB tightness. The findings underscore the influence of the gluteus medius and minimus muscles as well as the hip joint capsule on Ober test findings. The results of this study suggest that the Ober test assesses the tightness of structures proximal to the hip joint, such as the gluteus medius and minimus muscles and the hip joint capsule, rather than the ITB.
- In a study completed by Wang et al, ultrasonography was used to measure the width of the ITB during the Ober and modified Ober test. They saw a significant difference in the width of the ITB pre versus post-test for both the Ober and modified Ober. The width of the ITB was observed becoming more narrow. However, the modified Ober was observed to be able to assess the ITB to a further level than the normal Ober test. The modified Ober was able to apply more stretch to the ITB possibly due to the extended knee[20].
Key Research[edit | edit source]
- The study in Clinical Biomechanics by Gajdosik RL et al showed the hip adduction movement was restricted more with the knee flexed than with the knee extended for both genders (P < 0.009). Thus emphasizing the influence of knee positions and gender on the Ober test for the length of the iliotibial band[21].
- An exercise developed by the Postural Restoration Institute to recruit hamstrings and abdominal muscles showed a significant increase in passive hip-adduction angles (p<0.01) and a decrease in pain (p<0.01), immediately improve Ober's Test measurements in people with lumbopelvic pain. The study[22] showed hamstring/abdominal activation, rather than iliotibial band stretching, may be an effective intervention for addressing lumbopelvic pain and a positive Ober's Test.
- The study shows the effect of ITB stretching and Hamstring and Abdominal activation on positive Ober test in individuals with lumbopelvic pain[23] The hamstring and abdominal activation showed a greater reduction in pain and increase in hip adduction ROM as compared to only ITB stretching.
References[edit | edit source]
- ↑ Arab AM, Nourbakhsh MR. The relationship between hip abductor muscle strength and iliotibial band tightness in individuals with low back pain. Chiropractic & osteopathy. 2010 Dec;18(1):1.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2821316/ (accessed on 25/07/18)
- ↑ 2.0 2.1 2.2 Kendall, McCreary, Provance; Muscle Testing and Function with Posture and Pain 4th Edition; Tensor Fascia Latae; Page No.216
- ↑ 3.0 3.1 Fairclough J, Hayashi K, Toumi H, Lyons K, Bydder G, Phillips N, Best TM, Benjamin M. The functional anatomy of the iliotibial band during flexion and extension of the knee: implications for understanding iliotibial band syndrome. Journal of Anatomy. 2006 Mar;208(3):309-16.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2100245/ (accessed on 25/07/2018)
- ↑ 4.0 4.1 Kendall, McCreary, Provance; Muscle Testing and Function with Posture and Pain 4th Edition; pg No.432
- ↑ 5.0 5.1 Kendall, McCreary, Provance; Muscle Testing and Function with Posture and Pain 4th Edition; pg No.433
- ↑ 6.0 6.1 Kendall, McCreary, Provance; Muscle Testing and Function with Posture and Pain 4th Edition; pg No. 436
- ↑ Kendall, McCreary, Provance; Muscle Testing and Function with Posture and Pain 4th Edition; Fascia Latae; Page No.227
- ↑ Kendall, McCreary, Provance; Muscle Testing and Function with Posture and Pain 4th Edition; Fascia Latae; Page No.433
- ↑ Kendall, McCreary, Provance; Muscle Testing and Function with Posture and Pain 4th Edition; Fascia Latae; Page No.433
- ↑ Kendall, McCreary, Provance; Muscle Testing and Function with Posture and Pain 4th Edition; Fascia Latae; Page No.436
- ↑ 11.0 11.1 Fairclough, J., Hayashi, K., Toumi, H., Lyons, K., Bydder, G., Phillips, N., Best, T.M. and Benjamin, M., The functional anatomy of the iliotibial band during flexion and extension of the knee: implications for understanding iliotibial band syndrome. Journal of Anatomy, (2006);208: 309-316.
- ↑ Sahrmann, S. Movement System Impairmment Syndromes of the Extremities, Cervical, and Thoracic Spines. Elsevier Health Sciences. 2010
- ↑ 13.0 13.1 13.2 Kendall, McCreary, Provance; Muscle Testing and Function with Posture and Pain 4th Edition; Modified Ober Test; Page No,56-59.
- ↑ Magee D. Orthopedic Physical Assessment. 2nd ed.Pennsylvania:WB Saunders, 1992. p354-355
- ↑ Hoppenfeld S. Physical Examination of the spine and Extremeities. London: Prentice-Hall International 1976.p167
- ↑ Ober Test & Modified Ober Test. Available from https://www.youtube.com/watch?v=A0vTHVjhvFM
- ↑ Knee Orthopaedic Test - A Strategic Approach to Assessing the Knee; University of Western States, College of Chiropractic, Clinic Protocol; Ober test; Page No.23; Adopted 12/12. (accessed from Knee_Orthopedic_Tests.pdf on 30/07/18)
- ↑ Reese NB, Bandy WD. Use of an inclinometer to measure flexibility of the iliotibial band using the Ober test and the modified Ober test: differences in magnitude and reliability of measurements. Journal of Orthopaedic & Sports Physical Therapy. 2003 Jun;33(6):326-30.https://www.ncbi.nlm.nih.gov/pubmed/12839207 (accessed on 28/07/2018)
- ↑ Willett GM, Keim SA, Shostrom VK, Lomneth CS. An anatomic investigation of the Ober test. The American journal of sports medicine. 2016 Mar;44(3):696-701.https://www.ncbi.nlm.nih.gov/pubmed/26755689 accessed on 28/07/2018
- ↑ Tyng-Guey, W. Mei-Hwa, Jan. Kwan-Hwa, Lin. Hsing-Kuo, Wang. Assessment of Stretching of the Iliotibial Tract With Ober and Modified Ober Tests: An Ultrasonographic Study. Archives of Physical Medicine and Rehabilition. 2006 Oct. https://www.archives-pmr.org/article/S0003-9993(06)00531-4/abstract
- ↑ Gajdosik RL, Sandler MM, Marr HL. Influence of knee positions and gender on the Ober test for length of the iliotibial band. Clinical biomechanics. 2003 Jan 1;18(1):77-9.https://www.ncbi.nlm.nih.gov/pubmed/12527250 (accessed on 28/07/2018)
- ↑ Tenney HR, Boyle KL, DeBord A. Influence of hamstring and abdominal muscle activation on a positive Ober's test in people with lumbopelvic pain. Physiotherapy Canada. 2013 Jan;65(1):4-11.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3563370/ (accessed on 28/07/18)
- ↑ Effect of Iliotibial Band stretching versus Hamstrings and Abdominal muscle activation on a positive Ober’s test in subjects with Lumbopelvic Pain: A Randomized Clinical Trial by Vijay Kage, Saitej Kolukula Naidu; July 2015 https://www.ejmanager.com/mnstemps/12/12-1435370486.pdf (accessed on 30/07/18)