Managing Feeding in Children with Cerebral Palsy
Introduction[edit | edit source]
Eating is a fundamental part of life, not just for sustenance but also for social and cultural integration. For children with cerebral palsy, the act of eating can present unique challenges, particularly when dysphagia is involved. This section delves into managing feeding difficulties in these children, primarily from the viewpoint of a speech therapist. Dysphagia, a common issue in cerebral palsy, affects swallowing and requires specialised strategies for safe and effective nutrition. While the focus here is on speech therapy, the principles and practices discussed are part of a collaborative approach to care, involving expertise from the multidisciplinary team.
Eating[edit | edit source]
Eating is one of the fundamental processes in life. We can define it as a process for which all living entities consume different types of food with the objective of receiving necessary nutrients to survive.
But eating is much more than just consuming food. It is a moment of communication, of transmission of traditions, culture and transfer of affection. Sharing food with others is a human activity with important significance, one of them is the integration of the family and to a social group.
When this is not possible or it is difficult because a member of the group has specific problems with eating, the process of inclusion of the child to the family and community might not go smoothly. This is why that one of the main objectives for parents is to find a positive and easy way to feed their child.
Cerebral Palsy[edit | edit source]
Cerebral palsy is an umbrella term that refers to a group of disorders affecting a person’s ability to move. It is due to damage to the developing brain either during pregnancy or shortly after birth.
Cerebral palsy affects people in different ways and can affect body movement, muscle control, muscle coordination, muscle tone, reflex, posture and balance. Although cerebral palsy is a permanent life-long condition, some of these signs of cerebral palsy can improve or worsen over time.
People who have cerebral palsy may also have associated problems such as respiratory difficulties, Dysphagia, cognitive difficulties etc.
How can we classify Cerebral Palsy?[edit | edit source]
1. According to muscle tone (state of permanent contraction of the muscle).
- Hypertonia (rigid limbs)
- Hypotonia (limbs and trunk with low muscle tone, often involving reduced muscle streng.
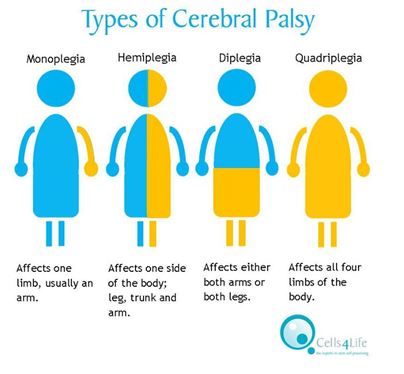
2. According to topographical distribution. Diplegia, hemiplegia, quadriplegia
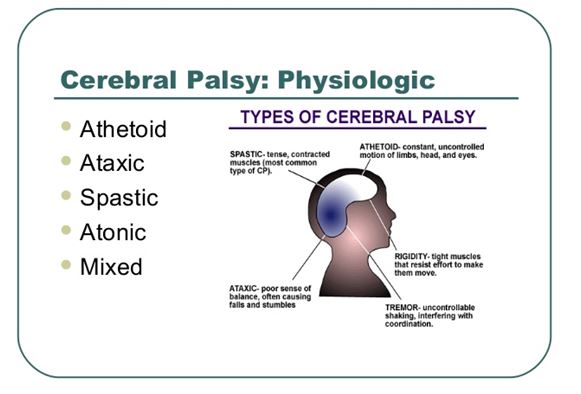
3. According to predominant motor characteristic (physiological grouping): spastic, dyskinetic, ataxic
4. Functional: According to the Gross Motor Classification System, the Manual Ability Classification System (MACS), the Functional Mobility Scale (FMS).
What other characteristics a child with cerebral palsy might have?
• Multiple disabilities
• Cognitive: Intellectual disabilities
• Sensory: abnormal touch or pain perceptions. Difficulty with vision and hearing.
• Difficulty with sucking or eating
• Motor impairments (stiffness, weakness, writhing movements)
• Epilepsy
Dysphagia in Cerebral Palsy[edit | edit source]
Swallowing[edit | edit source]
Swallowing is a complex neuromuscular process, whereby food from the mouth passes through the pharynx and esophagus into the stomach.
It corresponds to swallowing food and saliva, and in general, in making move from the mouth to the stomach any liquid food (water, juice, milk, etc.), semi-solid (porridge, compote, among others) and solids (biscuits, bread, meat and others)
Dysphagia[edit | edit source]
Dysphagia is difficulty swallowing and is evaluated by a professional speech pathologist and multidisciplinary team. This evaluation is performed through clinical observation, in addition, objective (or laboratory) evaluation methods can be used, such as videofluoroscopy and fiberoptic endoscopy swallowing (FEES).
Neurogenic Dysphagia[edit | edit source]
Neurogenic Dysphagia is an alteration of swallowing as a consequence of an alteration of the central or peripheral nervous system, which causes difficulty in any of the stages of swallowing. As a consequence of these alterations we may find dehydration, malnutrition, obstruction of the airway and pneumonia.
Signs and symptoms are associated with Dysphagia[edit | edit source]
- Sialorrhea: Sialorrhea is the unintentional loss of saliva from the mouth. This can be due to excessive production of saliva, lack of control of the lips and lack of lip closure (inadequate oral motor control).
- Delayed laryngeal elevation reflex: The reflex laryngeal elevation (10-15 mm) supports the closure of the airway and the passage of food into the esophagus. A normal delay is between 0.8 and 1 second. The laryngeal reflex is considered to be delayed when it takes more than 2 seconds to appear.
- Penetration and aspiration of food: The penetration of food occurs when it is above the level of the vocal cords, without getting to enter the lungs. In the aspiration the food enters the lungs (which can provoke pneumonias or other respiratory symptoms), being able to catch reflex of cough or to be a silent aspiration (without reflex of cough).
The cough allows expulsion of foreign bodies entering the airway, this is a measure of natural protection (physiological) that the human body has, in some children or young people with cerebral palsy this reflex is absent or greatly diminished. Food penetration or aspiration can occur at three crucial points in the swallowing process: Before swallowing, during swallowing or after swallowing of food.
- Chewing with open mouth: Insufficient control of the mandible favors the appearance of incorrect chewing movements (patterns). Proper mastication involves vertical, lateral and rotational movements, with adequate closure of the lips or mouth, which prevents food from escaping from the mouth. Children with hypertonia or hypotonia present difficulties in the correct sealing of the lips when chewing.
- Voice changes (wet voice): When food penetration or aspiration occurs, the mucous membrane covering the vocal cords is modified; this change produces a change in the voice and is what we call speech therapists a "wet voice". In those children, youngsters or young people who can not speak, this humid voice is evident in the cry or cry.
- Persistence of oral primitive reflexes and pathological reflexes: Primitive reflexes are all those that are present from birth to the age of abolition and are part of the normal development of the human being. These reflexes are: suction reflex, search reflex, bite reflex and arcade reflex.
The pathological reflexes are all those that are present in front of an alteration of the nervous system and are not part of the normal psychomotor development of the child. These reflexes are: lingual protrusion reflex, dystonia reflexes of the mouth or dystonia with open mouth and tonic bite reflex.
Delivering food[edit | edit source]
For the correct delivery of the food you must use a suitable food utensil. These can be spoons (metal or plastic) vases, plates, forks, etc. All these utensils can be those of daily use or with adaptations. From time to time they should be checked for condition and replacement due to wear. Whenever they are used they should be disinfected safely, either by washing them with soap and water or disinfectants.
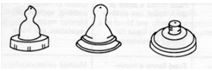
Eating utensils[edit | edit source]
- Breastfeed:The use of a bottle should be for those children who have a safe swallowing of liquids. Good posture and correct management technique should be maintained.The child should be as well seated as possible and have a head support to avoid hyperextension.
- Spoon: This is the main food utensil; it an be metal or plastic. We must have some considerations for its use. The spoon should never be larger than the tongue of the child, girl or young person. If there is a tonic bite, use a plastic spoon that is resistant.
- Nosey cup: This vessel has a recess in an edge that facilitates the ingestion of liquids (in those children or young people who can ingest them) because the liquid can be ingested without making head hyperextension.
- Plate with flange:The main characteristic of this dish is that it has a raised edge, which facilitates the withdrawal of food from the dish, mainly used in children and young people who can feed themselves and use cutlery (normal or adapted).
How to deliver food to the child[edit | edit source]
The delivery of the food considers several aspects. At the stage of preparation for food, we must consider three key elements:
- First, consider the type of food (liquid, porridge, whole) that the child ingests and the feeding way (mouth, nasogastric probe or mixed route).
- Second, the food utensil to be used, usually a small metallic spoon (tea), which is not larger than the child's or young person's tongue. If there is a strong bite, use a plastic spoon that is strong. An adapted spoon can also be used in children or young people who have the physical skills to use it.
- Third, we must consider the posture before and during the feeding process
During the feeding process, we must consider the way of approaching the spoonful of food, which must always enter from the bottom up and front, placing the well with the food in front of the child. This favors anticipation of the food process. A common precaution is to fill the spoon with food only halfway.
The child that can’t close the mouth while eating[edit | edit source]
One of the most common problems is that the child can not close their mouth (lip closure), which is related to oral motor control. To promote the correct closure of the lips and mouth, two techniques can be used:
1. The first is the frontal oral motor control. To do this, place the thumb on the chin under the lower lip, the index finger on the cheek and the other three fingers on the floor or base of the mouth.
2. The second corresponds to the lateral oral motor control, where the index finger is positioned on the chin, the thumb on the cheek and the remaining fingers on the floor of the mouth; this technique, in addition to promoting bilabial closure, helps to improve head control (head control).
In both cases, the hand must be firm, without too much force or pressure. It is only a support. In addition, it should only favor bilabial closure and the hand should not perform chewing movements that the child does not perform alone.
Time spent feeding a child[edit | edit source]
The time that is destined to the feeding is variable and will depend on each child. It must be considered that the food process is a pleasant moment and therefore must have all the necessary care. In general, taking all of the recommendations given, the food process can last from 20 to 45 minutes on average.
Posture and Environmental Management in Dysphagia[edit | edit source]
Importance of posture while feeding a child with cerebral palsy[edit | edit source]
It is very important to take care of the posture at the moment of feeding, since a correct posture improves the effectiveness for chewing and swallowing safely. At the same time, we can also notice that there are elements in the environment that distract attention from feeding activity, so we must seek a quiet place to feed, with pleasant smells, among other things, so as to convert to the feeding process in a pleasant moment and that the child would like to repeat.
Effective oral functioning[edit | edit source]
Effective oral functioning refers to the stability of the temporomandibular joint (TMJ) and the tongue for adequate ingestion of food.
Requirements for effective oral functioning
To have good stability of TMJ and language we need:
- Alignment and control of trunk (to be able to move the trunk controlled-mind).
- Development of head control.
- Postural tone as standard as possible.
- Stability / mobility points (one area of the body is supported so that another area can move).
- Stability and alignment of the scapular and pelvic girdles (pelvis and shoulders).
- Integration of trunk movement planes (the trunk has the ability to move in all directions in a controlled way)
All these elements are intimately related to achieve an adequate food intake.
Inadequate oral function in Cerebral Palsy[edit | edit source]
If the requirements of effective oral functioning are not given, either actively or passively, we can have:
- Unstable jaw (mouth moves without control).
- Depressed Jaw (open mouth).
- Lingual retraction (tongue goes back in the mouth).
- Lingual protrusion (tongue tends to move out of the mouth).
- Incoordination of tongue (tongue moves without control)
- Retraction of upper lip (upper lip is shortened)
What leads to:
- Lack of food retention (food falls out of the bottle).
- Difficulty chewing food.
- Delayed swallowing (swallowing food is delayed too much).
- Incoordination of breathing / swallowing (risk that food may pass into the lungs)
- Aspiration (food passes into the lungs)
- Severe respiratory distress (severe pneumonias)
Sucking and swallowing are basic survival skills for infants; chewing follows after certain developmental stages. Of course, these skills are important for nourishment, but they are also important for the future progress of speech.
As simple as it may seem to suck, swallow, or chew, it takes a lot of coordination of the mouth, jaw, and throat. A child may have trouble with this coordination, and therefore with one or all of these skills. She will need help and encouragement from you until she learns how to suck, swallow, and chew on her own. Be a part of the "feeding team" - with the family and health care specialists - that makes the plan to help the child develop oral motor skills and progress in feeding milestones.
If a child has a weak suck, she tires easily while feeding, and takes a long time to finish a feeding.
• The nipple can easily be removed from her mouth.
• There is not an easy flow or rhythm to the sucking pattern.
You can help her develop a stronger sucking motion by:
• Making sure the child is dry, warm, and rested before the feeding.
• Supporting the jaw, if necessary, to be sure the lips stay closed around the nipple - check with parent/feeding team if this is a problem.
• Trying different nipple shapes and sizes, and trying a softer nipple.
• (Do not try to poke a larger hole in a nipple - this may make the flow too fast and cause choking
• Cuddling the child if you can, and talking to her as you feed her.
• Offering a pacifier dipped in cold fruit juice.
A good sucking pattern is an important step towards good speech patterns which come later.
Considerations to have while feeding a child[edit | edit source]
- Place where you feed: In the arms, in a car, chair or wheel chair.
- Posture you adopt when feeding the child: lying down or sitting; Head and trunk flexed, hyperextension of head / neck
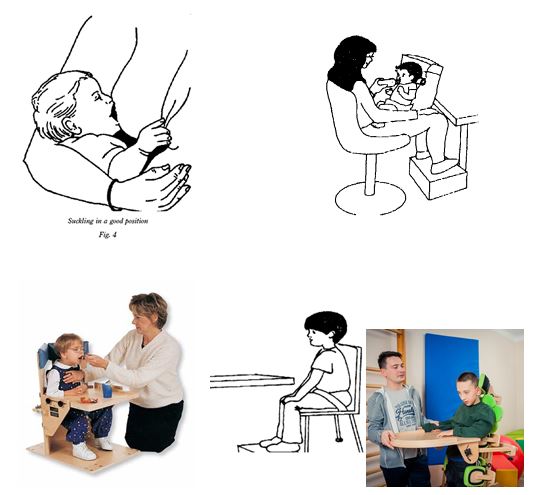
Optimal postures of the child during feeding[edit | edit source]
To generate an effective oral performance, we must ensure:
- The child's body should be upright in a sturdy seat.
- The head should be upright and slightly forward with chin tucked in.
- Arms should be forward and rest comfortably on the tray or table.
- Triple flexion of lower limbs (sitting with hips, knees and ankles at 90 °)
- Arms resting on a table or tray with a cutout when fed in a wheelchair
- Feet resting on a firm surface.
Parents should always:
- Wash your hands, and clean the child's hands and face, before positioning the child.
- Be seated in front of the child, girl or young person.
- With your feet flat on the floor.
- Always with arms supported.
- As close as possible to the child, girl or young person.
- Legs should be bent in a sitting position (about 90 degrees). You may need to use a seat belt or towels tucked around the child to keep her in position.
- Feet should rest flat on a firm surface. A covered book or box can be used to support the feet.
- Sometimes a special chair is needed to give the child support and help keep her in position.
To consider:
We achieve: Safe feeding (no risk of feeding to the lungs), improve child’s interaction with the feeder and the environment, have the child participate in the feeding process and prevent postures and patterns of abnormal movements that promote secondary complications (avoid deformities in the spine and extremities)
Swallowing and food texture[edit | edit source]
Some children have trouble with swallowing. They may gag and cough when eating, and may drool throughout the day. A child with a swallowing problem may be working with a therapist to improve swallowing skills - and may need certain food textures to allow for safe swallowing.
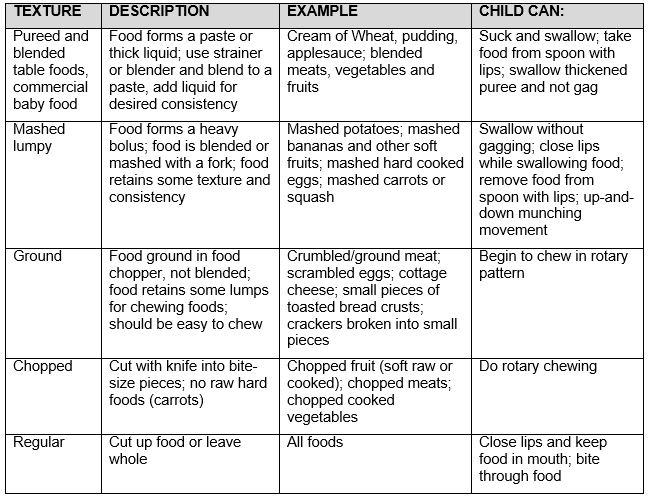
"Texture" is how smooth, lumpy, thick or thin the food is. The following table describes different textures, examples of foods, and tells what the child can usually do when she is able to handle the texture.
FOOD TEXTURE AND EATING SKILLS
Modifications in the food[edit | edit source]
Modifications will depend on the characteristics and needs of each child, and the family and medical team must be seen together. In general it must be adapted:
- Size of the serving portions: It is recommended to give small or reduced portions, but with high calories and nutrient intake. E.g. Add to meals; Olive oil or canola, butter, milk.
- Consistency or texture:It is important that the food forms smooth and homogeneous dough without lumps and thorns, easy to swallow or chew, for example creams, fruit or vegetable puree, yogurt. You should avoid textures where the liquid is mixed with the solid: E.g. noodle soup with meat.
1. Solid food: crushed, pure, soft food
2. Liquid food
Liquids are problematic for children or young people with dysphagia; it is necessary to increase their consistency to facilitate the intake. For this we can use thickeners such as fine flour (cornstarch), instant cereals or use other formulas indicated by medical staff. Some examples of consistency are: nectar-like, honey-like, pudding thick.
Introducing New Textures[edit | edit source]
A child's diet should include foods with a variety of textures to encourage mastering the skills of swallowing and chewing. With the direction of the feeding team, be sure to help the child with special needs advance to more texture in her food.
When offering a new texture to an infant or child, offer a few spoons of the familiar texture first, then the new texture. For example, when going from pureed to mashed/lumpy, offer blended carrots first - then fork-mashed carrots. This allows the child to:
- Have an opportunity to become familiar with the new texture without becoming overwhelmed or physically tired because she is dealing with a new texture.
- Learn to accept the mashed/lumpy texture without feeling rushed. In time, less of the pureed table food will need to be offered.
Textures Which Commonly Cause Problems[edit | edit source]
- Some children may have trouble swallowing thin liquids, so you will need to thicken the liquid. The thickened texture makes it easier to swallow because the liquid moves more slowly from the mouth to the throat, giving the child more time to swallow.
- The child may have trouble swallowing dry or lumpy foods. Give her pureed foods such as applesauce, cranberry sauce, or pureed fruits or vegetables in between bites of the dry or lumpy food; or use them as "dip" for the dry food.
- Multi-textured foods that involve thin liquid and solids, such as soups, can be difficult to swallow.
- Foods that do not dissolve, such as raw fruits and vegetables, can also be difficult to swallow.
Gagging[edit | edit source]
Gagging and choking can either be a sign of aversion to something new and different, or a sign that the child is having trouble swallowing. Listed below are some common causes:
- Offering the wrong texture can cause gagging and choking. Be sure to check with the feeding team specialists on proper food texture for the child.
- Offering new textures may cause gagging, even if the feeding team has recommended the new texture. Be patient - with the guidance of the feeding team specialists, introduce new textures gradually to build up tolerance of new foods.
- Gagging may be a warning for you to be careful of technique (such as placing the spoon too far back on the tongue), slow down the pace of the feeding, or put smaller amounts of food on the spoon.
- Gagging may be a behavioral response. It could be an emotional reaction from a negative experience (such as tube feedings), a way to get attention, or a form of a temper tantrum.
- Positioning of the child can affect swallowing. (Information on "Positioning" is included later in this section.)
If gagging and choking are chronic problems, it must be followed by a health care specialist. Be sure to find out why a child has swallowing problems, and what you need to do when feeding her.
Even with good oral motor control, choking can happen to any child. Here are some foods to avoid and food preparation techniques to help prevent choking:
• Cook foods until soft enough to easily pierce with a fork.
• Cut foods into small pieces or thin slices that can easily be chewed.
• Cut round foods like cooked carrots into short, thin strips rather than round pieces.
• Grind or mash and moisten food for young babies.
• Remove all bones from poultry, fish, and meat.
• Remove skins, pits, and seeds from fruit.
• Avoid nuts or seeds (such as sunflower or pumpkin), unless ground finely or chopped.
• Avoid plain peanut butter - always put on bread or crackers.
• Avoid popcorn, grapes, and hot dogs.
Chewing[edit | edit source]
When a child chews, large pieces of food are broken into smaller pieces and softened so that the food can be easily swallowed. Learning to chew may be difficult for the older child who has been on pureed foods for a long time. However, to keep the child on pureed foods when she should be advancing to more textured foods (determined by the health care specialist) will restrict her oral motor and speech development.
When a child is learning the skill of chewing, be sure to offer foods which are easy to chew.
When the child can’t be fed orally[edit | edit source]
Sometimes when oral feeding becomes a dangerous route, i.e. there is a high probability of aspiration of food to the lungs or it is not possible to cover the caloric, nutritional and water requirements of the child, girl or young, it is recommended to use other ways such as:
Nasogastric tube: It is a food route, which runs from the nose to the stomach. Its use is recommended when it is anticipated that the need to contribute by this route will not be more than 4 to 6 weeks in duration and there is no gastroesophageal reflux.
Gastrostomy: It is a food route that goes directly to the stomach, is implanted when the oral route is not used in a prolonged way (beyond 4-6 weeks). The advantages of a gastrostomy are that with this food route it is easier to handle at home and there are fewer risks of injury (nose, throat) and the main thing allows the incorporation of more food in comparison to the nasogastric tube.
Mixed: Both feeding routes are used (oral + nasogastric or Gastrostomy). The idea is to deliver orally the most consistent and safer foods, such as porridge and administering liquid foods (water, juices, milk).
Conclusion[edit | edit source]
Managing feeding in children with cerebral palsy, especially in the context of dysphagia, is a multifaceted challenge that requires a nuanced and comprehensive approach. The perspectives and techniques from a speech therapy viewpoint are crucial in addressing these complexities. However, it is the collaborative effort and expertise of various healthcare professionals, including occupational therapists and physiotherapists, that is needed to improve outcomes. Embracing an multidisciplinary team approach will ensure effective and safe nutrition as well as promoting the overall development and quality of life for children with cerebral palsy.
Bibliography[edit | edit source]
- Logemann, J. (1997). Evaluation and treatment of swallowing disorders. Pro Ed.
- Management of Movement Disorders of Children with Cerebral Palsy Scrutton, D; Damiano, A; Mayston, M; (2004) Management of Movement Disorders of Children with Cerebral Palsy.[Book]. Clinics in Developmental Medicine. (2nd ed.). Mac Keith Press: London.
- Ministerio de Salud. (2010). Guia clinica: alimentacion en niños con dificultad en masticar y deglutir derivado de alteracion del sistema nervio-so. Santiago: Ministerio de Salud, Subsecretaria de Salud Pública.
- Velasco, M., Arreola, V., Clavé, P., & Puiggrós, C. (2007). Abordaje clínico de la disfagia orofaríngea: diagnóstico y tratamiento. Nutrición clínica en medicina, 174-202.
- Feeding method and health outcomes of children with cerebral palsy. Rogers B1, J Pediatr. 2004 Aug;145(2 Suppl):S28-32.
- Feeding children with cerebral palsy and swallowing difficulties, J C Arvedson. European Journal of Clinical Nutrition (2013) 67, S9–S12; doi:10.1038/ejcn.2013.224
- https://www.cerebralpalsy.org.au/what-is-cerebral-palsy
- Gastrostomy feeding for children, Cerebral Palsy Alliance. https://www.cerebralpalsy.org.au/about-cerebral-palsy/interventions-and-therapies/gastrostomy-feeding-for-children-with-cerebral-palsy/
- Interventions for Feeding and Nutrition in Cerebral Palsy- Executive Summary. Effective Health Care Program, Comparative effectiveness Review Number 94
- Dysphagia- MyChild at CerebralPalsy.org. http://www.cerebralpalsy.org/information/dysphagia
- Clinical practice: swallowing problems in cerebral palsy. Erasmus CE, van Hulst K, Rotteveel JJ, Willemsen MA, Jongerius PH. Eur J Pediatr. 2012 Mar;171(3):409-14. doi: 10.1007/s00431-011-1570-y. Epub 2011 Sep 20.
- http://disabilitycentre.lshtm.ac.uk/files/2013/06/Module-6-Getting-to-know-cerebral-palsy-v1-hires.pdf