Neurocutaneous Syndromes
Introduction[edit | edit source]
Neurocutaneous syndromes are a group of congenital disorders affecting the skin, eye and nervous system which manifest in early childhood or adolescence. Neurofibromatosis (NF) and Tuberous Sclerosis Complex (TSC) are the most common among them and are together referred to as phakomatoses. Other conditions include Sturge-Weber syndrome and Von Hippel-Landau disease.[1][2]
Clinical Features[edit | edit source]
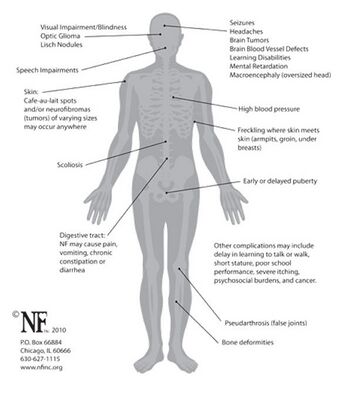
- NF commonly presents with café-au-lait spots (coffee colored lesions) and neurofibromas (soft flat or elevated dome-shaped tumors). Involvement of the Central Nervous System (CNS) can cause seizures and cognitive impairments. Half of the cases may present with spinal abnormalities such as scoliosis.[3]
- TSC presents with facial angiofibromas (symmetrical lesions around the nose and cheek), shagreen patch (a leathery patch around the sacral region), white-leaf macules (depigmentation seen over the trunk and lower legs), Koenen's tumor (an angiofibroma on the edge or surface of the nail plate). CNS symptoms include seizures and cognitive impairment.[3]
- Sturge-Weber syndrome commonly presents with hemifacial hemangioma (over the first or second division of the trigeminal nerve). CNS impairments can include contralateral hemiplegia, seizures and cognitive decline.[3]
- Von Hippel-Lindau syndrome may present with angiomas, café-au-lait spots and tumors in multiple body systems including renal and pancreatic tumors.[3]
- All neurocutaneous syndromes may involve the eye and present with varying severity of visual impairment. Cardiovascular impairments might be exhibited by some cases. Acoustic neuromas may lead to impairment of the facial and vestibulocochlear nerve.[3]
Management[edit | edit source]
The main treatment is symptomatic management of the patient.[3] Laser therapy is effective in the treatment of café-au-lait spots.[4] Neurofibromas are managed by surgical excision. Recurrence is common in both cases. Cryotherapy may have limited use. CNS symptoms are difficult to manage. Prognosis may be worse depending on the site, size and number of tumors.[3]
There are no clinical trials exclusively investigating the role of physiotherapy in the management of neurocutaneous syndromes. A case report suggests the use of physiotherapy in the management of musculoskeletal impairments in NF,[5] while another emphasizes the importance of multidisciplinary management of TSC, which includes physiotherapy.[6]
References[edit | edit source]
- ↑ Klar N, Cohen B, Lin DDM. Neurocutaneous syndromes. Handb Clin Neurol. 2016;135:565-589.
- ↑ Lucas AG, Mendez MD. Neurocutaneous Syndromes. StatPearls [Internet]. 2020 Oct 1.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 Shimizu H. Shimizu's dermatology. John Wiley & Sons; 2017 Feb 6.
- ↑ Baek JO, Park IJ, Lee KR, Ryu HR, Kim J, Lee S, Kim YR, Hur H. High-fluence 1064-nm Q-Switched Nd:YAG laser: Safe and effective treatment of café-au-lait macules in Asian patients. J Cosmet Dermatol. 2018 Jun;17(3):380-84.
- ↑ Helmers KM, Irwin KE. Physical therapy as conservative management for cervical pain and headaches in an adolescent with neurofibromatosis type 1: a case study. J Neurol Phys Ther. 2009 Dec;33(4):212-23.
- ↑ Gipson TT, Poretti A. Implementing a Multidisciplinary Approach to Treating Tuberous Sclerosis Complex: A Case Report. Child Neurol Open. 2017 Aug 22;4:2329048X17725609.